Insulin (Technique) Induced Hypoglycaemia
Adlyne Reena Asirvatham1, Shriraam Mahadevan2, Balasubramaniam Sathish Kumar3, Srinivas Devaganipalli Nrusimha4, Thiagarajan Radhakrishnan Vadivel5
1 Assistant Professor, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai, Tamil Nadu, India.
2 Associate Professor, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai, Tamil Nadu, India.
3 Senior Resident, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai, Tamil Nadu, India.
4 Medical Officer, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai, Tamil Nadu, India.
5 Medical Officer, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai, Tamil Nadu, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Shriraam Mahadevan, Associate Professor, Department of Endocrinology, Diabetes and Metabolism, Sri Ramachandra Medical College, Chennai-600116, Tamil Nadu, India.
E-mail: mshriraam@gmail.com
The most common side effect of insulin therapy is hypoglycaemia apart from weight gain. It occurs commonly due to insulin overdose, faulty injection site, technique and meal-insulin mismatch. In lean individuals even the needle size can be a contributing factor to hypoglycaemia. Here we report a case who presented with recurrent episodes of hypoglycaemia due to a combination of wrong insulin site, technique as well as needle size. On examination, he was found to have spotted dermopathy on his forearms (insulin injection site) which was consistent with intradermal insulin administration. Recently, insulin infusion through intradermal route has been found to reach the systemic circulation faster than even the conventional subcutaneous injection. This case emphasizes that hypoglycaemias can occur due to less common causes. It warrants a good clinical examination and patient education.
Hypoglycaemia, Intradermal insulin, Spotted dermopathy
Case Report
A 58-year-old male with type 2 diabetes mellitus for last 10 years presented with minor but recurrent episodes of hypoglycaemia for the past four months. The episodes were usually characterized by sweating and giddiness that promptly improved upon oral sugar intake. He was on metformin (1000 mg twice daily) and glimepiride (1 mg once daily) previously. In view of poor glycaemic control (HbA1c: 10.5%) he was started on premixed insulin (Regular 30% + NPH 70%) twice daily four months ago after which the hypoglycaemic episodes started. On examination, he was lean with no clinical signs suggestive of insulin resistance (acanthosis/skin tags). While evaluating for the cause of hypoglycaemia, clinical examination showed hyperpigmented spots on the anterior aspect of both forearms [Table/Fig-1]. On further questioning, he revealed that he had been injecting insulin at this site. He was using 6 mm 31 gauge needle (U-40 syringe) for insulin administration and never had pain or itching at the site of injection. Though he followed aseptic precautions, he was using ‘straight in’ no pinch injection technique with acute slant of the insulin syringe. Due to cost constraints, he was reusing the syringe for at least two days (four pricks). In addition to the above errors in insulin administration, he also had meal-insulin mismatch in timing and quantity of food taken. With the above information, a possibility of wrong insulin injection technique induced hypoglycaemia was considered. He was then educated well on diabetes and proper insulin injection technique. His insulin was changed to pen device (same premixed insulin) which invariably had 4 mm needles only and was advised to rotate the sites of injection. On follow up at three months, though the pigmentation did not show much improvement, there were no further episodes of hypoglycaemia and good glycaemic control was achieved.
Discussion
Hypoglycaemia is the most important complication of insulin therapy. It is usually due to insulin overdose, faulty injection site, technique and meal-insulin mismatch [1-3]. Insulin needle size may also play a role in hypoglycaemic episodes if not carefully looked for especially in lean individuals [4]. As our patient was very lean with negligible subcutaneous fat and was erring in injection technique, inadvertent intramuscular administration of insulin was considered as the initial possibility of hypoglycaemia. However, post inflammatory hyperpigmented spots at the injection sites (which usually occur due to hypersensitivity reaction to insulin) alerted us to the possibility of intradermal injections. Intradermal insulin injection causing intradermal bleb that resolved after rectifying insulin injection technique has been previously reported [5]. In a study done in 100 insulin requiring patients, 53 had local complications related to incorrect insulin technique including disfigurement and erratic absorption of insulin [6]. It is usually believed that absorption of insulin is poor with intradermal injection. But, recently it has been demonstrated that intradermal insulin infusion may in fact be absorbed faster through the dermal lymphatic channels and may reach systemic circulation sooner [7,8]. Intradermal aspart insulin had shown a shorter Tmax, higher early and lower late exposure in type 2 diabetes compared to subcutaneous short acting insulin proving faster insulin absorption [9]. We feel that this may also be contributing to hypoglycaemia in our index case. This case emphasizes that careful clinical examination helps to identify rare but easily correctable causes of hypoglycaemia.
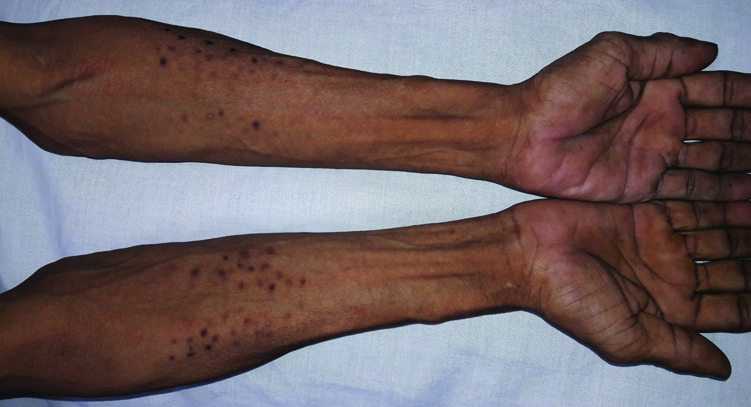
Spotted dermopathy in the anterior aspect of forearm due to intradermal insulin administration.
Conclusion
Hypoglycaemia is the most common and important complication of diabetes treatment. Faulty insulin injection technique could be the cause of hypoglycaemia as well as dermopathy at the local site. This case highlights the simple fact that good clinical examination could very well give a clue even to infrequent causes of hypoglycaemia.
[1]. Trief PM, Cibula D, Rodriguez E, Akel B, Weinstock RS, Incorrect insulin administration: a problem that warrants attentionClinical Diabetes 2016 34(1):25-33. [Google Scholar]
[2]. Geller AI, Shehab N, Lovegrove MC, Kegler SR, Weidenbach KN, Ryan GJ, National estimates of insulin-related hypoglycemia and errors leading to emergency department visits and hospitalizationsJAMA Intern Med 2014 174:678-68. [Google Scholar]
[3]. Peyrot M, Rubin RR, Kruger DF, Travis LB, Correlates of insulin injection omissionDiabetes Care 2010 33:240-45. [Google Scholar]
[4]. Gill HS, Prausnitz MR, Does needle size matter?J Diabetes Sci Technol 2007 1(5):725-29. [Google Scholar]
[5]. Chakraborthy PP, Biswas SN, Patra S, Faulty injection technique: a preventable but often overlooked factor in insulin allergyDiabetes Ther 2016 7(1):163-67. [Google Scholar]
[6]. Seyoum B, Abdulkadir J, Systematic inspection of insulin injection sites for local complications related to incorrect insulin techniqueTropical Doctor 1996 26:159-61. [Google Scholar]
[7]. Rini CJ, McVey E, Sutter D, Keith S, Kurth HJ, Nosek L, Intradermal insulin infusion achieves faster insulin action than subcutaneous infusion for 3-day wearDrug Deliv Transl Res 2015 5(4):332-45. [Google Scholar]
[8]. Pettis RJ, Harvey AJ, Microneedle delivery: clinical studies and emerging medical applicationsTher Deliv 2012 3(3):357-71. [Google Scholar]
[9]. Kochba EE, Levin YY, Raz II, Cahn AA, Improved insulin pharmacokinetics using a novel microneedle device for intradermal delivery in patients with type 2 diabetesDiabetes Technology & Therapeutics 2016 18(9):525-31. [Google Scholar]