Necrotizing Sialometaplasia of the Hard Palate: A Rare Entity of Dilemma on Cytology, Confirmatory on Histopathology
Archana Shetty1, Vijaya Chowdappa2, Chidananda R. Devasamudra3, Jayalakshmi Valligari Janardhan4
1 Assistant Professor, Department of Pathology, Sapthagiri Institute of Medical Sciences and Research Centre, Bangalore, India.
2 Professor and Head, Department of Pathology, Sapthagiri Institute of Medical Sciences and Research Centre, Bangalore, India.
3 Assistant Professor, Department of Ear, Nose and Thraot, Sapthagiri Institute of Medical Sciences and Research Centre, Bangalore, India.
4 Tutor, Department of Pathology, Sapthagiri Institute of Medical Sciences and Research Centre, Bangalore, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Archana Shetty, Department of Pathology, Sapthagiri Institute of Medical Sciences and Research Centre, Hesaraghatta Main Road, Bangalore-560090, India.
E-mail: archanashetty2924@gmail.com
Necrotizing sialometaplasia is a rare, benign reactive necrotizing lesion, involving sites where salivary gland tissue is usually present. The importance of this lesion is that it mimics malignancy clinically leading to treatments ranging from conservative excision to total maxillectomy. Cytologically and histologically also the lesion is often confused with neoplasms. We present a case of a lady with a hard palatal swelling, which was non – ulcerative unlike typical cases of necrotizing sialometaplsia. FNAC features made us strongly suspect a low grade mucoepidermiod carcinoma, following which the swelling was excised. Histopathology came to the rescue, on which the final diagnosis of necrotizing sialometaplasia of the hard palate was made.
Necrotizing siaometaplasia is often misdiagnosed by the inexperienced cytologist, with histopathological examination being confirmatory. We also emphasize the fact that lesions like necrotizing sialometaplasia need a high degree of suspicion along with clinical co relation before subjecting the patient to unnecessary surgical procedures.
FNAC, Minor salivary gland, Malignancy, Mucoepidermiod carcinoma, Oral lesions
Case Report
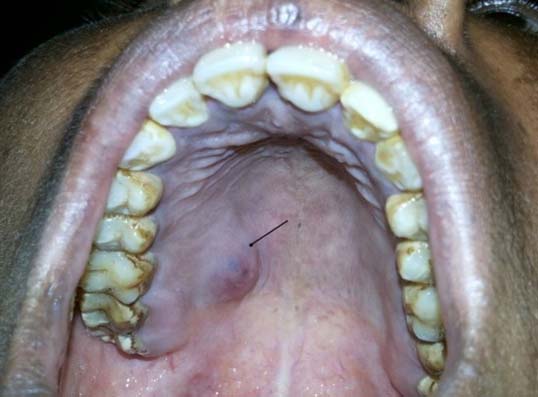
A 35-year-old female presented to the ENT outpatient Department of Sapthagiri Institute of Medical Sciences and Research Centre, Hesaraghatta, Bangalore, with a tiny swelling on the hard palate, noticed by her since two weeks. The patient had no significant past clinical history other than undergoing a molar tooth extraction two weeks before. On clinical examination a submucosal lesion measuring 1x0.5 cm was noted on the posterior aspect of the hard palate [Table/Fig-1]. The swelling was tender with mild radiating pain. Suspecting it to be a minor salivary gland neoplasm, FNAC was done, which yielded a transparent mucoid aspirate. Cytology of the smears showed sheets, tiny clusters and groups of squamous cells, which appeared benign [Table/Fig-2a&b] mixed with these was mild lymphocytic infiltrate in a background of pink eosinophilic material along with occasional salivary gland acini. A diagnosis of a benign salivary gland lesion was made, however a caution to rule out low grade mucoepidermoid carcinoma was conveyed to the surgeon. An excisional biopsy of the same was done. H & E sections showed a lining of stratified squamous epithelium along with foci of minor salivary gland tissue with preserved lobular architecture [Table/Fig-3a&b]. Few necrotic salivary gland acini were seen with the adjacent ducts being cystically dilated and undergoing squamous metaplasia of the lining epithelium. Also, noted was moderate chronic inflammatory infiltrate of lymphocytes and cholesterol clefts [Table/Fig-4a&b]. Meyer’s mucicarmine and PAS stain were negative for intracellular mucin, ruling out the possibility of mucoepidermoid carcinoma. A diagnosis of Necrotizing sialometaplasia was made. The patient had an uneventful recovery, after which she came for a follow up four weeks later and the lesion had regressed completely.
Submucosal nodule on the posterior aspect of the hard palate-Arrow.
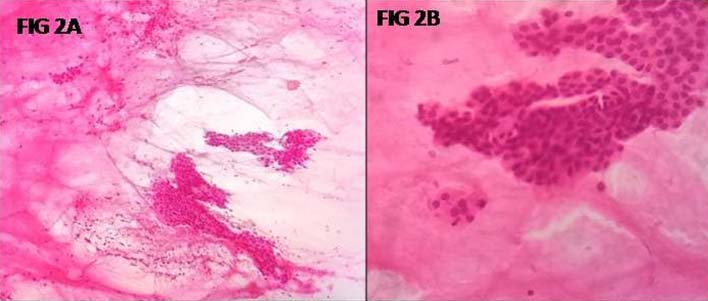
FNAC smears showing streaks of mucoid material along with sheets of squamous cells and few acinar cells: a) (H&E stain, 100X), higher magnification of the cells; b) (H&E stain, 400X)
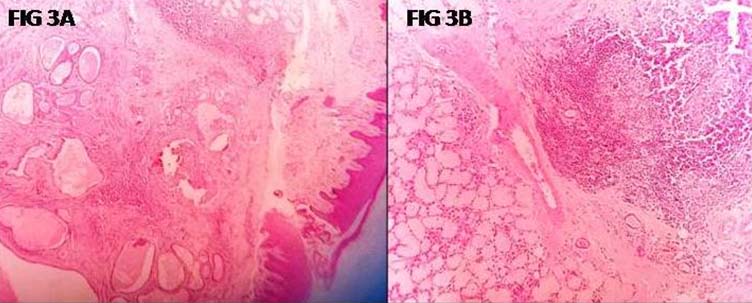
Histopathology of the lesion showing a lining of stratified squamous epithelium: a) (H&E, 40X), Higher magnification showing the retained lobular architecture and chronic inflammation; b) (H&E, 400X)
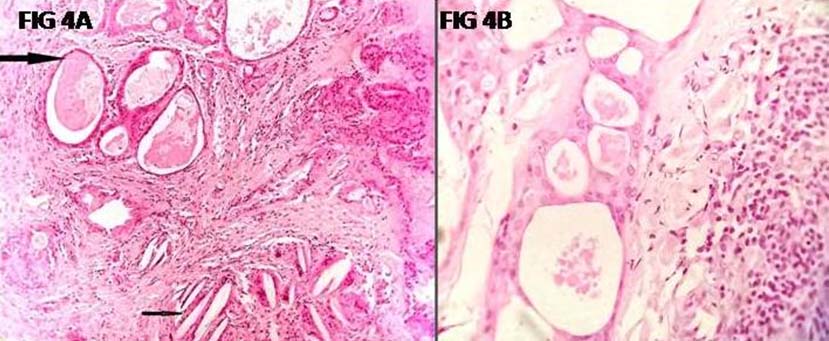
Lesion showing dilated ducts filled with mucin and lined by metaplastic squamous epithelium (upper Arrow) along with cholesterol clefts (lower arrow) and few degenerating salivary gland acini: a) (H&E 100X), higher magnification showing the cystically dilated ducts; b) (H&E, 400X)
Discussion
Necrotizing sialometaplasia (NS) was first described by Abrams et al., in the year 1973 as a reactive necrotizing inflammatory process. Although it mainly involves the minor salivary glands of the hard palate, cases have also been described in the nasal cavity, gingival, incisor canal, retromolar area, tonillar fossa lips, sinuses, larynx and the trachea, sites where the salivary gland tissue is present [1–4].
The lesion can occur in any age group with the mean age of 50 years in men and 36 years in women [3]. The patient in our case was a 35-year-old female. Ischemia of the blood vessels, leading to the infarct of salivary gland tissue is the most commonly postulated aetiology of this lesion [5]. Local anaesthesia, ill fitting dentures, history of recent tooth extraction, cocaine use, surgical procedures combined with radiation therapy and upper respiratory tract infections are documented as the precipitating factors [1]. The typical manifestation of necrotizing sialometaplasia is a deep ulcer, but our patient presented with an intact submucosal palatal nodule, which was probably presentation at a very early stage. NS can be divided into five histologic stages: infarction, sequestration, ulceration, the reparative stage, and healed stage. Moreover, according to Imbery and Edwards, squamous metaplasia of the salivary ducts and coagulation necrosis of the acini is observed in early lesions and reactive fibrosis during the late stage of NS [5].
FNAC is a simple procedure for the diagnosis of accessible oral lesions. Aspirate of NS shows squamous metplasia and epithelial atypia [6]. Such cytological features on FNAC smears often mislead the cytologists towards a diagnosis of malignancy. The high cellularity in our case along with areas of mucous and squamous metaplasia made us strongly suspect low grade mucoepidermoid carcinoma. Aspirates of necrotizing sialometaplasia can also show degenerative changes, nuclear pyknosis and necrotic material in the background on smears closely mimicking well differentiated squamous cell carcinomas [6].
Histopathological features of this lesion include ulceration of the overlying epithelium, vascular proliferation, chronic inflammation and partial necrosis of the salivary glands, with squamous metaplasia of the adjacent ducts and acini along with pools of mucin. Mucous cells can often be seen within the salivary gland lobules, masquerading a low grade mucoepidermoid carcinoma cytologically. However, preservation of lobular architecture of the glands is the single most feature of necrotizing sialometaplasia distinguishing it from neoplasms, in particular mucoepidermoid carcinoma. Thus histopathology is the mainstay in the diagnosis of this lesion. This diagnosis, when required can be supplemented by inmmunohistochemistry, showing low MiB -1 (Ki- 67) reactivity, focal to absent immunoreactivity for p53 and the presence of calponin positive myoepithelial cells [2,3].
Necrotizing sialometaplasia is a self limiting condition, the lesion often resolving spontaneously presumably after the ischemic injury heals. The suspected factor in our case could have been the tooth extraction process that triggered the ischaemia. The lesion has often been mistaken for malignancy in the past like in our case [2,4]. Reports of malignant tumours like adenoid cystic carcinoma, squamous cell carcinoma, angiocentric T-cell lymphoma and necrotizing sialometaplasia co-existing have been documented [7,8] making excision biopsy the mainstay of diagnosis. Also, it is always necessary to co relate the patients clinical history before unnecessarily subjecting the patient to mutilating surgery in case of necrotizing sialometaplasia.
Conclusion
The clinicians and pathologists must be aware of this lesion as this condition can often mimic malignancies both clinically and histologically. FNAC may not always give a correct diagnosis as in our case. Adequate biopsy as well as a good clinical history from the patient can give clues to the diagnosis, avoiding overtreatment in such cases, aiding in better patient care.
[1]. Uppal N, Baliga M, Necrotizing sialometaplasia: A rare lesion that mimics oral cancer clinically and histopathologicallyOtolaryngol Pol 2014 68(3):154-56. [Google Scholar]
[2]. Alves MGO, Kitakawa D, Carvalho YR, Cabral LAG, Almeida JD, Necrotizing sialometaplasia as a cause of non-ulcerated nodule in the hard palate: a case reportJournal of Medical Case Reports 2011 5(1):406 [Google Scholar]
[3]. Krishna S, Ramnarayan BK, Necrotizing sialometaplasia of palate: a case reportImaging Science in Dentistry 2011 41(1):35-38. [Google Scholar]
[4]. Dioguardi M, Santarelli A, Compilato D, Campisi G, Muzio LL, Salivary gland tumours in patients with necrotizing sialometaplasia: a case seriesAnnali de Stomatologica (Roma) 2013 4(Suppl 2):16 [Google Scholar]
[5]. Garcia NG, Oliveira DT, Faustino SE, Azevedo AL, Necrotizing sialometaplasia of palate: a case reportCase Reports in Pathology 2012 2012:679325 [Google Scholar]
[6]. Orel S, Sterret FG, Whitaker D, Chapter 4. Head and Neck: salivary glands in Fine Needle Aspiration Cytology Elsevier 2010 Fourth Edition:54-56. [Google Scholar]
[7]. Lee DJ, Ahn HK, Koh ES, Rho YS, Chu HR, Necrotizing Sialometaplasia Accompanied by Adenoid Cystic Carcinoma on the Soft PalateClinical and Experimental Otorhinolaryngology 2009 2(1):48-51. [Google Scholar]
[8]. Dominguez-Malagon H, Mosqueda-Taylor A, Cano-Valdez AM, Necrotizing sialometaplasia of the palate associated with angiocentric T-cell lymphomaAnnals Of Diagnostic Pathology 2009 13(1):60-64. [Google Scholar]