Complex Open Distal Femur Fracture Managed By Primary Autogenous Fibular Graft in Conjunction with DFLP- A Case Report
Vishant Gawri1, Yashika Garg2, Dharam Singh3, Radhe Shyam Garg4, Nishant Choudhary5
1 Junior Resident, Department of Orthopaedics, Guru Nanak Dev Hospital, Government Medical College, Amritsar, Punjab, India.
2 Senior Resident, Department of Pharmacology, Guru Nanak Dev Hospital, Government Medical College, Amritsar, Punjab, India.
3 Assistant Professor, Department of Orthopaedics, Guru Nanak Dev Hospital, Government Medical College, Amritsar, Punjab, India.
4 Professor, Department of Orthopaedics, Guru Nanak Dev Hospital, Government Medical College, Amritsar, Punjab, India.
5 Junior Resident, Department of Orthopaedics, Guru Nanak Dev Hospital, Government Medical College, Amritsar, Punjab, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Radhe Shyam Garg, Professor and Incharge, Orthopaedic Unit 3, Department of Orthopaedics, Guru Nanak Dev Hospital, Government Medical College, Amritsar, India. E-mail : Dr.rsg@hotmail.com
Fractures of the distal part of the femur account for 7% of all femoral fractures. They are complex injuries that are difficult to manage; despite advances in technique and improved implants, treatment remains a challenge in many situations. An 18-year-old boy presented with an open fracture of the femur with bone loss. After initial emergency management, patient was given skeletal traction and kept on bohler braun splint. Regular antiseptic dressings of loosely stitched wound were done and intravenous antibiotics given. After 2 weeks when wound healed and twice cultures from wound site were negative, the fractured femur was stabilized with a dflp along with an autogenous free fibular graft and cortico-cancellous graft to bridge the bone defect. At one-year follow-up, fracture united with incorporation of free fibular graft. An autogenous free fibular graft in conjunction with a dflp is a viable option to manage bone defects in complicated supracondylar fractures of the femur.
Dflp (distal femoral locking plate), Femoral fractures, Supracondylar fracture
Case Report
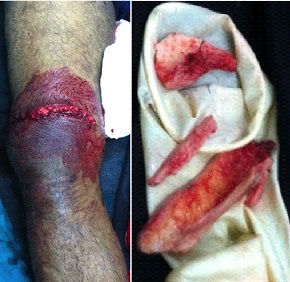
An 18-year-old boy who was involved in a motorcycle accident presented to emergency department after 6 hours of road traffic accident, with pain, swelling, and a large open wound on the right thigh. On examination, the Glasgow Coma Scale score was 15 of 15. A 10-cm lacerated wound with protruding distal end of proximal fragment about 1 cm was seen on the antero-medial aspect of the right distal thigh which was nibbled and lavaged before reducing it [Table/Fig-1], extruded bone fragments were part of comminution from metaphyseal and diaphyseal region of femur which were brought separately. There was local tenderness, crepitus, and abnormal mobility in the distal part of the thigh. There was no distal neurovascular deficit.
Wound over anteromedial side of Right knee with extruded bone
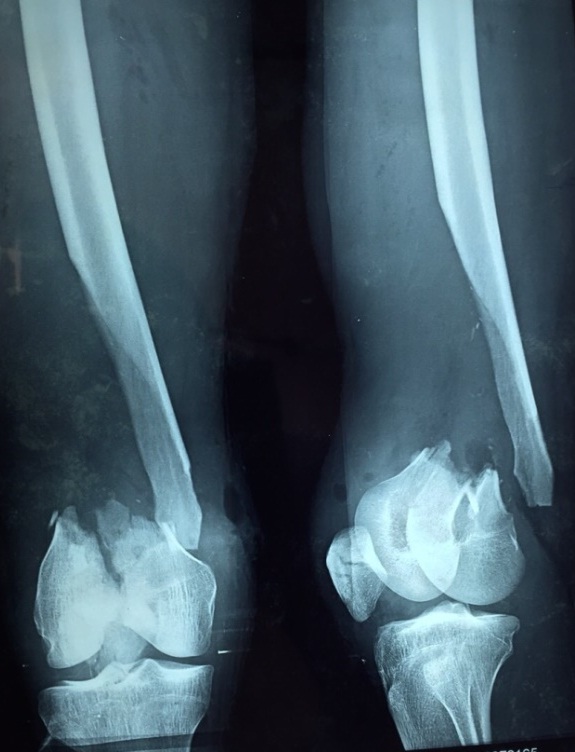
Radiographs revealed a comminuted supracondylar fracture with bone loss [Table/Fig-2], which was classified as an open Gustilo-Anderson type-III B AO/OTA (Arbeitsgemeinschaft furOsteosynthesefragen/Orthopaedic Trauma Association) type-C2 supracondylar fracture of the femur [1].
Radiograph of the part at the time of admission
Only one debridement was done in emergency OT immediately after admission of the patient. About 1 cm of the protruding distal spike of the proximal fragment was excised apart from discarding all the extruded pieces of the bone, copious lavage with normal saline mixed with povidone iodine and metronidazole (about 5 litres) was done. Fortunately there was no skin loss, skin margins were freshened and stitched loosely with few widely placed sutures. Skeletal traction with 5 kg weight given on bohler braun splint against gravity with foot end raised by 6 inches. Intravenous antibiotics (cefaperazone + tobramycin + metronidazole) were given and regular antiseptic dressings were done. Wound cultures were done twice; 48 hours after admission and another on 5th day, both were free from any organisms. As we planned for the second stage of the operation, we faced three problems: an open Gustilo-Anderson type III-B comminuted fracture in the supracondylar region, bone loss, and a shortening of 8 cm. After considering different options, we decided on dflp fixation with an ipsilateral autogenous fibular graft and a cortico-cancellous graft to bridge the bone defect.
After 2 weeks when wound healed and wound cultures were negative. The fracture site was exposed through a lateral approach. First, K wires were passed lateral to medial to align the fractured femoral condyles under image intensifier. We harvested an 11-cm long autogenous fibular graft from the ipsilateral leg. The fibular graft was inserted into the medullary canal both proximally and distally to bridge the defect caused by bone loss. Fracture was reduced and fixed with a distal femoral locking plate bridging fracture and locked distally and proximally. Cortico-cancellous graft from the ipsilateral iliac crest was also packed into the fracture site, and the wound was closed in layers over a negative suction drain. Postoperative radiographs showed good alignment of the fragments [Table/Fig-3]. The autogenous free fibular graft was seen inside medullary cavity with surrounding cortico-cancellous graft. Follow up [Table/Fig-4,5 and 6] was done every month with calcium, vitamin-d, high protein diet and active mobilization of knee joint and no weight bearing. Partial weight bearing allowed only after 2½ month postoperatively along with regular active physiotherapy of knee joint.
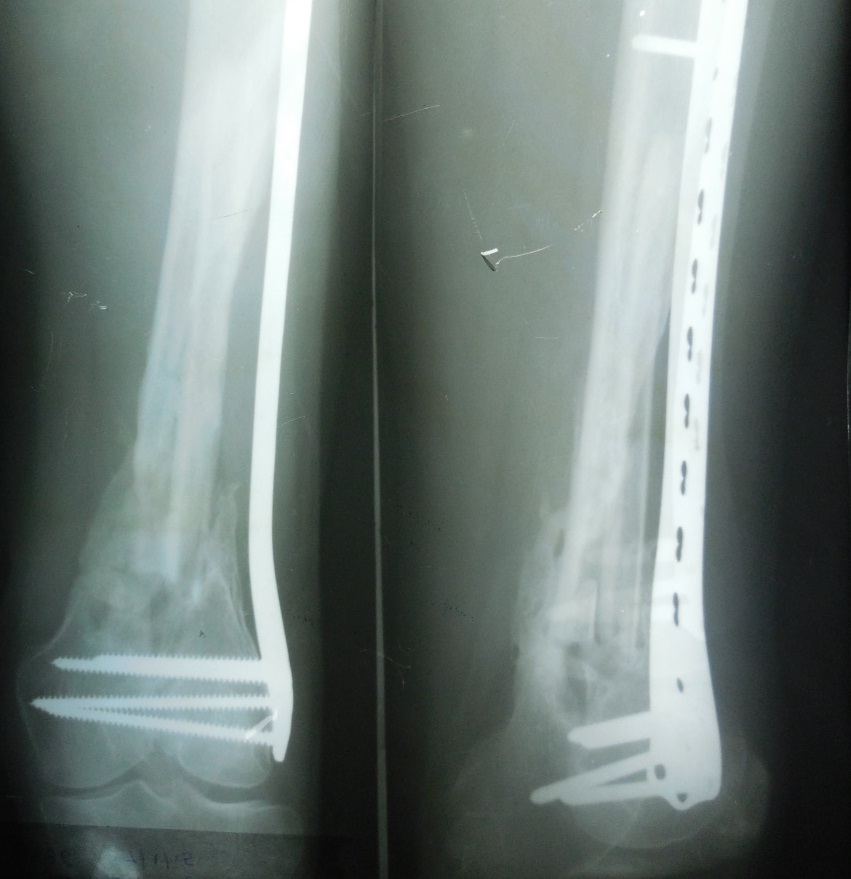
Immediate postoperative X-ray of the patient in anteroposterior and lateral views
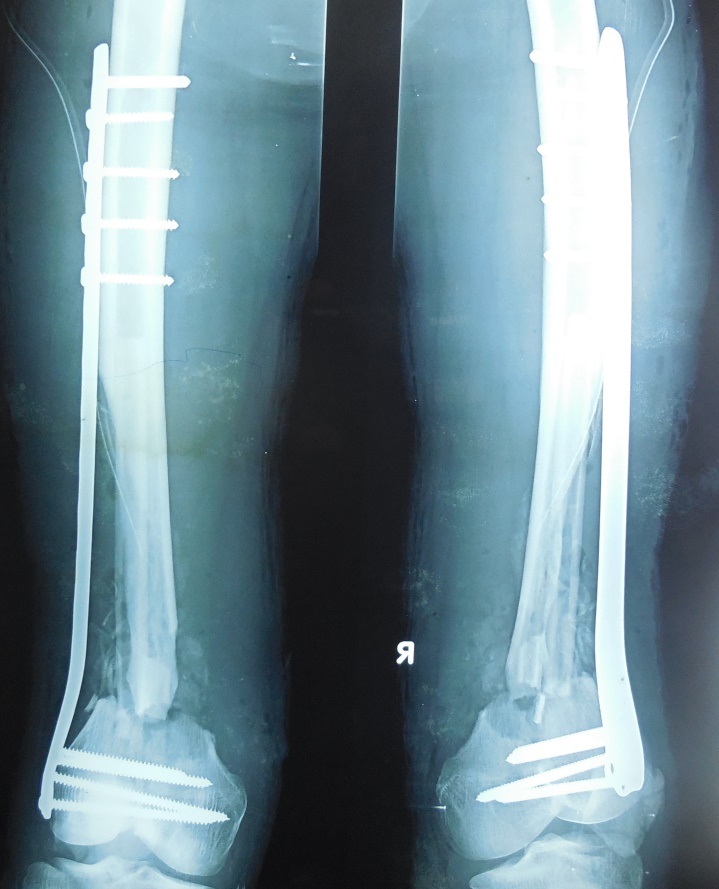
Postoperative radiograph of the part at 6 Months showing bone healing
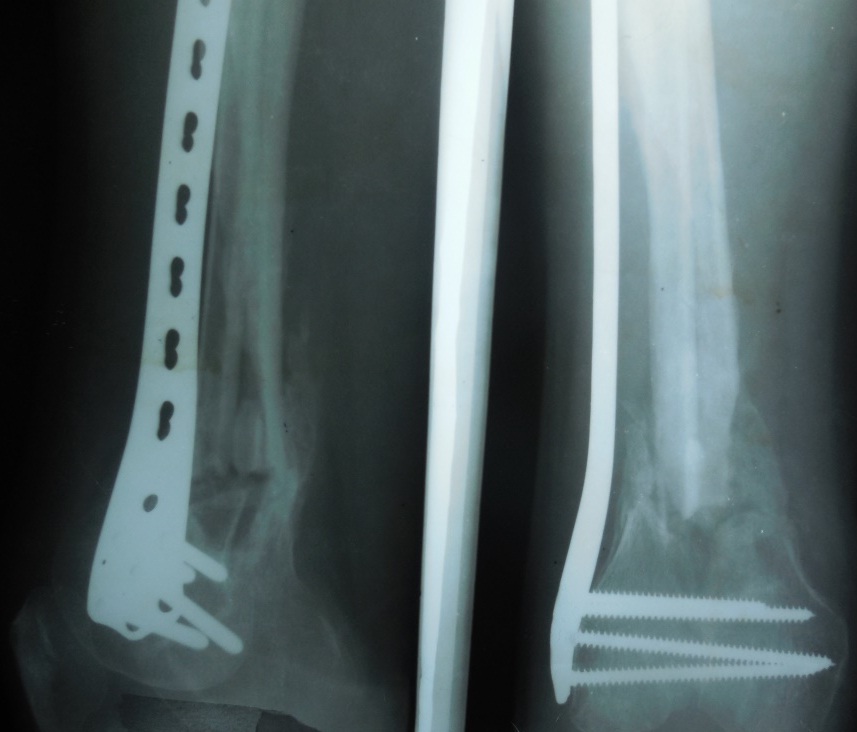
Radiograph of the part at 1 year showing adequate union
Showing patient standing and putting full weight on right leg

Discussion
Fractures of the distal part of the femur account for 7% of all femoral fractures [2]. Supracondylar fractures of the femur with bone defect/loss are a challenge for orthopaedic surgeons to treat. In our patient, we used an autogenous nonvascularised free fibular graft along with a cortico-cancellous graft to manage bone defect in conjunction with distal femoral locking plateto stabilize the fracture with excellent result.
Following a total knee arthroplasty, Tani et al., treated a supracondylar fracture of the femur with an autogenous fibular graft [3]. The graft was inserted into the medullary cavity from the intercondylar region and was fixed to the proximal fragment of the femur with augmented fixation with use of a small plate and screws, and the fracture united.
Ramesh et al., used an Ilizarov fixator with fibular and cortico-cancellous grafts in 13 patients with type-C3 distal femoral fractures [4]. They chose to use the ipsilateral fibula for grafting; they drilled unicortical drill holes in the fibula, and the fibula was telescoped between the proximal and distal fragments until the total length of the femur was equal to the length of the contralateral femur. They achieved a mean range of motion of 77°. Ten patients had good results and three patients had poor results with this technique.
In addition to an external fixator, Lawal et al., used an autogenous free fibular graft to manage bone defects in open fractures of the femur and tibia; they noted graft incorporation in 80% of their cases [5].
Yajima et al., treated 20 patients with nonunion due to various causes with vascularized free fibular grafts [6]. They had good results in 19 of 20 patients. Three of these patients had graft fracture, which united after treatment with casts. Osseous union occurred at a mean of 6.1 months.
Muramatsu et al., treated 17 patients with single, double, or folded vascularized fibular grafts for bone defects of the femur for an average period of 25 months [7]. In 11 patients, the defect resulted from trauma, and in six patients the defect occurred following tumour resection. There was a good outcome in 93% of their patients. Stress fracture occurred in three of the inlay fibular grafts. Muramatsu et al., concluded that vascularized fibular grafting is a reliable and safe procedure for massive bone defects; however, folded or double fibular grafts do not prevent stress fractures, and it is important to rigidly stabilize the fracture in an anatomically aligned position.
The purpose of the Gustilo-Anderson schema is to provide a prognostic framework that guides treatment and facilitates communication among surgeons and clinician-scientists. The variability among individuals and their interpretation of the Gustilo-Anderson classification [8] results in a spectrum of injuries having too much overlap [9], possibly owing to the observer error. As with other classification system Gustilo system heavily relies on “Subjective phraseology and terms like “extensive soft tissue damage”, “significant periosteal stripping” and “massive contamination” leading to wide variation in interpretation among surgeons. The above terms are ambiguous quantitatively and especially Gustilo classification is noncontributory in cases of open fractures with bone loss.
Bone defects with supracondylar fractures can be managed with an Ilizarov fixator along with an autogenous fibular graft, as used by Ramesh et al., [4]. Vascularized free fibular grafts can be used to achieve union, as noted by Yajima et al., and Muramatsu et al.,, whose patients achieved good results however, stress fractures of the fibular graft did occur in a few of their patients [6,7].
We used a nonvascularized autogenous free fibular graft alongwith a distal femoral locking plate, which prevents graft fracture, aids in union, and helps to maintain femoral length. This procedure is relatively simple and can be done without special expertise. Fracture union was achieved in our patient. He had no postoperative morbidity or complications in the ipsilateral leg from which the fibular graft was harvested. He did have knee stiffness in the operative leg, and the knee range of motion was 0° to 90°.
Conclusion
Delayed primary surgery using autogenous nonvascularised free fibular graft in conjunction with a locking compression plate with autogenous cortico-cancellous graft is a viable/sagacious option to manage bone defects in complex open supracondylar fractures of the femur with overall excellent results in terms of fracture union, fibular incorporation, adequate restoration of knee motion, no donor site morbidity and early rehabilitation, all attained with a planned single stage well timed definitive operative intervention. Saving the patient from lot of miseries and financial burden.
[1]. Marsh JL, Slongo TF, Agel J, Broderick JS, Fracture and dislocation classification compendium – 2007: Orthopaedic Trauma Association Classification, Database and Outcomes CommitteeJ Orthop Trauma 2007 21(10 Suppl):S1-133. [Google Scholar]
[2]. Arneson TJ, Melton LJ, Lewallen DG, O’Fallon WM, Epidemiology of diaphyseal and distal femoral fractures in Rochester, Minnesota, 1965-1984Clin Orthop Relat Res 1988 (234):188-94. [Google Scholar]
[3]. Tani Y, Inoue K, Kaneko H, Nishioka J, Hukuda S, Intramedullary fibular graft for supracondylar fracture of the femur following total knee arthroplastyArch Orthop Trauma Surg 1998 117(1-2):103-04. [Google Scholar]
[4]. Ramesh LJ, Rajkumar SA, Rajendra R, Rajagopal HP, Ilizarov ring fixation and fibular strut grafting for C3 distal femoral fracturesJ OrthopSurg (Hong Kong) 2004 12(1):91-95. [Google Scholar]
[5]. Lawal YZ, Garba ES, Ogirima MO, Dahiru IL, Maitama MI, Abubakar K, Use of non-vascularized autologous fibula strut graft in the treatment of segmental bone lossAnn Afr Med 2011 10(1):25-28. [Google Scholar]
[6]. Yajima H, Tamai S, Mizumoto S, Ono H, Vascularised fibular grafts for reconstruction of the femurJ Bone Joint Surg Br 1993 75(1):123-28. [Google Scholar]
[7]. Muramatsu K, Ihara K, Shigetomi M, Kawai S, Femoral reconstruction by single, folded or double free vascularised fibular graftsBr J Plast Surg 2004 57(6):550-55. [Google Scholar]
[8]. Gustilo RB, Anderson JT, Prevention of infection in the treatment of one thousand and twenty-five open fractures of long bones: retrospective and prospective analysesJ Bone Joint Surg Am 1976 58:453-58. [Google Scholar]
[9]. Brumback RJ, Jones AL, Interobserver agreement in the classification of open fractures of the tibia: the results of a survey of two hundred and forty-five orthopaedic surgeonsJ Bone Joint Surg Am 1994 76:1162-66. [Google Scholar]