A Rare Case of Fatal Endocarditis and Sepsis Caused by Pseudomonas aeruginosa in a Patient with Chronic Renal Failure
Manav Aggarwal1, Vikrant Vijan2, Anjith Vupputuri3, Sandya Nandakumar4, Navin Mathew5
1 Consultant, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Kochi, Kerala, India.
2 Consultant, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Kochi, Kerala, India.
3 Consultant, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Kochi, Kerala, India
4 Technician, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Kochi, Kerala, India.
5 Professor, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Kochi, Kerala, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Manav Aggarwal, Department of Cardiology, Amrita Institute of Medical Sciences (AIMS), Amrita Vishwa Vidyapeetham University, Ponekkara, Kochi, Kerala-682041, India.
E-mail: manav19@gmail.com
Nosocomial catheter-related and Arteriovenous fistula (AV)-related infections are significant concern in patients undergoing haemodialysis. These infections are associated with multiple complications as well as mortality and demands immediate and appropriate management. While coagulase-negative staphylococci, S.aureus, and Escherichia coli are the most common causes of catheter-related infections in haemodialysis patients, such infections caused by Pseudomonas aeruginosa are relatively rare. Here, we present an unusual case of 36-year-old male patient with chronic renal failure, who developed endocarditis and sepsis from Pseudomonas aeruginosa infection of the left hand arteriovenous fistula. The bacteraemia in the present case caused multiple complications including dry gangrene of bilateral lower limbs, stroke, endophthalmitis, left brachial artery thrombosis and vegetations on the interventricular septum and aortic wall. Despite antibiotic treatment, the patient suffered a cardiac arrest and could not be revived.
Arteriovenous fistula infections, Embolectomy, Endophthalmitis, Gangrene
Case Report
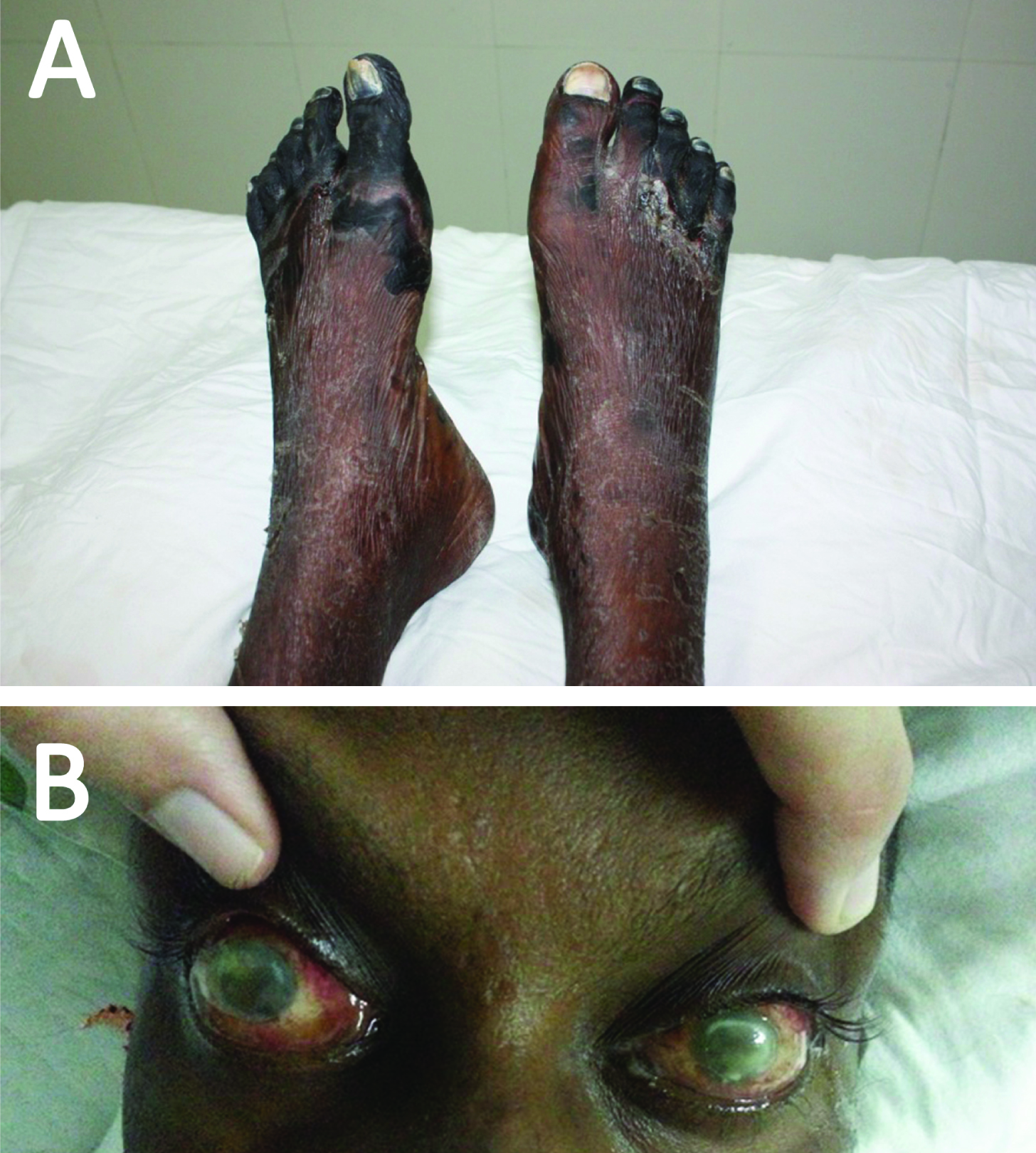
A 36-year-old male was transferred to our hospital from another hospital on a ventilator. He was a known case of Berger’s disease (IgA nephropathy) and was on maintenance haemodialysis for the past 3 months. He was undergoing haemodialysis by jugular venous catheter after creating Arteriovenous (AV) fistula on the left hand. One month ago, the patient was admitted at a local hospital with jugular venous catheter related infection. During his stay in the hospital, the patient had septic shock followed by resuscitated cardiac arrest. He was shifted to another secondary care hospital after resuscitation. His blood culture showed P. aeruginosa growth. He was initiated on intravenous antibiotics as per sensitivity and stabilized. Subsequently, the patient developed septic emboli and dry gangrene in both the lower limbs [Table/Fig-1a] and was advised amputation however the patient refused. Following this the patient developed severe pain in the left upper limb. Doppler imaging showed brachial artery thrombosis at the site of AV fistula. He was advised to undergo angioplasty, but the patient and bystanders refused further treatment in the hospital. He was discharged against medical advice. However, he was admitted again after three days at the same hospital with septicaemia and altered sensorium. He underwent surgical embolectomy of the left brachial artery. Magnetic Resonance Imaging (MRI) brain showed bilateral infarcts. Immediately, the patient was shifted to our hospital in the state of sepsis and encephalopathy. He was admitted to critical care unit and a bed-side Transthoracic Echocardiogram (TTE) was performed, which suggested large vegetation attached to the interventricular septum. Blood cultures were directed for evaluation. While awaiting the blood culture report, the patient was started on antibiotics that included meropenem and cefepime for P. aeruginosa based on previous sensitivity. Simultaneously, an ophthalmology consultation was sought in a view of redness of both eyes. The patient was diagnosed with bilateral endophthalmitis after thorough ophthalmoscopic examination [Table/Fig-1b]. Next day, a Transesophageal Echocardiogram (TEE) was performed to confirm the diagnosis. It showed large vegetation on the interventricular septum and on the descending aortic wall [Table/Fig-2a,b]. The patient subsequently suffered a cardiac arrest, and could not be revived.
(a) Bilateral dry gangrene of lower limbs; (b) Bilateral redness in both eyes; Diagnosed with endophthalmitis
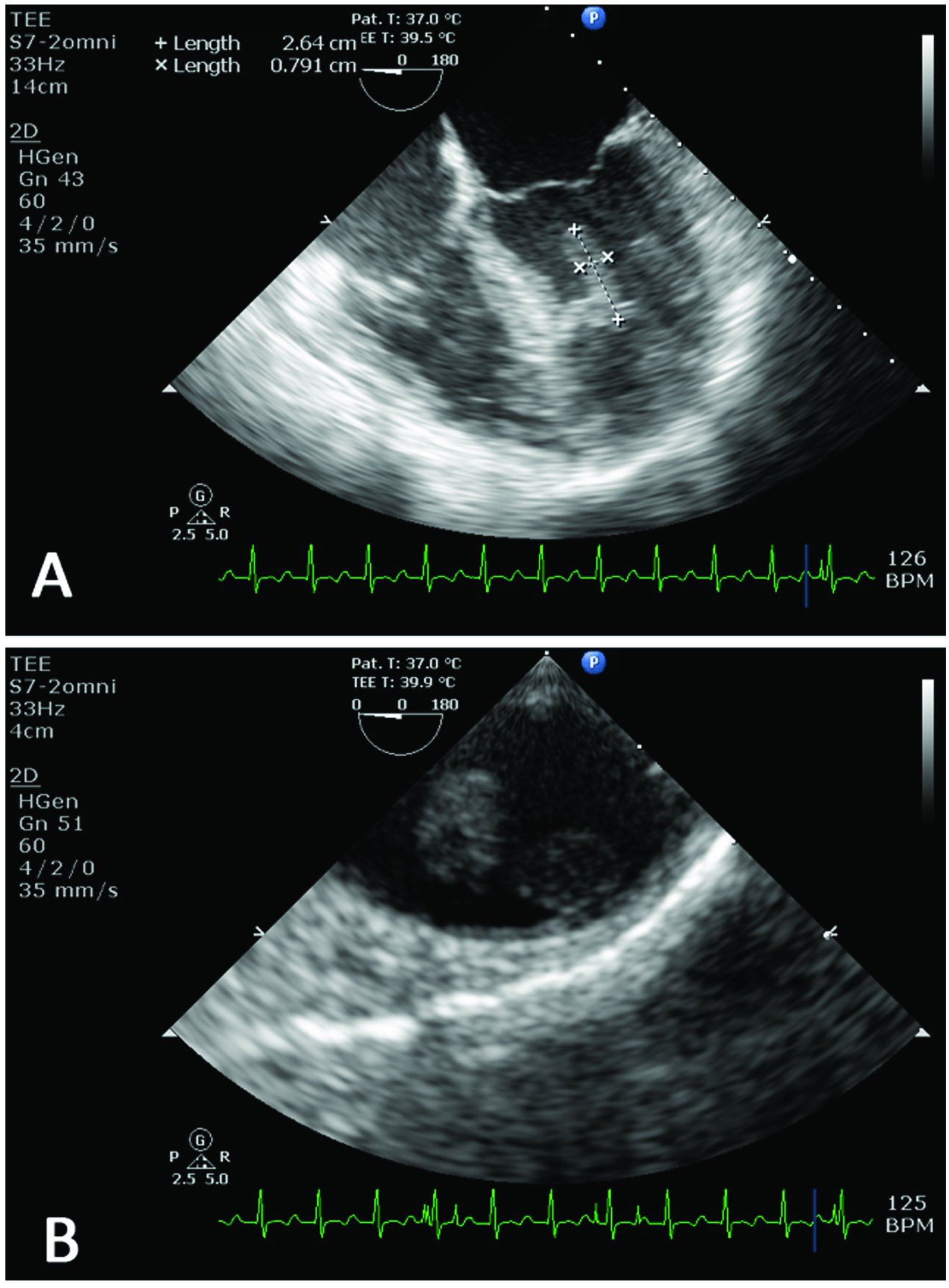
Transesophageal echocardiography indicating vegetation on the (a) interventricular septum and (b) on the descending aortic wall.
Discussion
Although catheter and AV fistula related infections are one of the major causes of increasing morbidity and mortality in haemodialysis patients [1]. Reports describing features and consequences of multiple complications are rare [2]. It should also be noted that coagulase-negative Staphylococci, S. aureus and Escherichia coli are the most common causes of catheter-related infections in haemodialysis patients, and infections caused by Pseudomonas aeruginosa are relatively rare [1]. In the present case, we have reported an unusual occurrence of haemodialysis-catheter and AV fistula related endocarditis and sepsis caused by P. aeruginosa with multiple complications.
Earlier, the end-stage renal disease was associated with high mortality and morbidity. Subsequent evolution of haemodialysis or peritoneal dialysis has improved the survival in such patients. However, a vulnerability to develop infection due to haemodialysis with AV fistula or AV graft has been a significant concern for many years. Available literature suggests that about 9–20% of AV grafts become infected in due course in patients undergoing chronic haemodialysis [2]. Infective endocarditis is relatively infrequent but a serious complication of bacteraemia in patients undergoing chronic haemodialysis [3]. This usually appear when bacteria from catheter gain access to the patient’s circulation [4]. While Gram-positive organisms are the most common cause of catheter-related infections, gram-negative pathogens remains the etiological cause in very few cases [5]. Endocarditis due to P. aeruginosa, a gram-negative pathogen, usually occurs among intravenous drug abusers and is uncommon as a nosocomial infection in haemodialysis patients [6]. TEE is frequently used in the diagnosis of infective endocarditis due to its higher sensitivity and ability to detect smaller lesions [7].
The present case can be viewed as unique, considering the multiple consequences after AV graft infection in a haemodialysis patient. Metastatic bacterial endophthalmitis is an uncommon yet devastating bacterial complication of haemodialysis catheter-related sepsis [8]. In the present case, a subsequent presentation of acutely inflamed eyes led us to explore the etiological cause. Since infective endocarditis and AV fistula infection due to P. aeruginosa were identified from blood cultures might be associated with infective endocarditis. This patient had Pseudomonas septicaemia, we believed that metastatic endophthalmitis in the present case followed by developing red eye. The diagnosis was confirmed by a thorough ophthalmoscopic examination.
Cardiac complications of arteriovenous fistulas in patients with end-stage renal disease have significant and potentially deleterious effects on cardiac functions. Chronic overload of the heart in AV fistula often leads to valvular damage in haemodialysis patients [9]. However, the intracardiac infections involving non-valvular structures are rare. Hence, the present case is unusual as the isolated huge vegetation was attached not only to the interventricular septum but also to the aortic wall, suggesting that non-valvular infective endocarditis can also occur primarily in compromised patients. In addition, the distant septic embolization in the present case also affected the brain by causing stroke, bilateral endophthalmitis and dry gangrene of bilateral lower limbs. To the best of our knowledge, no previous reports have described such multiple consequences after AV fistula infection in a haemodialysis patient.
Conclusion
In summary, infective endocarditis should always be considered as a consequence of suspected septicaemia in a haemodialysis patient. Distant dislodgment of the septic emboli is a major complication of infective endocarditis in selected cases. Immediate and appropriate management is vital for these patients.
[1]. Sanavi S, Ghods A, Afshar R, Catheter associated infections in haemodialysis patientsSaudi J Kidney Dis Transpl 2007 18(1):43-46. [Google Scholar]
[2]. Harish A, Allon M, Arteriovenous graft infection: a comparison of thigh and upper extremity graftsClin J Am Soc Nephrol 2011 6(7):1739-43. [Google Scholar]
[3]. Kamalakannan D, Pai RM, Johnson LB, Gardin JM, Saravolatz LD, Epidemiology and clinical outcomes of infective endocarditis in haemodialysis patientsAnn Thorac Surg 2007 83(6):2081-86. [Google Scholar]
[4]. Gahlot R, Nigam C, Kumar V, Yadav G, Anupurba S, Catheter-related bloodstream infectionsInt J Crit Illn Inj Sci 2014 4(2):162-67. [Google Scholar]
[5]. Fysaraki M, Samonis G, Valachis A, Daphnis E, Karageorgopoulos DE, Falagas ME, Incidence, clinical, microbiological features and outcome of bloodstream infections in patients undergoing haemodialysisInt J Med Sci 2013 10(12):1632-38. [Google Scholar]
[6]. Lin TI, Huang YF, Liu PY, Chou CA, Chen YS, Chen YY, Pseudomonas aeruginosa infective endocarditis in patients who do not use intravenous drugs: Analysis of risk factors and treatment outcomesJ Microbiol Immunol Infect 2014 Nov 1 [Epub ahead of print] [Google Scholar]
[7]. Seif D, Meeks A, Mailhot T, Perera P, Emergency department diagnosis of infective endocarditis using bedside emergency ultrasoundCrit Ultrasound J 2013 5(1):1 [Google Scholar]
[8]. de Lima LM, Cecchetti SA, Cecchetti DF, Arroyo D, Romão EA, Dantas M, Endophthalmitis: a rare but devastating metastatic bacterial complication of haemodialysis catheter-related sepsisRen Fail 2012 34(1):119-22. [Google Scholar]
[9]. Alkhouli M, Sandhu P, Boobes K, Hatahet K, Raza F, Boobes Y, Cardiac complications of arteriovenous fistulas in patients with end-stage renal diseaseNefrologia 2015 35(3):234-45. [Google Scholar]