Bilateral Carpal Spasm Under Spinal Anaesthesia During Abdominal Hysterectomy: A Case Report
Abhilasha Thanvi1, Udita Naithani2, Sneha Arun Betkekar3, Devendra Verma4, Basant Kumar Dindor5
1 Senior Resident, Department of Anaesthesia, R.N.T Medical College, Udaipur, Rajasthan, India.
2 Professor, Department of Anaesthesia, R.N.T Medical College, Udaipur, Rajasthan, India.
3 Junior Registrar, Department of Anaesthesia, R.N.T Medical College, Udaipur, Rajasthan, India.
4 Professor and Unit Head, Department of Anaesthesia, R.N.T Medical College, Udaipur, Rajasthan, India.
5 Assistant Professor, Department of Anaesthesia, R.N.T Medical College, Udaipur, Rajasthan, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Abhilasha Thanvi, Senior Resident, Department of Anaesthesia, R.N.T Medical College, Chetak Circle, Udaipur, Rajasthan-313001, India. E-mail : mailtanu24@gmail.com
Acute hypocalcaemia is a medical emergency that can have catastrophic implications like tetany, seizures, cardiac arrythmias or laryngospasm if left untreated. We are presenting a case of a 30-year-old female patient undergoing total abdominal hysterectomy with bilateral salpingoopherectomy under spinal anaesthesia. She developed unexpected bilateral carpal spasm intraoperatively which was promptly diagnosed and successfully managed with intravenous calcium administration. We conclude that the anaesthetist should be aware of the clinical presentation of acute hypocalcaemia, its causes and emergency management in the perioperative period to prevent any adverse outcomes.
Carpopedal spasm, Hypocalcaemia, Hyperventilation
Case Report
A 30-year-old female (weight - 55 kilograms, height - 150 cm) was admitted to undergo total abdominal hysterectomy with bilateral salpingoopherectomy for dysfunctional uterine bleeding. Patient’s history, physical examination and routine investigations were unremarkable and spinal anaesthesia was planned for the case.
In the operating room routine monitoring with non invasive blood pressure, ECG and pulse oximetry was applied which showed blood pressure of 126/80 mm Hg, pulse of 68 per minute, respiratory rate 16 per minute, peripheral oxygen saturation of 100% on room air. A 20 gauge I.V. cannula was secured in the patient’s left hand and preloading was done with 500 ml Ringer’s lactate. Spinal anaesthesia was performed with the patient lying in right lateral position using a 25G Quincke’s needle via the midline approach in L3-L4 interspace under all aseptic precautions. A 15mg (3ml) of 0.5% hyperbaric bupivacaine with 25mg tramadol was injected intrathecally. After 5 minutes of spinal injection T6 level of sensory block and Bromage score of 3 (complete motor block) were achieved and surgery was allowed to commence. Intravenous midazolam 2 mg and ondansetron 4 mg were administered at the start of surgery. Oxygen at 5 litre/min was administered using simple mask.
Thirty minutes after the subarachnoid injection, midway through the surgery the patient suddenly complained of nausea and started retching. We reassured the patient and administered dexamethasone 4mg i.v. She looked anxious, but no obvious hyperventilation was evident. 5 min later we noticed carpal spasm on patient’s right hand [Table/Fig-1a] where sphygmomanometer cuff was placed and inflated for measurement. The patient also developed carpal spasm in the other hand soon after [Table/Fig-1b]. We rechecked the level of sensory block which was found to be T6. Chest wall movement was adequate without any dyspnoea and tachypnoea. Chest was clear on auscultation. Oxygen saturation was 100%, blood pressure was 116/80 mm Hg and pulse was 60 per min. ECG was within normal limit. Carpal spasm persisted despite reassurance of the patient. We suspected hypocalcaemia as a cause of carpal spasm and administered 10 ml of calcium {Injection GluciR (Neon laboratories ltd.) each ml of which contains calcium gluconate 50 mg and calcium lactobionate 87.5 mg equivalent to elemental calcium 9 mg} diluted in 200 ml 5% Dextrose as intravenous infusion over 10 min, however, carpal spasm disappeared within 5 min of initiation of calcium infusion [Table/Fig-2a&b]. Remaining surgery was completed without any further complications. On further questioning patient gave a history of occasional cramps of fingers and hands which occurred once in two to three months since 2 years and were relieved by pressing the fingers. These episodes were unrelated to stress or anxiety and she had not sought any medical advice for the same. The patient was transferred to the ICU in fully conscious and stable condition with resolution of signs and symptoms. Physician was consulted postoperatively. No pathological cause for hypocalcaemia could be detected and further investigations revealed serum albumin 3.8 gm/dl, serum calcium 11.2 mg/dl and a normal ECG. On the following day, arterial blood gas analysis showed pH 7.46, pCO2 32mm Hg, pO2 104 mmHg and ionized calcium 3.89 mg/dl. Other electrolyte concentrations were within normal limit.
Carpal spasm in patient’s right hand with inflated sphygmomanometer cuff.
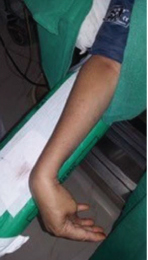
Carpal spasm in patient’s left hand.
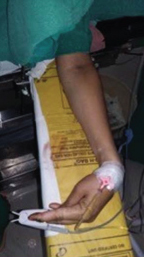
Carpal spasm relieved in both hands after intravenous calcium administration.
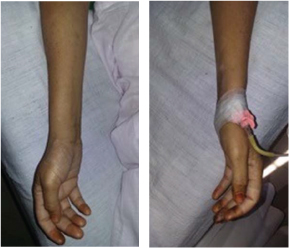
Postoperative course was uneventful and the patient was discharged as per hospital protocol after 7 days.
Discussion
Carpopedal spasm is defined as involuntary contraction of feet and (more commonly) hands observed in hyperventilation, calcium deprivation and tetany [1]. Serum total calcium (normal: 8.0-10.2 mg%, or 2.2-2.5 mmol/L) is present in three forms, as follows: approximately 50% of the calcium is bound with plasma protein (albumin is responsible for 80%), unbound ionized calcium, and 5-10% calcium bound and chelated with plasma anions (phosphoric acid, sulfuric acid, and citric acid) [1,2]. About half of the total calcium is ionized calcium (normal: 4.0-4.6 mg%, or 1.0-1.5 mmol/L) which is physiologically active [3,4]. Clinically hypocalcaemia refers to a decrease in ionized calcium hence ionized calcium should be measured when hypocalcaemia is suspected.
Pathological causes of hypocalcaemia are massive blood transfusion, hypoparathyroidism, renal failure, sepsis, acute pancreatitis, rhabdomyolysis, hypomagnesemia and medication (aminoglycosides, cimetidine and heparin) [3,5]. All these causes were excluded in our case by history, examination and investigations.
Previously cases of carpopedal spasm due to hypocalcaemia have been reported under spinal anaesthesia [2,3]. In these cases patient complained of nausea, headache, perioral numbness and carpal spasm. ECG changes in the form of second degree AV block, bradycardia and T wave inversion were noted in one of the cases [3]. In both cases emergent ABG revealed markedly decreased pCO2, increased pH and hypocalcaemia. In our case facility for ABG was not available on site; therefore we could not document respiratory alkalosis and hypocalcaemia at the time of occurrence of carpal spasm. There was no obvious hyperventilation and ECG was normal in our case.
Postoperatively, total calcium was 11.2 mg/dl which was above normal, this could be attributed to the administration of calcium intraoperatively. Serum albumin was within normal limits. ABG done on the following day showed a slight trend towards respiratory alkalosis pH-7.46, pCO2 -32mm of Hg and borderline hypocalcaemia (ionized calcium-3.89 mg/dl). This suggested a tendency of the patient towards hyperventilation and hypocalcaemia that could be contributory factor for history of cramps that she experienced in her hands. However, intraoperatively we did not observe any obvious hyperventilation. Physician also endorsed the possibility that anxiety could have led to hyperventilation, hypocalcaemia and carpal spasm in this case.
Hyperventilation is an autonomic response to extreme stress, fear or anxiety in which breathing in excess of metabolic requirements results in hypocalcaemia [3,6]. Loss of carbon dioxide drives bicarbonate to combine with hydrogen ions to form carbon dioxide. This causes a decrease in hydrogen ions leading to respiratory alkalosis. Respiratory alkalosis dissociates bound hydrogen ions from albumin, which binds with calcium thereby decreasing the freely ionized portion of total serum calcium by 0.05mmol/l for every 0.1 increase in pH. Hypocalcaemia increases neuronal excitability by decreasing the threshold potential needed to activate the sodium channel due to alteration in the electrical state of the channel protein [5].
The hallmark of acute hypocalcaemia is neuromuscular irritability. Patients often complain of numbness and tingling in their finger tips, toes and perioral region and may present as carpopedal spasm. Clinically, neuromuscular irritability can be demonstrated by eliciting Trousseaus’ sign or Chvostek’s sign. Trousseaus’ sign presents as carpal spasm secondary to ulnar and median nerve ischemia in response to the inflation of the sphygmomanometer cuff to 20mm Hg above systolic blood pressure [7]. In present case also carpal spasm first appeared in the limb after inflation of sphygmomanometer cuff then in the other limb. Moreover, pedal spasm did not occur due to motor blockade of lower extremities under spinal anaesthesia which was consistent with other case reports [2,3,6]. We did not observe any QT interval prolongation, although this lacks sensitivity for the diagnosis of hypocalcaemia [8].
Acute onset hypocalcaemia is a medical emergency that requires prompt attention as patient may present with tetany, seizures, cardiac arrythmias or laryngospasm [9]. Treatment with intravenous calcium is indicated without waiting for measurement of serum calcium levels and should be continued until signs and symptoms of neuromuscular irritability subside [10], as executed in our case as well. Calcium gluconate is the preferred intravenous salt which contains 90mg of elemental calcium per 10ml ampoule. A 1-2 ampoules diluted in 150ml of 5% dextrose is infused over 10min [11].
Conclusion
In conclusion we managed a case of acute onset carpal spasm in spinal anaesthesia which was promptly diagnosed and successfully treated with intravenous calcium administration and further complications were prevented. This report highlights that anaesthesiologist should be aware of the possibility of acute onset hypocalcaemia during perioperative period as its timely recognition and immediate management is vital for patient safety.
[1]. Kern B, Byrd RP, Rosh AJ. Hyperventilation Syndrome Clinical Presentation. http://emedicine.medscape.com/article/807277-clinical [Google Scholar]
[2]. Kumar N, Podder S, Sinha T, Puri GD, Acute hyperventilation leading to hypocalcaemia during spinal anaesthesiaSouth Afr J Anaesth Analg 2004 10:29-30. [Google Scholar]
[3]. Moon HS, Lee SK, Chung JH, In CB, Hypocalcaemia and hypokalemia due to hyperventilation syndrome in spinal anaesthesia – a case reportKor J Anesth 2011 61:519-23. [Google Scholar]
[4]. Lebowitz MR, Moses AM, HypocalcaemiaSemin Nephrol 1992 12:146-58. [Google Scholar]
[5]. Bushinsky DA, Monk RD, Electrolyte quintet: CalciumLancet 1998 352:306-11. [Google Scholar]
[6]. Parasa M, Saheb SM, Vemuri NN, Cramps and tingling: A diagnostic conundrumAnaesthesia Essays and Researches 2014 8(2):247-49. [Google Scholar]
[7]. Bansal T, Hooda S, Hyperventilation causing symptomatic hypocalcaemia during labour in a parturientEgyptian Journal of Anaesthesia 2013 29:333-35. [Google Scholar]
[8]. Rumancik WM, Denlinger JK, Narworld MR, The QT interval and serum ionized calciumJAMA 1978 240:366-68. [Google Scholar]
[9]. Mishra S, Bhat R, Anita Mahesh N, Kundra P, Hemavathy B, Badhe A, Postpartum Cardiomyopathy With Severe Hypocalcaemia And TetanyInternet Journal of Anesthesiology 2007 12(1)ISPUB.com [Google Scholar]
[10]. Bringhurst FR, Demay MB, Kronenberg HM, Hormones and disorders of mineral metabolism. In: Wilson JD, Foster DW, Kronenberg HM, Larsen PRWilliams textbook of endocrinology 1998 PhiladelphiaWB Saunders:1155-1209. [Google Scholar]
[11]. Cooper MS, Diagnosis and management of hypocalcaemiaBMJ 2008 336:1298-302. [Google Scholar]