Total Laparoscopic Hysterectomy (TLH) represents one of the most performed gynaecological procedures nowadays. The closure of the vaginal cuff is the most diffucult part of TLH because of the difficulty of laparoscopic suturing techniques. Our aim was to evaluate the efficacy and safety of vaginal cuff closure by vaginal route on patients submitted to TLH. During the period between January 2013 to December 2015 total number of 64 laparoscopic hysterectomy were performed in our clinic. TLH and vaginal vault closure was performed as described by Ghezzi for all patients. The length of cuff closure time and the frequency of vaginal cuff-related complications were measured. Mean age was 48.1 (38-71) years, mean parity was 2.6 (1-9). Most ranked indications for hysterectomy were abnormal uterine bleeding and symptomatic leiomyoma. Average cuff closure time was 6 (2-17) minute. In average 24 (2-36) month follow-up there were no vaginal vault dehiscence. Transvaginal vaginal cuff closure seems to be safe, easy and effective for total vaginal hysterectomy. Using vaginal route can significantly reduce the length of closure time. This technique has comparable complication rates with endoscopic suturing techniques.
Introduction
Nowadays the use of minimally invasive techniques for hysterectomy, which is the most performed gynaecological procedure, is being increasingly adopted. Vaginal hysterectomy is recommended method for hysterectomy for all patients. If vaginal hysterectomy is inappropriate, minimal invasive surgical techniques, like laparoscopic or robotic surgery is recently being performed in various centers [1]. During the last 20 years TLH implementation rate has increased and TLH was accounted for 9.9% of all hysterectomies in 1997 and 11.8 % in 2003 [2].
The final step of TLH is suturing vaginal cuff. According to surgeon’s preference several techniques and sutures are available. Laparoscopic suturing with intracorporeal or extracorporeal techniques, interrupted or continuous suturing and transvaginal cuff closure can be performed. The closure of the vaginal cuff is the most difficult part of TLH because of the difficulty of laparoscopic suturing techniques. Requirement of advanced surgical skills, long learning curve and time-consuming process are important disadvantages of operation. In a questionnaire study, surgeons declared that they are performing TLH less than abdominal or vaginal hysterectomy because of technical difficulties associated with TLH [3].
Although vaginal cuff dehiscence is a rare complication of hysterectomy; intestinal evisceration, peritonitis, intestinal injury and sepsis are serious complications associated to dehiscence [4]. There are studies reporting that, the rate of cuff dehiscence is higher after laparoscopic and robotic hysterectomy than after vaginal and abdominal hysterectomies [5–9]. The reasons for high cuff dehiscence rate after endoscopic surgery are reported as; inserting sutures too close to surgical area (<1 cm) due to misleading effect of laparoscopic magnification, failure to close full-thickness or non-compliant laparoscopic suture techniques [4]. Using barbed-delayed sutures and double thickness closing or using automatic suture devices are recommended techniques to reduce cuff dehiscence [10,11].
The aim of present case series was to investigate the effectiveness, convenience and reliability of cuff closure technique by vaginal route.
Case Series
The current retrospective cohort study was conducted at İzmir Katip Çelebi University, Atatürk Research and Training Hospital, Turkey, between January 2013 and December 2015. During this time period, total of 64 TLH cases were performed in our clinic. Informed consent was taken from all patients before surgery. Patients who underwent TLH for benign or premalignant-malignant indications were enrolled. Patients who could not tolerate long time Trendelenburg position or pneumoperitoneum were excluded from study. All operations were performed by same experienced laparoscopic surgeon (SK).
In 30 cases, TLH was performed by traditional laparoscopic hysterectomy and in 34 cases by mini-laparoscopic hysterectomy. A 10 mm laparoscope inserted through 12 mm port and three 5 mm assistant ports are used in conventional laparoscopy group. In mini-laparoscopy group, 5 mm laparoscope inserted through 5 mm port and two or three assistant ports were used. Laparoscopy is performed under general anaesthesia and in low-lithotomy position. Bladder is catheterized before surgery for all patients.
After pneumoperitoneum was ensured by Verres needle, 0 degrees, 5 mm or 10 mm laparoscope (Karl Storz, Tuttlingen, Germany) was applied through umbilical port to abdomen. Ancillary trocars were applied under direct visualization. One ancillary trocar was inserted from 3 cm above the symphysis at midline in all cases. Other ancillary trocars were applied to the lateral of medial umbilical ligaments in both sides. Most of operations were completed with bipolar coagulation and scissors. Consecutive to electrocoagulation and cutting of ovarian and/or infundibulo-pelvic ligaments, the broad ligament was opened up to the uterovesical fold that was then incised with caudal reflection of the bladder. Afterwards, the uterine arteries, the cardinal ligaments, and the uterosacral ligaments were coagulated and transected. Circular colpotomy was performed by monopolar energy with the asistance of Klermont-Ferrand (Germany – KARL STORZ GmbH & Co., KG, Germany) or RUMI (Cooper Surgical, USA) uterine manipulators. Uterus and bilateral adnexa were removed by vaginal route. Vaginal cuff was sutured continuously through vagina with 26 mm half-circle HR26 needled late absorbed sutures (No.1 Vicryl; Ethicon, Livingston, UK) [Table/Fig-1,2].
Vaginal wall preparation before cuff closure.
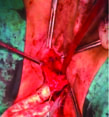
Cuff closure by vaginal route.

Patients were discharged on postoperative first or second day. Patients were informed about avoiding sexual intercourse for six weeks and to visit the clinic in case of vaginal bleeding, discharge, pain or fever. All patients were evaluted in postoperative three to four weeks and sixth month, then followed annually.
The mean age was 48.1 (38-71) years, mean parity was 2.6 (1-9). Most ranked indications for hysterectomy were abnormal uterine bleeding and symptomatic leiomyoma. Performed concomitant procedures were: salpingo-oophorectomy for 15 cases, Mccall culdoplasty for 10 cases, transobturator midurethral sling placement for seven cases, omentectomy for three cases and ovarian cystectomy for two cases. TLH was performed for eight patients of total 64 patients due to premalignant and malignant lesions. Conversion to laparotomy was required for two patients (3.1%) [Table/Fig-3]. Both of them were due to technical problems. Mean cuff closure time was six minutes (2-17). Bladder injury developed in one case (1.5%). Cuff haematoma and cuff cellulitis developed in two cases. Mean follow up time was 24 (2-36) months. There was no cuff dehiscence.
Patients’ demographics, and indications of surgery.
| Demographic Characteristics and Indication | (n=64) |
|---|
| Characteristics |
| Age (years) | 48.1±7.2 |
| Gravity | 3.4±1.7 |
| Parity | 2.6±1.4 |
| Premenopausal n (%) | 26 (40.6%) |
| Postmenopausal n (%) | 38 (59.4%) |
| Indication |
| Abnormal uterine bleeding n (%) | 26 (40.6%) |
| Uterine fibroids n (%) | 14 (21.8%) |
| Pelvic organ prolapse n (%) | 5 (7.8%) |
| Premalignant-malignant conditions n (%) | 8 (12.5%) |
| Others n (%) | 11 (17.1%) |
Discussion
The findings of this study suggest that no vaginal cuff dehiscence occured in our laparoscopic hysterectomies when the vaginal vault is closed transvaginally. We also observed that the incidence of other vaginal cuff complications is low (3.1%) when this technique is adopted. We concluded that vaginal cuff closure is an easy and safe method with low complication rates.
In literature, majority of the studies reported that vaginal cuff dehiscence after robotic and laparoscopic hysterectomy is higher than that after vaginal hysterectomy [4,6,12,13]. Studies comparing cuff dehiscence after minimal invasive procedures report cumulative cuff dehiscence 1/632, 1/200 and 1/60 for vaginal hysterectomies, lapaorscopic hysterectomies and robotic hysterectomies, respectively [9]. Although the risk factors associated with cuff dehiscence are reported as early postoperative sexual intercourse and infection, in most cases the risk is not defined except for uterine malignancies [4,14]. The effect of thermal damage by electrocauterization on dehiscence development is controversial. It is reported that reduction of monopolar energy power from 60 W to 50 W does not change dehiscence ratios [15]. Vaginal cuff closure technique is reported as one of the most important factors for cuff dehiscence. Cuff dehiscence is reported less with transvaginal cuff closure technique than laparoscopic and robotic surgeries. In our study, in 23 months follow up no vaginal cuff dehiscence developed in 64 cases. There are studies in literature reporting that vaginal cuff closure reduces postoperative cuff dehiscence risk. Ucella S et al., reported in his systematic review that dehiscence rate is less (0.7% vs 0.2%) after vaginal route cuff closure compared to endoscopic closure technique [9,15].
Vaginal cuff closure is the most difficult and time-consuming part of TLH operations. Mean cuff closure time is reported as 17 minutes in literature [16]. In our study group mean cuff closure time was 5.8 minutes (2-18) and was markedly shorter during vaginal technique than endoscopic suturing.
The necessity of advanced laparoscopic technique and surgical ability for endoscopic stiching is one of the most important obstacles of minimal invasive techniques in front of its widespread use. Barbed suture use is one of developed solutions for reducing stiching time and improving suture security. In studies comparing standard and barbed suture use, cuff closure time was shorter; blood loss was less with barbed sutures. With use of running sutures there was no necessity for a second surgeon. But there was no significant difference between two groups for cuff dehiscence [3,17–19]. Another study reported decrease in postoperative bleeding and cuff dehiscence with use of barbed suture [10].
Authors who are disagreeing with vaginal cuff closure technique during TLH declare that, reaching to cuff and suture stiching may be diffucult especially for women with narrow vagina. In our study group only 7.8% of cases had Pelvic Organ Prolapse (POP) and we did not have any difficulty to reach to cuff in both POP and other indicated patients. We believe that, stabilizing cuff with Kocher clamps from bilateral lateral fornixes and closing the cuff with HR26 needle after removal of uterus provides a sufficient area for operation.
Another aspect to vaginal cuff closure is rising infection risk due to vaginal contamination. However, postoperative infection rates are reported similar between endoscopic and vaginal cuff closure cases in literature [19]. The infectious factor could make significant contributive effect in formation of vaginal cuff dehiscence, but the minimal rate of dehiscence after vaginal route closure could disprove fear of vaginally contaminated infections.
Another advantage of vaginal cuff closure is providing opportunity to place mesh for sacrocolpopexy in POP cases.
There are many case reports in literature, when Y shaped mesh are fixed tranvaginally after vaginal hysterectomy in addition to sacrocolpopexy, which was performed laparoscopically after vaginal closure of cuff [20–22]. The same method is used in our unpublished cases, but in addition endotacker used for sacral fixation of mesh to simplify operation.
Conclusion
Transvaginal vaginal cuff closure seems to be safe, easy and effective for total laparoscopic hysterectomy. Vaginal route can significantly reduce the duration of closure time and requirement of advanced surgical skills. This technique has comparable complication rates with endoscopic suturing techniques.
[1]. Ridgeway B, Falcone T, Innovations in minimally ınvasive hysterectomyClinical Obstetrics & Gynecology 2014 57(1):83-94. [Google Scholar]
[2]. Lyons T, Laparoscopic approach to hysterectomyUpToDateAvailable at http://www.uptodate.com. Accessed: May 2010 [Google Scholar]
[3]. Einarsson JI, Matteson KA, Schulkin J, Chavan NR, Sangi-Haghpeykar H, Minimally invasive hysterectomiesea survey on attitudes and barriers among practicing gynecologistsJ Minim Invasive Gynecol 2010 17:167-75. [Google Scholar]
[4]. Hur HC, Guido RS, Mansuria SM, Hacker MR, Sanfilippo JS, Lee TT, Incidence and patient characteristics of vaginal cuff dehiscence after different modes of hysterectomiesJ Minim Invasive Gynecol 2007 14:311-17. [Google Scholar]
[5]. Cronin B, Sung VW, Matteson KA, Vaginal cuff dehiscence: risk factors and managementAm J Obstet Gynecol 2012 206:284-88. [Google Scholar]
[6]. Hur HC, Donnellan N, Mansuria S, Barber RE, Guido R, Lee T, Vaginal cuff dehiscence after different modes of hysterectomyObstet Gynecol 2011 118:794-801. [Google Scholar]
[7]. Robinson BL, Liao JB, Adams SF, Randall TC, Vaginal cuff dehiscence after robotic total laparoscopic hysterectomyObstet Gynecol 2009 114:369 [Google Scholar]
[8]. Agdi M, Al-Ghafri W, Antolin R, Arrington J, O’Kelley K, Thomson AJ, Vaginal vault dehiscence after hysterectomyJ Minim Invasive Gynecol 2009 16(3):313 [Google Scholar]
[9]. Uccella S, Ghezzi F, Mariani A, Cromi A, Bogani G, Serati M, Vaginal cuff closure after minimally invasive hysterectomy: our experience and systematic review of the literatureAm J Obstet Gynecol 2011 205:119.e1 [Google Scholar]
[10]. Siedhoff MT, Yunker AC, Steege JF, Decreased incidence of vaginal cuff dehiscence after laparoscopic closure with bidirectional barbed sutureJ Minim Invasive Gynecol 2011 18:218-23. [Google Scholar]
[11]. Sunyecz JA, Vaginal cuff closure during total laparoscopic hysterectomy: A new technique has been performed 100 times with very few complicationsAm J Obstet Gynecol 2013 209:71.e1-2. [Google Scholar]
[12]. Blikkendaal MD, Twijnstra AR, Pacquee SC, Rhemrev JP, Smeets MJ, de Kroon CD, Vaginal cuff dehiscence in laparoscopic hysterectomy: influence of various suturing methods of the vaginal vaultGynecol Surg 2012 9:393-400. [Google Scholar]
[13]. Ramirez PT, Klemer DP, Vaginal evisceration after hysterectomy: a literature reviewObstet Gynecol Surv 2002 57:462-67. [Google Scholar]
[14]. Iaco PD, Ceccaroni M, Alboni C, Roset B, Sansovini M, D’Alessandro L, Transvaginal evisceration after hysterectomy: is vaginal cuff closure associated with a reduced risk?Eur J Obstet Gynecol Reprod Biol 2006 125:134-38. [Google Scholar]
[15]. Uccella S, Ceccaroni M, Cromi A, Malzoni M, Berretta R, De Iaco P, Vaginal cuff dehiscence in a series of 12,398 hysterectomies: effect of different types of colpotomy and vaginal closureObstet Gynecol 2012 120:516 [Google Scholar]
[16]. Paek J, Kim SW, Lee SH, Lee M, Yim GW, Nam EJ, Learning curve and surgical outcome for single-port access total laparoscopic hysterectomy in 100 consecutive casesGynecol Obstet Invest 2011 72(4):227-33. [Google Scholar]
[17]. Neubauer NL, Schink PJ, Pant A, Singh D, Lurain JR, Schink JC, A comparison of 2 methods of vaginal cuff closure during robotic hysterectomyInt J Gynaecol Obstet 2013 120:99-101. [Google Scholar]
[18]. Nawfal AK, Eisenstein D, Theoharis E, Dahlman M, Wegienka G, Vaginal cuff closure during robotic-assisted total laparoscopic hysterectomy: comparing vicryl to barbed suturesJSLS 2012 16:525-29. [Google Scholar]
[19]. Hwang JH, Lee JK, Lee NW, Lee KW, Vaginal cuff closure: a comparison between the vaginal route and laparoscopic suture in patients undergoing total laparoscopic hysterectomyGynecol Obstet Invest 2011 71(3):163-69. [Google Scholar]
[20]. Athanasiou S, Grigoriadis T, Chatzipapas I, Protopapas A, Antsaklis A, The vaginally assisted laparoscopic sacrocolpopexy: a pilot studyInt Urogynecol J 2013 24(5):839-45. [Google Scholar]
[21]. Rigoriadis T, Protopapas A, Chatzipapas I, Athanasiou S, Vaginally assisted laparoscopic sacrocolpopexy for the treatment of complete uterovaginal prolapseInt Urogynecol J 2015 26(3):449-50. [Google Scholar]
[22]. Zhu L, Sun Z, Yu M, Li B, Li X, Lang J, Modified laparoscopic sacrocolpopexy with mesh for severe pelvic organ prolapseInt J Gynaecol Obstet 2013 121(2):170-72. [Google Scholar]