An Unusual Presentation of Congenital Cystoadenomatoid Malformation of Lung
Ansul Kumar1, Dileep Kumar Singh Rathor2, Anubhav Gupta3, Vijay Kumar Gupta4, Ajit Padhya5
1 Associate Consultant, Department of Cardio-Thoracic and Vascular Surgery, Fortis Escort’s Heart Institute, New Delhi, India.
2 Senior Resident, Department of Cardio-Thoracic and Vascular Surgery, PGIMER Dr. RML Hospital, New Delhi, India.
3 Professor, Department of Cardio-Thoracic and Vascular Surgery, PGIMER Dr. RML Hospital, New Delhi, India.
4 Professor and Head, Department of Cardio-Thoracic and Vascular Surgery, PGIMER Dr. RML Hospital, New Delhi, India.
5 Senior Resident, Department of Cardio-Thoracic and Vascular Surgery, PGIMER Dr. RML Hospital, New Delhi, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Ansul Kumar, Flat No. 68-D, Pocket A, Sukhdev Vihar, New Delhi-110025, India.
E-mail: docansul@gmail.com
Congenital cystic lesion of pulmonary airways, Recurrent lower respiratory tract infection, Malignant cystic disease
A 14-year-old male presented with dyspnoea and recurrent respiratory tract infection since two years, managed with conservative management, but symptoms aggravated and he developed three episode of left lower lobe pneumonia in last six month. This episode was not associated with persistent fever, weight loss, haemoptysis, immunocompromised condition or any cardiac illness since last one week. Patient developed left sided chest pain which got worse on deep inspiration along with fever and lower respiratory tract infection.
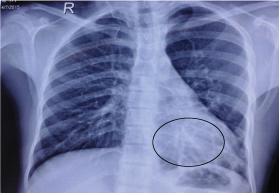
Chest radiograph PA view showed homogenous opacity in left lower zone of lung with incomplete obscuring of left costo-phrenic angle and dome of diaphragm [Table/Fig-1].
Chest radiograph (Postero-anterior view) showing uniform homogenous ill-defined opacity in the lower left lung field circle. There was no evidence of pleural/pericardial effusion or pneumothorax.
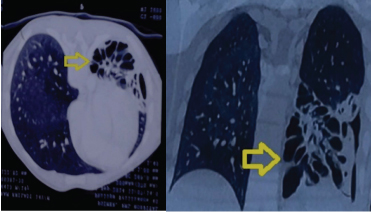
Contrast Enhanced Computed Tomography (CECT) chest revealed multiple well-defined cystic radiolucencies of variable sizes communicating with bronchi in left lower lobe, which were nearly completely replacing it. Broncheiactatic changes were observed in adjacent area and patchy areas of consolidation were noted in superior segment of left lower lobe [Table/Fig-2a,b].
(a) Contrast enhanced axial computed tomography of the chest demonstrating pneumatocele of the left lower lobe of the lung (arrow). There was presence of multilocular cystic lesions with thin walls of variable sizes on the left side compared to the normal lung parenchyma on the right side; (b) Contrast enhanced coronal computed tomography of the chest showing multiple large cystic areas in the left lower lobe of the lung (arrow). Air fluid levels were not evident.
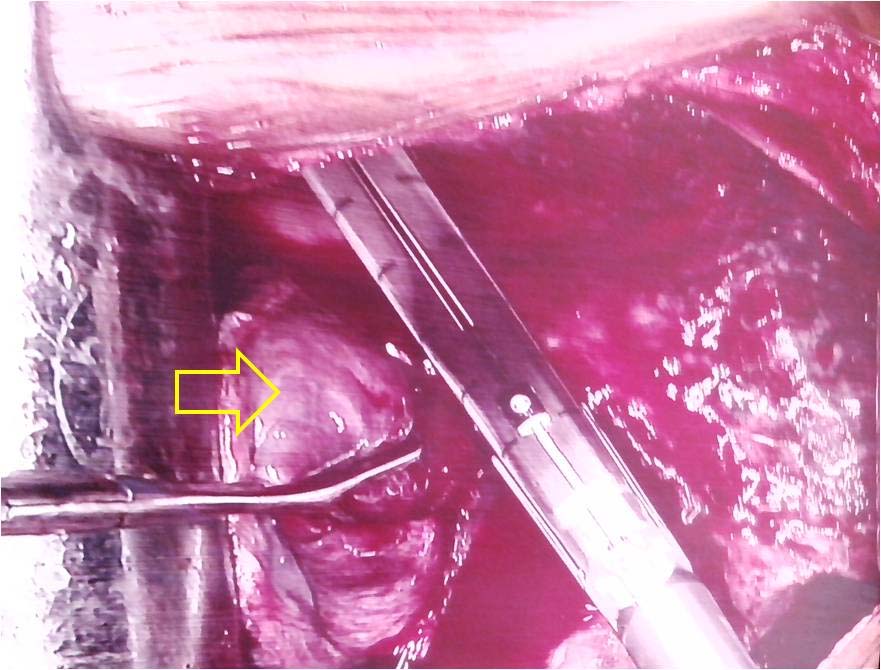
Left lower lobectomy was done. Intraoperatively large, fleshy, cystic, vascular mass involving whole left lower lobe with dense adhesion between lung mass and parietal pleura was observed [Table/Fig-3]. Resected specimen showed large cyst wall lined by necrotic debris along with multiple small cysts [Table/Fig-4]. Histopathological evaluation showed cysts lined by pseudostratified ciliated columnar epithelium with cystic and malformed bronchi and bronchioles. The findings confirmed the diagnosis of late onset left lower lobe Congenital Cystoadenomatoid Malformation (CCAM). On follow up satisfactory clinical and radiological improvement occur in nine month.
Intraoperative photograph showing large, fleshy, cystic, vascular mass involving left lower lobe.
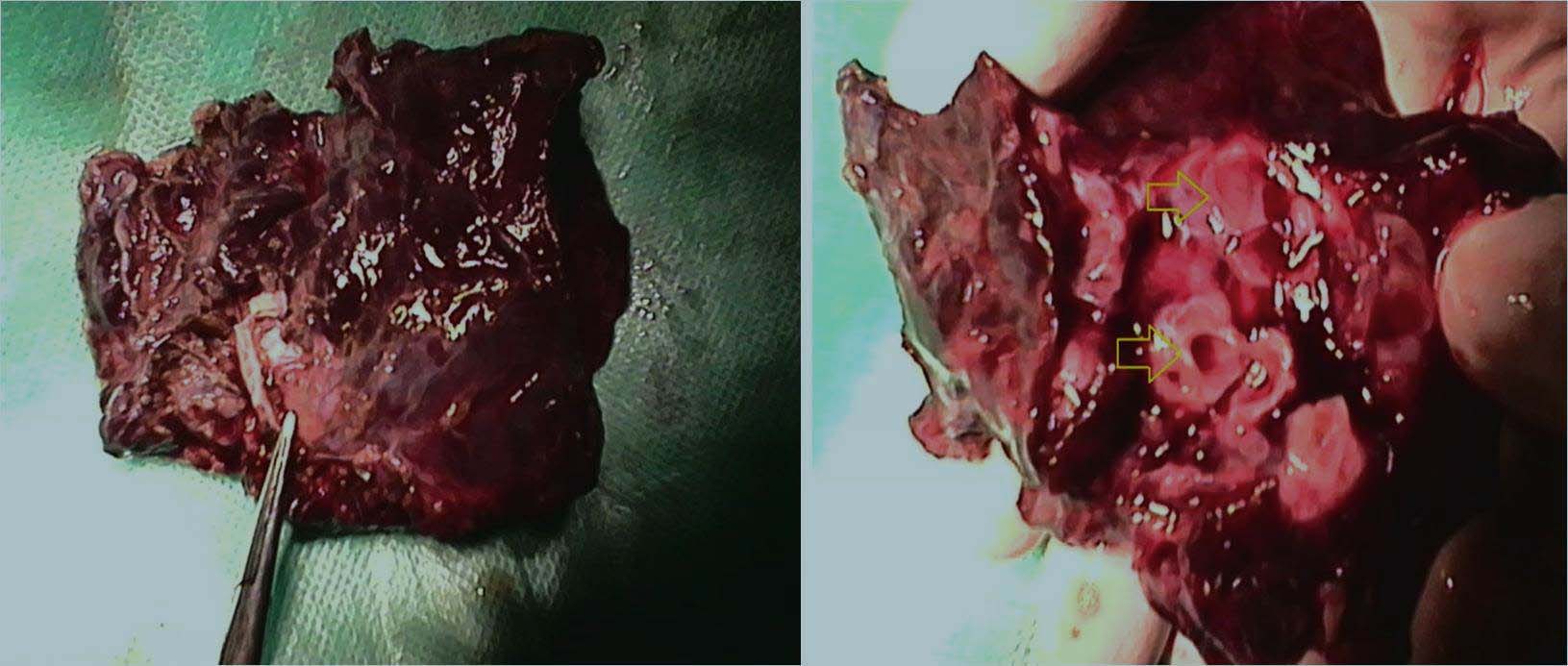
Photograph of the gross resected specimen showing large widely spaced and irregular cystic structures (arrow).
CCAM is a developmental abnormality of lung development which was originally described by Ch’in KY and Tang MY in 1949 [1]. The three subtypes traditionally associated with this congenital thoracic malformation have now been expanded into 5 types with a revised nomenclature of (CPAM) [2,3]. Majority of cases are diagnosed in the first two years of life. Clinical features include tachypnea, grunting, retraction, and cyanosis [4]. CCAM occurring in an adult is rare and presents as incidental finding or secondary to repeated infection [5]. Only few authors have previously reported CCAM occurring in adult or adolescent patients [5-8]. Differential diagnosis includes congenital pneumonia, pleural effusion, haemothorax, congenital diaphragmatic hernia, pediatric pneumothorax, pneumatocele, sequestration of lung.
Healthy individual with recurrent episode of pneumonias in same lobe of lung should be evaluated for acquired and congenital anatomical lesion of lung. Though CCAM is rarely present with adult patient, it should be kept in differential diagnosis of radiologically proven cystic lesion of lung parenchyma, for its small but definitive risk of malignant transformation [9]. Early diagnosis and surgical resection is mainstay of management. Close clinical and radiological follow up required for malignant change even after resection of the lesion.
[1]. Ch’in KY, Tang MY, Congenital adenomatoid malformation of one lobe of a lung with general anasarcaArch Pathol (Chic) 1949 48:221-29. [Google Scholar]
[2]. Stocker JT, Madewell JE, Drake RM, Congenital cystic adenomatoid malformation of the lung. Classification and morphologic spectrumHum Pathol 1977 8:155-71. [Google Scholar]
[3]. Stocker JT, Congenital pulmonary airway malformation: A new name and an expanded classification of congenital cystic adenomatoid malformation of the lungHistopathol 2002 41:424-31. [Google Scholar]
[4]. Chikkannaiah P, Kangle R, Hawal M, Congenital cystic adenomatoid malformation of lung: Report of two cases with review of literatureLung India: Official Organ of Indian Chest Society 2013 30(3):215-18. [Google Scholar]
[5]. Feng A, Cai H, Sun Q, Zhang Y, Chen L, Meng F, Congenital cystic adenomatoid malformation of lung in adults: 2 rare cases report and review of the literatureDiagn Pathol 2012 7:37 [Google Scholar]
[6]. Plit ML, Blott JA, Lakis N, Murray J, Plit M, Clinical, radiographic and lung function features of diffuse congenital cystic adenomatoid malformation of the lung in an adultEur Respir J 1997 10(7):1680-82. [Google Scholar]
[7]. Herrero Y, Pinilla Torres Nistal M, Pardo M, Gómez N, Cystic adenomatoid malformation of the lung presenting in adulthoodAnn Thorac Surg 2005 79(1):326-29. [Google Scholar]
[8]. Khan NU, Jones MT, Greaves M, Case report: Congenital cystic adenomatoid malformation of an entire lung in a 33-year-old man: a case report and review of the literatureBr J Radiol 2008 81(971):e276-78. [Google Scholar]
[9]. Lantuejoul S, Nicholson AG, Sartori G, Piolat C, Danel C, Brabencova E, Mucinous cells in type 1 pulmonary congenital cystic adenomatoid malformation as mucinous bronchioloalveolar carcinoma precursorsThe American Journal of Surgical Pathology 2007 31(6):961-69. [Google Scholar]