Paraquat Poisoning: A Case Report
Harish Kumar1, Veer Bahadur Singh2, Babu Lal Meena3, Subhash Gaur4, Rahul Singla5
1 Senior Resident, Department of Medicine, S P Medical College, Bikaner, Rajasthan, India.
2 Senior Professor, Department of Medicine, S P Medical College, Bikaner, Rajasthan, India.
3 Assistant Professor, Department of Medicine, S P Medical College, Bikaner, Rajasthan, India.
4 Assistant Professor, Department of Medicine, S P Medical College, Bikaner, Rajasthan, India.
5 Department of Medicine, S P Medical College, Bikaner, Rajasthan, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Harish Kumar, Department of medicine S P Medical college Bikaner, Rajasthan, India.
E-mail: drharishsgnr@gmail.com
Paraquat is commonly used herbicide by farmers in North West Rajasthan. Despite its easy availability, poisoning of its not common. Fatal dose of paraquat is so small that >10 ml poison can damage lungs permanently. Diagnosis is often difficult without proper history, absence of specific clinical feature and lack of diagnostic test. Inhalation exposures represent one of the most important routes of poisoning. We are reporting a case of inhaled paraquat poisoning with complication of irreversible acute kidney, liver and lung injury.
Inhalation, Paraquat, Poison, Prognosis
Case Report
A 50-year-old healthy male farmer was admitted in department of emergency, PBM hospital Bikaner 2 hour after accidental inhalation of unknown poison during spraying; with the chief complain of several episode of vomiting. The identity of the poison was confirmed by the family. As they had brought an empty pack of “Gramaxone”.
There was no evidence or history of any prior psychological disorders or any medications and addiction. After it patient has discomfort of mouth, nasal irritation, irritation of eyes, dyspnoea, nausea, vomiting. Patient was drowsy but conscious and co-operative. On examination blood pressure was 110/80 mmHg, heart rate 94/minute, regular, respiratory rate 18 per minute regular abdomino-thorasic and oxygen saturation 95% on room air. Temperature was 98.8 degree Fahrenheit by axilla. Cardiac examination was absolutely normal. Both lung fields were clear on auscultation. Other systemic examinations were normal.
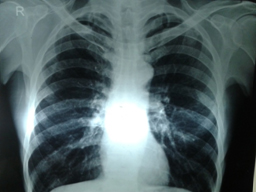
Gastric lavage was performed, and repeated doses of charcoal were given in the emergency department. Patient was shifted to intensive care unit for further management. Initially Blood Cell Line, Renal Function Test, Liver Function Test, Electrolytes and Arterial Blood Gas was within normal limits. ECG showed sinus tachycardia. Chest X- ray was normal [Table/Fig-1].
Initially Chest X- ray was normal.
After shifting to ICU patient was managed with IV fluid and supportive measure. Steroid (methylprednisolone 15-20 mg/kg/day) was started from first day. Patient was managed conservatively for two days. Patient becomes unstable on third day with the feature of adult respiratory distress syndrome. He became severely hypoxic (SpO2 50) Venturi Mask was used. ABG showed PaO2 of 50mmHg with mild respiratory alkalosis. Intubation was performed and placed on mechanical ventilation. Broad spectrum antibiotics (Pipracillin-Tazobectam 4.5 mg and metronidazole 100mg IV 8 hour) were started prophylactic after intubation. Blood investigations were successively deranged day by day [Table/Fig-2] and probable diagnosis of multiple organ dysfunction syndrome was made on fourth day. Chest X-ray showing diffuse bilateral coalescent opacities with diffuse alveolitis, probable diagnosis Acute Respiratory Distress Syndrome was made [Table/Fig-3]. On fifth day saturation and blood pressure was fall and patient placed on noradrenline and dopamine support. Despite our best effort patient was expired on sixth day.
Showing successive deranged blood investigation.
| Blood investigation | Day 1 | Day 2 | Day 3 | Day 4 | Day 5 |
|---|
| haemoglobin | 9.9 | 8.1 | 8 | | 8.5 |
| WBC | 8000 | 8500 | 11500 | | 15000 |
| platelets | 3.4lakh | 1.85lakh | 1.24lakh | | 1.5lakh |
| Blood urea | 80 | 102 | 165 | 201 | 117 |
| Serum creatinine | 1.8 | 2.1 | 6.3 | 6.4 | 7.7 |
| Bilirubin total | 1.5 | 3.5 | 9.2 | 6.8 | 11.1 |
| Conjugated bilirubin | 0.4 | 1.9 | 4.2 | 3.4 | 6.4 |
| SGOT/SGPT | 27/39 | 178/209 | 201/116 | 92/116 | |
| Na/K | 145/3.9 | 156/3.4 | | | 158/5.1 |
| PO2/PCO2 | 90/32 | 84/34 | 46/26 | 65/33 | 74/36 |
| Saturation | 94% | 86% | 50% | 75% | 70% |
On 4th day Chest X- ray showing diffuse bilateral coalescent opacities with diffuse alveolitis.
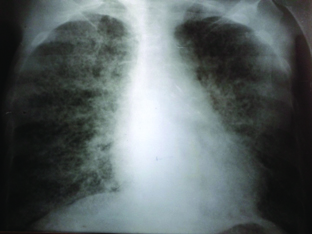
Discussion
Inhalation exposures represent one of the most important routes of poisoning. The lung provides an excellent route for absorption and distribution of toxic gases by its large surface area and good blood supply [1]. Besides causing irritation and injury to the lungs, inhalation of gases in some, may even lead to significant systemic poisoning involving vital organs such as the brain, kidney and liver [1–3]. In terms of its action on the weeds, paraquat interferes with the intracellular electron transfer systems, thus inhibiting the reduction of NADP to NADPH during photosynthesis. This will then result in the accumulation of superoxide radical which causes destruction of lipid cell membranes. [4] Commercial preparations of paraquat are normally sold in the form of liquid concentrate with a concentration ranging from 20% to 42% w/w. These solutions are available for agriculture use as dichloride salts which is water soluble. Besides being supplied in the form of a single active ingredient, there are products in the market containing paraquat in combination with other herbicides such as sodium chlorate and 2,4-dimethylamine. Paraquat is mainly eliminated by kidney and acute kidney injury is the complication of it. Ingestion of small quantities can cause severely damage to lung and kidney despite treatment [5–7].
Paraquat poisoning is not uncommon in India. Ingestion of this poison is more common than inhalation. Few cases have been reported from North India [3]. The cases which have been reported associated with both accidental and intentional ingestion. In our case paraquate is associated with accidental inhalation. Toxicity may range from mild to fulminate. How much it can dangerous that inhalation of this poison have same fatality rate as ingestion. Due to easy availability of this poison make it commonly used accidental or suicidal poison. Despite easy availability reported case this poisoning is rare. It is herbicide that is use on unwanted weeds and vegetation. In our case patient was a farmer and belonged to area where paraquat commonly used in the field as herbicide. Inhalation exposures represent one of the most important routes of poisoning. Here we present a case with acute respiratory distress following accidental paraquat inhalation.
Gastric lavage should be performed immediately if possible within 2 hours post-ingestion. This is to reduce further absorption of paraquat into the bloodstream. Absorption of paraquat is rapid and distributed in most tissue, slowly concentrated in lungs and kidney. So, the best approach to managing inhalation exposure is prevention. Involvement of lung in the form of diffuse alveolitis and subsequent pulmonary fibrosis is the hallmark of paraquat poisoning. Acute respiratory distress syndrome because of paraquat usually appears 24–48 h after ingestion [3]. Inhalational exposure to paraquat known to be associated with fatal pulmonary damage as result of superoxide radicals and other free radicals created due to the accumulation of paraquat in the lungs [8].
In our patient the cause of hypoxia was direct inhalation of paraquat poison. Ingestion of a smaller volume (10-20 ml) of the concentrate produces the same symptoms with the exception that the development of renal failure occurs within 2 to 6 days after ingestion [5]. Renal failure may be manifested by proteinuria and oliguria which then progresses to acute tubular necrosis. Due to rapid distribution of poison haemodialysis does not support in acute kidney injury in treatment. In our case lung and renal involvement was early. It causes irreversibly pulmonary damage defined by alveolitis, pulmonary oedema, and infiltration of inflammatory cells. It leads injury to every organ but in lesser extent, death is usually due to respiratory insufficiency. There is NO specific antidote for paraquat poisoning. Treatment of paraquat poisoning is largely supportive and aimed to removing paraquat from the site of absorption. Increasing its excretion from blood and preventing pulmonary damage is the major thing in management. Hospitalization is required as soon as possible in all cases of suspected paraquat poisoning [1].
Paraquat accumulates selectively in lung tissue and lung injury is exacerbated by administration of oxygen therapy which is mediated through lipid peroxidation [9]. Thus supplementation of oxygen withhold until unless PO2 less than 70 mm of Hg. Administration of 100 percent oxygen resulted in a significantly higher mortality rate when compared to those breathing room air. Steroids used to protect the lung through the reduction of fibrosis or displacing the paraquat from the lung. There is however no observed clear cut benefit. There are some studies suggested a definite trend in benefit with immunosuppressive therapy in patients with moderate to severe poisoning [10–12]. But did not find good evidence of benefit [2]. Steroid, superoxide dismutase, vitamins C and E, N-acetylcysteine, desferrioxamine, and nitrous oxide, has not been proven to be effective [2,4]. few cases reported with same complication, despite advance treatment and supportive care highlight the high mortality rate associated with paraquat poisoning [3]. There is need of large randomized controlled trial to support the role of immunosuppression in paraquat poisoning [12]. However prognosis of paraquat poisoning largely depend on amount of paraquat absorption.
Conclusion
Early diagnosis and aggressive management of paraquat poisoning reduce the mortality. Because small amount of paraquat poison leads to fatal outcome. There is not specific antidote of this poison. Treatment remains supportive in nature, thus causing a high mortality. So we should always think of this poison in case of respiratory and renal damage after unexplained poisoning.
[1]. Sandhu JS, Dhiman A, Mahajan R, Sandhu P, Outcome of paraquat poisoning a five year studyIndian Journal of Nephrology 2003 13:64-68. [Google Scholar]
[2]. Eddleston M, Wilks MF, Buckley NA, Prospects for treatment of paraquat-induced lung fibrosis with immunosuppressive drugs and the need for better prediction of outcome: a systemic reviewQJM 2003 96:809-24. [Google Scholar]
[3]. Singh S, Bambery P, Chaudhry D, Makharia G, Kakkar N, Singh D, Fatal paraquat poisoning: report of two casesJournal of Association of Physicians of India 1999 47(8):831-32. [Google Scholar]
[4]. Suntres ZE, Role of antioxidants in paraquat toxicityToxicology 2002 180(1):65-77. [Google Scholar]
[5]. Saravu K, Sekhar S, Pai A, Barkur AS, Rajesh V, Earla JR, Paraquat - A deadly poison: Report of a case and reviewIndian J Crit Care Med 2013 17:182-84. [Google Scholar]
[6]. Bullivant CM, Accidental poisoning by paraquat: Report of two cases in manBr Med J 1966 1:1272-73. [Google Scholar]
[7]. Kodagoda N, Jayewardene RP, Attygalle D, Poisoning with paraquatForensic Sci 1973 2:107-11. [Google Scholar]
[8]. Zhang , Succesful treatment of paraquat poisoningJ Zhejiang Univ-Sci B (Biomed & Biotechnol) 2012 13(5):413-18. [Google Scholar]
[9]. Olson KR, Poisoning. In: McPhee SJ, Papadakis MA, Tierney LM. edCurrent Medical Diagnosis Treatment 2007 46th edNew YorkMcGraw Hill:1663 [Google Scholar]
[10]. Lin JL, Leu ML, Liu YC, Chen GH, A prospective clinical trial of pulse therapy with glucocorticoid and cyclophosphamide in moderate to severe paraquat- poisoned patientsAm J Respir Crit Care Med 1999 159:357-60. [Google Scholar]
[11]. Lin JL, Lin-Tan DT, Chen KH, Huang WH, Repeated pulse of methylprednisolone and cyclophosphamide with continuous dexamethasone therapy for patients with severe paraquat poisoningCrit Care Med 2006 34:368-73. [Google Scholar]
[12]. Agarwal R, Srinivas R, Aggarwal AN, Gupta D, Immunosuppressive therapy in lung injury due to paraquat poisoning: a meta-analysisSingapore Med J 2007 48:1000-05. [Google Scholar]