Materials and Methods
After accomplishing Institutional Ethical Committee Clearance our study proceeded with 100 healthy subjects (males: 58%, females: 42 %) between 25 and 60 years of age who were attending tertiary health care center, in Southern India. These subjects had come to the health center for a routine health check conducted on behalf of their working institution. The nature of the study was explained to the subjects and then they were enrolled after obtaining their Informed Consent. In this cross–sectional study of randomly selected subjects those with the history of dyslipidemia, hypertension, diabetes mellitus, malignancy or any other major chronic illness, were excluded from the study, so were the individuals giving a history of use of lipid lowering agents, and/or other drug delivery system and family history of lipid related disorders. This was followed by a detailed clinical examination, including their general examination (pulse, blood pressure, respiratory rate, febrile conditions, pallor, oedema, icterus, cyanosis, clubbing, and lymphadenopathy) and systemic examination (cardiovascular, respiratory, per abdomen and central nervous system), haematological and serum lipid profile estimation. Thus, on the basis of a self- structured questionnaire and the clinical examination finally a total of 100 healthy males & females, were included in this analytical study. Independent variables measured were the four anthropometric parameters of this study, as WC in cm, measured at the end of normal expiration, midway between lower costal margin and iliac crest using a non- elastic tape. Hip circumference (HC) was measured, in cm, with subject standing in relaxed position, at the level of greater trochanters corresponding to maximum protrusion of gluteal muscles. WHR was later calculated by the formula,
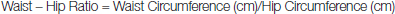
Body weight and height were measured without shoes and subject standing erect preferably with light or minimal clothing using an electronic measuring scale. WHtR was as well estimated using the following formula [9,10].
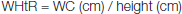
BMI was calculated based on Quetelet’s Index [11], as,
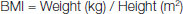
Each subject’s blood samples were collected after an overnight fast of 12-14 hours in Vacutainer, before breakfast. The serum was separated within one hour of the blood collection, then the samples were evaluated accordingly, if not, the samples were stored at -200C until analysed for lipid profile. Roche/Hitachi auto analyser was used to analyse the serum samples for lipid profile values [12–15]. Depending on the cut off values for all the males and females, the subjects were then classified into obese and non-obese groups. The WHO specified standard values for South Asian population [6] were considered. The cut off levels for obesity based on the WHO values are as follows [Table/Fig-1].
Standard cut off values for determining obesity based on anthropometric parameters
| Gender | Anthropometric parameter |
|---|
| BMI (kg/m2) | WHR | WHtR | WC (cm) |
|---|
| Male | 23 | > 0.9 | > 0.95 | >80 |
| Female | 23 | > 0.8 | > 0.90 | >90 |
(WC – waist circumference, WHR – waist hip ratio, WHtR – waist height ratio, BMI – body mass index, cm – centimeters, kg/m2 - kilograms per meter square)
According to the ATP III classification, dyslipidemia was defined as TC > 200 mg/dl, TG > 150 mg/dl, HDL < 40 mg/dl, and LDL > 100 mg/dl and based on these values subjects with lipid profile values in either cutoff levels were again categorized as obese and non-obese accordingly [16]. Individuals with 2 or more deranged lipid values were considered obese. We then compared all the parameters in terms of their capacity to identify the entire enrolled healthy subject as obese or non-obese and their individual lipid profile values.
Statistical Analysis
Data obtained was statistically analysed using SPSS version 16. Sensitivities and positive predictive values of anthropometric indices were compared. Significant value ‘p’ was taken to be < 0.001 and < 0.05.
Results
Along with a detailed clinical examination and anthropometric assessment, considering all the inclusion and exclusion criteria and based on self-structured questionnaire, our study included a total of randomly selected apparently healthy 58 males and 42 females. Mean age of all males was 42.26±7.45 years and females was 44.29±8.16 years.
Data from [Table/Fig-2] gives us the idea of the number of subjects considered to be obese and non - obese when the anthropometric parameters alone were considered (according to WHO standard cut-off values) without taking into consideration the lipid profile values off all the enrolled subjects.
Total number of Obese and Non – Obese Subjects based on various indices in both the genders
| WC | WHR | WHtR | BMI |
|---|
| Male | Female | Male | Female | Male | Female | Male | Female |
|---|
| Obese | 35 | 33 | 37 | 24 | 15 | 28 | 26 | 28 |
| Non Obese | 23 | 9 | 21 | 18 | 43 | 14 | 32 | 14 |
(WC – waist circumference, WHR – waist hip ratio, WHtR – waist height ratio, BMI – body mass index, cm – centimeters, kg/m2 - kilograms per meter square)
When average values of measurements of all parameters in both the genders were calculated as shown in [Table/Fig-3a,b], there was statistically significant (‘p’<0.001) difference between obese and non-obese anthropometric values in both males and females. We did consider BMI values same in both the genders. Within any given age category, men had higher anthropometric measurements than women.
Mean values±SD of all anthropometric indices in males
| WC (cm) | WHR | WHtR | BMI (kg/m2) |
|---|
| Obese | 97.43 ± 6.21* | 0.96 ± 0.04* | 0.61 ± 0.05* | 27.72 ± 2.4* |
| Non obese | 82.27 ± 5.33* | 0.83 ± 0.033* | 0.51 ± 0.03* | 22.80 ± 2.11* |
* - ‘p’ < 0.001
Mean values±SD of all anthropometric indices in females
| WC (cm) | WHR | WHtR | BMI (kg/m2) |
|---|
| Obese | 91.82 ± 5.18* | 0.92 ± 0.06* | 0.60 ± 0.04* | 27.7± 3.44* |
| Non - obese | 71.68 ± 7.33* | 0.78 ± 0.03* | 0.48 ± 0.03* | 21.82 ± 1.98* |
* - ‘p’ < 0.001
Serum lipid profile values as shown in [Table/Fig-4] were statistically significantly (‘p’< 0.001) higher in obese males and females than the non-obese individuals.
Biochemical parameters (Mean Values ± SD of lipid levels in mg/dl*)
| Lipid type | Gender | Obese | Non-obese |
|---|
| TC | Male | 225.28± 24.65** | 189.77 ± 23.08*** |
| Female | 229.23± 26.35** | 179.54± 22.81** |
| TG | Male | 184.8 ± 29.22*** | 134.87 ± 32.22*** |
| Female | 135.9± 12.22** | 85.90 ± 15.22** |
| HDL | Male | 41± 6.23** | 53 ± 5.83** |
| Female | 48.16± 9.55** | 54 ± 6.88** |
| LDL | Male | 123.3± 12.61** | 86.45 ± 14.61*** |
| Female | 134.78± 11.06** | 83.37 ± 8.01** |
(TC – total cholesterol, TG – triglyceride, HDL – high density lipoprotein, LDL – low density lipoprotein* - milligrams/deciliter, ** - ‘p’ < 0.001, *** - ‘p’ < 0.05).
Finally based on anthropometric values, both obese and non-obese subjects were classified based on their serum lipid profile findings with normal and abnormal values as shown in [Table/Fig-5].
Anthropometric Indices and Lipid Values in obese and non-obese subjects
| Abnormal FLP | Normal FLP |
|---|
| Males | Females | Males | Females |
|---|
| Non-obese | Obese | Non-obese | Obese | Non-obese | Obese | Non-obese | Obese |
|---|
| WC | 21 | 32 | 4 | 23 | 2 | 3 | 5 | 10 |
| WHR | 18 | 33 | 9 | 17 | 3 | 4 | 9 | 7 |
| WHtR | 28 | 11 | 5 | 18 | 15 | 4 | 9 | 10 |
| BMI | 14 | 24 | 6 | 16 | 18 | 2 | 8 | 12 |
Comparison of the selected anthropometric measures with respect to their ability to correctly identify dyslipidemia in healthy adults and predict rightly its presence is shown in preceding [Table/Fig-6]. There is a significant difference between the percentages of individuals whose risk factor status in terms of presence of dyslipidemia would be correctly predicted using WHR in males, WC and WHtR in females compared to BMI.
Percent Sensitivity and positive predictive value of anthropometric parameters in predicting dyslipidemia in healthy adults
| Anthropometric Parameter | Gender | Sensitivity | Positive Predictive Value |
|---|
| WC (cm) | Male | 67 | 79 |
| Female | 85 | 70 |
| WHR | Male | 65 | 90 |
| Female | 65 | 71 |
| WHtR | Male | 28 | 74 |
| Female | 79 | 92 |
| BMI (kg/m2) | Male | 64 | 72 |
| Female | 73 | 57 |
Discussion
The intention of this study was to compare the most frequently used anthropometric parameters WC, WHR, WHtR and BMI as predictors for the presence of dyslipidemia. WC associates well with visceral body fat mass in adults. WHR and WHtR in adults are successfully proved to be useful predictors for cardiovascular disease risk factors and coronary heart disease [17–20]. BMI was chosen because it is the most widely used index for the evaluation of obesity both in adults in daily practice. Non-communicable diseases (NCDs) caused as a result of dyslipidemia can be prevented by identification of individuals at risk by screening with simple anthropometric measurements, followed by individualized counselling, modification in lifestyle and/or by appropriate treatment [18,21]. Anthropometric measurements are considered as dimensions of obesity and part of diagnostic components of NCDs [19,20]. Our study has inferred that of all four anthropometric measurements used to assess healthy males and females, as shown in [Table/Fig-6], WHR in males and WC in females have most correctly anticipated deranged lipid profile in healthy females and males who are obese. The higher positive predictive value of WHR in males (90%) and of WHtR in females (92%) indicates that these healthy individuals are more prone to develop NCDs as an effect of their dyslipidemia. Our study has found that compared to BMI, the other 3 parameters are more reliable in predicting dyslipidemia in healthy adults.
Thus, in our study, we can recommend that WC, being a more sensitive anthropometric parameter, can be a better indicator of abnormal fat content within the body in males and WHR in females compared to BMI. This has also been validated by Quebec Health Survey done by Lemieux et al., [22]. WC, WHR, WHtR and BMI, though are simple adiposity measures, BMI does not reflect regional fat distribution. Individuals with similar BMI values can vary considerably in their abdominal fat mass [23,24]. Asians have large percentages of body fat at low BMI values [25]. BMI misclassifies substantial fractions of individuals as obese or non-obese; in general, BMI is less accurate classifying men than women.
Our study is in accordance with another wide based study which has inferred that WHtR was more closely related to metabolic risk factors than was BMI [19,26]. WC, and not BMI, explains obesity-related health risk, a possible explanation for this weakness of BMI may be BMI considers not just fat mass but bones, muscle and visceral organ mass within body of an individual [21,27,28]. A recently released WHO guideline for obesity screening suggested additional public health action points for Asian populations, i.e. a BMI of ≥ 23 represents increased risk and a BMI of ≥ 27.5 represents a high risk in being susceptible to NCDs [20,24,28–31].
Our study observed that compared to BMI; WC and WHR are good indicators for abnormal serum lipid levels in adults and additionally provide supplementary information about central fat distribution. This is in agreement with Rotterdam study of Visscher et al., [32], and fieldwork done by Ko GT et al., in the Chinese men and thus validates that WC and WHR are better predictors of dyslipidemia than BMI [33]. Studies with computed tomography sections of human subjects have disclosed the fact of closer affiliation between dyslipidemia and WC which includes intra-abdominal fat [34,35]. A surplus exposure of liver to fatty acids with raised WC is most likely associated with elevated predisposition to NCDs because of its relation with visceral fat accumulation [27,35]. The use, therefore, of indices that correlate to visceral fat is more justified.
Our study findings of WHtR having higher positive predictive value in females is in accordance with meta– analysis of Savva et al., [34], who concluded that WHtR is a more reliable predictor of cardio-metabolic risk factor. Another study done on Japanese males [35] it was concluded that WHR is an important contributor not only to NIDDM but also to impaired glucose tolerance, blood pressure, and serum lipids, thus, a measure of obesity that takes into account increased risk of obesity related illnesses due to accumulation of abdominal fat is desirable. WC or WHtR has been found to be a better predictor of CVD risk factors than BMI in Korean adults [36]. Earlier deterrence of unnecessary weight expansion can help reduce dyslipidemia linked diseases. If not, then recognizing early dyslipidemia can help in setting up corrective processes to reduce disease burden. We recommend using preferably WC, WHR or WHtR as inexpensive and easy method in clinical and epidemiological fields. The main constraints of this project were that we did not consider other confounding variables like physical activity level, dietary food intake and socio-economic status of participants. A greater number of subjects considered for similar study on large scale therefore are advisable.
Conclusion
In the present study while an attempt was made to determine and comparatively evaluate all the four anthropometric parameters we have concluded that WC is a more sensitive in identifying healthy individuals as having abnormal serum lipid values and WHR & WHtR as a reliable predictor of dyslipidemia in males and females, respectively. Prevention of future untoward health hazards by including these into routine health check-up will boost obesity related evaluation of cardio vascular risk factors.
(WC – waist circumference, WHR – waist hip ratio, WHtR – waist height ratio, BMI – body mass index, cm – centimeters, kg/m2 - kilograms per meter square)
(WC – waist circumference, WHR – waist hip ratio, WHtR – waist height ratio, BMI – body mass index, cm – centimeters, kg/m2 - kilograms per meter square)
* - ‘p’ < 0.001
* - ‘p’ < 0.001
(TC – total cholesterol, TG – triglyceride, HDL – high density lipoprotein, LDL – low density lipoprotein* - milligrams/deciliter, ** - ‘p’ < 0.001, *** - ‘p’ < 0.05).