Soft tissue deficiencies and defects around dental implants have been observed frequently. Soft-tissue defects after implant procedures originate from the process of modelling of periimplant mucosa and often cause aesthetic disharmony, food debris accumulation and soft tissue shrinkage. Periimplant mucogingival surgery focuses on creating an optimum band of keratinized tissue resulting in soft tissue architecture similar to the gingiva around natural teeth. A 23-year-old male reported to the Department of Periodontology with a complaint of gum soreness, foul smell and food accumulation at a site where a 3.75 x 11.5mm implant was placed previously. On clinical examination, fenestration of tissue above the cover screw was observed and there appeared to be a keratinized tissue of 1mm surrounding the implant. The case was managed by use of a rotated double-pedicle flap during second-stage implant surgery to correct the soft-tissue fenestration defect and to obtain a keratinized periimplant soft tissue. A periosteal bed was prepared by giving a horizontal incision at the mucogingival junction to a depth of 4 mm. Two split-thickness keratinized pedicles were dissected from the mesial and distal interproximal tissues near the implant. After rotation, both the pedicles were sutured to each other mid-buccally and the pedicles were rigidly immobilized with sutures. At 1 month, there was a 3mm band of stable and firm keratinized tissue over the underlying tissues. The procedure resulted in an aesthetic improvement due to enhanced soft tissue architecture and optimum integration between the peri-implant soft tissue and the final prosthesis.
Dental implants, Fenestration, Gingiva, Pedicle Flap
Case Report
In March 2014, following a delayed-loading protocol, a 3.75 x 11.5 mm implant (TouaregTM, Adin, Alon-Tavor, Israel) was placed in the left maxillary central incisor region. The subject, a 23-year-old male patient, was asked not to chew and brush the surgical area for the first two weeks postoperatively and subsequent soft tissue healing was uneventful. Showing signs of a failing implant after two months, the patient came to the Implantology clinic complaining of pus discharge, pain and swelling. A periapical radiograph [Table/Fig-1] of the region revealed an angular radiolucency at the coronal region of the implant. A repeat surgery was planned and surgical exposure of the coronal portion of the implant with full-thickness buccal and palatal flaps revealed a moderate osseous defect with loss of implant stability. Grade I mobility (according to the Misch’s Clinical Implant Mobility Scale) was detected with respect to the implant placed by using two rigid instruments to apply a labio-lingual force. The original osteotomy site was deepened by 3mm by using an undersized drilling sequence and the same implant was placed into the smaller osteotomy site with a pronounced buccal inclination for achieving greater primary stability. Guided bone regeneration was then performed by using a bone graft (0.25 cc; Rocky Mountain Tissue Bank, Aurora, Colorado, USA) and a membrane (PerioCol®, Eucare, Chennai, India) to augment a buccal defect seen at this time. Primary closure was obtained and the implant was allowed to heal for six months.
IOPA of the surgical site 2-months after surgery showing a 3.75 x 11.5mm implant with vertical bone loss (dotted red line).

At the completion of this period, the patient reported to the Department of Periodontology with a complaint of gum soreness, foul smell and food accumulation at the site. On clinical examination, fenestration of tissue above cover screw was observed and the cover screw was partially visible [Table/Fig-2], though the implant was stable. The lingual margin of the perforation showed an overlap with the border of the cover screw; the presence of mild gingival inflammation, bleeding on probing soft-debris accumulation and suppuration were also noted. The implant appeared to be in a more apical and buccal position than normal however, no clinical signs of mobility were seen. The probing depth measurement was 1 mm and there appeared to be a keratinized tissue of 1mm surrounding the implant.
At initial presentation, fenestration of tissue above cover screw was observed and the cover screw was partially visible. There appeared to be a keratinized tissue of 1mm surrounding the implant; the presence of mild gingival inflammation, bleeding on probing soft-debri accumulation and suppuration were also noted.

Procedure
In this subject, augmentation of the periimplant soft-tissue was planned primarily to improve aesthetics and to alter the soft tissue architecture for an optimal prosthetic outcome. There was a spontaneous early exposure of the implant through the soft tissue as well; implants with soft-tissue fenestrations should be completely exposed with appropriate surgical therapy as soon as possible after the perforation is observed [1]. Ideally, resective procedures such as gingivectomy would have been an ideal procedure to thoroughly expose the implant. However, there was an abundant proximal soft tissue (~4-5mm) above the implant level and a decision was made to manipulate this soft tissue to augment the periimplant mucosa at the time of the second-stage implant surgery. After securing local anaesthesia, a periosteal bed was prepared by giving a horizontal incision at the mucogingival junction to a depth of 4mm. Split-thickness dissection was performed to detach the mucosa and adherent fibrous tissue apically and laterally thus exposing the entire periosteal bed [Table/Fig-3]. Two split-thickness keratinized pedicles were dissected from the mesial and distal interproximal tissues near the implant [Table/Fig-4,5] and their widths (~4mm) were dictated by the apico-coronal height of the periosteal bed. Extreme care was taken to keep the pedicles intact with their bases and tension-releasing cutback incisions were given into the base of pedicle in the proximal directions to permit rotation of the pedicles into the periosteal bed [Table/Fig-4]. At this point, the cover screw of the implant was removed and was replaced with a gingival former. After rotation, both the pedicles were sutured to each other mid-buccally and the pedicles were rigidly immobilized with sutures [Table/Fig-5]. Sutures were removed 10 days after surgery and at one month, there was a 3mm band of stable and firm keratinized tissue over the underlying tissues and gingival former [Table/Fig-6]. At two months, the band of keratinized tissue was found to be healthy and stable enough to permit subsequent prosthetic procedures. A harmonious keratinized soft tissue margin with the stock abutment [Table/Fig-7] and the cemented laboratory-fabricated crown [Table/Fig-8] was noted and the patient was satisfied with the final results.
A periosteal bed (dotted and shaded area) was prepared by giving a horizontal incision at the mucogingival junction to a depth of 4 mm. Two split-thickness keratinized pedicles were dissected from the mesial and distal interproximal tissues near the implant (broken lines) and their widths (~4mm) were dictated by the apico-coronal height of the periosteal bed.

Extreme care was taken to keep the pedicles intact with their bases and tension-releasing cutback incisions were given into the base of pedicle in the proximal directions to permit rotation of the pedicles into the periosteal bed.
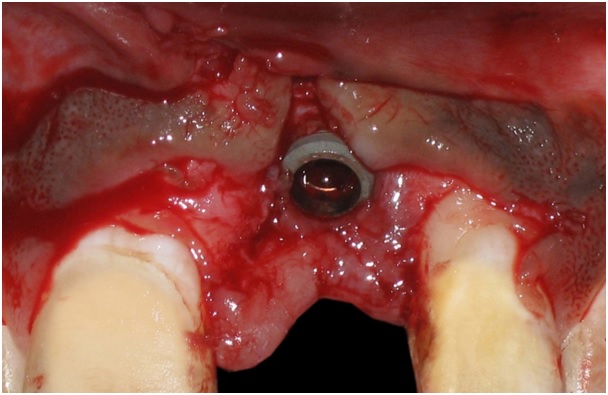
After rotation, both the pedicles were sutured to each other mid-buccally and the pedicles were rigidly immobilized with sutures.

At 1 month, there was a 3mm band of stable and firm keratinized tissue over the underlying tissues and gingival former.

A harmonious keratinized soft tissue margin with the stock abutment was observed.
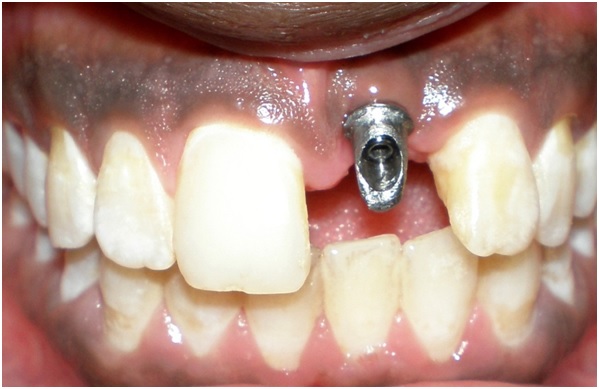
The keratinized soft tissue margin around the cemented laboratory-fabricated crown was healthy and firm. The patient was satisfied with the final results.

Discussion
Soft tissue deficiencies and defects around dental implants have been observed frequently [2]. The quantity, quality and position of the existing periimplant bone are an important determinant in subsequent soft tissue development and maintenance of soft tissue height [3]. Soft-tissue defects after implant procedures originate from the process of modelling of periimplant mucosa [3,4]. About 0.7mm and 0.6mm of bone resorption and soft tissue recession is believed to occur in the buccal aspect of the implants during the period between implant placement and abutment connection [4]. In this context, a band of keratinized tissue around an implant is believed to be protective against periimplant bone loss [5]. Muller et al., suggested that thin mucosa is friable and recedes more readily following mechanical stress and surgical procedures than thick mucosa [6]. Soft tissue recessions and defects often cause aesthetic disharmony, patient dissatisfaction and soft tissue shrinkage after one month of healing [5,6].
Periimplant mucogingival surgery focuses on creating an optimum band of keratinized tissue resulting in soft tissue architecture similar to the gingiva around natural teeth [3]. A plethora of studies have correlated the presence of keratinized and attached tissues with improved soft tissue health, prognosis and patient satisfaction [7]. The repertoire of mucogingival procedures performed around dental implants including Connective Tissue Graft (CTG), Coronally Advanced Flap (CAF), connective tissue graft in combination with an envelope flap or pouch, Free Gingival Graft (FGG) and Pediculated Connective Tissue Graft (PCTG) are known to achieve aesthetic gingival contours with an increase in the width of the keratinized tissues [3,7,8]. At the same time, unusual presentations such as vestibular implant fenestrations can also be corrected by using mucogingival procedures [9].
In Periodontology, a pedicle graft is a mucogingival flap which serves as a soft tissue graft while maintaining an intact blood supply from the donor site [3,7]. A lateral pedicle graft or a lateral repositioned flap is a rotated pedicle graft that can be moved laterally while pivoting around a point [3,7,10]. The "oblique rotational flap", the "rotation flap", and the "transpositioned flap" are primarily modifications of the lateral pedicle graft in incision design and flap mobilisation [11]. When flaps are mobilised mesial and distal to the defect, the flap is a “double pedicle flap” [11,12]. These flap designs have been incorporated into Implantology as well; for inter-implant papilla reconstruction, a technique described by Palacci [3] utilizes a rotated pedicle flap while Grossberg [13] suggested using a double-pedicle flap. The vascularised interpositional connective tissue graft [7] which is used to correct soft tissue defects around implants is also a rotated pedicle as it is “curved” into the recipient site and retains a patent vascular supply.
Unexpected early implant exposure is a result of apical displacement of the soft tissue margin as a response to the modelling process of the periimplant hard and soft tissues [1,4,6,14]. Tal et al., as a part of their study have classified mucosa covering endosseous implants into four classes; Class 0: mucosal covering over the implant is intact, Class I: a breach in the mucosa covering the implant is observed but the implant surface cannot be seen. Class II: mucosa above the cover screw is fenestrated, and the cover screw is visible. Class III: cover screw is visible and in some parts, the borders of the perforation aperture overlap the borders of the cover screw. Class IV: cover screw is completely exposed. In their study, there was a statistically significant difference between bone loss associated with intact (Class 0) and exposed soft tissues. As the anatomy of the perforated lesions could also act as a plaque-retentive site thereby increasing bone loss, they also recommend that partially exposed implants should be completely exposed with appropriate surgical therapy as soon as possible after the perforation is observed.
In Implantology, the need for soft tissue augmentation around endosseous implants remains a controversial and ambiguous topic. Levine et al., have stated that a thick tissue biotype is desirable and the decision to convert a thin tissue to a thick tissue needs surgical consideration through soft tissue grafting for more predictable surgical and prosthetic outcomes [8]. There are also situations where it is beneficial to have keratinized tissues and others in which it is wholly unnecessary [5,8,15]. Greenstein and Cavallaro have identified six situations where augmentation of periimplant soft tissue may be beneficial: 1) Chronically inflamed sites, despite oral hygiene instruction and periodontal therapy; 2) Locations with ongoing recession or continued loss of clinical attachment or bone; 3) Sites where the patient complains of soreness when brushing, despite the appearance of gingival health; 4) Dental history suggesting predisposition to periodontitis or recession; 5) Patients noncompliant with periodic professional maintenance; and 6) To improve aesthetics [15]. A recent systemic review [16] and a prospective comparative study [17] have stated that a lack of adequate keratinized mucosa around endosseous dental implants is associated with more plaque accumulation and tissue inflammation and an adequate band of keratinized mucosa was related with less plaque accumulation and mucosal inflammation. Thus, the incidence of peri-implantitis can be lowered by providing a firmer and resilient tissue phenotype [18].
Soft tissue augmentation procedures around an endosseous implant have been traditionally performed by using the patient’s palatal connective tissue graft or free gingival graft as the donor material [3,7,8]. However, harvesting palatal grafts have the disadvantages of bleeding, postoperative pain, local morbidity, compromised aesthetic outcome and secondary surgical site [7,8]. In contrast, laterally positioned pedicle graft is relatively easy to perform, produces excellent tissue aesthetics, and a second surgical site is not required [10,13]. A recent case report describes the use of a bilateral rotated pedicled lingual flap to augment keratinized tissue on the anterior mandibular ridge prior to implant placement [19]. A similar variant of this procedure is the mandibular connective tissue pedicle flap [20] which includes the elevation of a pediculate connective tissue flap to increase soft tissue volume during implant placement. Both the procedures report adequate soft tissue augmentation and acceptable aesthetic outcomes.
Interestingly, fenestrations and fistula formation are the most frequently reported soft tissue complications around implants [21]; however, there is a definite paucity of case reports on the management and correction of “pure” soft tissue periimplant fenestrations as opposed to the management of Bone Plate Fenestrations (BPFs) [5,21]. A recent case report describes the use of two mucogingival surgical techniques to treat vestibular implant fenestration in the visible area of the mouth [9]. A study by Zucchelli et al., found that a combination of coronally advanced flap, Connective Tissue Graft (CTG) and final restoration was effective in the coverage of buccal soft-tissue defects around single dental implants [22]. Burkhardt et al., however could not achieve complete implant soft tissue dehiscence coverage in any of the sites following treatment with the same combination of coronally advanced flap in combination with a free connective tissue graft [23]. The authors are not aware of published specific reports on the use of pedicle or double-pedicle flaps in the concomitant correction of a soft-tissue fenestration defect with periimplant soft-tissue augmentation, like the case here described.
Despite the limitation of being a single case report, the rotated double pedicle flap seems to offer an ideal periimplant soft tissue architecture and excellent soft tissue-prosthesis integration. This technique however may be surgically demanding and may require competence of a periodontist to perform. Mucogingival procedures around dental implants are known to give good results during the initial wound-healing phase [8], but the long-term results raise the question of what are the most effective techniques for periimplant soft tissue management [21]. Further evaluation of this procedure in a larger cohort with long-term follow-up is required and the use of this technique in combination with regenerative biomaterials such as platelet derivatives is an exciting possibility.
Conclusion
An appropriate surgical intervention using mucogingival surgery can be performed to correct aesthetic and soft tissue deformities around an implant. The technique described here is novel and utilizes the surrounding periimplant tissue to augment the keratinised tissues around an implant. However, case selection is paramount and the abundant presence of periimplant soft tissue is mandatory to carry out this procedure.
[1]. Tal H, Artzi Z, Moses O, Nemcovsky CE, Kozlovsky A, Spontaneous early exposure of submerged endosseous implants resulting in crestal bone loss: a clinical evaluation between stage I and stage II surgeryInt J Oral Maxillofac Implants 2001 16(4):514-21. [Google Scholar]
[2]. Esposito M, Maghaireh H, Grusovin MG, Ziounas I, Worthington HV, Soft tissue management for dental implants: what are the most effective techniques? A Cochrane systematic reviewEur J Oral Implantol 2012 5(3):221-38. [Google Scholar]
[3]. Palacci P, Nowzari H, Soft tissue enhancement around dental implantsPeriodontol 2000 2008 47:113-32. [Google Scholar]
[4]. Cardaropoli D, Gaveglio L, Gherlone E, Cardaropoli G, Soft tissue contour changes at immediate implants: a randomized controlled clinical studyInt J Periodontics Restorative Dent 2014 34(5):631-37. [Google Scholar]
[5]. Kaufmann R, Bassetti R, Mericske-Stern R, Enkling N, Enlargement of keratinized peri-implant mucosa at the time of second stage surgery (re-entry)Swiss Dent J 2014 124(12):1315-31. [Google Scholar]
[6]. Müller HP, Eger T, Masticatory mucosa and periodontal phenotype: a reviewInt J Periodontics Restorative Dent 2002 22(2):172-83. [Google Scholar]
[7]. Bhatavadekar N, Peri-implant soft tissue management: Where are we?J Indian Soc Periodontol 2012 16(4):623-27. [Google Scholar]
[8]. Levine RA, Huynh-Ba G, Cochran DL, Soft tissue augmentation procedures for mucogingival defects in aesthetic sitesInt J Oral Maxillofac Implants 2014 29(Suppl):155-85. [Google Scholar]
[9]. Dominguez E, Vazquez M, González-Martín O, Alandez J, Mucogingival therapy to treat implant fenestration in the esthetic zone: a case report after 2 year follow upInt J Esthet Dent 2014 9(1):40-53. [Google Scholar]
[10]. Espinel MC, Caffesse RG, Comparison of the results obtained with the laterally positioned pedicle sliding flap-revised technique and the lateral sliding flap with a free gingival graft technique in the treatment of localized gingival recessionsInt J Periodontics Restorative Dent 1981 1(6):30-37. [Google Scholar]
[11]. Roccuzzo M, Bunino M, Needleman I, Sanz M, Periodontal plastic surgery for treatment of localized gingival recessions: A systematic reviewJ Clin Periodontol 2002 29:17894 [Google Scholar]
[12]. Grupe H, Modified technique for the sliding flap operationPeriodontol 1966 37:491-95. [Google Scholar]
[13]. Grossberg DE, Interimplant papilla reconstruction: assessment of soft tissue changes and results of 12 consecutive casesJ Periodontol 2001 72(7):958-62. [Google Scholar]
[14]. Bengazi F, Lang NP, Caroprese M, Urbizo Velez J, Favero V, Botticelli D, Dimensional changes in soft tissues around dental implants following free gingival grafting: an experimental study in dogsClin Oral Implants Res 2015 26(2):176-82. [Google Scholar]
[15]. Greenstein G, Cavallaro J, The clinical significance of keratinized gingiva around dental implantsCompend Contin Educ Dent 2011 32(8):24-31. [Google Scholar]
[16]. Lin GH, Chan HL, Wang HL, The significance of keratinized mucosa on implant health: a systematic reviewJ Periodontol 2013 84(12):1755-67. [Google Scholar]
[17]. Boynueğri D, Nemli SK, Kasko YA, Significance of keratinized mucosa around dental implants: a prospective comparative studyClin Oral Implants Res 2013 24(8):928-33. [Google Scholar]
[18]. Adibrad M, Shahabuei M, Sahabi M, Significance of the width of keratinized mucosa on the health status of the supporting tissue around implants supporting overdenturesJ Oral Implantol 2009 35(5):232-37. [Google Scholar]
[19]. Herford AS, Tandon R, Pivetti L, Cicciù M, Pedicled lingual flap to provide keratinized tissue regeneration over dental implants: a description of the technique and a case reportJ Oral Implantol 2015 41(2):196-99. [Google Scholar]
[20]. Peñarrocha-Diago M, Gómez-Adrián MD, Balaguer-Martínez J, García-Mira B, Mandibular connective tissue pedicle flaps in implant dentistry: report of three casesJ Oral Implantol 2007 33(3):127-32. [Google Scholar]
[21]. Caplanis N, Romanos G, Rosen P, Bickert G, Sharma A, Lozada J, Teeth versus implants: mucogingival considerations and management of soft tissue complicationsJ Calif Dent Assoc 2014 42(12):841-58. [Google Scholar]
[22]. Zucchelli G, Mazzotti C, Mounssif I, Mele M, Stefanini M, Montebugnoli L, A novel surgical-prosthetic approach for soft tissue dehiscence coverage around single implantClin Oral Implants Res 2013 24(9):957-62. [Google Scholar]
[23]. Burkhardt R, Joss A, Lang NP, Soft tissue dehiscence coverage around endosseous implants: a prospective cohort studyClin Oral Implants Res 2008 19(5):451-57. [Google Scholar]