Anaesthesiology is branch of medical forte which has revealed significant changes in treatment modalities like newer anaesthetic drugs, devices which made to increase direct anaesthetic expenses in health care setup [1,2]. Expenditure on anaesthesia drugs is over one-third of the non-professional costs of anaesthesia care, and about 10% of hospital’s drug budget [3,4].
Pharmacoeconomics helps to analyse costs of drugs to health care systems and society [5]. It is used to identify measure and compare costs, risks, and benefits of programmes, therapies, and determine which strategies produce the best outcomes for the resources allocated. Thus, the purpose of pharmacoeconomics should not be limited to establishing the least expensive drug therapy, but should identify total cost of treatment [6].
Pharmaceutical wastage is major concern in anaesthesia department hence reduction of operating expenditure is common and a possible target for cost-reduction approaches [7,8]. Targeting to reduce unutilized/unused drug amount is particularly striking since it can reduce financial burden in health sector [9]. Even though a variety of factors like deviation in patient responses, hospital protocol lead to difficulties to avoid anaesthetic drug excess, approach for decrease in unutilized/unused drugs may condense cost without considerable effects on patient outcomes [8]. It may be possible to measure rational amounts of drugs needed before a procedure while better preserving unused drugs under most favourable and sterile environment [10]. Un-utilized drug is particularly common with intravenous drugs as these drugs, instead of inhaled anaesthetic agents, are packaged in discreet amounts [11]. For patient’s safety to avoid infection, partially used ampoules and syringes are discarded at the end of a procedure in most of health set up. Unused syringes are frequently discarded too. For the purpose of study, total un-utilized drug amount is the quantity of drug left in syringes, ampoules, or IV bags that have not been entirely utilized however unable to reuse due to expiration or contamination concerns [7]. This study also considers the un-used resources that are discarded due to safety concerns.
This study aimed at suggesting various strategies to reduce in cost of anaesthesia through a decrease in drug wastage without compromising on the quality of care. This is prospective observational study to analyse the amount of anaesthetic drug wastage in operating theatre as well as the financial implications to the hospital due to wastage of drugs and suggest appropriate steps to prevent it.
Materials and Methods
This study was conducted in B.J. Government medical college and Sassoon General Hospital in Pune. It was conducted after obtaining approval from Ethics committee. The study was approved by institutional ethics committee and carried out according to the Indian Council of Medical Research (ICMR) Guidelines [12] for Biomedical Research in Humans (2006); and in compliance with the International Conference on Harmonisation/Good Clinical Practice (ICH/GCP) Guidelines [13] and permission from anaesthesia department was taken. It was conducted from July – September 2014 in Department of Anaesthesia.
Two hundred cases were recorded in above given period undergoing surgical procedures under general anaesthesia while surgical procedures conducted under regional, spinal and local anaesthesia were excluded. Intravenous drugs including pre-anaesthetic and anaesthetic agents were considered only while inhalational anaesthetic drugs were excluded. Patients belonging to age greater than 12 years were included in the study.
The drug preparation and the doses administered were decided by the anaesthesiologist conducting the case. The amount of drug loaded in the syringes in each case for the patient and any ampoule or vial broken while loading was noted from the case file. The amount of drugs actually administered to the patient was noted at the end of surgery from the case paper. The drugs that were leftover in the syringes, vials, ampoules (partially used and discarded) after each case was included in this study as a waste. The vial of propofol was discarded after 6 hours of opening it and any residual drug left in the vial was included in waste. Even the drugs that were loaded in syringes but not used at all (discarded) were also included in the study.
Cost of amount of drug utilized – Amountof drug utilized X cost per unit value of that drug.
Cost of the amountof drug un-utilized – Amount of drug un-utilized X cost per unit value of thatdrug.
Cost of un-utilized drug per case –
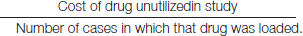
% of cost of a particula run-utilized drug–

The possible areas for reductionin drug wastage were identified and possible measures were suggested.
Results
According to WHO prescribing indicators [14], on average 6.5 drugs were prescribed per patient as pre-anaesthetic and intravenous inducing anaesthetic medications. 100% of drugs were prescribed by generic name, 92.30% from Essential Drug List [15]. Cost per unit value of each drug shown in [Table/Fig-1]. Cost per unit value of glycopyrrolate is maximum i.e. 23 Rs/mg and least for ketamine 0.0236 Rs/mg [Table/Fig-1].
Cost per unit (Rs) value of study drugs
| Sr.no | Drug | RC prices (Rs) | Cost Per Unit (Rs) |
|---|
| 1 | Vecuronium (4mg ampoule) | 24.10 | 6 /mg |
| 2 | Neostigmine (0.5mg/ 1ml ampoule) | 2.93 | 5.86/mg |
| 3 | Rocuronium (10 mg/ml, 5ml ampoule) | 247 | 4.94/mg |
| 4 | Atropine(0.6mg/1ml ampoule) | 2.80 | 4.67/mg |
| 5 | Glycopyrrolate (0.2mg/1ml ampoule) | 4.60 | 23/mg |
| 6 | Midazolam(1mg/ml,5ml vial) | 13.86 | 2.772/mg |
| 7 | Ondansetron (1mg/1ml,2ml ampoule) | 3.59 | 1.795/mg |
| 8 | Atracurium (10mg/ml,2.5ml ampoule) | 28.85 | 1.154/mg |
| 9 | Propofol(100mg/10ml vial) | 34.00 | 0.34/mg |
| 10 | Pentazocine (30mg/1ml ampoule) | 3.60 | 0.12/mg |
| 11 | Thiopentone Na (500mg/vial) | 43.50 | 0.087/mg |
| 12 | Succinyl choline (50mg/ml,10ml vial ) | 34.65 | 0.0693 /mg |
| 13 | Ketamine (50mg/ml,10ml vial) | 16.30 | 0.0236/mg |
Two hundred cases were included in the study in which thiopentone sodium was loaded as an intravenous inducing agent in 75% cases followed by propofol in 26% cases, & ketamine in 4%. Amongst pre-anaesthetics; atropine, glycopyrrolate, pentazocine, midazolam, ondansetron were loaded in 100% cases. Succinylcholine was most commonly used skeletal muscle relaxant in 76% of cases followed by vecuronium 62%. Neostigmine was commonly used for reversal in 79% cases [Table/Fig-2].
Amount of drug loaded while study period
| Sr.no | Drug | No of cases in which drug loaded | % |
|---|
| 1 | Atropine | 200 | 100 |
| 2 | Glycopyrrolate | 200 | 100 |
| 3 | Pentazocine | 200 | 100 |
| 4 | Midazolam | 200 | 100 |
| 5 | Ondansetron | 200 | 100 |
| 6 | Neostigmine | 158 | 79 |
| 7 | Succinyl choline | 152 | 76 |
| 8 | Thiopentone sodium | 150 | 75 |
| 9 | Vecuronium | 124 | 62 |
| 10 | Propofol | 52 | 26 |
| 11 | Atracurium | 30 | 15 |
| 12 | Rocuronium | 10 | 5 |
| 13 | Ketamine | 8 | 4 |
The study revealed that the wastage of various drugs varied from 4.67% to 79% [Table/Fig-3]. The maximum % of waste of loaded drugs was seen with atropine of about 79% and it was minimum for thiopentone sodium 4.67%. It was found that 8200mg propofol was loaded in cases performed under short GA but out of that 3000mg of propofol was wasted hence 36.59% of propofol was wasted during study period. Amongst pre-anaesthetic group, atropine was loaded in all 200 cases but only 25.2 mg was used out of 120 mg loaded. A 79% of atropine was wasted followed by ondansetron 50.67%, glycopyrrolate 45.95%, pentazocine 45.95%. Wastage for Vecuronium was 36.73% followed by succinyl choline 28.30%, rocuronium and atracurium 26.67% & 23.21% respectively. Neostigmine was used for reversal and 666mg was loaded out of that 192mg was wasted i.e. 28.83% of drug was wasted [Table/Fig-3].
Amount of drug wastage of various drugs
| Sr.no | Drug | Amount of drug loaded (mg) | Amount of drug partly used (mg) | Amount of drug partly un-used (discarded) (mg) | Amount of drug loaded but not used at all (mg) | Drug wasted (%) |
|---|
| 1 | Atropine | 120 | 25.2 | - | 94.8 | 79 |
| 2 | Ondansetron | 900 | 444 | 456 | - | 50.67 |
| 3 | Glycopyrrolate | 148 | 80 | 68 | - | 45.95 |
| 4 | Pentazocine | 11100 | 6000 | 5100 | - | 45.95 |
| 5 | Midazolam | 328 | 200 | 128 | - | 39.02 |
| 6 | Vecuronium | 784 | 496 | 288 | - | 36.73 |
| 7 | Propofol | 8200 | 5200 | 3000 | - | 36.59 |
| 8 | Ketamine | 1200 | 800 | 400 | - | 33.33 |
| 9 | Neostigmine | 666 | 474 | 192 | - | 28.83 |
| 10 | Succinyl choline | 21200 | 15200 | 6000 | - | 28.30 |
| 11 | Rocuronium | 1200 | 880 | 320 | - | 26.67 |
| 12 | Atracurium | 1120 | 860 | 260 | - | 23.21 |
| 13 | Thipentone sodium | 75,000 | 71500 | 3500 | - | 4.67 |
The cost analysis revealed that the total cost of the drugs loaded during the study period was Rs.34458.84. Of this, drugs amounting to Rs. 24182.58 were used while drugs amounting to Rs.10276.25 were wasted [Table/Fig-4]. Further analysis of the cost of total wastage (Rs.10276.25) for the study duration [Table/Fig-4] revealed that the cost of wastage of vecuronium was maximum being 16.82% (Rs.1728) of the total wastage cost, followed by rocuronium 15.38% (Rs.1580.80), glycopyrrolate 15.22% (Rs. 1564), neostigmine 10.95% (Rs. 1125.12) and propofol 9.93% (Rs 1020). Cost of drug wasted per case was maximum for rocuronium Rs158.08 and least for ketamine Rs 1.18 [Table/Fig-4].
Cost evaluation of study drugs
| Sr.no | Drug | Cost of drug loaded (Rs) | Cost of drug used (Rs) | Cost of drug wasted (Rs) | Cost wasted of total wastage (%) | Cost of wasted drug per case (Rs) |
|---|
| 1 | Vecruronium | 4704 | 2976 | 1728 | 16.82 | 13.94 |
| 2 | Rocuronium | 5928 | 4347.20 | 1580.80 | 15.38 | 158.08 |
| 3 | Glycopyrrolate | 3404 | 1840 | 1564 | 15.22 | 7.82 |
| 4 | Neostigmine | 3902.76 | 2777.64 | 1125.12 | 10.95 | 7.12 |
| 5 | Propofol | 2788 | 1768 | 1020 | 9.93 | 19.62 |
| 6 | Ondansetron | 1615.50 | 796.98 | 818.52 | 7.97 | 4.09 |
| 7 | Pentazocine | 1332 | 720 | 612 | 5.96 | 3.06 |
| 8 | Atropine | 560.4 | 117.68 | 442.71 | 4.31 | 2.21 |
| 9 | Succinyl choline | 1469.16 | 1053.36 | 415.80 | 4.05 | 2.74 |
| 10 | Midazolam | 909.22 | 554.4 | 354.82 | 3.45 | 1.77 |
| 11 | Thiopentone sodium | 6525 | 6220 | 305 | 2.97 | 2.03 |
| 12 | Atracurium | 1292.48 | 992.44 | 300.04 | 2.91 | 10.00 |
| 13 | Ketamine | 28.32 | 18.88 | 9.44 | 0.092 | 1.18 |
| Total Cost | 34458.84 | 24182.58 | 10276.25 | 29.82 | |
Discussion
It was observed that anaesthetists can directly affect health care costs through their practice patterns, including selection of anaesthetic drugs. This has been an issue of considerable interest, due to introduction of shorter-acting drugs such as propofol, midazolam, atracurium and vecuronium, rocuronium. Still there are no any indicators for intravenous agents to study their rational drug use. There is need to formulate such indicators for intravenous agents to study its utilization. It was seen that most commonly used drugs like glycopyrrolate and rocuronium are still not in Essential drug list [15]. Thus, there is need to revise National Essential Drug List.
It was seen that the maximum percentage wastage of loaded drugs was seen with atropine followed by ondansetron, which showed wastage of about 79% and 50.67%, respectively [Table/Fig-3]. Chaudhari et al., stated article named Anaesthetic drug wastage in operating room that wastage for atropine was 100% and Lejus C et al., in article named Atropine and ephedrine: A significant waste in the operating theatre, stated atropine wastage varied between 69% and 91% [1,16]. Although atropine was loaded in all 200 preoperatively as a prophylaxis for treatment of any intraoperative bradycardia, it was hardly ever required in routine cases and resulted in waste. Hence to reduce wastage of emergency drugs like atropine, there should be availability of common source in OT providing loaded syringes of emergency drugs as per necessity or to keep atropine ampoules on/near the anaesthetic machine with a saline filled syringe so that it can be easily accessed and prepared when needed, hence it will help to reduce wastage of loaded atropine per case. Prefilled syringes of atropine is also one of the good option to avoid wastage of atropine but as compared to cost of atropine 1ml ampoule + 2ml syringe, the cost of prefilled syringes is much higher, which is not affordable in government based hospitals.
It was found that 36.59% propofol was wasted compared to thiopentone sodium was just 4.67% [Table/Fig-3]. Chaudhari et al., stated article named Anaesthetic drug wastage in operating room that wastage for propofol was 56.27% and that of thiopentone sodium was 63.53% [1]. This amount calculate in this study appear miniature compared to study done by Chaudhari et al., but when considered overall cases operated in a year with such an anaesthetic approach, would account to be a considerable quantity of the total health expenses as illustrated by Kumar et al., and Watcha et al., [17,18]. A majority of wastage of propofol was seen to be due to drug remained in the vial due to reference to dispose of the vial after 6 hours of opening. During study period, it was observed that patient almost not required more than 20 ml of propofol for induction of anaesthesia (usually less than 15 ml suffices), so a best way would be to load up to the upper limit range for induction (2.5mg/kg) which would be less than 20 ml for an average 60–70kg patient so as to prevent wastage due to drug left in the syringe. Also, instead of using of two 10 ml vials for single case, use single 20 ml vial of propofol as cost of one vial of propofolis less than total cost of two 10ml vials. Thus, a better option for management would be to procure 20ml vials. Same strategy can be applied with rocuronium to reduce its wastage.
The cost of wastage was maximum for vecuronium (Rs1728) i.e.16.82% followed by rocuronium (Rs 1580.80) i.e. 15.38% out of total cost of drug wasted (Rs 10276.25) [Table/Fig-4]. Esaki R et al., in article named wastage of supplies and drugs in operating room stated cost of wastage for vecuronium was 12% [19]. The wastage of rocuronium and vecuronium can be prevented by calculating dose according to per kg body weight for each case before giving anaesthesia to patients so that un-touched drug left in the multi–dose vial can be used in next cases and is not wasted. The calculated dose may be displayed on case paper before the start of each case. Constant assessment of the necessity of neuromuscular blocker intraoperative, and loading the drug according to patient’s requirement is essential to eliminate unnecessary drug wastage. This would facilitate in estimating the drug needs of the patient for that procedure and ensure suitable loading thus preventing wastage.
Richard G Gillerman suggested that drug expenditure can also be limited by decreasing wastage of drugs used [9]. The cost analysis revealed that of the total cost of the drugs loaded (Rs. 34,458.84) during the study period, drugs amounting to Rs. 24,182.58 were used and drugs amounting to Rs. 10,276.25 were wasted [Table/Fig-4]. This indicates that drugs actually used during study period accounted for 70.18% of the total cost of drugs loaded. The findings reflect that cost of drug wastage was 29.82% of the total cost of drugs loaded [Table/Fig-4]. Chaudhari et al., in article named Anaesthetic drug wastage in operating room stated that cost of drug wastage was 87.17% [1] which indicates that consumption of un-touched loaded drugs for the next case in our institution may have practised for a lower estimate of drug waste costs in our study. This amount in our study may appear miniature, but when considered for bulky number of cases operated in a year with such an anaesthetic approach, would amount to be a significant fraction of the total health expenditure as illustrated by Kumar et al., and Watcha et al., thus there is need for awareness regarding wastage of drugs and their prudent management [17,18].
Efforts to increase cost awareness within hospitals may be effective (Hawkes et al.,) [2], but changes in the behaviour of practitioners may be momentary; once those efforts are condensed, so are cost-reducing conducts. (Weinger) [8] Hence education programs on drug-wastage reduction practices should be held repetitively at 4-6 monthly intervals. Endless consultations/meetings, addition of seminars/discussions on the cost of anaesthetic techniques and reduction of drug wastage, lectures education the above suggested ways, putting posters in theatres, anaesthetic rooms and recovery rooms may be very vital step in dropping drug wastage. The vigorous participation of senior registrars and faculty members in emphasizing and monitoring the above suggested modifications of existing drug preparations and their treatment practices would be most beneficial and effective.
This study has potential scope in pharmacoeconomic analysis of intravenous anaesthetic agents in non- government set up but entire non- government set up including nature of drug–use is unlike because anaesthetic practices vary. As well as, there are ethical and administrative problems in collecting records. But undoubtedly, study has further scope to compare anaesthetic practice in government and non government set up.
Conclusion
This study concludes that significant drug wastage seen during anaesthetic management can be reduced by simple ways suggested without compromising patient’s health. These approaches range from modifications in clinician’s behaviour to changes in the standard quantity in syringes or vials. Cost minimization is possible when there is sustained education is undertaken at regular interval to healthcare providers. Individual patients especially those in the lower socioeconomic group and developing countries are getting advantage from cost minimization strategies. Limitation of study is drugs used in spinal anaesthesia and local anesthesia are not considered to assess comparative analysis of drug audits in different approaches in anaesthesia. Further studies may be indicated to measure the extent of wastage in large number of cases and of volatile gases and other possible sources of waste and to assess the effectiveness of cost-saving strategies.