Atrial Septal Defect with Cyanosis Due To Over-Developed Eustachian Valve Directed Towards Left Atrium: A Very Rare Scenario
Arnab Banerjee1, Abhishek Mukherji2, Rajeev Ranjan3, Snehasis Das4, Niladri Sarkar5
1 Resident, Department of Internal Medicine, IPGMER, Kolkata, West Bengal, India.
2 Resident, Department of Internal Medicine, IPGMER, Kolkata, West Bengal, India.
3 Resident, Department of Internal Medicine, IPGMER, Kolkata, West Bengal, India.
4 Resident, Department of Internal Medicine, IPGMER, Kolkata, West Bengal, India.
5 Professor, Department of Internal Medicine, IPGMER, Kolkata, West Bengal, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Arnab Banerjee, ROOM NO.644, 242, AJC Bose Road, PG Doctors hostel, IPGMER, Kolkata-700020, India. E-mail : miluban007@gmail.com
Cyanosis in a case of ASD (atrial septal defect) without pulmonary arterial hypertension is quite rare. A patient with ASD and pneumonia is described who had a central cyanosis resulting from the drainage of deoxygenated blood from the inferior vena cava directly into the left atrium through the atrial septal defect due to the presence of an over-developed malpositioned Eustachian valve directed to the left atrium. In conclusion, ASD can present with cyanosis due to an over-developed Eustachian valve.
Respiratory distress, Tachycardia
Case Report
A 33-year-old non-diabetic, non-hypertensive man presented with fever followed by respiratory distress for the last 3 days prior to admission. There wasn’t any history of chest pain, palpitation, paroxysmal nocturnal dyspnoea. Fever was associated with chills and rigor. On further enquiry the patient revealed that he had been diagnosed with some heart disease in the past and he had similar episodes of fever and respiratory distress.
On examination he had tachycardia (120/min), tachypnoea (28/min), fever (102.8 degree F), central cyanosis [Table/Fig-1], clubbing [Table/Fig-2] and coarse crepitations with increased bronchial breath sounds in the right lower zone of the lung suggestive of pneumonic consolidation. Cardiovascular system examination revealed a down and out apex beat (5th intercostal space, 1.25 cm right of the mid-clavicular line) with a narrow and fixed split second heart sound. there was no murmur. ABG (arterial blood gas) revealed acidosis with hypoxia and hypercarbia. ECG revealed mild left axis deviation and there was neutrophilic leucocytosis in his peripheral blood (total count-13,400/cu.mm N82L16E2). Chest X ray showed right lower zone consolidation. Other investigations in his blood were within normal limits. Considering the history of some heart disease in childhood and central cyanosis, we performed a transthoracic echocardiography in which there was a septum secundum atrial septal defect (ASD) without any evidence of right to left shunt, pulmonary arterial hypertension or eisenmenger’s physiology. Pulmonary artery pressure was 27/12 mmHg; mean 17 mmHg, right atrial pressure 9 mmHg, and left atrial pressure 10 mmHg as evidenced by a right heart catheterisation. Oxygen saturation was 75% in inferior vena cava, 70% in the right atrium, 96% in the pulmonary veins and 86% in the aorta. As we could not account for the central cyanosis in this patient from these reports, we did a bubble contrast echocardiography with agitated saline injection. It revealed that the patient had an ASD but interestingly in this case the Eustachian valve (valve of the inferior vena cava) was over-developed & located so close to the ASD that the jet of deoxygenated blood from the inferior vena cava (IVC) was practically draining into the left atrium [video-1]. The oxygenated blood of the left atrium was thus contaminated by the deoxygenated blood from the IVC thus giving rise to the central cyanosis. The blood from the superior vena cava was draining normally into the right atrium and was going to the right ventricle, as expected. As the flow through the right atrium and ventricle was reduced, there had been no right atrial or ventricular hypertrophy.
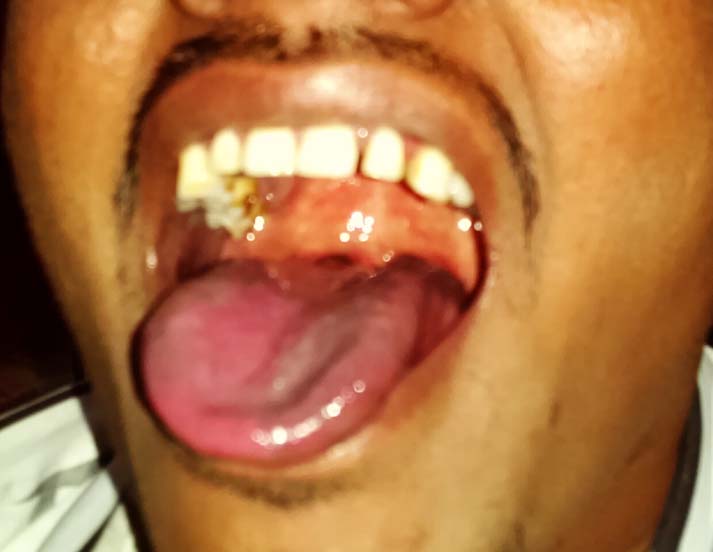
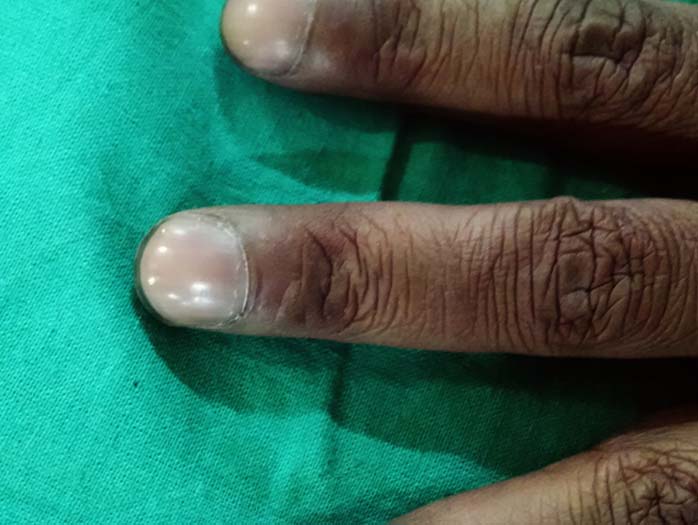
Therefore, in this patient we made a diagnosis of right lower zone consolidation along with an IVC which is practically draining into the left atrium through a septum secundum ASD. As a result the major portion of the venous inflow to the heart was going to the left atrium directly without being oxygenated, thus giving rise to a functional right–to-left shunt.
The patient was treated empirically with levofloxacin (750 mg IV OD) and ceftriaxone (2 gm IV OD) after obtaining sputum for culture and sensitivity testing. Reports revealed infection with pneumococcus sensitive to both levofloxacin and ceftriaxone. So the empirically given antibiotics were continued for a full course of 14 days. Other supportive therapy (e.g. moist oxygen inhalation, nebulisation as required) were also provided. After being stabilised, he was sent to the cardiothoracic department where his ASD was closed, thus correcting the pathway through which the right-to-left shunt was occurring.
The patient was followed up after 1 month and was doing fine with dramatic correction of the cyanosis.
Discussion
Strotmann et al., reported a case of a 36-year-old patient with a brainstem stroke of unknown origin and a secundum atrial septal defect in combination with a persisting prominent eustachian valve in 2001. Though the persistent eustachian valve posed difficulty during closure of the atrial septal defect, neither the actual importance of the persistent valve in this case was known nor did that defect cause any significant physiological or anatomical difficulty in the patient [1]. Morishita et al., described two cyanotic patients with venoarterial shunting from the inferior vena cava to the left atrium in an uncomplicated atrial septal defect with normal right ventricular pressures in 1985. Cyanosis was due to a large, anomalous inferior vena caval valve in both these cases [2].
Central cyanosis can occur in ASD due to various causes. If there is a right-to-left shunt resulting from pulmonary arterial hypertension, cyanosis can be there, but in that case there will be right atrial and ventricular hypertrophy.
Other causes of cyanosis in ASD include large ASD with equalisation of LA & RA pressures, ASD with associated valvar pulmonic stenosis. IVC blood can stream into LA by hitting preferentially the lower part of IAS (inter atrial septum), thus producing right-to-left shunt & cyanosis. During straining, (Valsalva and equivalents) right atrial pressure can exceed LA pressure & can cause cyanosis. In ASD with systemic venous anomaly like persistent left SVC connected to coronary sinus and with that coronary sinus connected to the LA, there can be significant cyanosis [3].
But in this case there was an abnormal over-developed Eustachian valve which is in very close proximity to the LA, resulting in the IVC practically draining into the left atrium such an abnormality is extremely rare and can result in significant confusion and misdiagnosis [4]. The right-to-left shunt, albeit functional, was well tolerated during normal periods, but during times of stress, as is the scenario in this patient with right lower zone pneumonia, the mixed blood is no longer sufficient to meet the needs of the patient and thus resulted in respiratory distress, hypoxaemia and exacerbation of cyanosis.
Conclusion
There can be many different causes of cyanosis in a patient with an ASD. But one must keep some very uncommon causes like an over-developed Eustachian valve draining into the left atrium in mind or else is liable to omit an easily remediable cause like this.
[1]. Strotmann J, Voelker W, Schanzenbaecher P, Persistence of the eustachian valve in secundum atrial septal defects: possible implications for cerebral embolism and transcatheter closure proceduresHeart 2001 86(1):e5doi:10.1136/heart.86.1.e5 [Google Scholar]
[2]. Morishita Y, Yamashita M, Yamada K, Arikawa K, Taira A, Cyanosis in atrial septal defect due to persistent eustachian valveAnn Thorac Surg 1985 40(6):614-16. [Google Scholar]
[3]. Thomas JD, Tabakin BS, Ittleman FP, Atrial septal defect with right to left shunt despite normal pulmonary artery pressureJ Am Coll Cardiol 1987 9:221-24. [Google Scholar]
[4]. Sommer RJ, Hijazi ZM, Rhodes JF., Jr., Pathophysiology of congenital heart disease in the adult: part I: Shunt lesionsCirculation 2008 117:1090-99.[PubMed] [Google Scholar]