Complicated Hydatid Cyst of Ulna- A Rare Case Report
I V Reddy1, A H Ashwin Kumar2, Bheemsingh Samorekar3, B Amar Babu4, Anil Kumar Mettu5
1 Consultant and Head, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad, Telangana State, India.
2 Consultant, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad, Telangana State, India.
3 Resident, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad, Telangana State, India.
4 Resident, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad, Telangana State, India.
5 Resident, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad, Telangana State, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Bheemsingh Samorekar, DNB Resident, Department of Orthopaedics, Krishna Institute of Medical Sciences Ltd., Secunderabad-500003, Telangana State, India.
E-mail: bheemsinghvs@gmail.com
Although hydatidosis is not uncommon in tropical countries, still bony involvement is comparatively rare. The aetiological agent is Echinococcus granulosus, a parasite belonging to cestode group with dog as definitive host and man as incidental host. We present a case of young male, who consulted us for painless, multiple swellings in his right forearm of three years duration, with restricted wrist movements. On examination multiple non tender, soft to firm swellings were noted with restricted terminal pronation. X-rays and MRI of right forearm showed multiple lobulated soft tissue components in intermuscular, subcutaneous and cutaneous planes and the main ulnar intramedullary cystic mass extending out as extramedullary cyst through proximal ulnar cortical breach. Proximal 2/3rd radius were also affected. On surgical exploration of forearm, cystic swelling measuring 8 × 6 × 5 cm sprouting out from proximal ulnar erosion was found. Intraoperative histopathology showed multiple endocysts suggestive of hydatid cyst; hence with protective measures wound closed back in layers and six weeks of oral albendazole 400 mg daily was given.
At six weeks follow-up wrist movements improved but serous discharge persisted at drain site. Patient is still under regular follow-up.
Thus, a differential diagnosis of bony hydatidosis should be considered while evaluating soft tissue swellings.
Albendazole, Bone, Echinococcus granulosus, Endocyst
Case Report
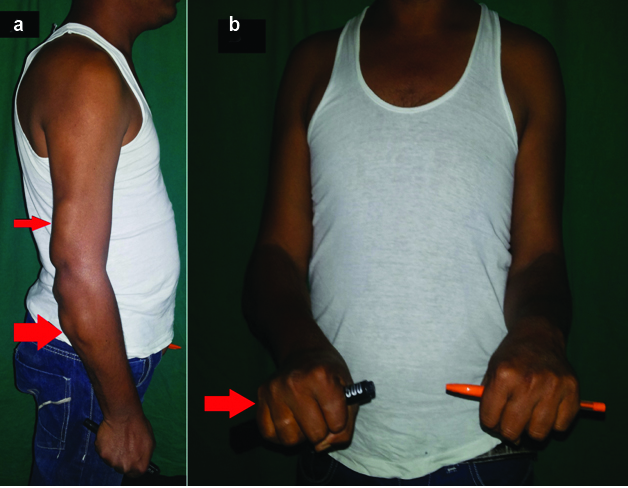
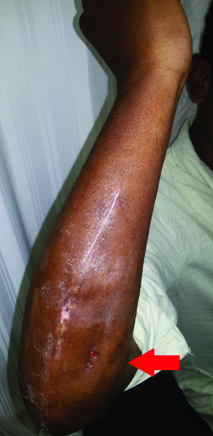
A 30-year-old male, right handed skilled labourer, presented to us with painless, multiple swellings on right forearm since three years with restricted wrist movements affecting his fine work job. He didn’t give history of involvement with cattle; sheep etc., but consumes non-vegetarian food. On examination of forearm there were multiple swellings, which were non tender and soft to firm in consistency. The largest was measuring about 8 × 6 × 5 cm, located posteromedially below elbow joint and was restricting terminal pronation [Table/Fig-1].
a) Right proximal forearm swellings posteriorly and in distal arm posteriorly (arrow); b) Terminal pronation (arrow) restricted.
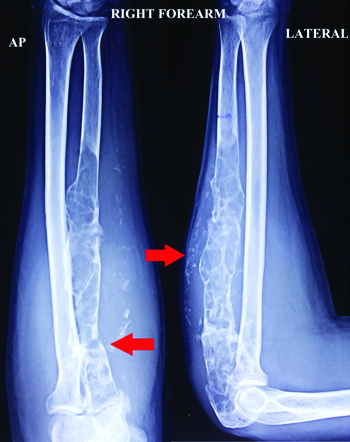
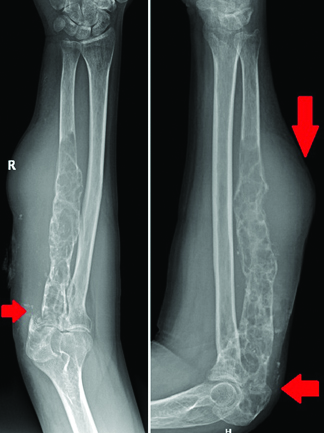
X-rays of right forearm showed multiple cystic areas, extensive lytic lesions with erosion of bony cortex of proximal 2/3rd ulna with overall loss in bone structure. There was breach in the cortex at proximal ulna due to pathological undisplaced fracture and proximal radius also showing similar features. Soft tissues surrounding ulna, showed calcinosis extending upto wrist in subcutaneous and cutaneous planes [Table/Fig-2]. MRI showed multiple lobulated soft tissue components in intermuscular, subcutaneous and cutaneous planes extending upto wrist. The main mass of expansive lytic lesion was in proximal ulna extending from proximal articular end down into the midshaft for approximate length of 16 cm with a sharp well defined distal margin. The affected part of ulna was expanded, with grossly thinned out cortex and areas of cortical break through which the intraosseous lesion extended out extraosseously [Table/Fig-3]. Proximal radius also showed similar changes with a provisional diagnosis of haemangiomatosis by the radiologist.
X-Ray right forearm showing expansile lytic lesion of ulna with thinned out cortex (arrow) and pathological fracture proximally with similar features (arrow) in proximal radius and calcinosis of subcutaneous tissue.
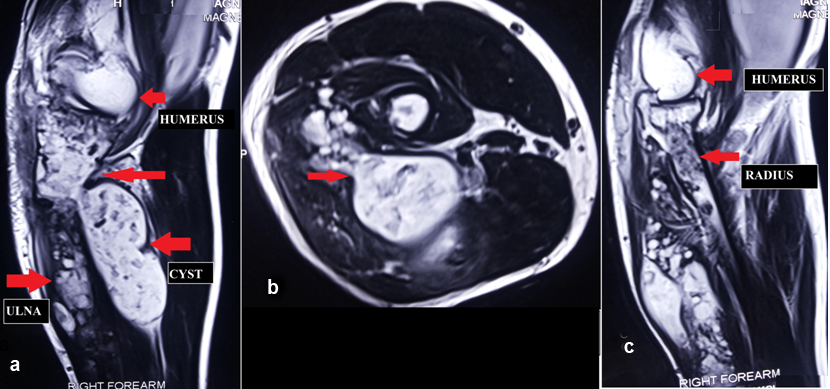
MRI right forearm, T1W and T2W images showing hypointense bony and soft tissue expansile, lobulated lesions (arrow) with the main intramedullary proximal ulnar mass extending outside as extramedullary through the proximal cortical breach.
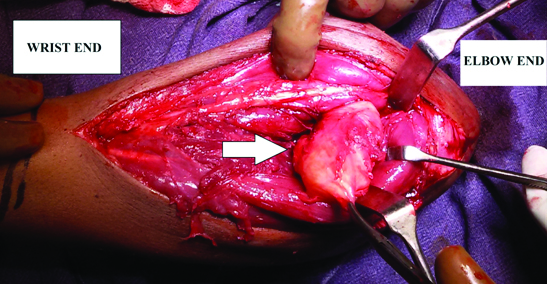
Routine blood examination with ESR and eosinophil count was normal. On surgical exploration of forearm, cystic swelling measuring 8 × 6 × 5 cm sprouting out from proximal ulnar erosion [Table/Fig-4] was found along with another cystic swelling of similar size at distal arm posteriorly without bony attachment. Intraoperative findings showing non tumour features, the ulnar medullary canal was curetted out to remove the remaining cysts with protective measures and wound closed back in layers. No hypertonic saline was used as we were not expecting hydatidosis at that instinct.
Intraoperative images showing ulnar intramedullary hydatid cyst extending out through proximal ulnar pathological fracture as extramedullary soft tissue cyst.
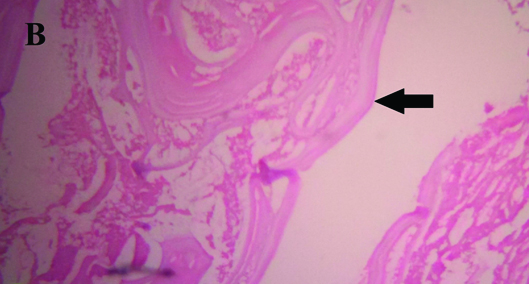
Histopathology showed thick, fibro-collagenous cyst wall with proliferating capillaries and chronic inflammatory reaction with lymphocytes, plasma cells and eosinophils infiltrating it. Inner surface of endocyst was lined by foreign body, giant cells and histiocytes. Cyst cavity contained a lamellated acellular membrane of parasitic cyst along with acidophilic granular material suggestive of hydatid cyst [Table/Fig-5].
Histopathology showing fibro-collagenous acellular lamellated cystic wall (arrow) along with endocysts (B- H&E stain, 40x magnification).
Hence six weeks of oral albendazole 400 mg daily was given to prevent recurrence due to surgical spilling of the schizonts. Elbow and wrist range of motion exercises were advised and weight lifting was avoided to prevent pathological fracture. On six weeks follow up patients forearm surgical scar was healthy but persisting discharge from drain site and pronation improved comparatively [Table/Fig-6]. Blood routines including ESR at follow up were within normal range. Follow up x-ray right forearm showed soft tissue swelling at the discharging patent drain site with same old ulnar changes [Table/Fig-7]. Patient is still under regular follow up for further management.
Post-op six weeks follow-up showing healed surgical scar but persisting discharge from drain site.
Follow-up x-ray right forearm showing soft tissue swelling with old ulnar changes. (left to right)
Discussion
Hydatidosis or echinococcosis is caused by the cestode Echinococcus in its larval stage. It is a parasite usually found in cattle or sheep rearing population. Dog is the definitive host and man an intermediate host, hence is also called “dog tapeworm” [1]. Four species of Echinococcus are known of which E. granulosus causes the typical cystic echinococcosis and E. multilocularis causes alveolar echinococcosis. The others are rarely seen in humans and are E. vogeli which causes polycystic echinococcosis and E. oligarthus [2]. Hydatidosis is characterized by a slow growing cyst, usually seen in visceral organs likely – liver, spleen, lung, etc. It is a common disease in sheep and mostly seen in areas of Australia, Eastern Europe, South America and South Asia. Although eradicated in most of the parts of the world, it still remains a serious endemic health problem in certain developing countries. Highest prevalence in India is reported from Andhra Pradesh and Tamilnadu [2]. The presence of raised specific antibody is done by various techniques such as indirect haemagglutination or latex agglutination, complement fixation, immunoelectrophoresis, indirect fluorescent antibody tests, Bentonite-Flocculation Test (BFT) [3], western blot, Enzyme Linked Immuno Sorbent Assay (ELISA), Enzyme-Linked Immune Electro Diffusion Assay (ELIEDA), immunoblotting etc. X-rays, Ultrasonography (USG), CT and MRI are non invasive diagnostic aids [4]. Treatment involves excision of the cyst along with a six weeks course of oral albendazole to prevent surgical spillage growth of the organism in soft tissue [5].
In today’s world, due to increased health consciousness among general population and well developed medical infrastructure for diagnosis and available chemotherapeutic agents for echinococcosis like albendazole, mebendazole, praziquantel etc., the incidence of hydatid cyst involving bone is very less. As per literature, the most common sites of echinococcosis are the liver (50%–70%), lung (20%), and spleen (5%–8%). The kidneys, brain, bone, spinal cord, and heart are rarely involved with an average incidence of 1.5% in bone [6]. Sixty percent of all bony hydatid disease occurs in the spine, pelvis and hip joint. Almost 28% of cases are found in long bones like femur, tibia and humerus and 8% in the ribs and scapula. Isolated infections occur in the calvaria and phalanges [2,7]. Bony hydatid cysts are always primary and the larva reaches the skeletal site via a systemic artery [8]. The significance of the case reported here is the unusual spread of hydatidosis to the both bones of forearm along with surrounding soft tissue, without involving the liver, lungs, and spleen. The large dissemination of parasites might have resulted from an accidental rupture of the primary focus from ulna due to proximal end pathological fracture with the consequent release and spread of scolices. The absence of liver or lung involvement suggests that spreading did not occur via the blood vessels. As per Iuliano L et al., parasites possibly might have disseminated via the lymphatics [9].
The hydatid larva develops very slowly within the medullary part of bone and usually manifests itself in adults rather than in children. In bone, the parasite is not able to follow its usual mode of development because of the resistance of tissue [10]. The bony tissues show a minimal response, and no adventitial wall forms as in other body parts. Microvesicles are produced by exogenous budding and spread throughout the spongiosa of the involving bone to create a lesion which initially molds itself to the rigid bony confines. The hydatid cyst then develops multiple exogenous daughter cysts in the absence of any adventitial pericyst, which insinuate themselves between the bony trabeculae, destroying them. The end result being extensive destruction of the medullary bone by multivesicular cyst [6].
The differential diagnosis of bone hydatidosis includes tuberculosis, chondrosarcoma, malignant fibrous histiocytoma, myeloma, metastatic disease, giant-cell tumour, aneurysmal bone cyst plasmacytoma, a simple bone cyst, brown tumour of hyperparathyroidism, chondromyxoid fibroma [5,7].
Conclusion
Echinococcosis though rare in bones, a differential diagnosis for swellings around bony structures should be kept in mind especially in developing countries where hydatid cyst is endemic. The diagnosis has to be made by clinical, serological and radiological tests correlation. During surgical excision of hydatid cyst, chances of anaphylactic reactions due to spillage of cystic fluid may be encountered; hence prior prophylactic measures to tackle the situation have to be done. Oral albendazole course with or without praziquantel has to be given postoperative to prevent recurrence.
[1]. Salama AA, Othman AA, Zayed HA, Cystic echinococcosis in the middle region of the Nile Delta, Egypt: Clinical and radiological characteristicsEgypt J Radiol Nucl Med 2014 45(3):641-49. [Google Scholar]
[2]. Khader Faheem N, Nusrath N, Syama Sundara Rao B, Raja Ram G, Sushma C, Subramanyam Y, The scenario of Hydatid cyst disease in epidemic areas of Andhra Pradesh – evaluation and analysisInt J Res Dev Health 2013 1:120-28. [Google Scholar]
[3]. Kagan IG, A review of serological tests for the diagnosis of hydatid diseaseBulletin of the World Health Organization 1968 39(1):25-37. [Google Scholar]
[4]. Sbihi Y, Janssen D, Osuna A, Serologic recognition of hydatid cyst antigens using different purification methodsDiagn Microbiol Infect Dis 1996 24:205-11. [Google Scholar]
[5]. Sk M, Sg S, Hydatid cyst of radial boneJ Nepal Med Assoc 2009 48(4):321-23. [Google Scholar]
[6]. Medicine T, Resource C. Tropical Medicine Central Resource http://www.isradiology.org/tropical_deseases/tmcr/chapter3/references.htm. 2015;569-75 [Google Scholar]
[7]. Fotoohi S, Hashemi Tabar GR, Borji H, Serodiagnosis of human hydatidosis with an ELISA developed based on antigens derived from sheep hydatid cysts and comparison with a commercial human ELISA kitAsian Pac J Trop Med 2013 6(9):723-27. [Google Scholar]
[8]. Oshi NJ, Artinez AHE, Azquez RSE, Primary sacral hydatid cystA case report. Acta Orthop Belg 2007 73(5):674-77. [Google Scholar]
[9]. Iuliano L, Gurgo A, Polettini E, Gualdi G, De Marzio P, Musculoskeletal and adipose tissue hydatidosis based on the iatrogenic spreading of cystic fluid during surgery: report of a caseSurg Today 2000 30(10):947-49. [Google Scholar]
[10]. Arti HR, Darani HY, Fibular Hydatid cystIndian Journal of Orthopaedics 2007 41(3):2-3. [Google Scholar]