Atypical Presentation of Capillary Hemangioma in Oral Cavity- A Case Report
Veena Raj Vasantha Kumari1, Chitra Girija Vallabhan2, Seema Geetha3, Manoj S Nair4, Tharun Varghese Jacob5
1 Post Graduate Student, Department of Periodontics, Sri Sankara Dental College, Vennicode, Trivandrum, Kerala, India.
2 Senior Lecturer, Department of Periodontics, Sri Sankara Dental College, Vennicode, Trivandrum, Kerala, India.
3 Professor, Department of Periodontics, Sri Sankara Dental College, Vennicode, Trivandrum, Kerala, India.
4 Professor, Department of Oral Pathology, Sri Sankara Dental College, Vennicode, Trivandrum, Kerala, India.
5 Reader, Department of Oral Pathology, Sri Sankara Dental College, Vennicode, Trivandrum, Kerala, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Veena Raj Vasantha Kumari, Ravi Bhavan, Vembayam, P.O., Trivandrum, Kerala- 695615, India. E-mail : veenarajv1@gmail.com
Capillary Haemangioma is a benign vascular tumour characterized by proliferation of blood vessels that are primarily reported to be a developmental hamartomatous lesion of infancy and childhood. Pyogenic granuloma is a non-neoplastic benign lesion found in the oral cavity having a striking predilection for occurrence in the gingiva. The present case report is an atypical presentation of capillary haemangioma on gingiva which is considered to be extremely rare. The lesion in this case was clinically diagnosed as pyogenic granuloma but histopathologically as capillary haemangioma. These lesions present as a diagnostic dilemma to the clinician and can lead to serious complications if not carefully managed.
Excision, Gingiva, Histopathology, Pyogenic granuloma
Case Report
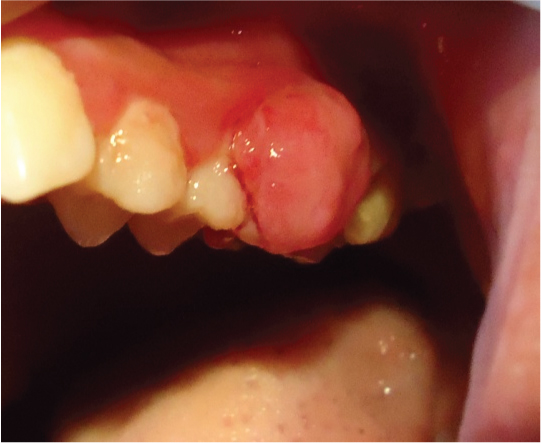
A 28-year-old female patient reported with a painful swelling in the upper left back tooth region. The swelling was noticed 3 months back, which gradually increased in size with a history of frequent bleeding, and difficulty in chewing and brushing. The patient’s medical history was non-contributory. On intraoral examination, 1x1 cm sized solitary, sessile, reddish pink swelling with distinct borders and smooth surface was seen on the buccal aspect of 26 extending onto the distobuccal aspect of 25 [Table/Fig-1]. On palpation, the swelling was tender, soft in consistency and blanched on pressure. The patient had poor oral hygiene with Grade I mobility and deep caries on 26. The radiograph revealed deep caries involving the pulp, periapical pathology and bone loss in relation to 26 [Table/Fig-2]. Preoperative haematological examination revealed all readings within normal parameters. Based on the clinical appearance of the lesion a provisional diagnosis of pyogenic granuloma was made. The differential diagnosis included peripheral ossifying fibroma, peripheral giant cell granuloma, haemangioma and fibroma.
Preoperative view of the lesion
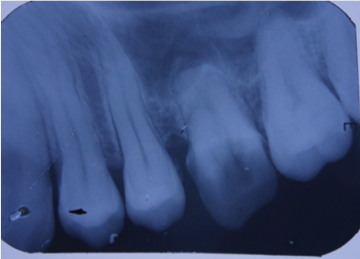
IOPA showing deep caries, peri-apical pathology and bone loss in relation to 26 and external root esorption
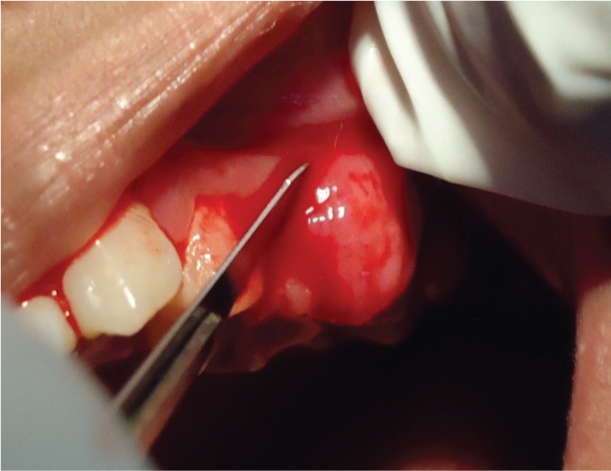
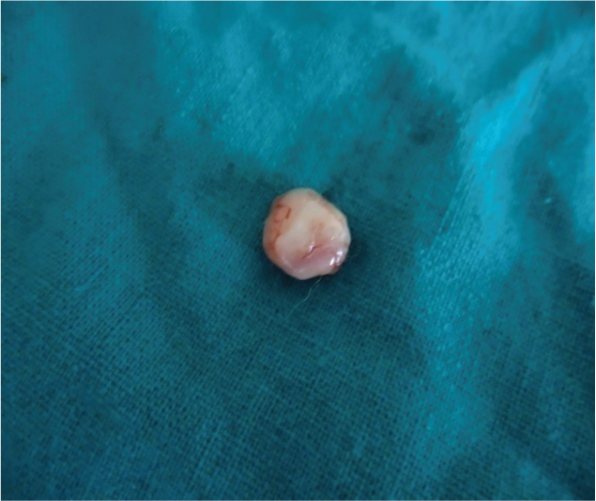
After obtaining informed consent from the patient, a thorough scaling and root planing was done to remove the local irritating factors and patient education was done regarding good oral hygiene maintenance. After 1 week, excision of the growth along with the surrounding gingival tissue was done under local anaesthesia [Table/Fig-3]. Bleeding was controlled by pressure application with a gauze. Thorough curettage was done and complete haemostasis achieved. The tissue was excised [Table/Fig-4,5] following which sutures and periodontal dressing were placed on the operated area, and the patient was given postoperative instructions. The excised tissue was fixed in 10% neutral buffered formalin and was sent for routine histopathological examination. The patient was recalled after 1 week for removal of periodontal pack and suture. The healing was uneventful and satisfactory after one month [Table/Fig-6] and was referred to the Department of Endodontics for the restoration of 26.
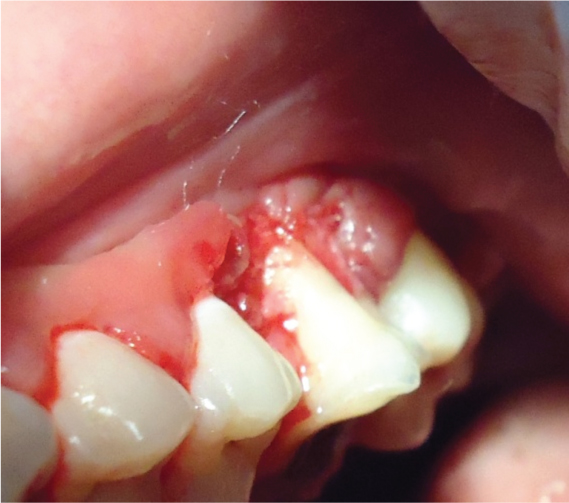
Surgical excision of the lesion
Tissue after surgical excision
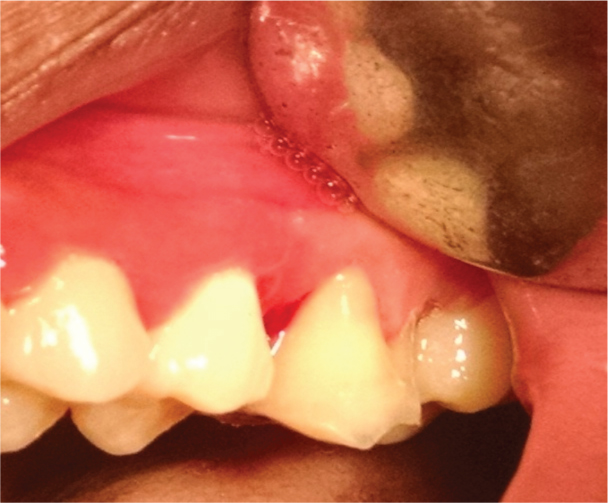
Immediate Postoperative view
Postoperative view after 1 month
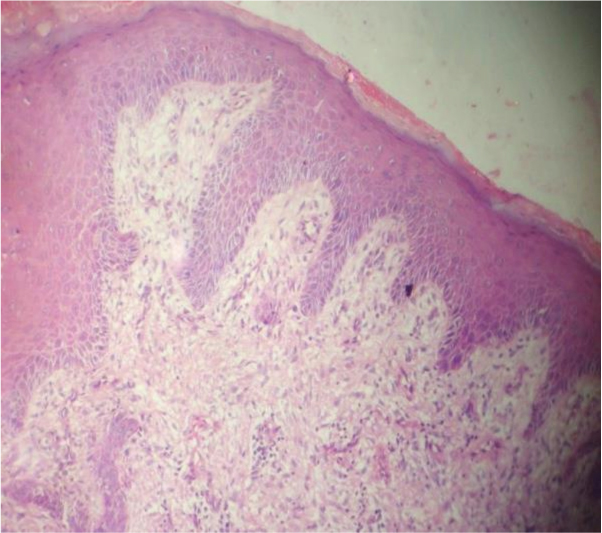
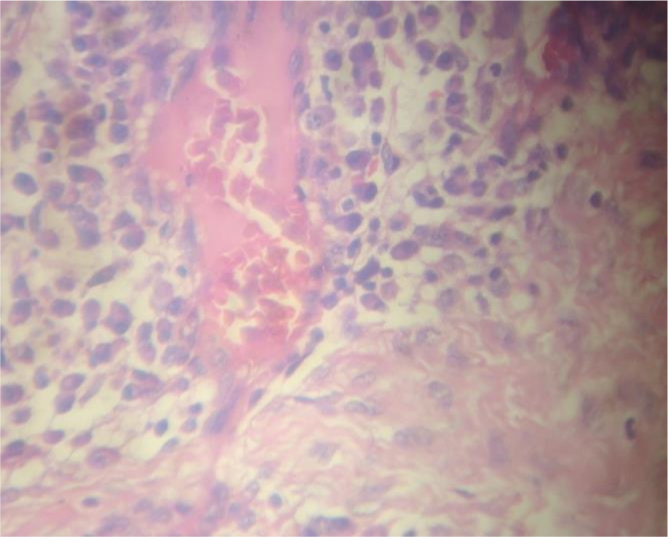
Histopathological report revealed a nodular mass of tissue covered with hyperplastic stratified squamous epithelium showing spongiosis. There was an area of ulceration covered with granulation tissue. The mass is composed of fibrous tissue containing several thin walled blood vessels arranged perpendicular to the epithelial surface [Table/Fig-7,8]. The intervening tissue is densely infiltrated by plasma cells and lymphocytes which is suggestive of an infected capillary haemangioma.
Histological section of the lesion (H&E stain Low power magnification x10x)
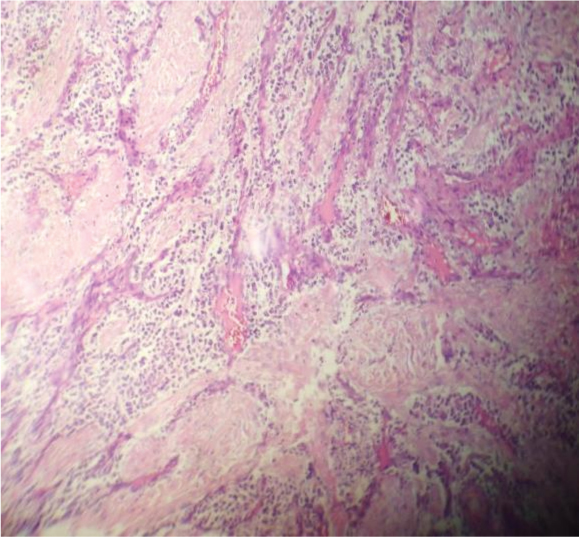
Histological section of the lesion H&E stain high power magnification x 45x)
Discussion
Haemangiomas are benign vascular tumours, classified histologically into capillary and cavernous types [1]. Though capillary haemangioma is a common soft tissue tumour of head and neck, its occurrence in the oral cavity is relatively rare. Capillary haemangiomas are composed of many small capillaries lined with endothelial cells supported in the connective tissue stroma and shows a rapid growth phase followed by gradual involution [2–4]. Pyogenic granuloma is a common, non-neoplastic soft tissue tumour of the oral cavity. These two lesions usually present a clinical dilemma and challenge to the clinician in diagnosing it.
Haemangiomas are considered to be benign tumours of infancy (7%), affecting as many as 12% whites, but it rarely occurs in dark-skinned individuals. The incidence of intraoral capillary haemangiomas are extremely rare [5] and it varies from 0.5-1.0% of all intraoral neoplasms [6,7], especially with female predilection (ratio of 3:1) in second and third decades of life [4]. Nayouki Matsumoto et al., studied 31 cases of intra oral capillary haemangioma and found that most lesions were located on buccal mucosa (45.2%), followed by the tongue (35.5%), lip (9.7%), gingiva (6.5%), and palate (3.2%) [8]. In addition, confusion with other conditions can occur since haemangiomas may mimic other lesions clinically, radiographically and at times histologically. Clinically, haemangiomas of the oral soft tissues appears as a painless, soft, smooth or lobulated, sessile or pedunculated mass and may be seen in any size from a few millimeters to several centimeters [9]. The development of these lesions is usually slow and presents with deep red or bluish red in colour. Periodontally these lesions often appear to arise from the interdental papilla and spread laterally to involve adjacent teeth which is usually painless.
Pyogenic granulomas (PG) are most commonly seen on the gingiva and histologically classified into Lobular Capillary Haemangioma (LCH) type and non-LCH type. LCH pyogenic granuloma is characterized by proliferating blood vessels that are organized in lobular aggregates. The non-LCH pyogenic granuloma shows vascular proliferation that resembles granulation tissue. The foci of fibrous maturation were seen in 15% of non-LCH pyogenic granuloma but were totally absent in LCH type of pyogenic granuloma [10]. It usually occurs on the lips, oral mucosa, tongue, and nasal cavity.
Vascular anomalies of head and neck historically have confused clinicians which have resulted in difficult study, improper diagnosis and inappropriate treatment. The differential diagnosis of haemangiomas includes pyogenic granuloma, peripheral giant cell granuloma, peripheral ossifying fibroma, chronic inflammatory gingival hyperplasia (epulis), epulis granulomatosa, and squamous cell carcinoma [11]. The classification of haemangiomas is based on histological appearance, therefore histopathological assessment remains the most accurate and satisfactory means of diagnosis. Since CH and PG exhibits similar clinical features, biopsy of the lesion is mandatory for definitive diagnosis and to rule out more serious conditions.
The management of haemangiomas of the oral mucosa varies according to various factors like the age of the patient, the size of the lesion, the site of involvement and the clinical nature of the haemangioma [12]. The most common treatment of choice for haemangioma is surgical excision of the lesion with or without ligation of vessels and embolization [13]. Recently other treatment modalities are also developed which includes steroid therapy, electrosurgery, Nd: YAG laser, CO2 laser, cryosurgery and use of sclerosing agents. Surgical management should be executed with caution taking into consideration the possibility of bleeding intraoperatively and postoperatively.
The present case in the discussion is worthy of importance because of its uncommon location on the gingiva and were rarely encountered by dentists. In this case the lesion was painful and symptomatic which may be due to deep caries and periapical pathology related to the tooth. Radiographs were advised to rule out malignancy and to identify the presence of any other foreign body which has to be removed along with the lesion [14]. In this case, surgical excision was selected as the treatment modality based on the provisional diagnosis of pyogenic granuloma, in addition to the lesion being small sized on presentation and submitted for histopathological examination. Usually surgical excision of haemangiomas produce profuse bleeding but in this case minimal bleeding was encountered which might be due to the fact that the haemangioma might not be in an active proliferative stage. The patient responded well to the treatment, and was kept on maintenance visits for 6 months. No recurrence is reported till date.
Conclusion
Capillary haemangioma is a lesion that clinically resembles pyogenic granuloma which is identified based on its histological findings. Even though it is asymptomatic, its site and size may require immediate careful intervention. It often presents as a diagnostic dilemma to the clinician. This necessitates biopsy of such lesions for establishing a definite diagnosis and proper management and prevention of various complications. Most importantly, the surgical excision of CH should be performed with caution taking into consideration the intra-operative and postoperative bleeding. CH is associated with increased risk of postoperative recurrence that necessitates longer follow up of the site.
[1]. Mills SE, Cooper PH, Fechner RE, Lobular capillary hemangioma: The underlying lesion of pyogenic granuloma. A study of 73 cases from the oral and nasal mucous membraneAm J Surg Patho 1980 4:470-79. [Google Scholar]
[2]. Bayrak S, Dalci K, Tansel H, Capillary hemangioma of the palatal mucosa: Report of an unusual caseSÜ Dishek Fak Derg 2010 19:87-89. [Google Scholar]
[3]. Chen YK, Lin LM, Huang HC, Lin CC, Yan YH, A retrospective study of oral and maxillofacial biopsy lesions in a pediatric population from southern TaiwanPediatr Dent 1998 20:404-10. [Google Scholar]
[4]. Neville BW, Damm DD, Allen CM, Bouquot JE, Oral & Maxillofacial Pathology 2002 2nd editionPhiladelphiaSaunders:390-92. [Google Scholar]
[5]. Schoen FJ, Vessels B, Robbins and Cotran: Pathological basis of disease 2004 7th editionPhiladelphiaSaunders:511-54.In: Kumar V, Abbas AK, Fausto N [Google Scholar]
[6]. Dahlin DC, Unni KK, Bone tumours: General aspects and data on 542 cases 1986 14Springfield III:3-17. [Google Scholar]
[7]. Yih WY, Ma GS, Merrill RG, Sperry DW, Central hemangioma of the jawsJ Oral Maxillofac Surg 1989 47:1154-60. [Google Scholar]
[8]. Matsumoto N, Tsuchiya M, Nomoto S, Matsue Y, Nishikawa Y, Takamura T, CD105 expression in oral capillary hemangiomas and cavernous hemangiomasJournal of Oral Science 2015 57:45-53. [Google Scholar]
[9]. Jananni M, Gubernath U, Mahendra J, Sivaramakrishnan M, Capillary hemangioma of gingiva mimicking as pyogenic granuloma: Report of two casesJ Interdiscip Dent 2012 2:218-20. [Google Scholar]
[10]. Epivatianos A, Antoniades D, Zaraboukas T, Zairi E, Poulopoulos A, Kiziridou A, Pyogenic granuloma of the oral cavity: Comparative study of its clinicopathological and immunohistochemical featuresPatho Int 2005 55:391-97. [Google Scholar]
[11]. Wood NK, Goaz PW, Differential diagnosis of oral and maxillofacial regions 1997 5th editionMosby:549-50. [Google Scholar]
[12]. Rachappa MM, Triveni MN, Capillary hemangioma or pyogenic granuloma: A diagnostic dialemmaContemporary clinical dentistry 2010 12:119-22. [Google Scholar]
[13]. Açikgöz A, Sakallioglu U, Ozdamar S, Uysal A, Rare benign tumours of oral cavity: Capillary hemangioma of palatal mucosa: A case reportInt J Paediatr Dent 2000 10:161-65. [Google Scholar]
[14]. Handa R, Sheikh S, Shambulingappa P, Aggarwal A, Mago J, Salaria S, Capillary hemangioma of palate: A case reportPakistan Oral & Dental Journal 2013 33(1):55-57. [Google Scholar]