Fibroepithelial Polyps of the Vagina in Pregnancy
Sunil Kumar Samal1, Setu Rathod2, Seetesh Ghose3
1 Assistant Professor, Department of Obstetrics and Gynaecology, Mahatma Gandhi Medical College and Research Institute, Puducherry, India.
2 Assistant Professor, Department of Obstetrics and Gynaecology, Mahatma Gandhi Medical College and Research Institute, Puducherry, India.
3 Professor and Head, Department of Obstetrics and Gynaecology, Mahatma Gandhi Medical College and Research Institute, Puducherry, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Setu Rathod, 4-D, Type II Staff Quarters, Mahatma Gandhi Medical College, Pillaiyarkuppam, Puducherry-607402, India.
E-mail: seturathod@gmail.com
Pedunculated polyps, Polyposis Vaginalis, Pseudusarcomatous polyps of vagina
A 25-year-old primigravida mother at 36 weeks pregnancy presented with mass descending per vaginum for last one month. In the antenatal history she had regular antenatal visits without any pregnancy complication. General and systemic examination revealed no abnormality. On local examination of external genitalia, there was a large pedunculated polyp [Table/Fig-1] of the vagina which measured 8 x 6 cm with multiple large atypical polyps found inside the vagina. Cervix was healthy and os was closed. An excisional biopsy of the largest polyp was done and histopathology revealed benign fibroepithelial polyps. So decision was taken to allow spontaneous vaginal delivery. Since operative vaginal delivery should be avoided in such cases to reduce the risk of trauma and haemorrhage [1]. Her pregnancy continued well and she went in to spontaneous labour at 40+2 weeks. But caesarean section was done for intrapartum fetal distress. On follow up after 6 weeks, the patient is asymptomatic and the polyps were reduced in size and number which proved their hormone dependant nature [Table/Fig-2].
Large pedunculated polyp with multiple fibroepithelial polyps of vagina
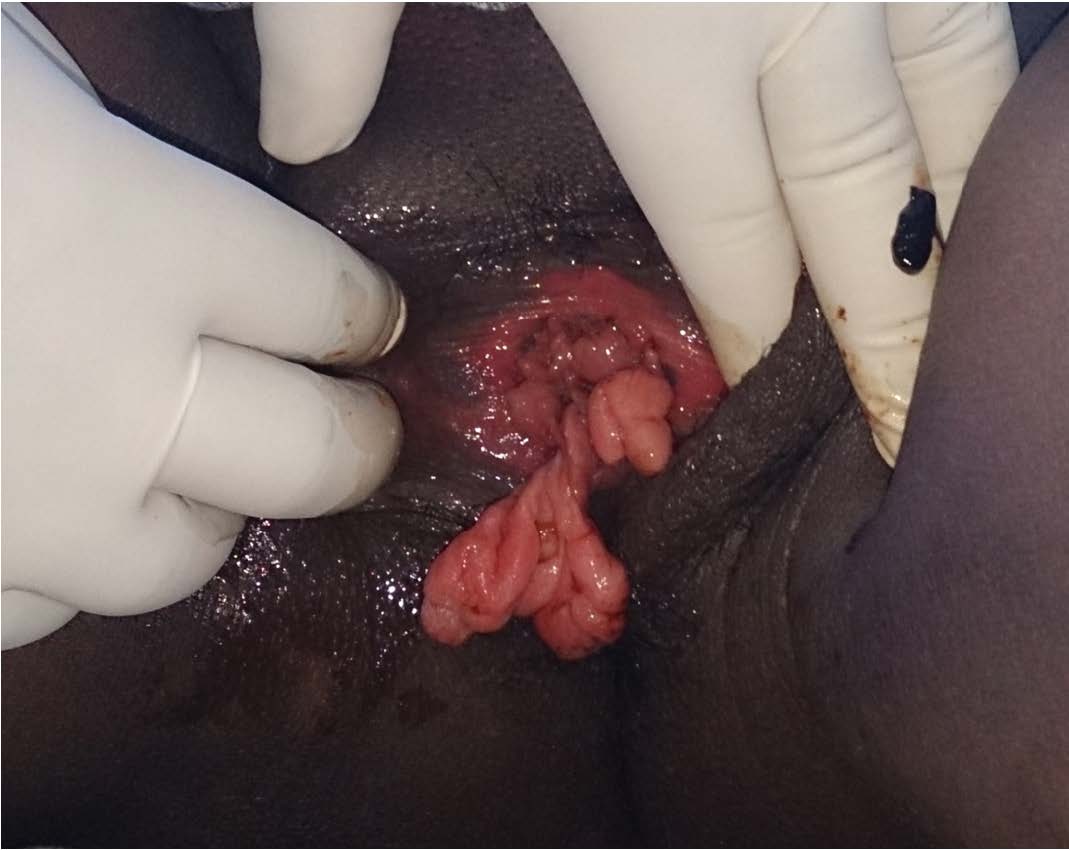
After 6 weeks polyps reduced in size and numbers
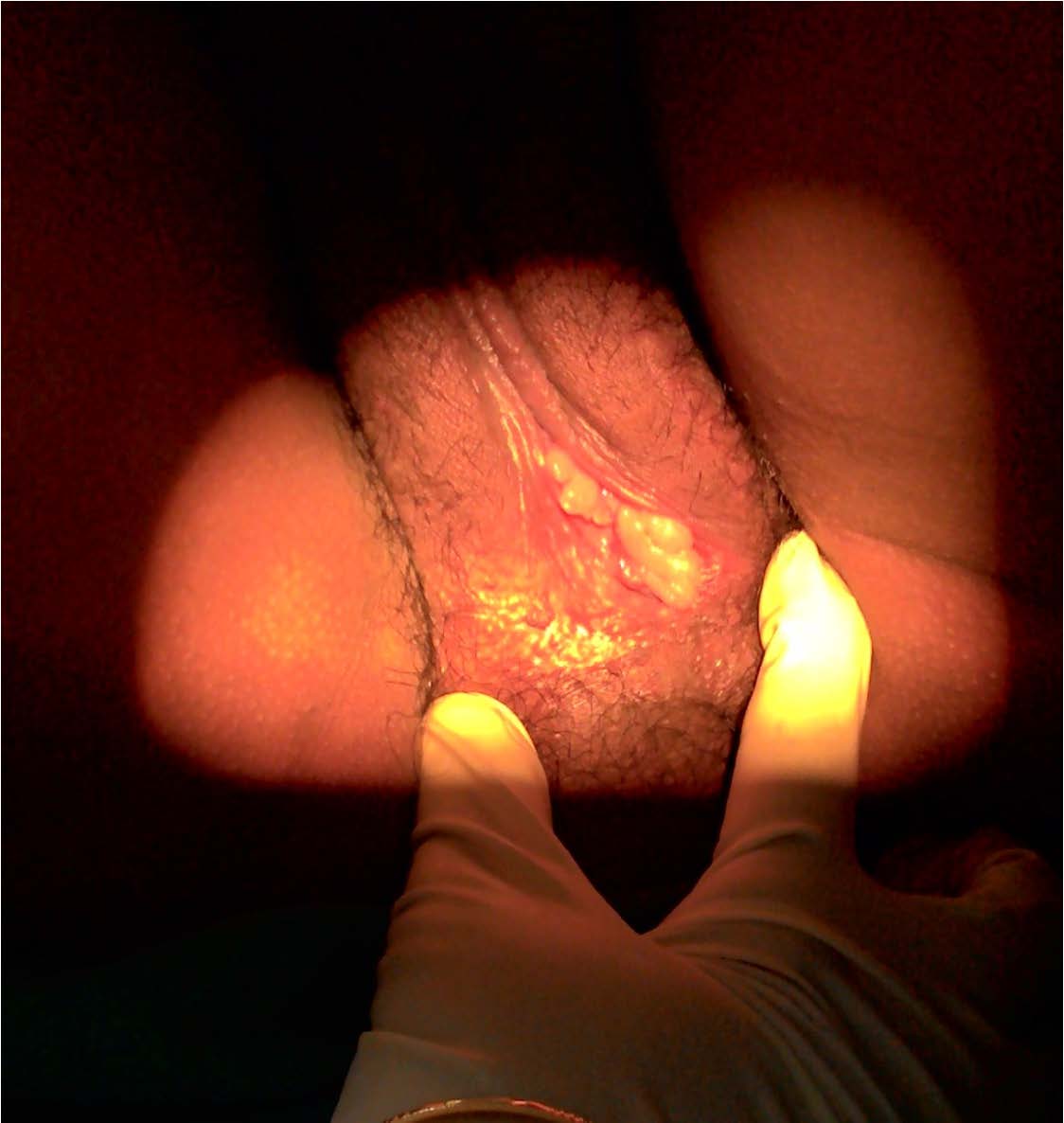
Fibroepithelial polyps of the vagina (FEPV) are mucosal polypoid lesions with a connective tissue core covered by a benign squamous epithelium [2]. They are thought to be rare as few cases are reported in literature and the cases are compared with the present case in [Table/Fig-3].
Comparison of reported cases in literature with the present case
| Author | Case history | Treatment | Follow up |
|---|
| Pearl ML et al., [1] in 1991 | 38-year pregnant lady with FEPV | Biopsy confirmed diagnosisUnderwent spontaneous vaginal delivery | Polyps reduced in size and number after 6 weeks |
| Halvorsen TB et al., [2] in 1992 | 62 cases of FEPV | Histopathology confirmed the diagnosis | Hormonal factors modulate the growth of FEPV during pregnancy |
| Hartmann CA et al., [3] in 1990 | 4 cases of FEPV | Histopathology confirmed the diagnosis | FEPV expressed vimentin, desmin, and receptors for estrogen and progesterone |
| Ramirez Melgar E et al., [4] in 2000 | 27-year woman with a great pedunculated polyp | Local excision after biopsy confirmed the diagnosis | No recurrence |
| Nucci MR et al., [5] in 2000 | 33 cases of FEPV among which 5 were pregnant | Local excision | Three of 21 patients with follow-up had local, nondestructive recurrence |
| Tobon H et al., [6] in 1989 | 15-year old pregnant lady with multiple polyps in vagina and portio vaginalis of cervix | Spontaneous vagina delivery | Polyps disappears 6 weeks postpartum |
| Lasso de la Vega J et al., [7] in 1995 | A case of pregnancy with FEPV | Caesarean sectionLocal excisional biopsy | No recurrence |
| Maenpaa J et al., [8] in 1988 | 25-year old primigravida with large FEPV with intercurrent human pappiloma virus infection of vagina | Caesarean section followed by excisional biopsy | No recurrence |
| Burt RL et al., [9] in 1976 | 5 cases of FEPV | Local excision after biopsy confirmed the diagnosis | No recurrence |
| Present case [2015] | 25-year primigravida with large FEPV | Biopsy confirmed the diagnosisCaesarean section for obstetric indication | Polyps reduced in size and in number after 6 week post partum |
The aetiology of FEPV may be as a result of a granulation tissue reaction after some local injury of the vaginal mucosa. It is because of delayed differentiation of myofibroblastic stromal cells which explains why granulation tissue sometimes does not contract properly but turns into polyps [2]. But during pregnancy hormonal factors may modulate the growth of FEPVs. Hartmann CA et al., reported after examination with immunohistochemistry that FEPV expressed vimentin, desmin, and receptors for estrogen and progesterone which indicates the hormone dependant nature of these polyps [3]. Although benign, it can be confused with malignant connective tissue lesions because of its bizarre histology. The differential diagnoses are sarcoma botryoides, rhabdomyosarcoma and mixed mesodermal tumour [4]. Histopatholgy confirms the diagnosis. The other terminologies of FEPV reported in literature are Pseudosarcoma botryoides, Cellular pseudosarcomatous fibroepithelial stromal polyps and Polyposis vaginalis [5,6]. Treatment of FEPV is simple local excision [7,8]. It can be performed after pregnancy as an interval procedure when the vaginal vascularity has returned to normal. Recurrence is extremely uncommon [9]. Nucci MR et al., studied 65 cases of FEPV and reported that awareness of the spectrum of histopathologic features that these lesions can exhibit and is crucial in their accurate diagnosis thus avoiding potential overtreatment [5].
FEPV in pregnancy is a rare lesion. Although benign, it can be confused with some malignant tumours. Histopathology confirms the diagnosis. Treatment is simple local excision and recurrence is uncommon. Hence knowledge of clinical and histopathological features of these lesions is important for accurate diagnosis for avoiding potential overtreatment.
[1]. Pearl ML, Crombleholme WR, Green JR, Bottles K, Fibroepithelial polyps of the vagina in pregnancyAm J Perinatol 1991 8(4):236-38. [Google Scholar]
[2]. Halvorsen TB, Johannesen E, Fibroepithelial polyps of the vagina: are they old granulation tissue polypsJ Clin Pathol 1992 45(3):235-40. [Google Scholar]
[3]. Hartmann CA, Sperling M, Stein H, So-called fibroepithelial polyps of the vagina exhibiting an unusual but uniform antigen profile characterized by expression of desmin and steroid hormone receptors but no muscle-specific actin or macrophage markersAm J Clin Pathol 1990 93(5):604-08. [Google Scholar]
[4]. Ramirez Melgar E, Kunhardt Urquiza E, Romero Arauz J, García Barcenas JL, Fibroepithelial polyp of the vagina. Report of a caseGinecol Obstet Mex 2000 68:368-70. [Google Scholar]
[5]. Nucci MR, Young RH, Fletcher CD, Cellular pseudosarcomatous fibroepithelial stromal polyps of the lower female genital tract: an underrecognized lesion often misdiagnosed as sarcomaAm J Surg Pathol 2000 24(2):231-40. [Google Scholar]
[6]. Tobon H, McIntyre-Seltman K, Rubino M, Polyposis vaginalis of pregnancyArch Pathol Lab Med 1989 113(12):1391-93. [Google Scholar]
[7]. Lasso de la Vega J, Singh Gómez C, Lasso de la Vega J Jr, Pseudosarcoma botryoides during pregnancyRev Med Panama 1995 20(1-2):45-49. [Google Scholar]
[8]. Maenpaa J, Soderstrom KO, Salmi T, Ekblad U, Large atypical polyps of the vagina during pregnancy with concomitant human papilloma virus infectionEur J Obstet Gynecol Reprod Biol 1988 27(1):65-69. [Google Scholar]
[9]. Burt RL, Prichard RW, Kim BS, Fibroepithelial polyp of the vagina. A report of five casesObstet Gynecol 1976 47(1):52-54. [Google Scholar]