Cyclophosphamide and Doxorubicin Induced Melanonychia: A Case Report
Vivek Bhanubhai Prajapati1, Sharath Madhyastha2, Raviraj Acharya3, Vinaya Gopalaswamy4, Akhila Doddamani5
1 Intern, Department of Pharmacy Practice, Manipal College of Pharmaceutical Sciences, Manipal University, Manipal, Karnataka, India.
2 Assistant Professor, Department of General Medicine, Kasturba Medical College, Manipal University, Manipal, Karnataka, India.
3 Professor, Department of General Medicine, Kasturba Medical College, Manipal University, Manipal, Karnataka, India.
4 Senior Resident, Department of General Medicine, Kasturba Medical College, Manipal University, Manipal, Karnataka, India.
5 Lady Medical Officer, Department of Community Medicine, Kasturba Medical College, Manipal University, Manipal, Karnataka, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Sharath Madhyastha, Assistant Professor, Department of General Medicine, Kasturba Medical College, Manipal University, Manipal-576104, Karnataka, India.
E-mail: dr.sharathymc@gmail.com
Chemotherapeutic agents may rarely cause discoloration and hyperpigmentation of the nails. We present a patient who developed blackish discoloration of nails also referred as melanonychia during six cycles of R-CHOP chemotherapy regimen (rituximab, cyclophosphamide, doxorubicin, vincristine and prednisone) for the treatment of Non Hodgkin Lymphoma (NHL) follicular type. The patient developed blackish brown discoloration in all the nails. As suggested by previous literature evidence the melanonychia could be associated with cyclophosphamide and doxorubicin. According to the Naranjo causality assessment scale, we established that there was a ‘probable’ association of nail discoloration with the drug.
Chemotherapy, Hyperpigmentation, Naranjo causality assessment scale, Non Hodgkin lymphoma
Case Report
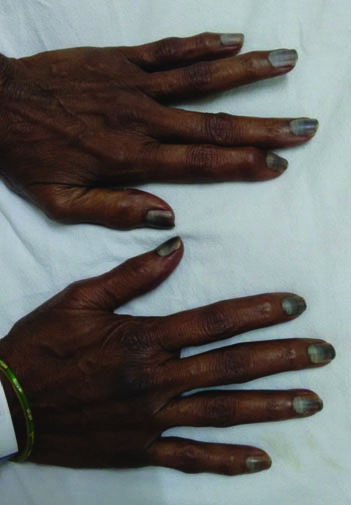
A 67-year-old woman came with complaints of increasing breathlessness and nodular swelling in the axillary and cervical regions since three weeks. On examination, she had generalized lymphadenopathy and massive right pleural effusion. Lymph node biopsy revealed non Hodgkins lymphoma – follicular type. Breathlessness was relieved by thoracocentesis and no malignant cells were detected in pleural fluid. She was treated with the R-CHOP chemotherapy regimen. The patient was being given the following dosage; injection rituximab 525 mg, injection cyclophosphamide 1050 mg, injection doxorubicin 50 mg, injection vincristine 1.9 mg and dexamethasone 12 mg per cycle. Total six cycles of chemotherapy were given over a period of four months with an interval of three weeks between each cycle. Positron Emission Tomography (PET) scan done post chemotherapy showed near complete resolution of all the malignant lymph nodes. After the third cycle of chemotherapy patient started noticing diffuse blackish discoloration of her nails which progressed with subsequent chemotherapy. The discoloration pattern was uniform and involved all the nails of hands [Table/Fig-1,2] and toes [Table/Fig-3]. There was no associated skin or mucous membrane pigmentation. Interestingly, the blackish nail discoloration started to regress after the completion of chemotherapy.
Diffuse blackish discoloration of all finger nails.
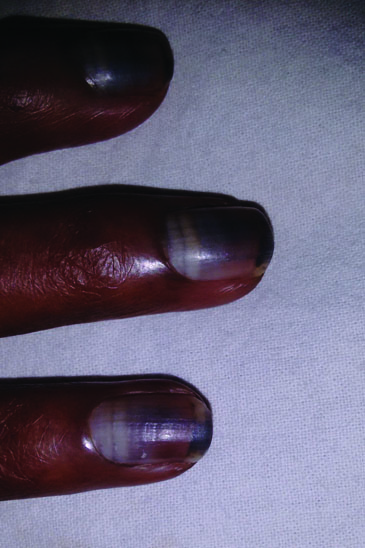
Close-up look of pigmented nails, also note the regression of pigmentation as the new nail grows, after the completion of chemotherapy.
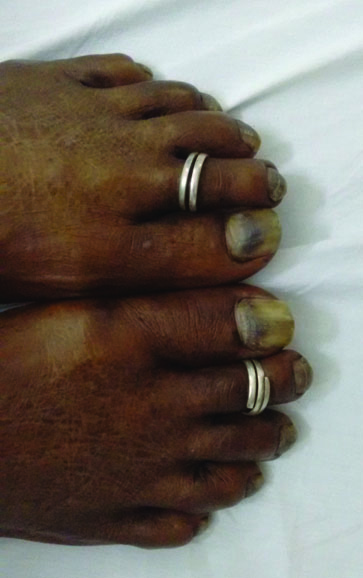
Discussion
Melanonychia is described as the brown to black pigmentation of the nail. It may be due to stimulation and hyperplasia of nail matrix melanocytes, invasion of nail by melanin producing pathogens, subungual haemorrhage and also due to drugs [1–5]. We present a brief report on a patient with non Hodgkin lymphoma - follicular type who developed diffuse blackish discoloration of nails during six cycles of R-CHOP chemotherapy regimen. Drug induced melanonychia usually affects numerous nails and appears as multiple light brown to black longitudinal or transverse bands or diffuse nail discoloration [6]. These depends on the type of melanocytic activation; in case of cluster activation they will be presented as single longitudinal pigmented bands while diffuse activation will result to discoloration of the whole nail [6,7]. A number of chemotherapeutic agents are associated with melanonychia like; bleomycin sulfate, cyclophosphamide, methotrexate, dacarbazine, doxorubicin, etoposide, 5-fluorouracile, hydroxyurea, imatinib, melphalan hydrochloride, daunorubicin hydrochloride, nitrogen mustard, nitrosourea, busulfan, and tegafur [3,6].
Our patient was on cyclophosphamide and doxorubicin which precipitated the discoloration of the nails. Cyclophosphamide is an alkylating agent which acts by introducing an alkyl group to the DNA strand resulting in the DNA cross-linkage leading to disruption of DNA replication stopping cancer cells from growing. It also has immunosuppressant activity; it has cytotoxic effect on lymphocytes. There are many mechanism proposed for cyclophosphamide induced nail pigmentation like genetic predisposition, toxicity to the nail bed and matrix, focal activation of melanocytic matrix and photosensitization. There are few reports on cyclophosphamide induced nail pigmentation, it has been reported that cyclophosphamide may cause purple, brown or black discoloration with different pattern ranging from diffuse to transverse to longitudinal [1,2,6,8] . Doxorubicin acts by intercalating the DNA and also inhibits the progression of topoisomerase II inhibiting DNA synthesis. Doxorubicin has been said to cause longitudinal bands or diffuse brownish nail discoloration [1,6]. Toxicity is generally asymptomatic and limited to cosmetic concern [6], although in some rare case it may be associated with pain and distress.
In some cases, melanonychia may be as a presentation of Nail Apparatus Melanoma (NAM), thus biopsy of melanonychia should be done to confirm whether it is due to melanoma or as a result of other factors. Biopsy is done based on the clinical presentation and patient history indicative of possibility of NAM. NAM is associated with the following features [3,4,9]:
It involves a single digit; mainly the thumb, index finger and the great toe;
It develops after the age of 40 or more;
Associated with a history of digital trauma;
A family or previous history of melanoma or dysplastic nevus.
NAM is suspected if there is no possible explanation for the melanonychia of the nail and presence of the features mentioned above, thereby biopsy is done for confirmation. In our patient, there was no need for biopsy as she had discoloration in all the nails of the hands and toes rather than single digit involvement, also patient did not have any family or personal history of melanoma or dysplastic nevus and also nail discoloration was not associated with any history of digital trauma thus ruling out the possibility of NAM. Another peculiar sign, seen in NAM, is the Hutchinson’s sign [3,9] characterized by extension of nail discoloration to the adjacent cuticle and proximal or lateral nail folds, which was absent in our patient.
There is no specific treatment for melononychia, it’s a self-limiting and it regresses slowly upon discontinuation of the offending agent. The discoloration subsides as the nail grows however it takes a long duration depending on the severity of toxicity, the dose and duration of drug use and also the time of cessation of the offending agent [6]. Patients who are worried about the appearance of the nails can mask it using cosmetics like nail polish.
Conclusion
Cyclophosphamide and doxorubicin induced nail discoloration is a rare adverse event that is under-reported. It is not associated with any deleterious effect to patient health and only affects the physical appearance of the nails. It resolves upon the completion of therapy or discontinuation of the offending agent as the new nails grow.
[1]. Lopes M, Jordao C, Grynszpan R, Sodre C, Ramos-E-Silva M, Chromonychia secondary to chemotherapyCase Rep Dematol 2013 5(2):163-67. [Google Scholar]
[2]. Kumar S, Dixit R, Karmakar S, Paul S, Unusual nail pigmentation following cyclophosphamide-containing chemotherapy regimenIndian J Pharmacol 2010 42(4):243-44. [Google Scholar]
[3]. Jefferson J, Rich P, MelanonychiaDermatol Res Pract 2012 2012:952186 [Google Scholar]
[4]. Haneke E, Baran R, Longitudinal melanonychiaDermatol Surg 2001 27(6):580-84. [Google Scholar]
[5]. Andre J, Lateur N, Pigmented nail disordersDermatol Clin 2006 24(3):329-39. [Google Scholar]
[6]. Gilbar P, Hain A, Peereboom VM, Nail toxicity induced by cancer chemotherapyJ Oncol Pharm Pract 2009 15(3):143-55. [Google Scholar]
[7]. Piraccini BM, Tosti A, Drug induced nail disorders: Incidence, management and prognosisDrug Saf 1999 21(3):187-201. [Google Scholar]
[8]. Ranawaka RR, Patterns of chromonychia during chemotherapy in patients with skin type V and outcome after 1 year of follow upClin Exp Dermatol 2009 34:920-26. [Google Scholar]
[9]. Rich P, Nail surgery in dermatology. In: Bolognia JL, Jorizo JL, Rapini RP, editors 2006 2nd edNew YorkMosby:2260-68. [Google Scholar]