Delirious State and Agitation Following Heparin Induced Stevens-Johnson Syndrome
Reza Bidaki1, Sogol Ale Saeidi2, Mojtaba Babaei Zarch3
1 Research Center of Addiction and Behavioral Sciences, Shahid Sadoughi University of Medical Sciences, Yazd, Iran; Diabetes Research Center, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
2 Medical Student, Shahid Sadoughi University of Medical Sciences, International Campus, Yazd, Iran.
3 Medical Student, Student Research Committee, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Mojtaba Babaei Zarch, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
E-mail: mojtaba.babaei72@yahoo.com
Delirium, Mucocutaneous lesion, Anticoagulant
Dear Editor,
The side effects of heparin include hemorrhage, osteoporosis, telogen effluvium, hypoaldosteronism, hypersensitivity reactions (urticaria and anaphylactic shock), hypereosinophilia, vasospastic reactions (pain, cyanosis and severe itching or burning plantar sensations), erythematous infiltrated plaques, skin necrosis and thrombocytopenia [1].
Stevens–Johnson Syndrome (SJS) is a life threatening cutaneous adverse drug reaction. The incidence of SJS is evaluated from one to two cases per million person-years [2]. We hereby report SJS as a rare complication of heparin.
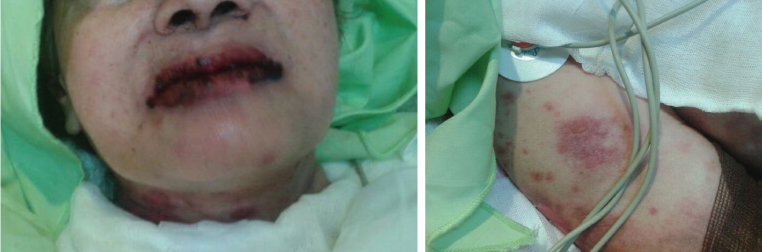
A 61-year-old married woman, from central Iran was hospitalized due to acute pancreatitis and pancreatic abscess. Heparin prophylaxis was initiated, subsequent to which mucocutaneous lesions appeared [Table/Fig-1]. Dermatology consultation was done and the required treatment was started.
Mucocutaneous lesions caused by heparin.
The patient had a history of diabetes mellitus, hypothyroidism and hypertension. She received tablet prednisolone 50 mg 1/2 bid, tablet metoprolol 50 mg bid, tablet lorazepam 2 mg 1/2 qhs, tablet alprazolam 0.5 mg daily.
For the present condition, fluconazole and pantoprazole were prescribed. She was irritable, had insomnia, persecutory and visual hallucinations because of severe lip and oral mucosa burning. Psychiatric consultation was requested for delirium. The patient had a history of insomnia without mood or psychotic disorder. The psychiatrist prescribed tablet doxepin 25 mg/every night, tablet chlorodiazopoxide 10 mg/12 hourly, and tablet halopridol 0.5 mg/8 hourly. The patient responded favourably to drugs. Naranjo score was 9 in our case. Irritability decreased significantly and the patient was able to get adequate sleep. She was discharged after 48 hours with a good general condition.
[1]. Breathnach S, Drug reactionsRook’s Textbook of Dermatology 2010 8th ed:1-177. [Google Scholar]
[2]. Marzano AV, Borghi A, Cugno M, Adverse drug reactions and organ damage: The skinEur J Intern Med 2016 28:17-24. [Google Scholar]