Unusual Complication of Surgical Abortion with Pelvic Extrusion of Fetal Head: A Case Report
Jasmina Begum1, Sunita Samal2, Seetesh Ghose3
1 Associate Professor, Department of Obstetrics and Gynecology, Mahatama Gandhi Medical College and Research Institute, Puducherry, India.
2 Professor, Department of Obstetrics and Gynecology, Mahatama Gandhi Medical College and Research Institute, Puducherry, India.
3 Professor, Department of Obstetrics and Gynecology, Mahatama Gandhi Medical College and Research Institute, Puducherry, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Jasmina Begum, Associate Professor, Department of Obstetrics & Gynecology, Mahatama Gandhi Medical College and Research Institute, Pillaiyarkuppam, Puducherry -607402, India.
E-mail: jasminaaly@gmail.com
Unsafe abortion is one of the causes of maternal mortality and morbidity in developing countries. The complications mostly results following unsafe abortion procedure done by unskilled provider with or without minimal medical knowledge in rural part of developing countries. These complications can endanger the life of mother if proper medical or surgical interventions are not offered in time. A majority of these complications remains confidential. The uterine perforation is one of the serious but preventable complications of surgical abortion. A 21-year-old woman G4P2L2A1, presented in the emergency ward with complaints of lower abdominal pain for four days after attempting twice surgical termination of pregnancy at 19 weeks of gestation for an unwanted pregnancy. Transabdominal sonography and MRI revealed uterine rent with pelvic extrusion of fetal head. Emergency laparotomy with removal of fetal head and uterine rent repair was done. This case illustrates the importance of maintaining a high index of suspicion by the gynaecologist for uterine perforation in patient presenting with abdominal pain a few days after undergoing surgical abortion, also shows the complementary role of sonography and MRI in evaluation of the similar patient and this case also highlights the rampant illegal unsafe abortion procedure in rural India despite of legalization of abortion act.
Magnetic resonance imaging (MRI), Uterine perforation
Case Report
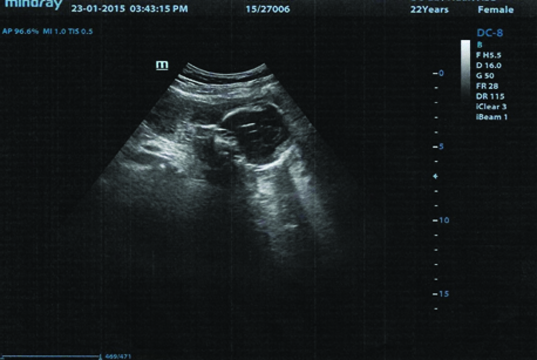
A 21-year-old woman G4P2L2A1, presented in the emergency ward with complaints of lower abdominal pain for four days after surgical termination of pregnancy at 19 weeks of gestation for an unwanted pregnancy. She had undergone twice elective dilatation and curettage in a private clinic by an untrained personal. First procedure was done six days before the day of admission and the second procedure was done two days after first, for excessive bleeding per vagina and for retained product of conception. She had similar history of induced abortion for an unwanted pregnancy at second trimester one year back but her post abortion period was uneventful. On general examination she was afebrile and her vitals were stable. On abdominal examination, abdomen was soft with severe tenderness felt in the left iliac fossa and no signs of peritoneal irritation were present. On pelvic examination no active bleeding or any purulent discharge through external cervical ostium, uterus was enlarged tender upto 12 weeks size, internal cervical ostium admitted one finger, left fornix was full and tender, right fornix was normal. With this finding a clinical suspicion of endometritis or retained product of conception was made, ultrasound of pelvis along with routine investigations was done. All the routine investigations were normal limits except with the evidence of significant moderate anaemia with Hb of 7.7gm%. Transabdominal ultrasound of pelvic organ after careful scanning showed fetal parts in the left lilac fossa in the form of deformed fetal skull. The uterine defect was not identifiable [Table/Fig-1]. Magnetic resonance imaging of the pelvis was subsequently performed to evaluate the uterus and left adnexa. It showed a transmural defect at the lower part of uterus with enhancing extruded fetal part (deformed fetal head) in left adnexa [Table/Fig-2]. Based on recent history of surgical induced abortion, sonography and MRI finding, a diagnosis of uterine perforation with abdominal expulsion of fetal part was made. Case was posted for emergency laparotomy. Fetal head was removed from left broad ligament after opening the left anterior leaf of ligament [Table/Fig-3]. A rent of 5 cm in length was identified in the left lateral wall of uterus [Table/Fig-4]. Rent repair and abdominal toileting was done. Bilateral tubal ligation was not performed as the patient denied giving consent prior to surgery. The patient was discharged after two weeks of uneventful postoperative recovery. During discharge the couple was explained the consequences of further pregnancy related complications and advised for permanent method of sterilization.
TAS of pelvis showing fetal part in the left lilac fossa in the form of deformed fetal skull. The uterine defect was not clearly identifiable
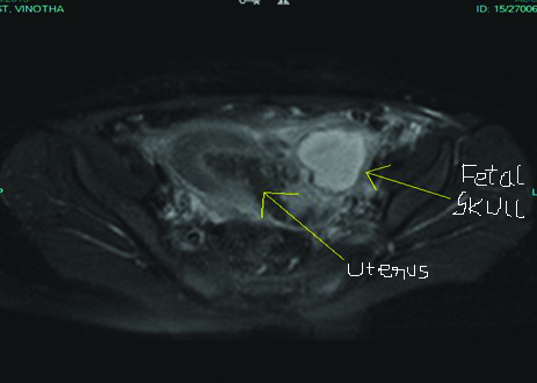
MRI of pelvis showing a transmural defect at the lower part of uterus with enhancing extruded fetal part (deformed fetal head) in left adnexa
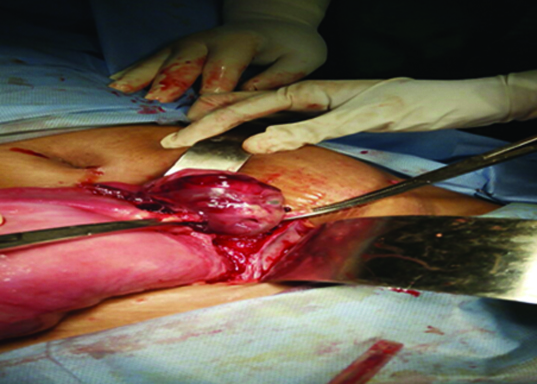
Intraoperative finding showing removal of fetal head from the left broad ligament after opening the left anterior leaf.
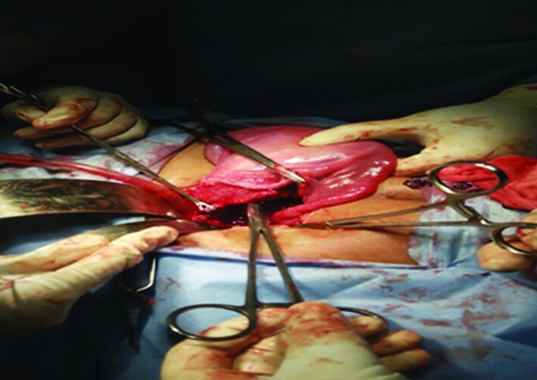
Intraoperative finding showing a rent of 5 cm in length in the left lateral wall of uterus.
Discussion
Unsafe abortion is defined as a procedure for terminating an unwanted pregnancy that is performed by someone lacking the necessary skill or in an environment lacking minimal medical standards or both [1]. It is primarily a cause of maternal mortality and morbidity in developing countries. Worldwide data estimates that approximately 8% of all maternal mortality are due to unsafe abortion and related complications [2]. In India, complications of unsafe abortion accounts an estimated 9% of all maternal deaths according to the latest government report on causes of death from 2010 [3]. Uterine perforation is a serious complication of unsafe abortion and it occurs in between 0.07 to 1.2% with dilatation and curettage [4]. The complications resulting from unsafe abortions are preventable. The early complications of abortion includes uterine perforation, blood loss, retained product of conception, injury to bowel, bladder, cervix, aspiration of visceral organ, endometritis, pelvic infection and peritonitis. The late complications are more diverse in their presentation which includes secondary infertility, ectopic pregnancy, endometritis and cervical incompetence. A study conducted on 157 women admitted for unsafe abortion over a period of three years showed that majority were admitted with serious complications like peritonitis (70%), visceral injuries (60%), septic and haemorrhagic shock, renal failure (17.4%), life threatening complications like DIC, hepatic failure, and encephalopathy [5]. These complications mostly results following unsafe abortion procedure done by unskilled person with or without minimal medical knowledge in rural part of developing countries as stated in various volumes of research articles, case reports and letters to the editor. This is supported by a study conducted on 381 post abortal women in ten districts and medical college hospitals in Madhya Pradesh, India where majority of women (95%) visited atleast one health care provider before they seek care at district or medical college hospitals, out of which 68% of them are ineligible to provide abortion services in India [6]. Uterine perforation is a serious but preventable complication of abortion. It is seen that the risk of iatrogenic perforation increases significantly with conditions like advanced gestation age, greater parity, retroverted gravid uterus, history of prior abortion or caesarean section, failure to perform songraphy guided procedure and unskilled provider [7]. In India, although abortion was legalized way back in the year 1972, an estimated 4.7 million abortion are performed annually outside the approved facilities and only 10% of all abortions are registered in India [8]. The lack of education, social stigma and the legal issues may be the causes of deliberate suppression of abortion related facts in India.
Other unusual occurrence of combined uterine perforation and extruded fetal part via the uterine wall defect and outward herniation of internal structure like the bowel and fallopian tube had been reported earlier [4,9]. Cases, where MRI aided the diagnosis along with sonography to detect the uterine wall defect and extruded fetal part had also been reported [9].
In a study done by Kohlenberg CF et al., a fall in uterine perforation rate from 1.4% to 0.2% and overall complication rate from 5.7% to 2.8% with the use of sonography was observed. To prevent or reduce complication from surgical pregnancy termination, the author has proposed use of intraoperative sonography during dilation and curettage at greater than 15 week’s gestation [10]. This case also shows the complementary role of sonography and MRI in evaluation of the patient. Although the intra pelvic extruded fetal part was identified on sonogrphy but MRI had clearly defined the location and the extent of uterine perforation along with extruded fetal part. CT and MRI are equally efficacious in diagnosing the present scenario and neither of them scores over the other.
Conclusion
Maternal mortality becomes inevitable due to complications of unsafe abortion if proper medical or surgical interventions are not offered in time. This case shed light upon the importance of maintaining a high suspicion for uterine perforation in patient presenting with abdominal pain a few days after undergoing surgical abortion. This case also gives importance to the role of sonography as initial diagnostic modality but cases where diagnosis is uncertain, to confirm the findings, exact site, extent of uterine perforation and associated visceral injury we suggest the usage of CT or MRI which complement the role of sonography. As it is a one of the important public health problems the best way to prevent unsafe abortion consequences in developing countries is by reducing the unmet need for contraception, making safe abortion services accessible to women, controlling unauthorized medical practice, providing training and provision of equipments for MTP and ensuring proper supervision of medical facilities.
[1]. Unsafe abortion: global and regional estimates of incidence of unsafe abortion and associated mortality in 2003. WHO. 5th ed: Geneva, 2007 [Google Scholar]
[2]. Say L, Chou D, Gemmill A, Global causes of maternal death: a WHO systematic analysisLancet Glob Health 2014 2:e323-33. [Google Scholar]
[3]. Registrar General of India, Report on medical certification of cause of death, 2010, New Delhi: Registrar General of India, 2014 [Google Scholar]
[4]. Chauhan NS, Gupta A, Soni PK, Surya M, Mahajan SR, Iatrogenic uterine perforation with abdominal extrusion of fetal parts: A rare radiological diagnosisJournal of Radiology Case Reports 2013 7(1):41-47. [Google Scholar]
[5]. Bhattacharya S, Mukherjee G, Mistri P, Pati S, Safe abortion - still a neglected scenario: a study of septic abortions in a tertiary hospital of rural IndiaOnline J Health Allied Scs 2010 9(2):7 [Google Scholar]
[6]. Banerjee SK, Andersen KL, Warvadekar J, Pathways and consequences of unsafe abortion: A comparison among women with complications after induced and and spontaneous abortions in Madhya Pradesh, IndiaInt J Gynaecol Obstet 2012 118:113-20. [Google Scholar]
[7]. Augustin G, Majerovic M, Lueti T, Uterine perforation as a complication of surgical abortion causing small bowel obstruction: a reviewArchives of Gynaecology and Obstetrics 2013 288:311-23. [Google Scholar]
[8]. Das V, Agarwal A, Mishra A, Despanda P, Septic abortionJ Obstet Gynaecol India 2006 56:236-39. [Google Scholar]
[9]. Gakhal MS, Levy HM, Sonographic diagnosis of extruded fetal parts from uterine perforation in the retroperitoneal pelvis after termination of intrauterine pregnancy that were occult on magnetic resonance imagingJ Ultrasound Med 2009 28:1723-27. [Google Scholar]
[10]. Kohlenberg CF, Casper GR, The use of intraoperative ultrasound in the management of a perforated uterus with retained products of conceptionAust NZ J Obstet Gynaecol 1996 36:482-84. [Google Scholar]