Central Giant Cell Granuloma of Jaw with Multiple, Multifocal Recurrences
Amita Aditya1, Priyam Aditya2
1 Reader, Department of Oral Medicine and Radiology, Sinhgad Dental College and Hospital, Pune, Maharashtra, India.
2 Consultant Prosthodontist, Aditya’s Dental Privilege, Baner Road, Pune, Maharashtra, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Amita Aditya, Department of Oral Medicine and Radiology, Sinhgad Dental College & Hospital, S. no. 44/1, Vadgaon (Bk), Off Sinhgad Road, Pune-411041, Maharashtra, India.
E-mail: dr.amita30@rediffmail.com
Central giant cell lesion, Mandible, Multilocular, Radiolucency, Recurrent
A 27-year-old female reported with a complaint of recurrent nodule formation in her mouth since four years. Patient was apparently asymptomatic four years back when she noticed a nodular swelling in upper left posterior region of jaw. She underwent surgical excision of the lesion along with surrounding bone by a local dentist. The lesion was histopathologically diagnosed as Central Giant Cell Granuloma. Three years later she noticed a similar nodule in the lower right posterior region of jaw which was again surgically excised and histopathologically diagnosed as Central Giant Cell Granuloma. Three months prior to reporting, the patient again developed a similar nodular swelling in the lower left anterior region of jaw for which she consulted the dentist and was advised surgical excision of the same. Patient was referred to the department for further evaluation and advanced imaging investigations.
Patient had been diagnosed with hyperthyroidism four years back for which she reportedly did not take any treatment except for dietary modifications. These modifications included decreased consumption of salt, sodium and iodine-rich food, processed food etc., and increased consumption of fresh fruits and vegetables, as advised by an Ayurvedic practitioner.
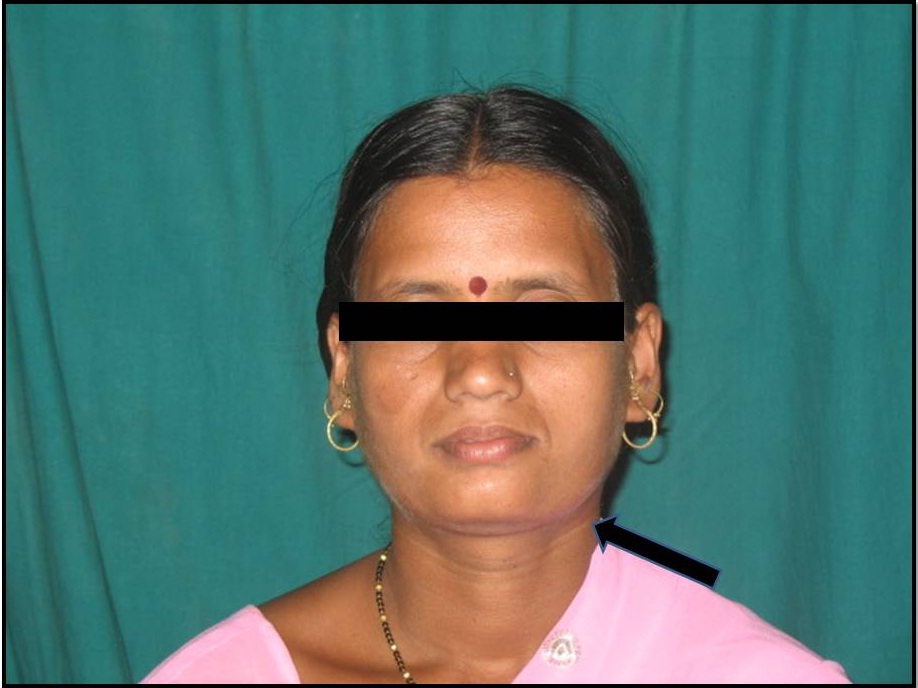
Extra-oral examination revealed a diffuse, hard, non-tender swelling in parasymphyseal and antero-posterior region of left mandibular body, extending mesio-laterally from corner of the mouth to around 3cm distally [Table/Fig-1]. Intra-oral examination revealed single, irregular nodular swelling involving alveolar bone corresponding to lower left canine and premolar region. It extended mesio-distally from the mesial aspect of mandibular left canine to mesial aspect of first molar, antero-posteriorly from the buccal aspect to the lingual aspect of corresponding alveolar bone. Overlying mucosa appeared bluish-red. Swelling was hard to palpate over the inferior aspect and firm superiorly, with mild tenderness. Mobility of canine and first premolar, labial displacement and rotation of first premolar was also observed. Bi-cortical expansion in the affected region of canine and premolars was present [Table/Fig-2a-2c]. On the basis of the clinical examination and history of previous recurrences, a provisional diagnosis of recurrent Central Giant Cell Lesion associated with left mandibular canine and premolar region was thought of. Although, the swelling was nodular, considering the clinical appearance, predominant bony involvement and expansion and displacement of teeth in the region, the lesion was unlikely to be Peripheral Giant Cell Granuloma. A differential diagnosis of Brown’s tumor secondary to hyperparathyroidism was also thought of and hence, serum investigations were carried out for further diagnostic process, although the previous serum investigations of the patient were not suggestive of the same.
Diffuse swelling present in the left antero-posterior region of mandible.
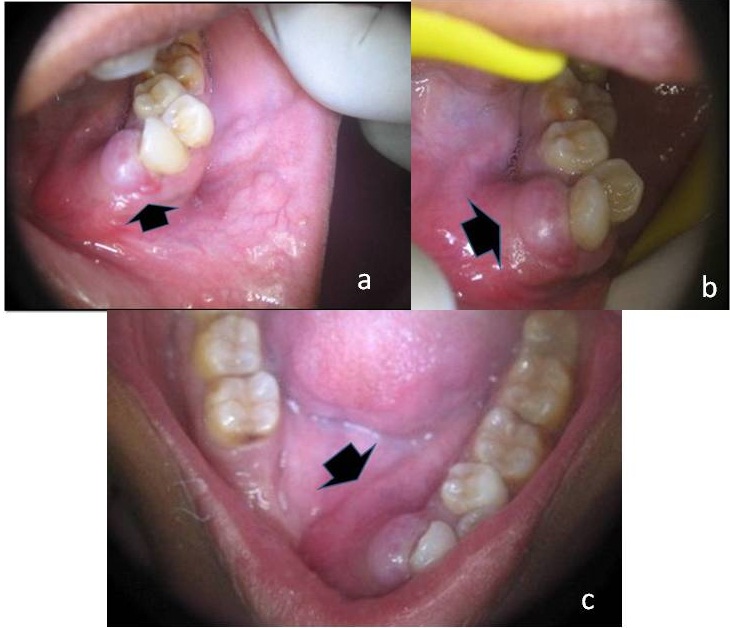
Single, irregular nodular swelling present intra-orally, involving alveolar bone corresponding to lower left canine and premolars region. Bi-cortical expansion and buccal displacement of associated teeth can also be appreciated.
For investigating the lesion radiographically, panoramic radiography and computed tomography imaging was suggested for the patient. Apart from this, routine blood investigations and serum chemistry for thyroid hormone level were also suggested.
Blood and serum investigation did not reveal any abnormality and the patient’s thyroid and parathyroid hormone levels were also found to be within normal range.
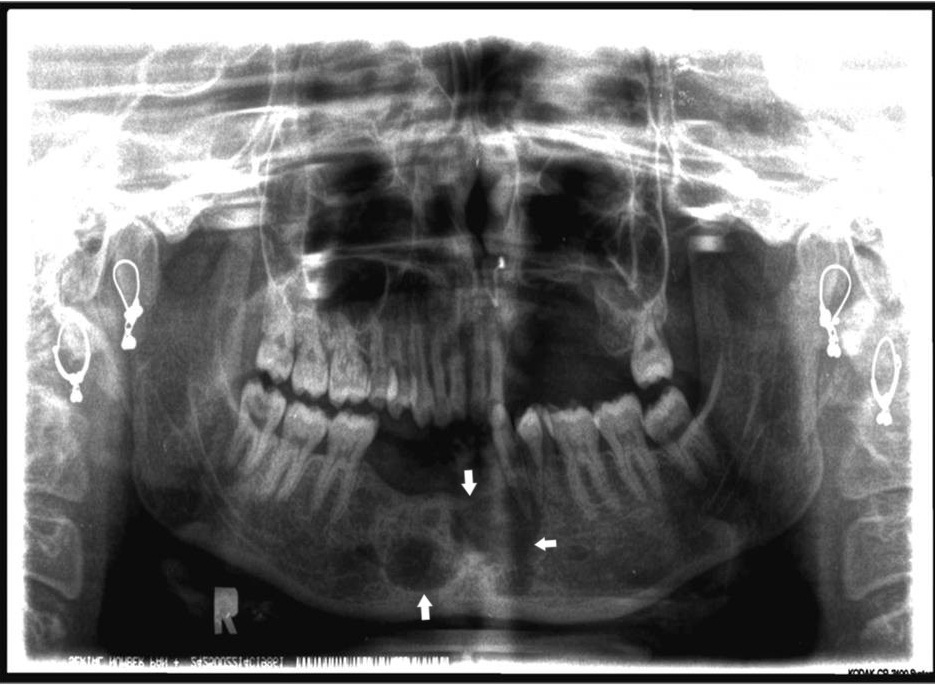
Panoramic radiograph revealed single, well-defined multilocular radiolucency present in the mandibular symphyseal and parasym-physeal region corresponding to mandibular left premolar to right canine region (crossing the mid-line), causing destruction of the overlying crestal bone. Partial alveolectomy was seen in the maxillary left posterior region [Table/Fig-3]. Computed tomography showed expansile, multiloculated lytic lesion present in left hemimandible, involving the menti, extending just beyond the symphysis menti. Associated enhancing soft tissue was seen within the lesion. Both inner and outer cortices of mandible destroyed giving impression of a multiloculated lytic lesion [Table/Fig-4].
Panoramic radiograph revealing well-defined multilocular radiolucency in the anterior region of the mandible. Cortical destruction could also be noted.
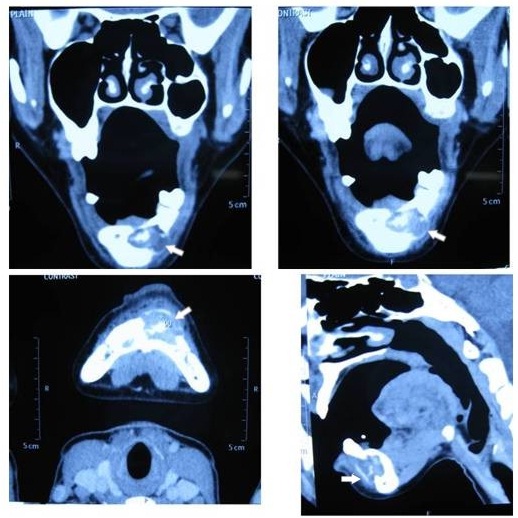
Computed tomography images (axial, coronal and sagittal sections) showing expansile, multiloculated lytic lesion present in left hemimandible, involving the menti, extending just beyond the symphysis menti. Destruction of both the cortical plates could also be seen.
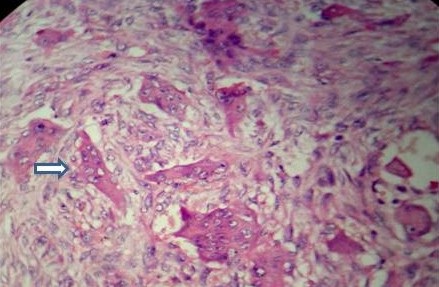
A surgical excision of the lesion was carried out, followed by histopathological examination. H&E stained sections showed fibrocellular connective tissue infilterated with large multinucleated giant cells. Each giant cell consisted of 8 to10 nuclei and showed slight pleomorphism [Table/Fig-5]. Based on the clinical, radiological and histopathological findings and after ruling out the probability of hyperparathyroidism, a final diagnosis of Central Giant Cell Lesion of mandible was made. Patient was then referred to Department of Prosthdontics for occlusal rehabilitation. Till the time of reporting this case, patient did not report any further recurrences.
Photomicrograph (H&E, 40X) showing fibrocellular connective tissue infilterated with large multinucleated giant cells.
Discussion
Giant cell lesions are benign lesions found exclusively in jaws and were distinguished from other jaw lesions by Jaffe in 1953. Jaffe termed these lesions “Giant Cell Reparative Granulomas”, however later the term “Reparative” was abolished as not all the lesions were reported to be self healing in nature [1]. Central Giant Cell Granuloma (CGCG) or giant cell lesions are reported commonly in females and in first two decades of life [2].
The etiology and clinical behaviour of giant cell lesions are still debatable. Initially they were thought to be related to teeth in some way, although they were not considered completely odontogenic in origin. Later they were thought of being derived from odontoclasts which also was considered as an explanation of their predominant occurrence in youngsters and in areas of the jaws that had previously held deciduous teeth. Similar lesions are not frequently seen elsewhere in the body and are usually considered to rather be a variant of low grade osteosarcoma [3].
Clinical behaviour of giant cell lesions of jaw is variable as well as unpredictable. Most commonly it causes asymptomatic expansion of jaws. However, an aggressive variant of giant cell lesions has also been reported which is seen to be associated with features like pain, bone destruction, cortical perforation and root resorption. This variant is also reported to be associated with incidences of recurrences between 13%-49% [4]. Our patient probably presented with similar aggressive variant with an unusual high rate of recurrence within a short span of time.
The radiographic features of giant cell lesions are variable and non-pathognomonic. The lesion usually appears as an unilocular or multilocular radiolucency and may spread across the midline of jaws [1].
The characteristic histopathological feature of giant cell lesions, both central and peripheral, is the presence of distinct multinucleated giant cells in a prominent fibrous stroma [5]. This feature was distinctly seen in our case.
Differential diagnosis of giant cell lesions of jaw includes Giant Cell Tumors (GCT) of bone and Brown’s tumor of hyperparathyroidism. Histopathologically, giant cell lesions of jaw can be differentiated from GCT by the presence of plump bland fibroblast, hemosiderin and fewer giant cells with smaller number of nuclei, which are less uniformly distributed [5]. Differentiation from Brown’s tumor may be done on the basis of clinical and laboratory findings.
Management of giant cell lesion of jaw depends on its clinical and radiographic features. A variety of surgical and medical treatment modalities have been attempted with variable results. Surgically localized lesions can be managed with wide curettage while aggressive lesions seek more invasive procedure like partial maxillectomy or mandibulectomy. Medical management modalities that have been used include steroid, calcitonin, Interferon-alpha injections and intravenous administration of bisphosphonate [1,5].
A diagnostic and prognostic dilemma is often associated with clinically aggressive variant of giant cell lesions of jaws. In fact, only a few cases have been reported in the literature with uncertain clinical, radiographic and histopathologic features of these lesions. This may lead to inadequate treatment of such lesions, because of which patient has to undergo multiple surgeries [6]. Therefore, present case is an attempt to highlight the aggressive and recurrent behaviour of certain giant cell lesions of jaw.
[1]. Pogrel AM, The diagnosis and management of giant cell lesions of the jawsAnnals of Maxillofacial Surgery 2012 2(2):102-06. [Google Scholar]
[2]. Motamedi MH, Eshghyar N, Jafari SM, Peripheral and central giant cell granulomas of the jaws: A demographic studyOral Surg Oral Med Oral Pathol Oral Radiol Endod 2007 103:39-43. [Google Scholar]
[3]. Yamaguchi T, Dorfman HD, Giant cell reparative granuloma: A comparative clinicopathologic study of lesions in gnathic and extragnathic sitesInt J Surg Pathol 2001 9:189-200. [Google Scholar]
[4]. Yadav S, Singh A, Kumar P, Tyagi S, Recurrent case of central giant cell granuloma with multiple soft tissue involvementNational Journal of Maxillofacial Surgery 2014 5(1):60-66. [Google Scholar]
[5]. Murphey MD, Nomikos GC, Flemming DJ, Gannon FH, Temple HT, Kransdorf MJ, Imaging of giant cell tumor and giant cell reparative granuloma of bone: radiologic-pathologic correlationRadiographics 2001 21:1283-309. [Google Scholar]
[6]. Stolovitzky JP, Waldron CA, McConnel FM, Giant cell lesions of the maxilla and paranasal sinusesHead Neck 1994 16:143-48. [Google Scholar]