Rapid growth of Emergency Department (ED) visits is a common problem in most countries [1–3]. Governments are forced to outcome larger healthcare invoice than ever, and this problem nearly grows into international crisis. Past decade statistics showed increased number of ED visits at about twice the rate of population increase in western countries [4,5], and stated that nearly whole population visit ED within a year in East and Middle East [3,6]. Patients returning to the ED shortly after the first admission make a substantial contribution to the crowding of EDs. These patients not only obstruct hospitals, but they are also important indicators of quality and access to health care, because the number of early revisits to ED might indicate failure to give a proper assessment, treatment, or follow up instructions [7]. Considering this, the problem is even more important if the source of the hitch indicates a tertiary care center.
Literature is rich for studies investigating six months, 30 days and three to seven days ED returns [3,7,8]. These time frames are used to indicate several deficiencies in the healthcare system; six months and 30 days ED return can be caused either by medical errors, mismanagement, or unexpected reasons, and tend to raise healthcare utilization issues. Short term ED revisits, three to seven days, could be due to the poor quality of service, possible errors, or adverse events. Risk assessment studies can allow high risk patient identification who might require personalized local care and/or specialty, and some targeted interventions [9,10].
Here we present a study investigating even shorter term revisit to ED; we studied the first 24 hours after discharge from ED. The reason why we considered such a concentrated time was to investigate urgent revisits that possibly represent serious deficiency of emergency health care.
With this study, we aimed to audit the return visit chart of patients in a tertiary care center ED that gives emergency care for children. We objected to recognize characteristic statistics and describe the rate of children who returned to the Paediatric ED (PED) in order to give contribution to literature and to suggest solutions on this topic.
Materials and Methods
We retrospectively reviewed all records of patients visiting our PED in Duzce Medical School Hospital during the period between July 01, 2010 to June 30, 2016. PED of the hospital does not have a trauma follow up unit, so we provide health care service to patients without any traumatic injury. The study was carried out with the approval of the responsible Ethics Committee in accordance with National Law and the Helsinki Declaration from 1975 (in its current revised form).
All patients younger than 19 years who were registered in the PED were included in the database. We collected data on the bases of time of day of the first and return visit, month, year, and age. Time of visit was determined as the time of registration in the ED. Furthermore, we examined the records to determine if the patient had presented to the ED preceding their current visit. Patients were considered to be in the return visits group if they had a return visit to the ED within 24 hours of their previous visit.
We excluded patients who were admitted with traumatic injuries and those who were admitted with complaints different from the ones in the initial admission to PED. We also excluded visits if they were the third or fourth return to the ED in 24 hours, because they were associated with a patient who had already returned and was included in the study, so that we avoid repetitive inclusion of a patient.
Statistical Analysis
Six-year data were collected from the hospital computerized record system. We calculated the rate of return visits (number of return visits within 24 hours divided by the total number of visits). We then compared the characteristics of patients in the return visit group with those who did not return. Data was analysed with statistical software SPSS 17.0, p-value below 0.05 were considered statistically significant. Categorical variables were expressed in numbers and percentages. Continuous variables were presented as mean (±standard deviation) with the range and the chi-square tests were used to evaluate categorical variables used in the study.
Results
Return rate and age: There were a total of 111219 visits to the PED during the six year study period. A total of 1994 of these (1.79%) returned to PED within 24 hours. A great number of the patients who returned (45%, n= 901) were children younger than two-year-old, and the younger the child, the higher the likelihood of returning was detected [Table/Fig-1]. Infants (<one year of age) constituted 14.6% (n=16216) of our study population, and 2.85% (n=462) of the children who returned to PED within 24 hours. Preschool children (3-6-year-old) represented moderate odds of returning (n=459), and the minimal likelihood of returning was in young adult group (15-18 years of age), was 4.1% (n=82) of the children who revisited PED within 24 hours.
Number and age distribution of patients admitted and readmitted to Paediatric Emergency Department between July 01, 2010 to June 30, 2016.
| Distribution of patient numbers and percentages with regard to the age |
|---|
| Age (year) | Total (n=) | Revisits (n) | % |
|---|
| 0 | 16216 | 462 | 2.85 |
| 1 | 19572 | 439 | 2.24 |
| 2 | 13233 | 267 | 2.02 |
| 3 | 9904 | 173 | 1.75 |
| 4 | 8001 | 129 | 1.61 |
| 5 | 7058 | 84 | 1.19 |
| 6 | 5842 | 73 | 1.25 |
| 7 | 4665 | 60 | 1.29 |
| 8 | 3704 | 48 | 1.30 |
| 9 | 3141 | 37 | 1.18 |
| 10 | 2745 | 40 | 1.46 |
| 11 | 2404 | 26 | 1.08 |
| 12 | 2267 | 25 | 1.10 |
| 13 | 2090 | 25 | 1.20 |
| 14 | 2145 | 24 | 1.12 |
| 15 | 2156 | 25 | 1.16 |
| 16 | 2303 | 22 | 0.96 |
| 17 | 2623 | 24 | 0.91 |
| 18 | 1150 | 11 | 0.96 |
| Total | 111219 | 1994 | 1.79 |
Time of revisit: We investigated the revisits into three groups: immediate (within 0-8 hours after discharge), early (within 9-16 hours), and late revisits (within 17-24 hours). 90 (4.5%), 627 (31.4%), and 1277 (64%) patients were readmitted to PED respectively within 24 hours after first discharge; the mean time of revisit was 17.8 hours after first discharge [Table/Fig-2].
Distribution of the patients with regard to time of readmission after first discharge.
| Number of patients |
|---|
| Age(years) | 0-8 hours(n-%) | 9-16 hours(n-%) | 17-24 hours(n-%) | mean time (hours) |
|---|
| 0 | 16 | 3.46 | 129 | 27.92 | 317 | 68.62 | 18.51 |
| 1 | 23 | 5.24 | 136 | 30.98 | 280 | 63.78 | 17.68 |
| 2 | 11 | 4.12 | 85 | 31.84 | 171 | 64.04 | 17.73 |
| 3 | 13 | 7.51 | 61 | 35.26 | 99 | 57.23 | 17.10 |
| 4 | 2 | 1.55 | 36 | 27.91 | 91 | 70.54 | 18.55 |
| 5 | 2 | 2.38 | 31 | 36.90 | 51 | 60.72 | 17.83 |
| 6 | 7 | 9.59 | 29 | 39.73 | 37 | 50.68 | 16.52 |
| 7 | 2 | 3.33 | 20 | 33.33 | 38 | 63.33 | 17.50 |
| 8 | 2 | 4.17 | 14 | 29.17 | 32 | 66.66 | 18.02 |
| 9 | 0 | 0 | 11 | 29.73 | 26 | 70.27 | 18.46 |
| 10 | 0 | 0 | 12 | 30.00 | 28 | 70.00 | 18.80 |
| 11 | 0 | 0 | 8 | 30.77 | 18 | 69.23 | 19.04 |
| 12 | 0 | 0 | 8 | 32.00 | 17 | 68.00 | 17.76 |
| 13 | 0 | 0 | 7 | 28.00 | 18 | 72.00 | 19.04 |
| 14 | 2 | 8.33 | 9 | 37.50 | 13 | 54.17 | 16.04 |
| 15 | 5 | 20.00 | 10 | 40.00 | 10 | 40.00 | 14.12 |
| 16 | 0 | 0 | 8 | 36.36 | 14 | 63.64 | 17.95 |
| 17 | 5 | 20.83 | 7 | 29.17 | 12 | 50.00 | 15.63 |
| 18 | 0 | 0 | 6 | 54.55 | 5 | 45.45 | 17.00 |
| 90 | 4.51 | 627 | 31.44 | 1277 | 64.04 | 17.84 |
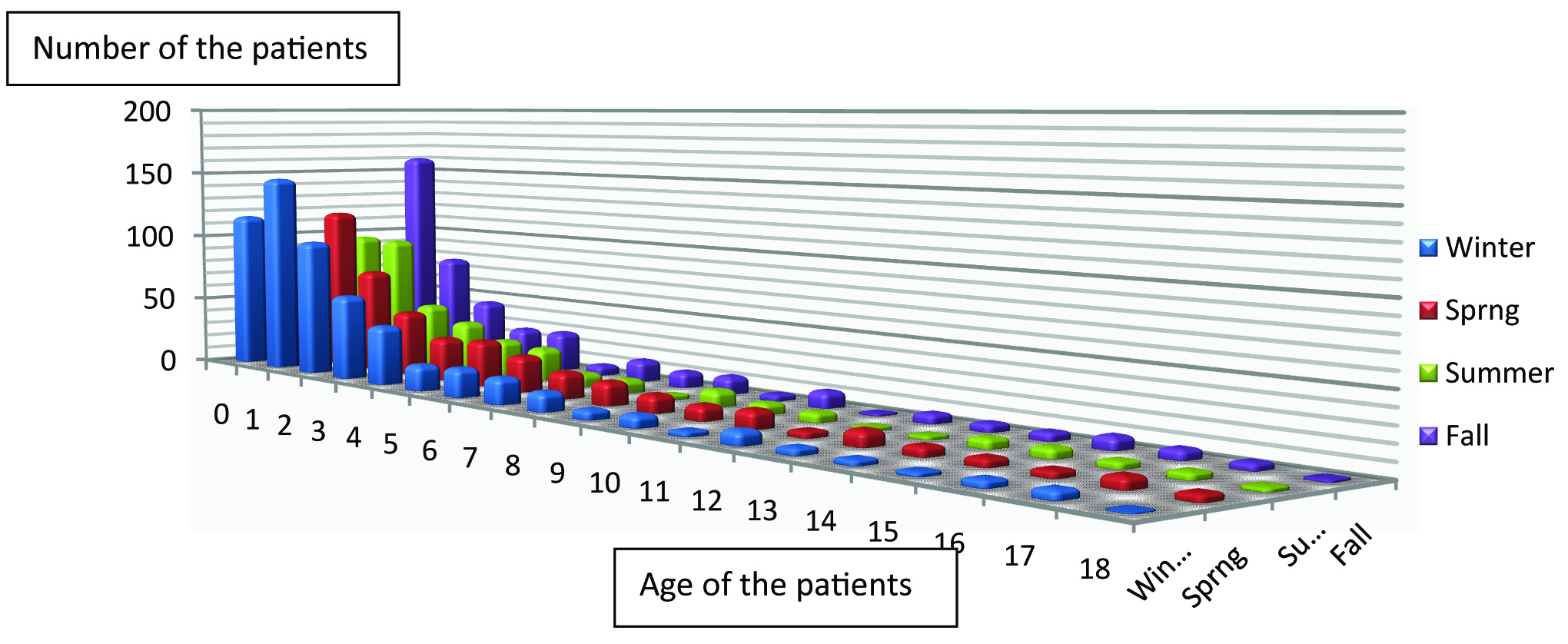
Season and the year: We found some minor, but not significant seasonal difference among same age groups (p>0.05) [Table/Fig-3], though, again the younger the child the higher was the likelihood of returning to the ED.
Seasonal distribution of patients readmitting to Paediatric Emergency Department.
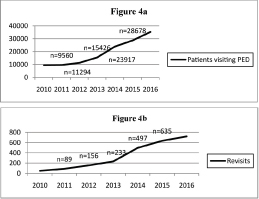
Six year investigation of PED visits and revisits definitely pictured us that emergency departments get more crowded through years; patients’ number admitting to PED was significantly higher at the end of the study than in the beginning (p<0.05). This analysis was also true for revisit patients; numbers of revisits were 89 (0.9%), 156 (1.38%), 233 (1.5%), 497 (2.14%), and 635 (2.2%) respectively in 2011 to 2015 [Table/Fig-4a,b].
Number of patients: (a) visiting; and (b) revisiting Paediatric Emergency Department between July, 2010 to June, 2016.
Discussion
Each return visit to ED of the patient is associated with various deficiencies either of hospital or health providers. In order to investigate them we conducted a six year experience data with children returning to a tertiary care PED in Duzce, Turkey. About 2% of our patients readmitted to PED within 24 hours. As far as we could find, it was one of the lowest ratio of revisits described in the literature [10,11]. Some urban hospital data and reports of tertiary care hospital ED declared return visits as 4-7% of total ED visits [10,12,13]. Nevertheless it is clear that return visits within 24 hours of discharge are not a desirable outcome of an ED. They may contribute to overcrowding of the ED and could serve as an indicator of the quality of care in the ED [10].
Return rate and age: Studies report us with different return rates for adult and paediatric populations; 0.2% - 3.4% for adults and 3.3% to 13.4% for children, respectively [3,8,10,11,14]. It is difficult to compare these studies with ours because of variations of both study design and health care systems of the countries they were conducted in. Nevertheless, the ratio of revisits under 2% (1.79% exactly) is one of the lowest described in literature for PEDs. This may be explained with time frame that we had chosen for the study; many studies considered the return visit to be within 48 or 72 hours. In our study we preferred to investigate return visits on the following day after first admission. The question of return visits to the ED has been carefully studied in malpractice law on emergency medicine [15,16].
Age was the strongest effect on the rate of returning to the PED within 24 hours after discharge; the younger the patient was, the higher the odds of returning, particularly in 0-2 year age group. These results were quite similar to previous reports [7,17,18] and are not surprising because young children have less adequate communication skills and may not be able to express their discomfort. Again, parents of young children tend to return to the ED more than experienced parents. This results correlates to some reports from literature regarding young parents that are less experienced regarding childhood illnesses and are more anxious [18–20]. Physicians should pay more attention towards giving recommendations to these patients, in order to reduce anxiety and their coming back.
Time of revisit: Even though most of early revisits were detected at 17-24 hours after initial admission, revisits even immediately after discharge (within 0-8 hours) were reported. This is even crucial because early revisits are highly connected with high mortality and morbidity risk of the patients [1,2].
Season and the year: In recent years, the number of initial ED visits has increased in many countries [1,3], and this is no different in our country [6] nor in our hospital; in our study total number of PED admissions increased about two to three folds during the last six years. This increase is similar to the increase in ED utilization in most countries [21]. We documented similar increase among patients, who revisited our PED, but with a significantly higher elevation rate; about six to seven folds. Studies analysing revisits to PEDs report increase in number of readmission to PED between two to six folds [18,20,22].
In the analysis of our study, families were somewhat less (not significantly) likely to return to the ED during summer and fall, compared with winter and spring. This is similar with number of studies on this subject [10,18], and may be explained with correlated increase in total ED admissions during the winter season [10,18]. Based on these information physicians should be alert about increasing risk of returning patients during winter.
Limitation
This study was based on patients’ data collected from hospital database, thus the weakness of our study was inability to accurately assess the details of the patient-physician interaction, especially with respect to discharge instructions, that limits analysis of a potentially important factor leading to revisits to PED.
Conclusion
Considering the importance of emergency care, more proper and strategic assessment and treatment for patients determining emergency care should be provided. Strategies on emergency triage systems should be considered. So, further studies should be conducted to explain the reasons for returning to ED, and to find possible solutions are essential.