Chondroid Metaplasia in a Fibroepithelial Polyp of Gingiva
Fernando Tenorio1, Paola Campos2, Juan Ignacio Paramo3, Javier De La Fuente4, Nancy Pérez5
1 Professor, Department of Oral and Maxillofacial Pathology, National Autonomous University of Mexico, National School of Superior Studies, Unit Leon Mexico.
2 Clinical Professor, Basic Integral Clinic, Endodontics Department, National Autonomous University of Mexico, National School of Superior Studies, Unit Leon Mexico.
3 Clinical Professor, Basic Integral Clinic, Periodontics Department, National Autonomous University of Mexico, National School of Superior Studies, Unit Leon Mexico.
4 Professor, Department of Public Health, National Autonomous University of Mexico, National School of Superior Studies, Unit Leon Mexico.
5 Senior Resident, Department of Oral and Maxillofacial Pathology, National Autonomous University of Mexico, National School of Superior Studies, Unit Leon Mexico.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Fernando Tenorio, Blvd.UNAM 2011, Predio El Saucillo y El Potrero, León, Gto. C.P.37684, Mexico.
E-mail: ftenorioenes@gmail.com, ftenorio@enes.unam.mx
Gingival masses are commonly encountered in clinical practice and can be a result of many conditions one of them could be metaplasia. Metaplasia is defined as the replacement of the lining of an organ with the type of lining normally found at another site. We are reporting a case of a 17-year-old Mexican male who presented with a pedunculated nodule associated to maxillary anterior gingiva. The histopatological examination revealed a chondroid material covered by stratified squamous epithelium and was diagnosed as chondroid metaplasia.
Cartilaginous, Gingiva, Mucosa, Nodule
Case Report
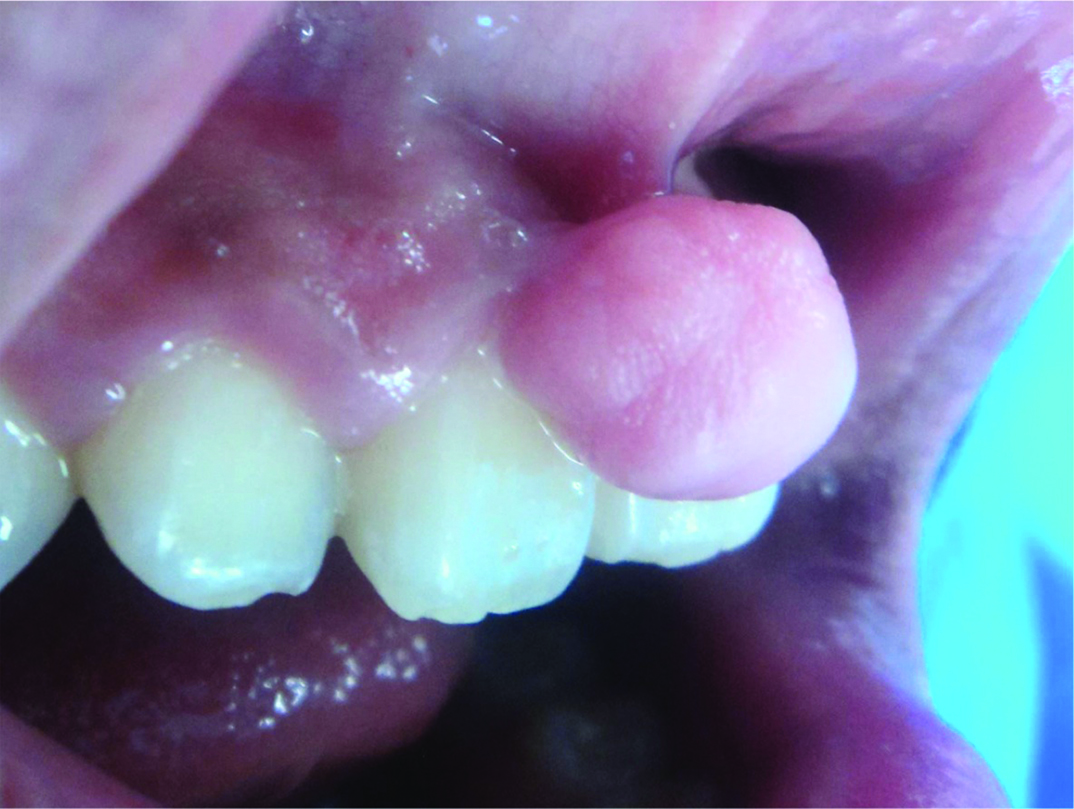
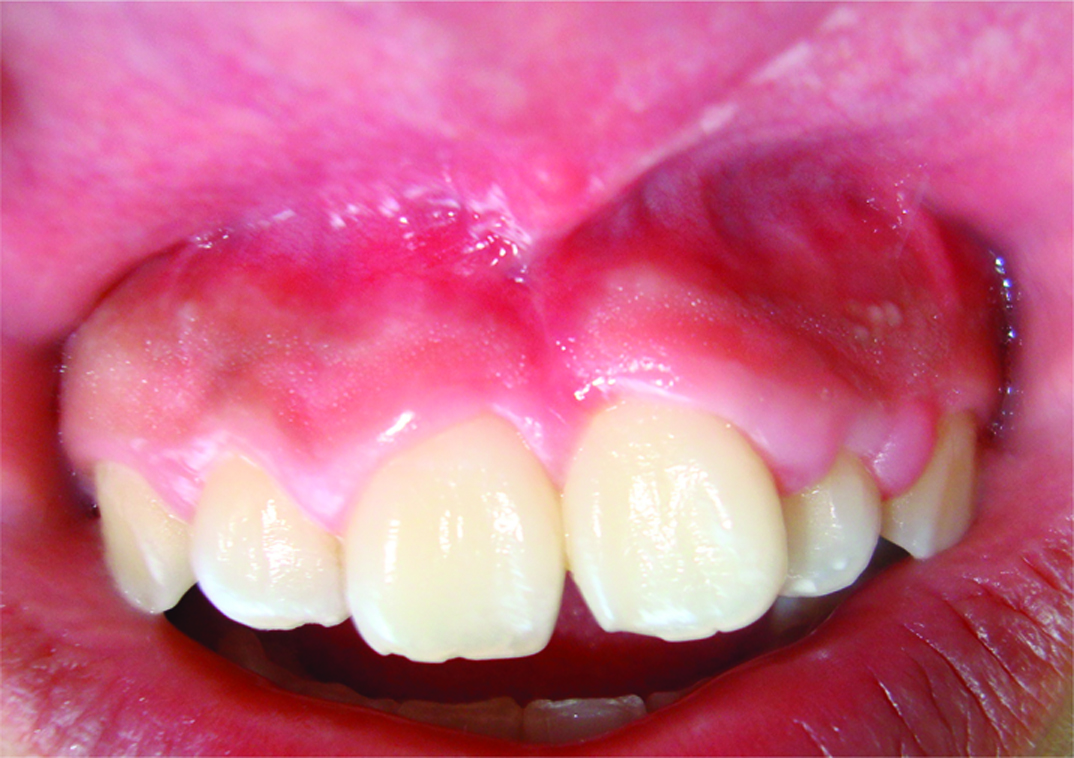
A 17-year-old Mexican male with no systemic involvement, presented to the Oral Pathology Department at León Campus of the National Autonomous University of Mexico, with the complaint of difficulty in biting and chewing, that started several months ago. The Intraoral examination revealed an asymptomatic pedunculated nodule measuring 2.4cmx2.1cm in size, with the same color as that of adjacent gingival mucosa of maxillary anterior teeth [Table/Fig-1]. On palpation, the nodule was found to be firm, with unknown time of evolution. The patient had no history of any significant medical or surgical illnesses in the past. The lesion was provisionally diagnosed at the first appointment as a fibrous hyperplasia, however, based on clinical findings, oral fibroma and the peripheral ossifying fibroma were established as the differential diagnoses.
Pedunculated nodule on gingiva.
Further, the patient was scheduled for excisional biopsy and histological analysis [Table/Fig-2].
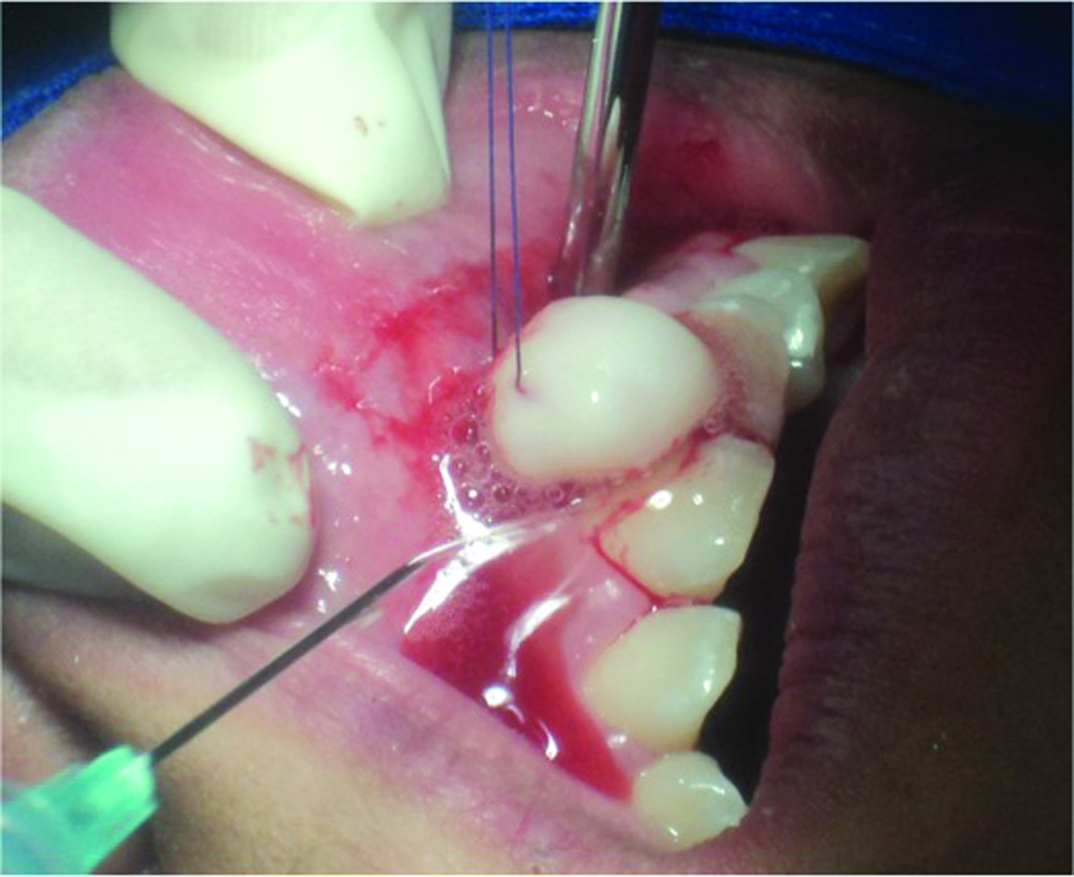
The surgical procedure was performed under local anaesthesia with 2% lidocaine and epinephrine, an incision was made below the peduncle with scalpel blade number 15, removing the nodule entirely; curettage was then performed, and irrigation was done with physiologic saline solution. Subsequently, the excised specimen was placed in 10% neutral buffered formalin, and sent for histopathological examination.
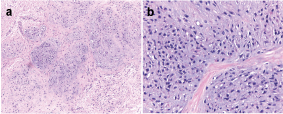
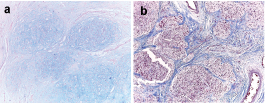
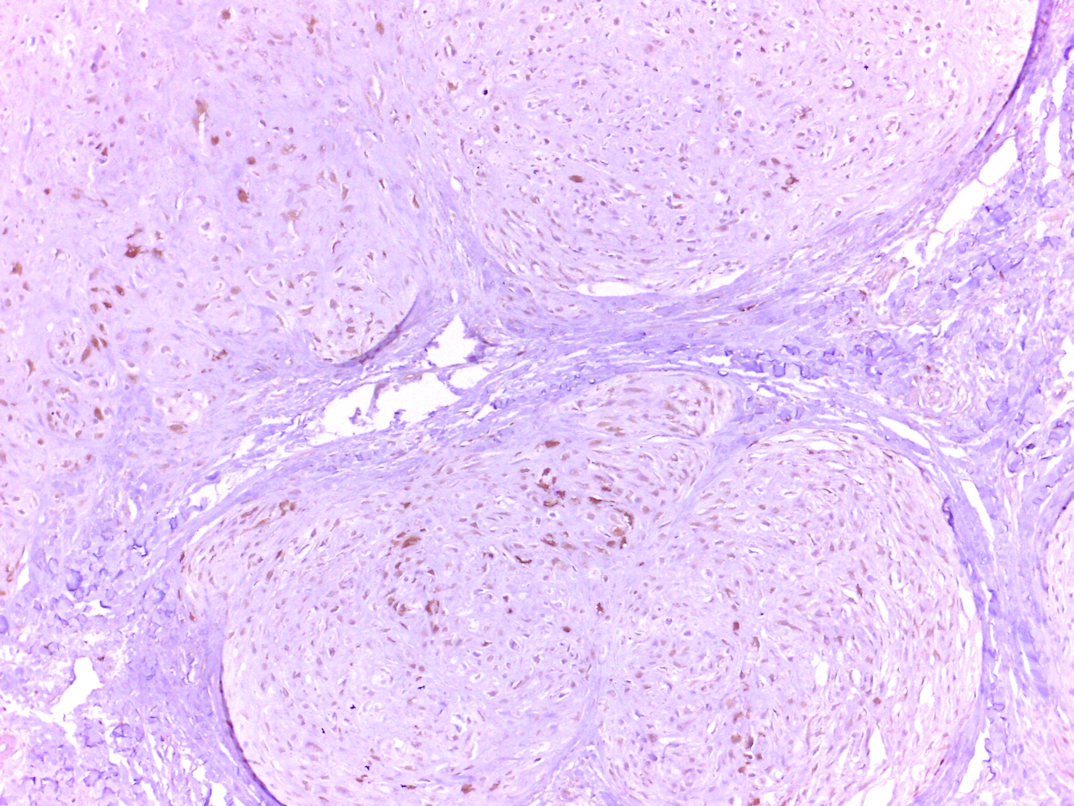
The specimen was routinely processed and histochemically stained with H&E, Masson’s trichrome stain and Alcian blue stain. A thorough microscopic observation showed the presence of multiple well circumscribed lobules of chondroid material of varying shape and size surrounded by fibrous septa and dense fibrous connective stroma [Table/Fig-3a,b], which was covered by variably thick but intact surface epithelium. The histological observations also revealed it to be cartilage-like tissue. However, immunohistochemical marker (S-100, ck-50) based analysis further confirmed the findings [Table/Fig-4a,b,5]. Taken together, the gingival mass was diagnosed as chondroid metaplasia. The post-operative course was uneventful. The patient was closely followed for the next 2 years with no evidence of recurrence or persistence [Table/Fig-6].
a, Multiple well circumscribe lobules of cartilage (haematoxylin and eosin stain [H&E]. magnification x10; b, magnification x40).
a, Masson trichrome stain (magnification x10); b, alcian blue positive (magnification x10).
S-100 protein reactivity highlights chondrocytes associated. (magnification x10), (magnification x40).
Clinical appearance after two year follow-up.
Discussion
Lloyd et al., reported that fibroepithelial polyps are the commonest tumour-like lesions with an estimated prevalence of 12 per 1000 in a population with a slight male preponderance, which develop on the gingiva, buccal mucossa and on the edge or tip of the tongue [1]. Herein, we report a case of 17-year-old Mexican male with an asymptomatic nodule on the gingiva.
The differential clinical diagnosis was established among exophytic entities that are mentioned in the literature and which arise in the gingiva such as: pyogenic granuloma, peripheral ossifying fibroma, fibroma, peripheral odontogenic fibroma, oral focal mucinosis [2], or less frequently lesions like myxoma have been reported by Rawal et al., [3].
Several pathologic conditions as scar, inflamatory processes, haemorrhagic foci, and degenerative lesions, have been described with metaplastic areas with bone and cartilage formation [4]. Likewise, chondroid tissue formation has been reported in conditions such as varicose veins, blood vessels associated to atheromatous plaques [5] and some tumours, such as pleomorphic adenoma, lipoma, undifferentiated aesophageal carcinoma, and chordoid glioma with chondroid metaplasia [1,4].
Chondroid metaplasia has been known to occur in unusual tissues of the body, such as endometrium [6] or in the head and neck region including the oral cavity and the brain, as a response protective mechanism of the local tissue to injury or irritation [7].
Cases of cartilaginous metaplasia in tongue, associated to distinct reparative processes have also been reported [7]. Certain pulpal and carious lesions seem to cause undifferentiated mesenchymal cells that promote the differentiation of odontoblasts, fibroblasts, and osteoblasts; they also show the ability to create osteocyte-like or chondro cyte-like cells post injury, which secrete bone matrix or chondroid matrix [4]. However, the patient in the present case denied having any previous trauma in the region.
The chondroid metaplasia should be distinguished from cartilaginous choristoma that is almost entirely formed by mature hyaline cartilage [8,9] and also, it should be included as differential histopatological diagnosis. The chondroma or soft-tissue chondroma are rare and only few cases have been reported in the oral cavity [1,10,11]. Lesions are formed by lobules of mature (chondrocytes) or immature (chondroblasts) hyaline cartilage with varying degrees of cellularity [12]. Like normal chondrocytes, the cells of chondroid tissue are positive for Vimentin and S100 protein, in adition, biochemically this was characterized by a gradual increase in the mucopolysaccharide content towards the area of chondroid metaplasia. In the present case, mature hyaline cartilage was absent and showed multiple well circumscribed lobules of chondroid material, of varying in shape and size. The chondroid material was surrounded by fibrous septa and was intermixed with dense fibrous connective stroma, covered by epithelium. Further, the tissue was found to be positive for immunohistochemical markers, alcian blue and S100 protein.
The purpose of this paper was to describe an entity which has similar characteristics to reactive lesions that develop in the gum, in case of chondroid metaplasia, histopathology alone confirms the diagnosis. Though a rare entity in the oral cavity, and associated mainly with local irritative processes, it needs to be considered in the differential diagnosis of gingival swellings.
Conclusion
It is concluded that the cases published in the literature do not fit this location; additionally, that providing differential diagnoses prior to surgery must be relevant. The best way to establish a final diagnosis for such lesions is by histopathology.
[1]. Lloyd S, Lloyd J, Dhillon R, Chondroid metaplasia in a fibroepithelial polyp of the tongueThe journal of Laryngology & Otology 2001 115(8):681-82. [Google Scholar]
[2]. Neville BW, Damm DD, Allen CM, Bouquot JE, Oral and maxil- lofacial pathology 2016 4th edSt. LouisSaunders Elsevier:73:483:487:515 [Google Scholar]
[3]. Rawal YB, Mustiful-Martin D, Rosebush MS, Anderson KM, Mincer HH, Slow-growing gingival mass, Clinicopathologic conferenceOral Surg Oral Med Oral Pathol Oral Radiol 2012 113:161-67. [Google Scholar]
[4]. Giardino L, Savoldi E, Pontieri F, Piattelli A, Tallarigo F, Chondroid metaplasia in inflamed pulp tissue: a case reportOral Surg Oral Med Oral Pathol Oral Radiol Endod 2006 102:e42-25. [Google Scholar]
[5]. Caggiati A, Franceschini M, Cartilaginous metaplasia of varicose veins: a case reportPhlebology 2013 28:165-67. [Google Scholar]
[6]. Patil SB, Narchal S, More SS, Endometrial cartilaginous metaplasia: A case report with literature reviewJ Midlife Health 2013 4:19597 [Google Scholar]
[7]. Houang M, Merkur H, Russell P, Chondroid metaplasia of the peritoneumPathology 2010 42(6):585-87. [Google Scholar]
[8]. Kazuhiro M, Masahiko T, Hidetoxhi S, Eiji N, Toshikatsu F, Cartilaginous choristoma deep in the upper midline oral vestibuleBritish Journal of Oral and Maxillofacial Surgery 2004 42:436-38. [Google Scholar]
[9]. Naresh J, Ghosh N, Arora P, Goyal V, Chondroid choristoma of palatine tonsil – a rare entityJournal of Clinical and Diagnostic Research 2013 7(8):1700-01. [Google Scholar]
[10]. Vescovi P, Meleti M, Merigo E, Manfredi M, Corradi D, Giovannacci I, Soft tissue chondroma of the oral cavity: an extremely rare tumour localized on the hard palateCase Reports in Medicine 2014 2014:4148615 pages [Google Scholar]
[11]. Shibasaki M, Iwai T, Chikumaru H, Inayama Y, Tohnai I, Cartilaginous choristoma of the lower lipThe Journal of Craniofacial Surgery 2013 24(2):192-94. [Google Scholar]
[12]. Gungor S, Kamali G, Canat D, Gokdemir G, Soft tissue chondroma of the index finger: Clinical, histological and radiological findings in a unique caseDermatology Online Journal 2013 19(5):7 [Google Scholar]