Variation in the Branching Pattern of Third Part of Axillary Artery- A Case Report
Aritra Banerjee1, Chiman Kumari2, Saroj Kaler Jhajhria3
1 Junior Resident, Department of Anatomy, All India Institute of Medical Sciences, New Delhi, India.
2 Senior Resident, Department of Anatomy, All India Institute of Medical Sciences, New Delhi, India.
3 Associate Professor, Department of Anatomy, All India Institute of Medical Sciences, New Delhi, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Saroj Kaler Jhajhria, Associate Professor, Department of Anatomy, Teaching Block, First Floor, AIIMS, New Delhi-110029, India.
E-mail: sarojkaler@gmail.com
Anatomical variation of the branching pattern of axillary artery is very common. The knowledge of this variation is often useful during different surgical and interventional procedures. Variations include typically of Lateral Thoracic Artery (LTA) and Posterior Circumflex Humeral Artery (PCHA). The present case has been reported to document the variation of LTA and PCHA. The axilla of a 65-year-old embalmed female cadaver was routinely dissected for educational purpose in the Department of Anatomy, AIIMS, New Delhi, India. Cunnighams Manual of Dissection was followed during the whole dissection procedure. We found that the third part of axillary artery gave rise to a common trunk which divided into PCHA and LTA. The PCHA curved backwards around the humeral neck and made anastomosis with the anterior circumflex humeral artery. The LTA supplied serratus anterior and the pectoral muscles and made anastomosis with intercostal arteries. The axillary nerve accompanied PCHA while the thoracodorsal nerve accompanied LTA. The rare anatomical variation of the branching pattern of axillary artery is assumed to be helpful in the surgical procedures and various therapeutic interventions of the upper limb.
Lateral thoracic artery, Posterior circumflex humeral artery, Serratus anterior
Case Report
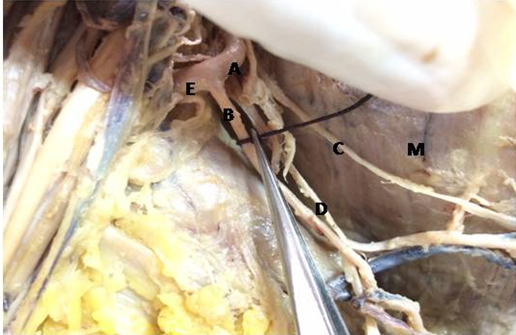
In the routine dissection of the axilla of a 65-year-old female cadaver in the Department of Anatomy, AIIMS, New Delhi, India, we found a common trunk arising from the third part of axillary artery in the right limb. It then divided into two branches LTA and PCHA. Cunninghams manual was followed for the whole procedure. After removing the skin and fascia in the axilla, pectoralis minor was retracted to have the full view of the axillary artery. The three parts of the axillary artery and their branches were noted. In this cadaver the LTA instead of arising from the second part of axillary artery, arose from the third part. The third part of axillary artery gave a common trunk, which was 1.4cm in diameter. It first ran parallel to the axillary artery for 2.5cm, gave the LTA and then continued as the PCHA which wound backwards round the humerus and made anastomosis with the anterior circumflex humeral artery. The LTA (diameter-0.3cm) ran along the lateral thoracic wall for 4.5cm and divided into two branches diameter-0.1cm each. They finally ended by making anastomosis with intercostal arteries and supplying serratus anterior muscle. The subscapular artery arose separately from the third part of axillary artery and supplied the subscapular area along with the subscapular nerve. The axillary nerve and the thoracodorsal nerve accompanied the PCHA and the LTA respectively [Table/Fig-1,2]. The opposite axilla showed the same variation. No other neuro-musculo-vascular anomalies were seen in the upper and lower trunk in this cadaver.
A-Third part of axillary artery; B-Lateral thoracic artery; C-Long thoracic nerve; D-Thoracodorsal nerve; E-Posterior circumflex humeral. M-Medial wall of axilla.
A-Branch of lateral thoracic artery supplying lateral thoracic wall; B-Branch of lateral thoracic artery supplying latissimus dorsi; C-Latissimus dorsi.

Discussion
The axillary artery, which is a continuation of the subclavian artery is divided into three parts by the pectoralis minor muscle. First part, superior to the muscle, gives one branch viz., superior thoracic artery. Second part, behind the muscle, gives rise to two arteries viz., acromiothoracic and lateral thoracic arteries. Three arteries arise from the third part (inferior to pectoralis minor) viz., subscapular, anterior circumflex humoral and posterior circumflex humoral. The subscapular artery continues as the lateral thoracic artery. However, various authors have reported branching patterns different from the one that is normally seen. Nearly, 62.5% of population may have a variated pattern of axillary artery which means that one has to be careful in dealing with this artery [Table/Fig-3,4] [1–9].
Comparison of present observation with other author’s work on the basis of origin of lateral thoracic artery [1–7].
| Authors | Results on basis of origin of lateral thoracic artery |
|---|
| Olinger et al., [2] | From subscapular artery in 4.2% cases |
| Loukas M et al., [3] | From thoracoacromial artery in 67.62% casesFrom axillary artery in 17.02% casesFrom thoracodorsal artery in 5 % casesFrom subscapular artery in 3.93% casesAbsent in 3.33% cases |
| Shantakumar SR and Rao KGM [4] | From 2nd part of axillary artery as common trunk with subscapular artery (case report) |
| Astik R and Dave U [1] | From subscapular artery in 23.5% cases |
| Sreeja MT and Leo R [5] | As common trunk with subscapular artery (case report) |
| Sarkar S et al., [6] | As common trunk along with subscapular and PCHA |
| Saralaya V et al., [7] | A common subscapular trunk gave rise to acromiothoracic, pectoral branch and lateral thoracic as well as PCHA |
| Present observation | As common trunk from third part of axillary artery along with PCHA |
Comparison of present observation with other authors’ work on the basis of origin of posterior circumflex humoral artery [2,7–9].
| Authors | Results on basis of origin of posterior circumflex humoral artery |
|---|
| Standring S [8] | From profunda brachii artery |
| Olinger et al., [2] | From subscapular artery in 12 % cases |
| Saeed et al., [9] | As common trunk along with lateral thoracic artery and subscapular artery |
| Saralaya V et al., [7] | From a common subscapular trunk which also gave rise to the lateral thoracic artery |
| Present study | As common trunk along with lateral thoracic artery |
Embryological Basis
Arterial variation was first mentioned by Von Haller in 1813. The persistence, enlargement and differentiation of capillaries which form the initial plexus may determine the type of variation [10]. The reason behind the development of any abnormal blood vessel is due to the choice of unusual paths in the primitive vascular plexuses or may also be due to the persistent presence of the vessel which was supposed to be disappeared in the normal course of development [11]. The defect of the proximal part of the lateral branch of the seventh cervical intersegmental artery may result in such type of variation [12]. Development of the pattern of blood vessels is also to some extent genetically predetermined [13]. Identity and positioning of blood vessels are genetically determined during early embryogenesis while in later part of embryogenesis remodeling of blood vessels is greatly influenced by blood flow [14].
Clinical Significance
Any type of variation in the body is of utmost importance in the surgical and other interventional medicine to prevent avoidable complications during the procedures. This type of abnormal blood vessels is often to be kept in mind in pectoralis major myocutaneous graft, plastic surgery or during cardiac bypass surgery for grafting. They can be easily delineated by doppler study or angiography, and by doing such kind of study, unwanted vascular injuries can be avoided during any of the surgeries involving intervention of axillary region, as in mastectomy. Even the presence of such type of variation may help in the explanation of the cause and pathogenesis of various peripheral vascular diseases in the upper limb and their treatment such as stenting of subclavian artery. They are also important in the ante grade cerebral perfusion in vascular surgery in case of axillary artery thrombosis [6].
Conclusion
The knowledge of the variation of the axillary artery and its branches is useful in determining pathology, appropriate treatment and proper surgical procedures. A proper vascular and musculocutaneous flap determines the outcome of the surgical procedures. Sometimes the surgeon has to take on-table decision to choose which vessel is appropriate for a reconstructive surgery. This requires knowledge of the normal as well as variated pattern of the vascular system so that a good postsurgical outcome is obtained. A humble attempt has been made to report a case which can contribute to the gross anatomical, diagnostic and therapeutic knowledge in medical sciences.
[1]. Astik R, Dave U, Variations in branching pattern of the axillary artery: A study in 40 human cadaversJ Vasc Bras 2012 11(1):12-17. [Google Scholar]
[2]. Olinger A, Benninger B, Branching patterns of the lateral thoracic, subscapular, and posterior circumflex humeral arteries and their relationship to the posterior cord of the brachial plexusClin Anat 2010 23(4):407-12. [Google Scholar]
[3]. Loukas M, Plessis M, Owens DG, Kinsella CR, Litchfield CR, Nacar A, The lateral thoracic artery revisitedSurgRadiol Anat 2014 36(6):543-49. [Google Scholar]
[4]. Shantakumar SR, Rao KGM, Variant branching pattern of axillary artery: A case reportCase Reports in Vascular Medicine 2012 :1-3. [Google Scholar]
[5]. Sreeja MT, Leo Rathinaraj AS, Clinically significant variation in the branching pattern of the human axillary artery-A case reportIOSR Journal of Dental and Medical Sciences 2014 13(11):56-59. [Google Scholar]
[6]. Sarkar S, Kundu B, Bose A, Saha PK, Variation of branching pattern of axillary arteryInternational Journal of Anatomical Variation 2014 7:27-29. [Google Scholar]
[7]. Saralaya V, Joy T, Madhyastha S, Vadgaonkar R, Saralaya S, Abnormal branching of the axillary artery: Subscapular common trunk. A case reportInt J Morphol 2008 26(4):963-66. [Google Scholar]
[8]. Standring S, Pectoral Region, shoulder and AxillaThe anatomical basis of clinical practice 2008 40th EdNew YorkChurchill Livingstone Elsevier [Google Scholar]
[9]. Saeed M, Rufai AA, Elsayed SE, Sadiq MS, Variations in the subclavian-axillary arterial systemSaudi Med J 2002 23:206-12. [Google Scholar]
[10]. Rodriguez M, Vazquez T, Parkin IG, Sanudo JR, Arterial patterns of the human upper limb: Update of anatomical variations and embryological developmentEur J Anat Suppl 2003 7(1):21-28. [Google Scholar]
[11]. Saunders WB, Arey LB, Developmental Anatomy 1957 6th EdPhiladelphia:375 [Google Scholar]
[12]. Decker GAG, du Plessis DJ, Lee McGregor, Synopsis of Surgical Anatomy 1986 12th EdMumbaiK. M. Varghese Company [Google Scholar]
[13]. Weinstein BM, What guides early embryonic blood vessel formation?Developmental Dynamics 1999 215:2-11. [Google Scholar]
[14]. Jones EAV, Noble F, Eichmann A, What determines blood vessel structure? genetic prespecification vs. hemodynamicsPhysiology 2006 21:388-95. [Google Scholar]