The oral candidal infections have soubriquet “Disease of diseased”. It has been prevailing remarkably among diabetics and denture wearers. There are many effective antifungal agents which are available for treating oral candidal infections, however the primary or secondary resistance is not uncommon after prolonged use of these antifungals, with the advent of novel discovery the natural products have been an alternative with reduced side effects and low cost. Many in-vitro studies have been done on phytochemicals, although not much of the studies have been done invivo [1].
Oral candidiasis is the most prevalent opportunistic infection affecting the oral mucosa [2]. Although many species of candida subsist; Candida albicans and C.tropicalis are the most prevalent species which cause variety of fungal infections in the oral cavity. Several predisposing factors have been enumerated for cause of oral candidiasis and candidal associated lesions. However, the colonization and growth of candida in patients with prosthesis and endocrine disorders have escorted to clinical importance [3]. A wide and ample variety of antifungal drugs are available for treatment of candidiasis nevertheless high recurrence has been eminent primarily in immunocompromised individuals after stopping the medication hence, there is a need for search of novel antifungal drugs [4,5]. The use of medicinal plants has been an old age practice since the dawn of civilization. The herbal remedies used in traditional folk medicine may be useful to combat different diseases and may perhaps help to overcome the problem of resistance caused by conventional antifungal drugs [6,7]. Henceforth phytochemicals have been emerging as novel drugs with ongoing drug trials in different diseases of oral cavity. With one such attempt in the present study a novel clinical trial of ethanolic extracts of crude lawsone has been tried in denture wearers and candidates with uncontrolled diabetes attributing to its antifungal property.
Listerine an essential mouth rinse contains many active and inactive ingredients, its active ingredients include eucalyptol (0.092%), menthol (0.042%), methyl salicylate (0.060%), thymol (0.064%) and inactive constituents include water, alcohol (26.9%), benzoic acid, poloksamer 407, sodium benzoate and caramel. It has been widely used in dentistry as an antiseptic mouth wash due to its antimicrobial activity [13], although the information on mechanism of action on candida is diminutive. Meiller et al., has done an invitro study against C. albicans and evaluated that the minimum inhibitory concentration of listerine against candida is 100μg/ml [14]. The antifungal studies on listerine are still sparse and the comparison studies with other mouth rinses have not yet elucidated and expounded.
The present study was aimed to compare the antifungal efficacy of essential oil based mouth wash with crude lawsone invivo.
Materials and Methods
The present study was a randomized single blinded parallel group trial conducted in the Department of Oral Medicine and Radiology Drs. Sudha & Nageswararao Siddhartha Institute of Dental Sciences, Gannavaram, Andhra Pradesh, India, from June 2015 to December 2015 and the trial was registered in Clinical Trial Registry of India (CTRI) with number REF/2016/03/11053. All the study procedures were carried out according to Declaration of Helsinki which was revised in 2000 and the approval was taken from Institutional Ethical Committee. Initially informed consent was obtained from the subjects who were willing to participate in the study. Subjects were allowed to leave at any moment of study procedures. A total of 100 subjects who were known diabetics and denture wearers, wearing either removable or fixed dentures, were randomly selected by simple randomization method using coin toss. These patients were evaluated for blood sugar levels by using Standardized Glycosylated Hemoglobin Assay. The test results were standardized according to American Diabetes Association, accordingly subjects with HbA1C >7% were considered as poor diabetic controls and were incorporated in the study [15]. Out of 100 subjects 70 were declared as poor diabetic controls, of which 10 patients were not willing to proceed with the study due to various reasons. So, a total of 60 subjects who were denture wearers and diagnosed as poor diabetic controls by HbA1C were included in the study [Table/Fig-1]. The exclusion criteria were patients who were pregnant or lactating, subjects who were allergic to the prepared mouth wash, patients with known systemic diseases like liver, cardiac and renal diseases and uncooperative patients who were unable to follow the directions of the study.
Patient In flow chart according to consort guidelines.
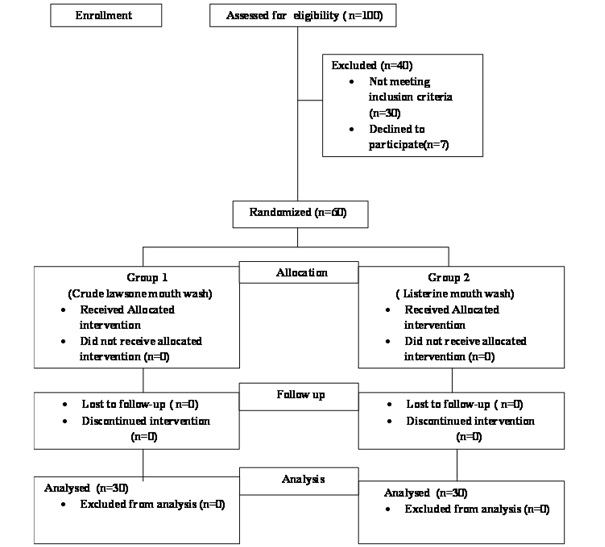
The present study was a single blinded trial, where all the study subjects were blinded regarding usage of their mouthwashes. All the mouth washes were dispensed in identical amber colored bottles of 500ml which was coded as Group I and Group II.
Subject population: The incorporated study subjects were divided into two groups.
Group 1 - 30 patients, were advised to use crude lawsone mouth wash.
Group 2 - 30 patients, were advised to use listerine mouth wash.
Case history and thorough oral examination was performed in all the subjects. The subject’s data on age, gender, marital status, adverse oral habits was also noted.
Preparations of crude lawsone mouth wash: Plant Material: The dried leaves of LI was identified and collected in April 2015 from Jai Hanuman Plantation and its botanical identification was done by Dr. AK Mohta Acharya Nagarjuna University, India. The dried leaves were initially grinded into 42 mesh size which was later pulverized into fine powder using blender.
Preparation of plant extract and mouth wash: Subsequently the extraction procedure was done using ethanol as a solvent. To determine the antifungal activity of crude lawsone the ethanolic extract was prepared. Only 10gms of leaf powder was dissolved in 100 ml ethanol and kept in rotary shaker at speed of 180 rpm for 3hrs following the same procedure was repeated and it was kept overnight. The residue was filtered using Whatman’s filter paper of size 1. The combined residue was later subjected to drying using rotary evaporator with reduced pressure at 600c. The resulting residue was then stored at 40oc and utilized for further experiment.
Phytochemical screening: The extracts were subjected to qualitative phytochemical analysis to detect the presence of active constituents like napthoquinones, alkaloids, sterols, xanthones coumarins and flavonoids by standard phytochemical screening procedures. The qualitative test for each constituent is described in [Table/Fig-2]. The final yield concentrate was 0.8gms which was then super added with glycerol 10ml, L-menthol 0.2gm and peppermint oil of 0.05gm and citric acid 0.2gms. Subsequently sufficient water was added to make a total volume of 100ml. [Table/Fig-3].
Qualitative phytochemical screening tests of Lawsonia inermis ethanolic leaf extracts.
| Test Name | Lawsone ethanolic leaf extract |
|---|
| Napthoquinones |
| • Dam-Karrer Test method | + |
| • Borntrager’s Test | + |
| Alkaloids |
| • Dragendorff’s Test | + |
| • Mayer’s Test | + |
| • Wagner’s Test | + |
| • Hager’s Test | + |
| • Tannic Acid Test | + |
| Sterols |
| • Libermann Burchad Test | + |
| • Salkowaski Test | + |
| • Sulfur powder Tes | + |
| Coumarins |
| • Fluorescence Test | + |
| Flavonoids |
| • Shinoda Test | + |
| • Alkaline Reagent Test | + |
| • Zinc Hydro chloride Test | + |
| Tannins | + |
(a) Materials used in preparing lawsone mouth wash; (b) Dried leaves of lawsonia inermis and prepared crude lawsone mouth wash.

Study procedures: The oral rinse technique was performed with distilled water in all the selected subjects before use of mouth wash and CFU of candidal species were determined at baseline. Subsequently, the subjects were randomly allocated to use either crude lawsone or listerine mouth wash. Post therapeutic samples were then collected after 1hr following drug usage and they were further advised to use given mouth washes twice daily with volume of 5ml/rinse for one week and again the CFU were evaluated. Any allergy to prescribed mouthwash was recorded at all time points 1hr and 1week. Nevertheless the subjective satisfaction of taste and smell were also recorded during this time period. Taste and olfactory satisfaction was assessed using 9 point hedonic scale to grade the degree of satisfaction regarding taste and smell [16]. This scale is a balanced bipolar scale which is neutral at the centre, and with four positive and four negative categories on each side. The four positive categories were considered as strongly satisfied, where the neutral and two negative categories were considered as moderately satisfied and the last two negative categories as weakly satisfied [Table/Fig-4].
Sample ballot for assessment of taste and smell using 9 point Hedonic Scale.
INTERPRETATION OF HEDONIC SCALE
4 Positive categories (Like) - Strong satisfaction
Neutral and negative categories (Dislike slightly and moderately) - Moderate satisfaction
Negative categories (Dislike very much and extremely) - Weak satisfaction

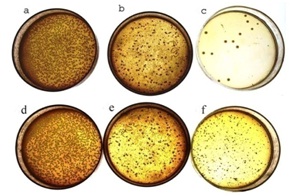
The burning sensation after using mouth wash was assessed using Visual Analogue Scale (VAS). [Table/Fig-5]. The samples were collected in a sterile container. Each sample was subjected to serial dilution technique following which the samples were diluted in physiological saline, 0.2 ml of each sample was diluted in 9.8ml of physiological saline, five dilutions were done for each sample and 5th dilution was subjected to determine the CFU, subsequently the inoculation was done for 48hrs [Table/Fig-6a-6f]. The species identification of the resulting candida was done using Hi- Chrome candida differential agar Hi media lab, Mumbai India as Candida albicans or C. tropicalis M1297A. [Table/Fig-7a, 7b].
Assessment of burning sensation upon using mouth wash by VAS (Visual analogus scale).
| VAS Score |
|---|
| ≤5 | >5 | Total |
|---|
| Group-1 | 30(100%) | 0(0%) | 30(100%) |
| Group-2 | 26(87%) | 4(13%) | 30(100%) |
Fisher value=0.11 difference in frequency=1 p>0.05 Not Significant
Petri dishes with lawsone showing colonies of candida at different time intervals (a,b,c). Petri dishes with listerine showing colonies of candida at different time intervals (d,e,f).
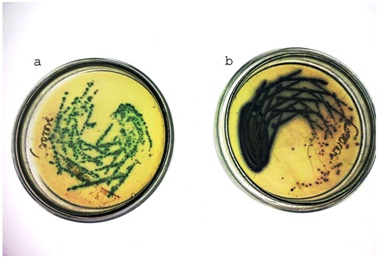
Isolation of candida species in chrome agar: a) Green Color; b) Dark purple colour.
Statistical Analysis
The data was analyzed using SPSS 16.0. The demographic data was analyzed using descriptive statistics where the mean age and gender distribution were determined. Confidence interval was calculated using inferential statistics. Comparison of CFU between the groups was analyzed using independent t-test. Subjects satisfaction of using mouth wash i.e., taste and smell was evaluated using chi square test with p<0.01. The probability value was assessed as p≤0.05 which was considered statistically significant and p≤0.01 as highly significant where p≥0.05 as not significant.
Results
Subjects in the current study were selected with almost equal age and gender distribution.
The mean reduction in CFU was calculated at different time intervals, where more reduction in CFU was seen after 1 hr and 1 week of using mouth wash in Group 1 compared to Group 2. Although, not much reduction was seen at baseline hence, to derive better results inferential statistics were obtained, where confidence interval was calculated showing lower and upper bound values, which also showed tremendous decrease in CFU after 1 hr and 1 week in Group 1. Finally, these values depict the fact that lawsone was more effective in reducing CFU when compared with listerine at all the time intervals attributing to its excellent antifungal activity [Table/Fig-8].
Mean reduction of CFU in each group by different time intervals (At baseline, 1hr, 1 week).
| Type of Mouth Wash | Time Interval | N | Min | Max | Mean | SD | SE | 95% Confidence Interval Mean |
|---|
| Lower Bound | Upper Bound |
|---|
| Group 1 | Base Line | 30 | 38 | 290 | 148 | 65 | 12 | 124 | 172 |
| After 1 hr | 30 | 0 | 110 | 34 | 29 | 5 | 23 | 45 |
| After 1 week | 30 | 0 | 20 | 6 | 6 | 1 | 4 | 9 |
| Group 2 | Base Line | 30 | 46 | 290 | 151 | 58 | 11 | 129 | 172 |
| After 1 hr | 30 | 0 | 180 | 63 | 43 | 8 | 47 | 79 |
| After 1 week | 30 | 0 | 92 | 30 | 25 | 4 | 20 | 39 |
SD- Standard deviation, SE- Standard error
The intergroup comparison was done at different time intervals using independent t-test (baseline, 1hr, 1week) which demonstrated outstanding and tremendous decrease in CFU after 1hr and 1week of using mouth wash in Group I with (p<0.01). Nevertheless not much of difference was seen at baseline (p>0.05) [Table/Fig-9].
Intergroup comparison of mean CFU by different time intervals.
| Time | Mean | Independentt-value | p-value | Inference |
|---|
| Group 1 | Group 2 |
|---|
| Base Line | 148 | 151 | 0.16 | 0.87 | Not Significant |
| After 1 hr | 34 | 63 | 3.06 | <0.01* | Highly Significant |
| After 1 week | 6 | 30 | 5.09 | <0.01* | Highly Significant |
* Highly significant p-value; Independent t test.
The subject’s satisfaction on taste and smell was analyzed using chi square test which was categorized into strong, weak and moderate satisfaction. The taste satisfaction was significantly higher in Group1 with p<0.01 whereas, the olfactory sensation was more satisfactory in Group 2 with p<0.01 [Table/Fig-10].
Subjects satisfaction of taste and smell in Group1 and Group 2.
| Group | Taste | Total |
|---|
| Weak Satisfaction | ModerateSatisfaction | Strong Satisfaction |
|---|
| Group-1 | 3(10%) | 13(43%) | 14(47%) | 30(100%) |
| Group-2 | 12(40%) | 13(43%) | 5(17%) | 30(100%) |
| Group | Smell | Total |
| Weak Satisfaction | Moderate Satisfaction | Strong Satisfaction |
| Group-1 | 12(40%) | 14(47%) | 4(13%) | 30(100%) |
| Group-2 | 2(7%) | 10(33%) | 18(60%) | 30(100% |
Taste - Chi-square= 9.66; Smell - Chi square =16.7
Difference in frequency=2; p<0.01 Highly Significant
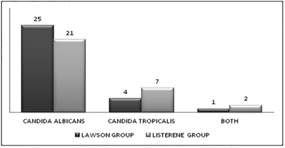
[Table/Fig-11] reveals prevalence of candidal species in the two groups. Candida albicans was seen in Group 1, where as C. tropicalis was chiefly seen in Group 2. However, both C.tropicalis and C.albicans species together were seen more in Group 2.
Prevalence of candidal species in the two groups. Candida albicans was seen in Group 1, where as C. tropicalis was chiefly seen in Group 2.
Discussion
The incidence of fungal infections has been rising eminently with increased prevalence in the developing countries [17]. The oral candidiasis or candidosis caused by candidal species is one of the most common and frequent opportunistic fungal infection of the oral cavity in humans [18]. The prevalence of these increased infections has been associated with some systemic and local predisposing factors like use of dentures, xerostomia, prolonged therapy with antibiotics, malnutrition, endocrine disorders, which in turn diminish the quality defense of the individual [19]. Candidaalbicans a dimorphic fungus is most commonly isolated from the oral cavity which is more potent and virulent occurring in approximately 50% of the cases of oral candidiasis in humans [20]. The treatment of candidiasis is always a dispute because of recurrence owing to prolonged use of antifungals. Polyenes and Azoles have been widely used in the treatment of candidiasis but majority of them have various draw backs pertaining to resistance, toxicity etc., [3]. Hence, the rationale of selecting the particular cohort was to bring out a novel traditional and curative approach for treating candidiasis among diabetics and denture wearers. Phytochemicals either in mono or poly herbal combination may provide boundless hunt for new drug leads. Plants by tradition have proved to be a rich source of novel drug compounds, as the blend of different herbs have made large contributions to human health and welfare [21]. Hence, in the present study we tried to evaluate the antifungal efficacy of ethanolic crude extract of lawsonia inermis as it is a matter of intense scientific study. Subsequently following standardization to prepare our mouth wash first we tried to evaluate the active constituents responsible for the antifungal activity of lawsonia inermis and as an initial step we assessed the constituents like napthoquinones, alkaloids, sterols, xanthones coumarins and flavonoids by qualitative phytochemical analysis which were positive in the present trial. The plant extracts have both polar and non polar compounds although for extraction of hydrophilic compounds ethanol is the best solvent which is desirable to substantiate the use of phytomedicine against fungal infections [22]. Many in vitro antifungal activities have been conducted on lawsonia inermis using different polar and non polar solvents; in the present study we used ethanolic crude extracts of lawsone, and as ethanol is also toxic to bacteria it may be best solvent for preparation of mouth wash. Lawsone (2-hydroxy1, 4 napthoquinone) is the principal constituent responsible for dying and coloring matter of plant. This compound is liable for antifungal effect of lawsone. The anticandidal action of lawsone is not clear; however specific studies on the mode of action of lawsone against candida should be carried out to determine how it affects the microorganism [23]. Hence, using ethanolic crude extracts of lawsone the mouth wash was prepared and compared with listerine. In order to prepare the mouth wash Sritrairat et al., used potassium salt for preparation of lawsone methyl ether mouthwash to estimate the antifungal activity [24]. Although in the current study to evaluate the proper efficacy of phyto constituents of lawsone, we peculiarly prepared ethanolic extract of crude lawsone owing for stronger inhibitory effects and this is the first of its kind and prototype, where crude lawsone showed excellent impending result pertaining to its antifungal activity. Nittayananta et al., has conducted an in vitro and in vivo study to determine the antifungal efficacy of lawsone methyl ether mouth wash and compared with chlorhexidine mouthwash and confirmed that LME mouth wash possesses potent antifungal activity [25]. Current study was in accordance with the previous study done by Nittayananta et al., where the results of the present study illustrated superior antifungal activity of crude lawsone compared to Listerine [25]. Listerine is an essential oil based mouth wash which has little antifungal activity.
But there are no such studies on the mechanism of action of listerine against candida, although the ultra structural studies done by Thosar et al., have revealed that the essential oils in listerine produces liposoluble effect, which in turn increases permeability and cell death [26]. Furthermore, in the present study the viable colonies were more decreased with lawsone (T>1hr- 50%), (T>1 week -85%) and the results were remarkable with crude lawsone. Similarly listerine showed not much reduction of CFU at (T<1hr, 1week) when compared with lawsone. This attributes to the fact that long term use of lawsone may be a first-rate antifungal drug. Moreover, lawsonia inermis is safe and non toxic. Its leaves, roots and seeds can be safely used up to 8000mg [27].
Gull et al., carried out a toxicological evaluation of ethanolic extract of lawsone and revealed that it can be administered orally up to 300 mg/kg body wt and he found no signs of toxidrome [28].
In the current study 500mg of leaf extract was taken to determine the antifungal activity which yielded 0.4gm. Consequently we could not find any signs of toxic effects in the study subjects. Staining effect, burning sensation and any ulceration were evaluated in all the subjects using Visual Analogue Scale (VAS) score for burning sensation and staining effects were assessed using modified discoloration index proposed by Macpherson et al., where visual stain assessment was made on buccal/labial and lingual/palatal aspects of the index teeth [29]. Likewise we also concentrated on staining effect of lawsone in the oral cavity; we perhaps did not notice any staining in study candidates at 1 hr and 1 week of using the crude lawsone mouth wash. However, few subjects reported mild burning sensation and few subjects reported with minor apthous ulcers, although the subject’s satisfaction of taste was good with lawsone than listerine. Despite patients using listerine reported more burning sensation and however, olfactory sensation was good with listerine compared to lawsone.
In addition we tried to differentiate species of candida in the oral cavity such as C. albicans and C. tropicalis perhaps C. albicans, C. tropicalis and C. glabrata are predominantly seen in the oral cavity. However other species like, C. krusei, C. parapsilosis can also be appreciated [30]. In our study we differentiated C. albicans and C. tropicalis using Hi chrome candidal differential agar, where Candida albicans showed green color and C. tropicalis was seen as dark purple color. Our study was in accordance with previous study done by Duane et al., [31]. Finally our findings suggest that crude lawsone is an alternative source of antifungal agent. It is very imperative to reinforce and buttress further investigations on other candidal species and establish a basis for comparison of lawsone with conventional antifungals.
Future prospects: In future the prospective clinical trials should focus on isolation of each phyto constituent from plants, and their mode of action as well whether they act on cell wall or cytoplasmic membrane or any precise path ways could be established. More over poly herbal formulations need to be studied in future for their superior antifungal properties with minimal side effects. Lastly as advances in the provision of health care continue, the work of fiction on phytochemicals and implementation of prompt antifungal therapy without resistance needs to be commenced. To the best of our knowledge our study was opening and first of its kind which particularly emphasized on crude extracts of lawsone in vivo.
Limitation
Long term follow-up with large sample size can be performed to evaluate further effects of mouth wash. In the present study species of C.albicans and C.tropicalis were identified, further investigations can be carried out to identify the changes in the genotype before and after usage of mouthwash.
Conclusion
Herbaria are boon to nature owing to their excellent diverse properties. The present study justifies that ethanolic extract of crude lawsone mouth wash illustrated superior antifungal activity when compared to listerine. As an ideal anti-fungal agent is not available; phyto chemicals like lawsone may be used as an alternative. At the end of this preventive strategy and extensive research engine, we summarize that the long term studies needs to be accomplished to establish the fact that phytochemicals can be used as regular medication by the clinicians to bring a new era in phytomedicine.
Fisher value=0.11 difference in frequency=1 p>0.05 Not Significant
SD- Standard deviation, SE- Standard error
* Highly significant p-value; Independent t test.
Taste - Chi-square= 9.66; Smell - Chi square =16.7
Difference in frequency=2; p<0.01 Highly Significant