Is the Cage an Additional Hardware in Lumbar Interbody Fusion for Low Grade Spondylolisthesis? A Prospective Study
Ramachandran Govindasamy1, Prince solomon2, Deepak Sugumar3, James J Gnanadoss4, Yuvaraja Murugan5, Syed Najimudeen6
1 Assistant Professor, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
2 Assistant Professor, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
3 Postgraduate Student, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
4 Professor, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
5 Assistant Professor, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
6 Professor, Department of Orthopedics, PIMS Medical College, Pondicherry, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Ramachandran Govindasamy, L-32 MK colony, Mandharakuppam, Neyveli, Tamil Nadu, India.
E-mail: mail2ram8544@gmail.com
Introduction
Lumbar interbody fusion has become the standard of care for the management of lumbar instability, where fusion is achieved using bone grafts, cages, etc.
Aim
The aim of the study was to compare the outcomes of the interbody fusion using interbody cage technique and stand alone local bone graft technique.
Materials and Methods
A total of 30 patients, operated for single level instability with low grade lytic and degenerative spondylolisthesis of L4-5/L5-S1, were selected and grouped into two groups: Group I (stand alone grafts) and Group II (interbody cage and graft) based on computer generated random numbers. All patients who underwent interbody fusion through conventional open posterior approach were included in the study. Data regarding the time taken for interbody fusion, formaninal height maintenance, disc height restoration, translation, functional scores (VAS,ODI) and operative complications were analysed using in both the groups was collected and a student’s-t test was performed to evaluate the difference.
Results
The mean age of patients in Group I was 46.7 years whereas, the mean age of patients in Group II was 43.5 years with mean age of 46.7 years and 43.5 years respectively. Interbody fusion, was achieved in seven and eight months in Group I and II respectively (p>0.05). The clinical results of both groups were comparable and there was no significant difference between the two groups in VAS score (p-0.147) and ODI score (p-0.983). Radiological parameters were also comparable and there was no significant difference between the postoperative measurements of the two groups (p=0.348 for translation, p=0.310 for intervertebral disc height and p=0.135 for foraminal height). One patient in Group I had transient foot drop which recovered, while one in Group II had infection, wound was managed with wound wash and antibiotics and another patient in Group II had pseudoarthrosis.
Conclusion
Lumbar interbody fusion with standalone local bone grafts is sufficient in single level low grade spondylolisthesis treated by conventional open surgery.
Conventional posterior approach, Disc height, Foraminal height, Stand alone bone graft, Translation
Introduction
Spinal instability pain due to spondylolisthesis is a common problem and spinal fusion is performed if conservative treatment fails. Lumbar spinal fusion is of various types, ranging from uninstrumented posterolateral fusion to instrumented interbody fusion. The current standard of care for instability related back pain is instrumented interbody fusion.
Interbody fusion can be achieved by either local autografts or by using various types of cages along with grafts. The cages vary from titanium cages, Poly Ether Ether Ketone (PEEK) cages, expandable cages etc., of various shapes. The grafts that were most commonly used varies from simple local autograft, iliac crest autograft, and autograft expanders like demineralized bone matrix, allograft, artificial bone, rh BMP 2,7 etc., [1].
The placement of cage to the intervertebral space increases the intrevertebral disc height, which further increases the foraminal height and helps in indirect decompression of the roots. [2]. It also aids in reduction of listhesis in high grades, and acts as anterior load sharing device [3]. The increase in intervertebral height is responsible for the maintenance of segmental and global lumbar lordosis in degenerated disc disorders [4]. The disadvantage of using a cage is that it adds an extra cost to the surgery, has chances of subsidence in osteoporotic vertebra, chances of nerve root and dural injuries while insertion, as well as difficulty in assessment of fusion postoperatively [5].
The usage of standalone graft technique in the form of local autograft or iliac graft provides more surface area for fusion, less fear of infection especially in interbody fusion for discitis, is cost-effective and is more biological. But it was always a concern when it comes to disc height if not instrumented from posterior and graft site morbidity is a major concern in iliac graft harvesting [6].
The purpose of this prospective study was to evaluate and to compare the advantages, disadvantages of using an additional cage over standalone local bone graft in low grade spondylolisthesis of single motion segment secondary to lytic and degenerative types.
Materials and Methods
This prospective randomized study was conducted between September 2013 to September 2016, with minimum follow up of one year. All patients between 25-60 years of age and who underwent modified Trans-foraminal Lumbar Interbody Fusion (TLIF) through conventional open means for single level low grade antero listhesis were included in the study. A written informed consent was obtained from all the patients. Hospital ethical committee approval was obtained before commencement of the study. All patients underwent standing and dynamic radiographs, along with Magnetic Resonance Imaging (MRI). Visual Analog Scale (VAS) score [7], ODI score [8], translation, intervertebral disc height, and foraminal height were all measured and recorded both preoperative, postoperative and at follow up. Those with low grade spondylolisthesis of degenerative and lytic types (n=30) were included after excluding patients with high grade listhesis, spondylolisthesis of traumatic and dysplastic aetiologies, previously operated for lumbar pathology, more than one level, retrolisthesis, associated spinal fractures, scoliotic deformities, localised or generalized infections and not willing for the study (n=15). Diabetes mellitus, hypertension and patients with neurologic deficits, were not considered as determining factor in selection of the patients. Those included in study were randomized using computer generated random numbers to Group I – stand alone local bone graft (n=13) and Group II – interbody titanium cage (n=17). These patients were operated by conventional approach with laminectomy of the listhetic vertebra and bilateral facetectomy by either author 1 or author 2. In all patients decompression of central canal, exiting and traversing roots on bilateral sides were done irrespective of the side of the symptoms. Instrumentation was done with posterior pedicle screw through free hand technique of that single motion level with preservation of the cephalad facet. Discectomy and end plate preparation was done from the side of predominant symptoms. In Group I the local corticocancellous chips were designed to large grafts and were inserted into the disc space. In Group II, titanium TLIF cage of appropriate size was inserted along with the morselized local graft after careful retraction of dura and traversing root. In both groups compression of the intervertebral grafts were done and maintained with contoured lordotic rods. These patients were mobilized the next day and were discharged after third day once their drains were removed. They were followed periodically at 2 weeks, 6 weeks, 3 months, 6 months, 12 months interval and whenever patients had any complaints. Patients were allowed to do light work like household activities at 6 weeks, and moderate activities like desk job office works with bending down, squatting at 3 months and were allowed to heavy works like running, manual labour, athletics after 6 months. Functional scores (VAS score, ODI) and radiological parameters (translation, intervertebral disc height, foraminal height) were evaluated pre and post op by author 3. Fusion status was analysed using Bridwell criteria [Table/Fig-1], where the patients were considered fused in Grade I and II while Grade III and IV were considered pseudoarthrosed [9]. CT scan was done to analyse fusion status in doubtful cases of union.
Bridwell criteria for fusion [9].
| Grade I | Fused with remodelling and trabeculae present |
| Grade II | Graft intact, not fully remodelled and incorporated but no lucency present |
| Grade III | Graft intact, potential lucency present at top and bottom of graft |
| Grade IV | Fusion absent with collapse/resorption of graft |
Statistical Analysis
Statistical analysis was done using Student’s t-test, on SPSS 13.0 (SPSS Inc., Chicago, Illinois).
Results
The mean age of the patients in Group I was 46.7 years and in Group II was 43.5 years. The females were predominant in our study with ratio of 13:2. Degenerative type of listhesis was the predominant type and L4-5 was predominant motion level [Table/Fig-2]. All patients were followed up to a minimum of one year, with the mean follow up of 13.07 months (12-17 months) in Group I and 14.17 months (12-19 months) in Group II. VAS score of 8.15 in Group I improved to 1.84 postoperatively (p=0.001), while in Group II a score of 7.61 to 1.53 (p=0.001). ODI score in Group I was 74.30 which improved to 21.23 (p=0.001) and in Group II 71.17 to 22.05 (p=0.001) [Table/Fig-3]. Radiological parameter translation of 0.74 cm in Group I improved to 0.34 cm postoperatively (p=0.0001), while in Group II from 0.68 cm to 0.27 cm (p=0.0001). Intervertebral disc height of 0.92 cm in Group I remained same postoperatively (p=0.06), while in Group II improved from 0.93 cm to 1.06 cm (p=0.03). Foraminal height of 1.62 cm in group I remained same postoperatively (p=0.342), while in Group II improved from 1.42 cm to 1.63 cm (p=0.03). Even though the intervertebral disc height and foraminal height remained the same after surgery in Group 1, there was no significant difference between the preoperative (p=0.880 for intervertebral disc height and p=0.142 for foraminal height) and postoperative measurements (p=0.310 for intervertebral disc height and p=0.135 for foraminal height) of the two groups [Table/Fig-4]. The clinical and radiological results were comparable between the two groups based on statistical analysis. The mean time taken for fusion in Group I was seven months and in Group II was eight months (p>0.05) [Table/Fig-5,6,7,8,9 and 10].
Table depicting the level and type of listhesis.
| Type | Level | Group I | Group II |
|---|
| Degenerative | L4-5 | 9 | 6 |
| L5-S1 | 1 | 1 |
| Lytic | L4-5 | 2 | 4 |
| L5-S1 | 1 | 6 |
| GROUP | Vas Score | p-value | ODI | p-value |
|---|
| Pre | Post | Pre | Post |
|---|
| Group I | 8.15 | 1.84 | 0.001 | 74.30 | 21.23 | 0.001 |
| Group II | 7.61 | 1.53 | 0.001 | 71.17 | 22.05 | 0.001 |
| p-value | 0.196 | 0.147 | | 0.436 | 0.983 | |
| Group | Translation | p-value | intervertebral DiscHeight (cm) | p-value | Foraminal height (cm) | p-value |
|---|
| Pre | Post | Pre | Post | Pre | Post |
|---|
| I | 0.74 | 0.34 | 0.001 | 0.92 | 0.92 | 0.06 | 1.62 | 1.62 | 0.342 |
| II | 0.68 | 0.27 | 0.001 | 0.93 | 1.06 | 0.03 | 1.42 | 1.63 | 0.03 |
| p-value | 0.858 | 0.348 | | 0.880 | 0.310 | | 0.142 | 0.135 | |
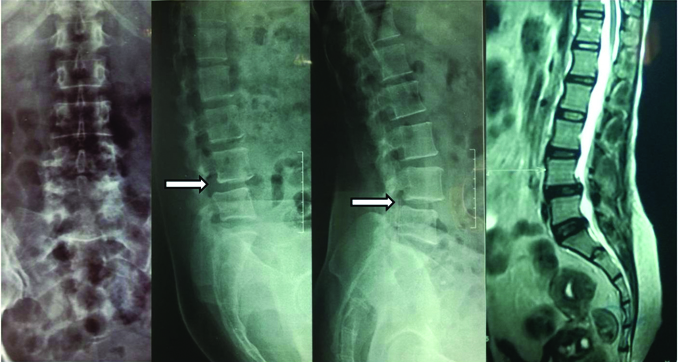
A 45/F with instability back pain and bilateral L5 radiculopathy. Radiograph revealed L4-5 grade I degenerative spondylolisthesis, and well maintained intervertebral disc height; MRI shows the compression of cauda roots by prolapsed disc.
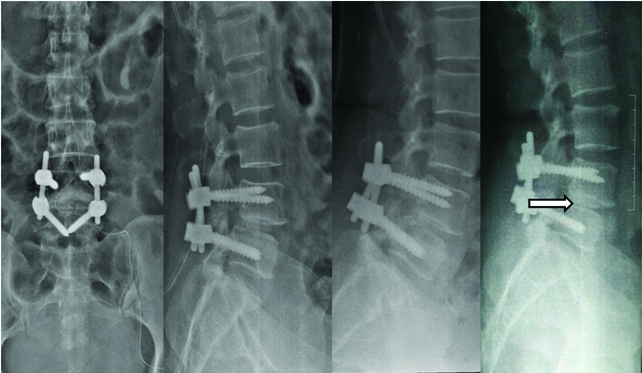
Radiograph done serially at 0, 6, 12 months following interbody fusion with stand alone bonegraft showing Grade II fusion.
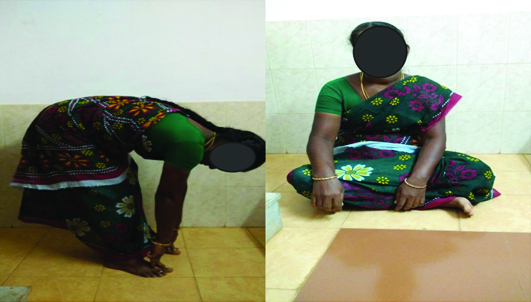
One year follow up, with excellent functional outcome.
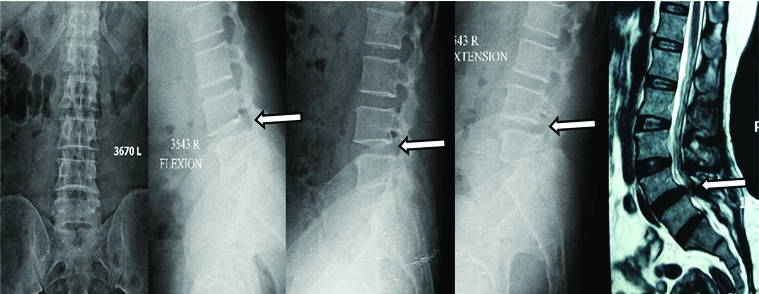
A 49/F low back pain and neurogenic claudication–dynamic x-rays depicting Grade I spondylolisthesis; MRI revealing lumbar canal stenosis secondary to disc prolapse and ligamentum flavum hypertrophy.
Follow up x-rays done at 0, 6 and 12 months of interbody fusion with cage technique showing Grade I fusion.
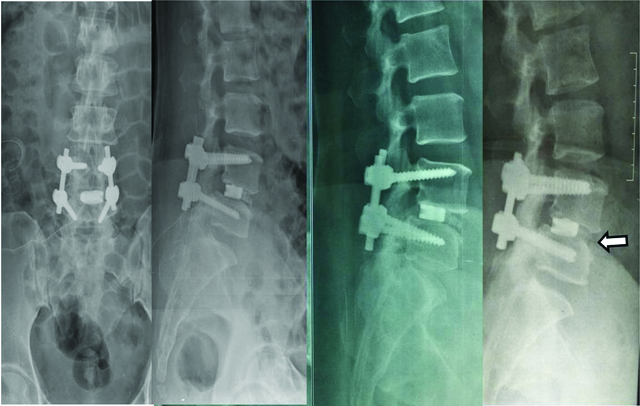
Full functionality at one year final follow up.

One patient in Group I had infection which was managed by debridement, antibiotics for six weeks and another who had transient foot drop secondary to a pedicle breach, found and revised intraoperatively, recovered completely by three months. One patient in Group II had an excessive bleeding secondary to epidural venous varices, and that patient developed pseudoarthrosis eventually because of inadequate end plate preparation. He was advised revision surgery through anterior approach and he is under close follow up. The results revealed no stastically significant difference based on the Mann whitney test and t-test.
Discussion
The techniques of access to the intervertebral disc for interbody fusion have evolved over time of which posterior approach has special advantages. Posterior approach helps in not only decompressing the neural elements [10] but also in instrumenting the tension surface of the lumbar spine with biomechanically stronger pedicle screw and rods [11].
The graft expanders allograft has risk of disease transmission [12], while demineralized bone matrix, artificial bone, rh BMP has risk of heterotopic ossification and cancer. It is also expensive [13].
The fusion obtained is dependent on the graft placed in the interbody region and failure to fuse will eventually lead to implant failure. The time required for fusion in our study does not show any statistical difference in both groups. The time taken for fusion is comparable to other studies and we had only one case of pseudoarthrosis in Group II. The fusion rate for local autogenous graft is 98.3% and iliac graft for 96.3% [6]. The fusion rate with local graft was 72.4% after six months and 100% after 12 months [14]. Hashimoto T et al., reported a fusion rate of 100% at two years after PLIF with local bone mixed with Apatite and Wollastonite-Glass Ceramic (AW-GC) grafted in a single intervertebral space [15]. Nemoto O observed 96% fusion rate in the titanium at 12 months [16].
Interbody cage acts as a spacer to maintain the intervertebral disc height in a collapsed disc space and also adds to stability by providing anterior column support. There was no significant difference in intervertebral disc height and foraminal height of both groups and it is because of low grade listhesis with relatively maintained disc height in all preoperative patients. In only graft group the disc and foraminal height remained same as there was no attempt in increasing the height and it’s not possible to increase with local grafts alone. Global lumbar lordosis is attributed by disc height at all levels which remained unaltered as fusion was performed at single motion level. These results were similar to Patil SS et al., observations [11]. Translatory correction achieved was significant in both groups and it was maintained till the end of follow up.
All patients selected for this study had spinal instability with neurological symptoms which failed to improve with conservative treatment. Hence, the functional results were largely dependent on the neurological decompression and fusion. Indirect decompression by increasing the foraminal height secondary to increase in intervertebral disc height is an important way of decompressing the nerve roots in MIS TLIF [17]. In our study ODI, VAS score improved significantly post surgery and it’s attributed to the direct decompression in open posterior approach. Increasing disc height and hence indirect decompression has minimal role in low grade listhesis operated by conventional open surgeries where direct decompression is more beneficial.
Complete laminectomy and bilateral facetectomy not only decom-pressed the neural elements but also provided ample amount of local grafts for interbody fusion. There was no difference in postoperative mobilisation protocol between the groups. All patients including the bone graft group were mobilised immediately, as the pedicle screws were biomechanically strong to allow mobilization [18].
The limitations of our study is the short follow up because of which the incidence of adjacent segment degeneration could not be studied. We also have not measured the lordosis at various levels but Hu MW et al., [19] have previously demonstrated that local graft alone is sufficient enough to maintain lordosis.
Limitation
The limitations of this study was that groups involved two motion levels L4-5 or L5-S1 which again were not inter comparable. The group size is small and the results of this study have to be validated with large group randomised controlled studies.
Conclusion
The use of standalone local autologous bone graft can provide comparable results functionally and radiologically with that of fusion with cage and bone graft in conventional posterior interbody fusion, single level fusion surgeries, and low grade spondylolisthesis.
[1]. Williams AL, Gornet MF, Burkus JK, CT evaluation of lumbar interbody fusion:current conceptsAJNR Am J Neuroradiol 2005 26:2057-66. [Google Scholar]
[2]. Oliveira L, Marchi L, Coutinho E, Pimenta L, A radiographic assessment of the ability of the extreme lateral interbody fusion procedure to indirectly decompress the neural elementsSpine 2010 35(26 Suppl):S331-37. [Google Scholar]
[3]. Okuyama K, Kido T, Unoki E, Chiba M, PLIF with a titanium cage and excised facet joint bone for degenerative spondylolisthesis--in augmentation with a pedicle screwJ Spinal Disord Tech 2007 20:53-59. [Google Scholar]
[4]. McAfee PC, DeVine JG, Chaput CD, Prybis BG, Fedder IL, Cunningham BW, The indications for interbody fusion cages in the treatment of spondylolisthesis:analysis of 120 casesSpine (Phila Pa 1976) 2005 30:S60-65. [Google Scholar]
[5]. Liu XY, Qiu GX, Weng XS, Yu B, Wang YP, What is the optimum fusion technique for adult spondylolisthesis- PLIF or PLF or PLIF plus PLF?A Meta-analysis from 17 Comparative StudiesSpine (Phila Pa 1976) 2014 39(22):1887-98. [Google Scholar]
[6]. Ito Z, Imagama S, Kanemura T, Hachiya Y, Miura Y, Kamiya M, Bone union rate with autologous iliac bone versus local bone graft in posterior lumbar interbody fusion (PLIF):a multicenter studyEur Spine J 2013 22:1158-63. [Google Scholar]
[7]. Hawker GA, Mian S, Kendzerska T, French M, Measures of adult pain:Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP) Arthritis Care Res (Hoboken) 2011 63(Suppl 11):S240-52. [Google Scholar]
[8]. Vincent JI, Macdermid JC, Grewal R, Sekar VP, Balachandran D, Translation of oswestry disability index into Tamil with cross cultural adaptation and evaluation of reliability and validityOpen Orthop J 2014 8:11-19. [Google Scholar]
[9]. Bridwell KH, Lenke LG, McEnery KW, Baldus C, Blanke K, Anterior fresh frozen structural allografts in the thoracic and lumbar spine. Do they work if combined with posterior fusion and instrumentation in adult patients with kyphosis or anterior column defects?Spine 1995 20(12):1410-181. [Google Scholar]
[10]. Jain AK, Dhammi IK, Prashad B, Simultaneous anterior decompression and posterior instrumentation of the tuberculous spine using an anterolateral extrapleural approachJ Bone Joint Surg Br 2008 90:1477-81. [Google Scholar]
[11]. Patil SS, Rawall S, Nagad P, Shial B, Pawar U, Nene AM, Outcome of single level instrumented posterior lumbar interbody fusion using corticocancellous laminectomy bone chipsIndian J Orthop 2011 45:500-03. [Google Scholar]
[12]. Giannoudis PV, Dinopoulos H, Tsiridis E, Bone substitutes:an updateInjury 2005 36(Suppl 3):S20-27. [Google Scholar]
[13]. Carragee E J, Chu G, Rohatgi R, Hurwitz EL, Weiner BK, Yoon ST, Cancer risk after use of recombinant bone morphogenetic protein-2 for spinal arthrodesisJ Bone Joint Surg Am 2013 95(17):1537-45. [Google Scholar]
[14]. Miura Y, Imagama S, Yoda M, Mitsuguchi H, Kachi H, Is local bone viable as a source of bone graft in posterior lumbar interbody fusion?Spine (Phila Pa 1976) 2003 28:2386-89. [Google Scholar]
[15]. Hashimoto T, Shigenobu K, Kanayama M, Clinical results of single-level posterior lumbar interbody fusion using the Brantigan I/F carbon cage filled with a mixture of local morselized bone and bioactive ceramic granulesSpine (Phila Pa 1976) 2002 27:258-62. [Google Scholar]
[16]. Nemoto O, Asazuma T, Yato Y, Imabayashi H, Yasuoka H, Fujikawa A, Comparison of fusion rates following transforaminal lumbar interbody fusion using polyetheretherketone cages or titanium cages with transpedicular instrumentationEur Spine J 2014 23:2150-55. [Google Scholar]
[17]. Kim MC, Park JU, Kim WC, Lee HS, Chung HT, Kim MW, Can unilateral approach minimally invasive transforaminal lumbar interbody fusion attain indirect contralateral decompression?A preliminary report of 66 MRI analysisEur Spine J 2014 23(5):1144-49. [Google Scholar]
[18]. Chao CK, Hsu CC, Wang JL, Lin J, Increasing bending strength and pullout strength in conical pedicle screws:biomechanical tests and finite element analysesJ Spinal Disord Tech 2008 21:130-38. [Google Scholar]
[19]. Hu MW, Liu ZL, Zhou Y, Chen CL, Yuan X, Posterior lumbar interbody fusion using spinous process and laminaeJ Bone Joint Surg Br 2012 94:373-77. [Google Scholar]