Incisional Hernia as a Cause of Blader Outlet Obstruction: A Case Report
Suhani1, Shadan Ali2, Gunjan Desai3, Kartikeya Sharma4, Shaji Thomas5
1 Assistant Professor, Department of Surgical Disciplines, AIIMS, Delhi, India.
2 Associate Professor, Department of General Surgery, LHMC and SSKH, New Delhi, India.
3 Trainee, Department of Surgical Gastroentrology, Leelavati Hospital, Mumbai, India.
4 Postgraduate Student, Department of General Surgery, LHMC and SSKH, New Delhi, India.
5 Professor and Surgical Unit Head, Department of General Surgery, LHMC and SSKH, New Delhi, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Suhani, Room Number 5025, Teaching Block, AIIMS, Ansari Nagar, New Delhi-110029, India.
E-mail: drsuhani@gmail.com
Incisional hernia usually contains intra peritoneal organs as its content. Extra peritoneal structures like bladder as a content of incisional hernia are relatively uncommon. We managed a young male with an incisional hernia containing a large bladder diverticulum as its content. The bladder diverticulum was going up to the base of scrotum along the posterolateral surface of penile corpora. The patient was diagnosed pre operatively with radiological investigations and underwent exploration with release of diverticulum from corpora and pubic arch followed by diverticulectomy and herniorraphy. To the best of our knowledge and available literature search, there isn’t any similar reported case.
Bladder diverticula, Pelvic fracture, Urethroplasty
Case Report
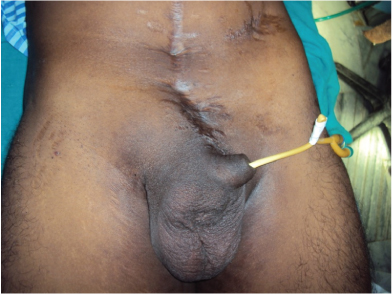
A 30-year-old male presented with swelling in lower abdomen for three years. The swelling was painless and accompanied by voiding urinary symptoms like straining during micturition, thinning of urinary stream and feeling of incomplete bladder evacuation. There was a previous history of pelvic fracture and open suprapubic cystostomy for urethral injury, followed by urethroplasty in childhood. On examination, there was a swelling in the lower abdomen reaching up to base of scrotum, which was partly compressible but non reducible [Table/Fig-1].
Clinical picture of patient showing hernia.
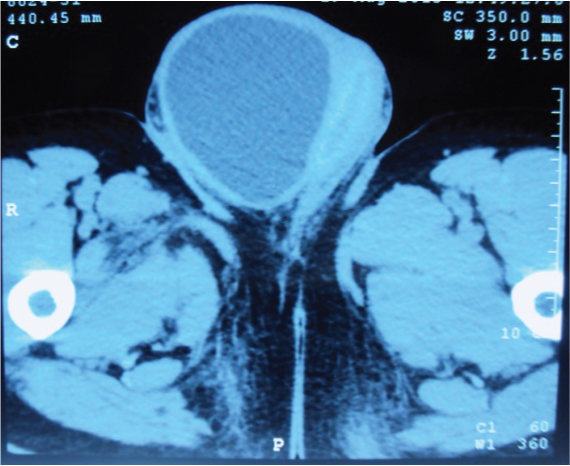
The patient underwent ultrasonography of abdomen including inguinoscrotal region which revealed right cystocele and bilateral hydrouretronephrosis. Since the biochemical investigations were deranged (serum creatinine – 2.8mg/dl), patient underwent Non Contrast Computed Tomography (NCCT) of the abdomen which depicted herniation of antero inferior wall of urinary bladder, through a defect in the linea alba at the site of previous surgical scar, which reached upto base of right scrotum with displacement of right testis to opposite side [Table/Fig-2,3]. The bladder had thick walls and sacculations. Old healed fracture of right inferior pubic rami and bilateral superior pubic rami, without any pubic diastases, was also seen. Further uroflowmetry depicted low maximum and average flow rates with prolonged voiding time. A pan cystourethroscopy revealed normal urethra. Per urethral catheterisation was done for four weeks for optimization of renal parameters, as the herniated urinary bladder impinging upon bladder neck was considered a cause for obstructive uropathy. A diagnosis of incisional hernia with herniation of bladder into right scrotum was made and the patient was taken up for exploration under anaesthesia. Intraoperatively, there was a large bladder diverticulum which was herniating into the right scrotum along the penile corpora [Table/Fig-4]. The bladder diverticula was densely adhered to the penile corpora and the undersurface of pubic arch from which it was separated by a combination of sharp and blunt dissection. The diverticula was seen herniating through a 1.5x0.5cm defect in linea alba, which was opened vertically to indentify the bladder. Diverticulectomy was done with widening of the diverticular neck. A Supra Pubic Catheter (SPC), Retropubic Drain (RPD) insertion and primary herniorraphy with closure of linea alba with prolene was done. Postoperatively, patient had uneventful recovery except for penile oedema which subsided over a week.
CT scan image showing herniated bladder diverticulum in scrotum, pushing the right testis.
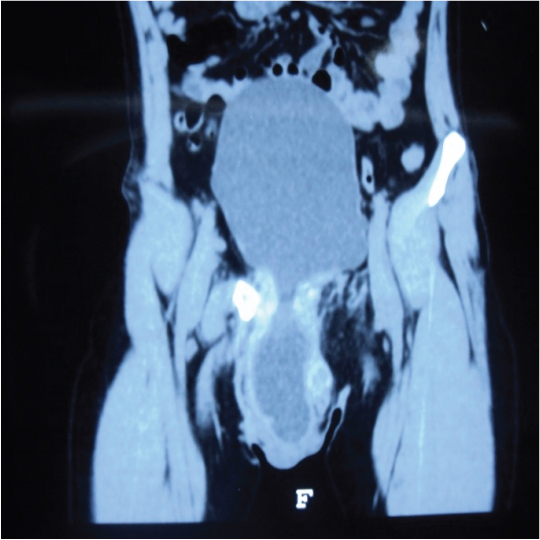
CT scan showing urinary bladder herniating into the scrotum.
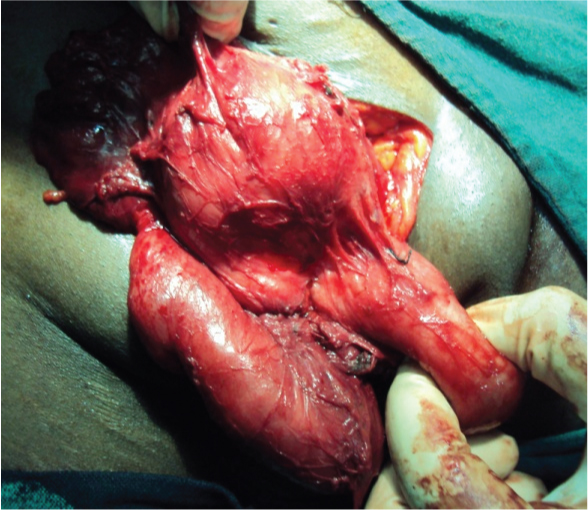
Intraoperative image showing bladder diverticula adhered to penile corpora.
Discussion
Incisional hernia is a very common surgical disease and usually contains intra-peritoneal viscera as its content. An extra peritoneal organ such as the bladder usually doesn’t form a content of the hernia sac. Inguinal and femoral hernias sometimes contain herniated bladder diverticulum [1,2]. However the same is not usually seen in incisional hernia.
Hernias usually result from weakness of musculoaponeurotic layer of abdominal wall, often compounded by an increased intra-abdominal pressure [1]. Herniation of urinary bladder or its diverticulum is a relatively uncommon condition and occurs when the urinary bladder herniates into the inguinal canal, scrotal sac or femoral canal. The herniation of bladder into scrotum has also been termed "scrotal cystocele". Herniation of bladder is seen in 1-3% of all inguinal hernias and around 10 % of men are older than 50 years [3]. However, to the best of our knowledge, there has been no case reported in the literature of an incisional hernia containing a urinary bladder diverticulum.
Bladder diverticula and its herniation are usually caused by an increased intravesical pressure as a result of infravesical obstruction due to benign prostatic hypertrophy, urethral stricture or bladder neck contracture. In our case, the infravesical obstruction was caused by a herniated bladder diverticulum causing extrinsic compression of the bladder neck. Bladder diverticula do not have any specific clinical features and a high index of suspicion along with proper imaging studies are of great help in making a timely diagnosis [1]. A long standing history of Lower Urinary Tract Symptoms (LUTS) in the setting of a hernia should increase the suspicion for the diagnosis of a hernia containing the urinary bladder or a bladder diverticulum [2].
Urinary bladder diverticula have been reported to be contained in inguinoscrotal hernias [2]. The inguino scrotal bladder hernias are classified in the literature as paraperitoneal, intra peritoneal (herniated bladder is completely covered by peritoneum) or extra peritoneal type (bladder is not covered by peritoneum at all) according to its relation with the peritoneum. The paraperitoneal hernia is the most frequent type, in which extraperitoneal portion of hernia lies along medial wall of sac [4].
Most of such hernias are asymptomatic, but sometimes may be accompanied by symptoms such as dysuria, frequency, urgency, nocturia and haematuria. A typical symptom which can be elicited in cases with high index of suspicion is reduction of hernia size after passing urine, and the ability to pass urine after pressing the hernia sac [3].
Although hernia is a clinical diagnosis and doesn’t require any radiological imaging for diagnosis, preoperative imaging may sometimes be needed to confirm diagnosis in doubtful cases, know the contents, its relationship with the surrounding structures and any treatable cause of hernia prior to its repair [5]. Ultrasonography is often the initial diagnostic modality owing to its easy availability and non invasive nature. Although it has a low sensitivity, fluid filled sac in continuity with urinary bladder may be seen [1]. Retrograde cystography and urethrography is an excellent technique to image bladder hernia showing a dumbell shaped bladder, especially if this imaging is required as a workup for LUTS [4].
CT scan imaging is considered to be the study of choice in correctly localizing the hernia, in demonstrating its relationship with the surrounding and in the characterization of its contents [6]. Pointing of bladder towards the side of hernia, i.e. angulation of bladder base anteroinferiorly, is the CT sign of bladder herniation [6].
MRI offers a good resolution and may be helpful in doubtful cases as coronal and sagittal planes can clarify the issue. Also, relations to adjacent vascular landmarks can be well identified [1].
Surgery is the preferred treatment of incisional hernia after treatment of the inciting event if any, like urethral stricture, BPH.
Conclusion
Urinary bladder diverticula as a content of incisional hernia is extremely uncommon. As the clinical features of such a case are not specific, a high index of suspicion along with detailed imaging studies are of great help in making a timely diagnosis. Surgery for hernia after treatment of any predisposing factor like urethral stricture remains the most appropriate treatment modality.
[1]. Omari AH, Alghazo MA, Urinary bladder diverticulum as a content of femoral hernia: a case report and review of literatureWorld Journal of Emergency Surgery: WJES 2013 8:20 [Google Scholar]
[2]. Schuster F, Steinbach F, Scrotal diverticulum of the urinary bladder, a rare cause of inguinal herniaAktuelle Urol 2005 36:55-57. [Google Scholar]
[3]. Bacigalupo LE, Bertolotto M, Barbiera F, Pavlica P, Lagalla R, Mucelli R, Imaging of urinary bladder herniasAJR 2005 184:546-51. [Google Scholar]
[4]. Thompson JE, Taylor JB, Nazarian N, Bennion RS, massive inguinal scrotal bladder hernis: A review of literature with two new casesJ Urol 1986 136:1299-301. [Google Scholar]
[5]. Francoise F, Brunner P, Cucchi JM, Mourou MY, Bruneton JN, Inguinal herniation of a bladder diverticulumClin Imaging 2006 30:354-56. [Google Scholar]
[6]. Izes BA, Larsen CR, Izes JK, Malone MJ, Computerized tomographic appearance of hernias of the bladderJ Urol 1993 149:1002-05. [Google Scholar]