Simultaneous Occurrence of Thyroiditis in Ectopic and Eutopic Thyroid Masquerading as Thyroglossal Cyst
Aditi Chopra1, Yogendra Singh2, Manju Kaushal3, Anil Taneja4, Bindu Kulshreshtha5
1 Senior Resident, Department of Endocrinology, PGIMER, Dr RML Hospital, Delhi, India.
2 Senior Resident, Department of Endocrinology, PGIMER, Dr RML Hospital, Delhi, India.
3 Professor, Department of Pathology, Dr RML Hospital, New Delhi, India.
4 Professor, Department of Radiology, Dr RML Hospital, Delhi, India.
5 Associate Professor, Department of Endocrinology, PGIMER, Dr RML Hospital, Delhi, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Bindu Kulshreshtha, Associate Professor and Head, PGIMER, Dr RML Hospital, New Delhi-110001, India.
E-mail: drbindu25@yahoo.co.uk
Ectopic thyroid gland is a rare condition usually presenting with neck swelling or hypothyroidism. In most cases, ectopic thyroid tissue is the only functioning thyroid tissue, but it may rarely be associated with normal thyroid gland. Thyroiditis in an ectopic thyroid gland is very rare. Here, we describe a 13-year-old girl who was initially suspected, as a having a thyroglossal cyst. Thyroid functions were suggestive of thyrotoxicosis. She was diagnosed to have simultaneous occurrence of thyroiditis in the ectopic and eutopic thyroid glands. This case was exceedingly rare since this patient presented with thyrotoxicosis unlike previous reported cases who were either euthyroid or hypothyroid.
Autoimmunity, Ectopic thyroid tissue, Thyrotoxicosis
Case Report
A 13-year-old girl, a resident of Delhi, presented to the Department of Surgery with chief complaints of swelling in the midline of neck since one year. She told that the swelling was not associated with pain, fever, dysphagia, hoarseness of voice or any respiratory complaints. History of heat intolerance, palpitations, anxiety and weight loss was present since two months. There was no history of tremors, any bowel complaints or protrusion of eyes. Patient had attained menarche two months prior to presentation. Examination of the neck revealed swelling in the infrahyoid region that moved with deglutition. An initial presumptive diagnosis of thyroglossal cyst was made. Patient was advised for Thyroid Function Tests (TFT). Thyroid Stimulating Hormone (TSH) was 0.02 μU/ml (normal 0.5-5.0), Free Thyroxine (FT4) was 1.78 ng/dl (normal 0.7-2.0) and free Tri-iodothyronine (FT3) was 6.9 pg/dl (normal 2.0-4.4). Other blood investigations were normal. With reports suggesting thyrotoxicosis, she was referred to the Department of Endocrinology. On examination the blood pressure was 118/80 mmHg and the pulse rate was 108/min. Her height was 152 cm and weight was 39 kg. There were no tremors, ophthalmopathy, or dermopathy. A 1.5×1.5 cm firm, non-tender swelling was present in the midline of the neck above the thyroid gland.
The swelling moved with deglutition and protrusion of the tongue. In addition, the thyroid gland was also diffusely enlarged, the right lobe being more enlarged than the left lobe. The thyroid gland was firm and non-tender and there was no bruit. The systemic examination was normal.
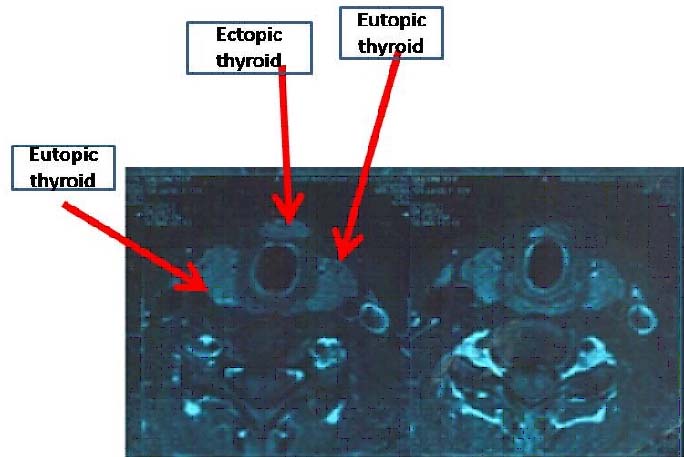
An ultrasound of the neck was done that showed a midline heterogenous mass (1.48 × 0.58 × 2.15 cm) predominantly hypoechoic, superior to isthmus of thyroid and a possibility of ectopic thyroid was considered. Both the lobes of thyroid gland at normal position were also enlarged with heterogenous echotexture and increased vascularity. Magnetic Resonance Imaging (MRI) of the neck also showed a midline lesion just above thyroid with signal intensities and post contrast enhancement similar to thyroid suggestive of ectopic thyroid [Table/Fig-1]. A Tc 99m-pertechnetate scan revealed no accumulation of radiotracer in the region of both lobes of thyroid or anywhere in the head and neck region [Table/Fig-2]. Radioactive Iodine Uptake (RAIU) showed decreased uptake (2hr – 0.9% & 24 hr – 0.7%) suggestive of thyroiditis. Fine Needle Aspiration Cytology (FNAC) from both ectopic nodule and eutopic thyroid gland showed cytological features of chronic diffuse lymphocytic thyroiditis. [Table/Fig-3]. On the basis of history, examination and investigations a final diagnosis of thyroiditis of both ectopic and eutopic thyroid tissue was made. She was given symptomatic treatment and propranolol 40 mg twice a day was started. After a period of three to four months, she had improvement in her symptoms and she even reported a mild decrease in the size of the swelling. A TFT was then repeated which was normal. TSH was 2.74 μU/ml, FT4 was 0.8 (ng/dl), FT3 was 3.42 (pg/dl) and anti-Thyroid Peroxidase (anti-TPO) was 40 IU/ml (normal < 60). Repeat Tc 99 pertechnate scan thyroid scan showed normal uptake in the thyroid gland [Table/Fig-4].
MRI of the neck showing eutopic and ectopic thyroid gland in the midline.
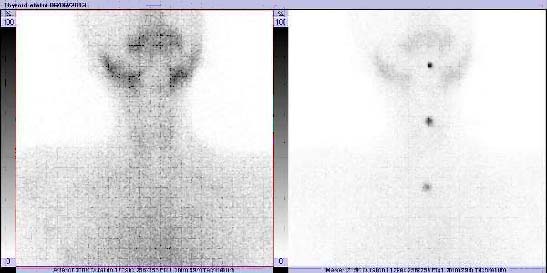
Tc-99m thyroid scan at presentation showing no tracer uptake in both ectopic and eutopic thyroid gland.
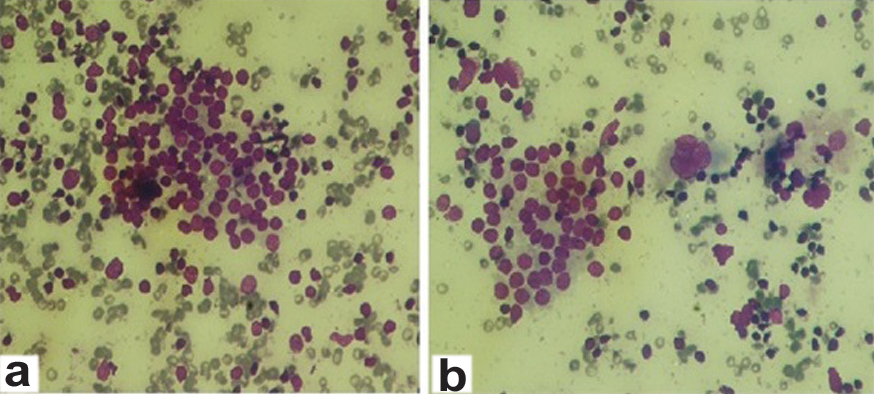
FNAC from both the ectopic and eutopic thyroid tissue showing cytological evidence of diffuse lymphocytic thyroiditis(Geimsa stain 400 X).
Tc-99m thyroid scan four months after initial presentation showing normal uptake in the thyroid
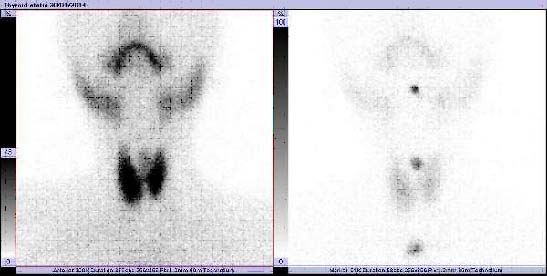
Discussion
Ectopic Thyroid Tissue (ETT) is a rare developmental anomaly with a reported incidence of 1 in 1,00,000 [1]. ETT results due to abnormal migration of gland from posterior dorsal midline of tongue to its normal pretracheal position. The various locations of ectopic thyroid tissue could be lingual, sublingual, prelaryngeal or substernal, depending on degree of descent. Amongst all locations lingual thyroid is the most common, contributing to 90% of all cases. In most cases (70-75%), ectopic thyroid is the only functioning thyroid tissue present. However, rarely eutopic thyroid gland which is usually hypoplastic can be found along with ectopic thyroid. On rare occasions, a normal sized thyroid at normal position can be present along with ectopic thyroid [1-3].
The patients with ectopic thyroid may report at any age; however presentation during adolescence or pregnancy is more common due to increase physiological demand of thyroid hormones. Patients usually present with complaints of neck mass, lump in throat, or features of hypothyroidism. Hormone production in ectopic thyroid is usually insufficient, leading either to a subclinical or clinical hypothyroid state. The incidence of clinical hypothyroidism in ectopic thyroid tissue varies from 24-60% [1,2]. Primary malignant transformation has also been reported rarely in ectopic thyroid tissue. All forms of carcinoma including papillary, follicular, Hurthle cell and medullary carcinoma in ectopic locations have been described [1,2].
Autoimmune affliction of ectopic thyroid tissue has also been reported earlier, though rarely. Till date, we found 15 case reports of Graves’s disease in ectopic thyroid on pubmed search with terms “Graves’ disease and ectopic thyroid”. Graves’s disease has been described in ectopic thyroid locations including lingual, infrahyoid, suprahyoid, submandibular, mediastinal and even in thyroglossal duct tissue remnant [3-17].
There are only anecdotal case reports of thyroiditis in ectopic thyroid tissue. We found eight such cases on pubmed search (six female and two male; 7-83 years of age). The various locations of ETT were lingual (three cases), infrahyoid (three cases) and submandibular (one case) and strap muscles (one case) [18-25]. In six of the eight cases, ectopic thyroid was the only functioning thyroid tissue present [19-24]. Five of the eight patients had either clinical or subclinical hypothyroidism [19-23], whereas three were euthyroid [18,24,25]. Thyroiditis in ectopic thyroid was diagnosed with difficulty. In three cases an initial presumptive diagnosis of thyroglossal cyst was considered as in our case [18,19,22]. Akpinar ME et al., reported a case of a 60-year-old lady with a submandibular mass who was suspected to have Hurthle cell neoplasia on FNAC [24]. But later she was diagnosed to have thyroiditis on histopathology of post operative specimen. Our patient presented with neck swelling and self limiting thyrotoxicosis due to thyroiditis involving both eutopic and ectopic thyroid tissue. Unlike previous eight cases that had hypothyroidism or euthyroidism at presentation, our patient presented with self-limiting thyrotoxicosis. The initial decreased uptake on the thyroid scan in our patient was surprising. However, an initial negative uptake on thyroid scan in patients with painless thyroiditis has been reported earlier [26,27].
Conclusion
In conclusion, for the first time, we describe simultaneous occurrence of thyroiditis in the ectopic and eutopic thyroid tissue in a 13-year-old girl. Only a few cases of thyroiditis in the ectopic thyroid gland have been described earlier. Also, this patient presented with self limiting thyrotoxicosis unlike hypothyroidism reported in the previous cases.
[1]. Noussios G, Anagnostis P, Goulis DG, Lappas D, Natsis K, Ectopic thyroid tissue: anatomical, clinical, and surgical implications of a rare entityEur J Endocrinol 2011 165(3):375-82. [Google Scholar]
[2]. Ibrahim NA, Fadeyibi IO, Ectopic thyroid: etiology, pathology and managementHormones Athens 2011 10(4):261-69. [Google Scholar]
[3]. Khan SH, Rather TA, Syed T, Simultaneous occurrence of Graves’ disease in eutopic and ectopic thyroid tissues: A case report and review of literatureIndian J Nucl Med 2012 27(4):254-56. [Google Scholar]
[4]. Mollar-Puchades MA, Merino-Torres JF, Segovia-Portolés R, Abellán-Galiana P, Gómez-Vela J, Piñón-Sellés F, Ectopic thyroid tissue and Graves’ disease in an elderly patientThyroid 2006 16:701-02. [Google Scholar]
[5]. Prakash R, Lakshmipathi N, Jena A, Behari V, Chopra MK, Hyperthyroidism caused by a toxic intrathoracic goiter with a normal-sized cervical thyroid glandJ Nucl Med 1986 27:1423-27. [Google Scholar]
[6]. Basaria S, Cooper DS, Graves’ disease and recurrent ectopic thyroid tissueThyroid 1999 9:1261-64. [Google Scholar]
[7]. Shinto A, Bandopadhyay A, Selvakumar J, Graves disease with midline ectopic and bifid pyramidal lobes on pertechnetate thyroid scintigraphyClin Nucl Med 2009 34:31-32. [Google Scholar]
[8]. Yamauchi M, Inoue D, Sato H, Ashida C, Hiraumi H, Shan L, A case of ectopic thyroid in lateral neck associated with Graves’ diseaseEndocr J 1999 46:731-34. [Google Scholar]
[9]. Kumar R, Gupta R, Bal CS, Khullar S, Malhotra A, Thyrotoxicosis in a patient with submandibular thyroidThyroid 2000 10:363-65. [Google Scholar]
[10]. Kisakol G, Gonen S, Kaya A, Dikbas O, Sari O, Kiresi D, Dual ectopic thyroid gland with Graves’ disease and unilateral ophthalmopathy: A case report and review of the literatureJ Endocrinol Invest 2004 27:874-77. [Google Scholar]
[11]. Qiu ZL, Xue YL, Shen CT, Zhu RS, Luo QY, Graves’ disease in an adolescent with dual congenital ectopia and no orthotopic thyroid gland identified by Tc-99m-pertechnetate SPET/CT imagingHell J Nucl Med 2014 16(3):237-39. [Google Scholar]
[12]. Winters R, Christian RC, Sofferman R, Thyrotoxicosis due to ectopic lateral thyroid tissue presenting 5 years after total thyroidectomyEndocr Pract 2011 17(1):70-73. [Google Scholar]
[13]. Basili G, Andreini R, Romano N, Lorenzetti L, Monzani F, Naccarato G, Recurrence of Graves’ disease in thyroglossal duct remnants: relapse after total thyroidectomyThyroid 2009 1912:1427-30. [Google Scholar]
[14]. Buckingham H, Sauerwein TJ, Golding AC, Graves’ disease in the cervical thyroid and thyroglossal duct remnant: case report and review of literatureEndocr Pract 2006 12(4):401-05. [Google Scholar]
[15]. Rao PN, Pandit N, Kumar R, Upadhya IV, Vidya Sagar MS, Ectopic functioning thyroid tissue in the thyroglossal duct detected by radionuclide imagingClin Nucl Med 2005 30(9):630 [Google Scholar]
[16]. Azzam A, Nitunga N, Baulieu JL, De Calan L, Royere D, Lecomte P, Thyroid ectopia and Basedow’s diseasePresse Med 1988 17(8):383-85. [Google Scholar]
[17]. Cunha FM, Rodrigues E, Oliveira J, Saavedra A, Vinhas LS, Carvalho D, Graves’ disease in a mediastinal mass presenting after total thyroidectomy fornontoxic multinodular goiter: a case reportJ Med Case Rep 2016 10:70 [Google Scholar]
[18]. Gök U, Kele E, Cobanolu B, Yildiz M, Dönder E, Ectopic thyroid and Hashimoto’s thyroiditis arising from a thyroglossal duct cyst: a case reportKulak Burun Bogaz Ihtisas Dergisi 2003 10(1):29-32. [Google Scholar]
[19]. Wein RO, Norante JD, Doerr TD, Hashimoto’s thyroiditis within ectopic thyroid gland mimicking the presentation of the thyroglossal duct cystOto Laryngol Head Neck Surgery 2001 125:274-76. [Google Scholar]
[20]. Cappelli C, Gandossi E, Cumetti D, Castellano M, Pirola I, De Martino E, Ectopic lingual thyroid tissue and acquired hypothyroidism: case reportE. Ann Endocrinol(Paris) 2006 67(3):245-48. [Google Scholar]
[21]. Mariani M, Palpacelli A, Mussoni A, Rossodivita AN, Hashimoto’s thyroiditis: an accidental discovery of a lingual thyroid in a 7-year-old childBMJ Case Rep 2013 :1-4. [Google Scholar]
[22]. Pradeep PV, Jayashree B, Ectopic thyroid with Hashimoto’s thyroiditis presenting as goitrous hypothyroidismEur J Pediatr Surg 2013 21(5):339-40. [Google Scholar]
[23]. Pandey P, Dixit A, Bedi S, Kapoor K, Mahajan NC, Hashimoto’s thyroiditis in ectopic thyroid tissue: a diagnostic surpriseCytopathology 2012 23(6):419-21. [Google Scholar]
[24]. Akpınar ME, Azizli E, Gör AP, Behzatoglu K, Yigit O, Ectopic thyroid tissue in the submandibular region presenting with signs of thyroiditisIstanbul Med J 2013 14:146-48. [Google Scholar]
[25]. Garcia-Rodriguez L, Dharia R, Massey B, Ectopic thyroid tissue with Hashimoto’s thyroiditisWMJ 2016 115(1):47-48. [Google Scholar]
[26]. Oh SB, Ahn J, Kim IJ, Thyrotoxic periodic paralysis associated with transient thyrotoxicosis due to painless thyroiditisJ Korean 2012 27-7:822-26. [Google Scholar]
[27]. Ramtoola S, Maisey MN, Clarke SE, Fogelman I, The thyroid scan in Hashimoto’s thyroiditis: the great mimic 1988 9(9):639-45. [Google Scholar]