Bilateral Multifocal Renal Angiomyolipoma Associated with Wunderlich’s Syndrome in A Tuberous Sclerosis Patient
Sushma Shankar1, Kiran Shankar Hulikanthimatt2, Shreeharsha Mallappa Awatti3, Suresh Turuvekere Narayanrao4
1 Assistant Professor, Department of Pathology, Sri Devaraj Urs Medical College, SDUAHER, Tamaka, Kolar, India.
2 Post Graduate Student, Department of Surgery, Sri Devaraj Urs Medical College, SDUAHER, Tamaka, Kolar, India.
3 Assistant Professor, Department of Urology, Sri Devaraj Urs Medical College, SDUAHER, Tamaka, Kolar, India.
4 Professor, Department of Pathology, Sri Devaraj Urs Medical College, SDUAHER, Tamaka, Kolar, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Sushma Shankar, No 402, 4th Floor, Garuda Residency, Next to Shobha Rose Apartments, Whitefeild Main Road, Bangalore, India. E-mail : dr.sushma1985@gmail.com
Renal Angiomyolipoma (renal AML) is a benign clonal neoplasm with a incidence of 0.3-3%, occurring as isolated sporadic entity or in association with Tuberous sclerosis (TS) in 80% cases. Multiple, bilateral renal AML are considered diagnostic of Tuberous sclerosis. Wunderlich’s syndrome, a urological emergency is a spontaneous nontraumatic bleeding into subcapsular and or peri-renal space and is a life threatening complication of renal AML occurring in 10% cases which has to be timely diagnosed and treated. Here, we present an unusual case of TS with bilateral, multifocal renal AML in a 25-year-old female who presented with Wunderlich’s syndrome, which is a rare but life threatening complication that has to be suspected, timely diagnosed and treated. We have discussed the importance of early diagnosis, timely treatment, follow up and education of patient and relatives of the possible complications associated.
Bilateral, Female, Life threatening
Case Report
A 25-year-old female presented to urology OPD with complaints of abdominal pain, mass in right side of abdomen, fever since two months. She gave history of sudden increase in pain and size of the mass and frank haematuria. On examination, patient was pale, had multiple adenoma sebaceum on her face [Table/Fig-1]. Abdominal examination revealed tender, firm, bimanually palpable mass extending from the right hypochondrium to right lumbar region.
Multiple adenoma sebaceum on face
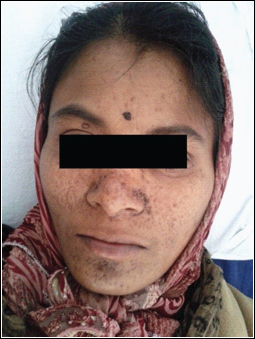
A positive history of mother and brother having adenoma sebaceum was present. There was no history of seizures, loss of vision. Haemoglobin was 9gm/dl. Urine microscopy showed red cell casts and RBC’s. Further investigations were done. Ultrasonography revealed bilateral enlarged kidneys showing multiple, nodular, hyperechoic lesions with right kidney showing a large haematoma.
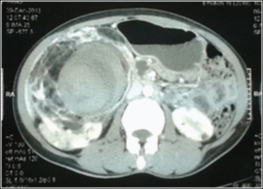
Contrast enhanced CT abdomen revealed bilateral enlarged kidneys showing multiple fat densities. Right kidney showed a large heterogenous lesion measuring 13.2 x 11.5 x 7.5 cms and large sub acute haematoma measuring 8.2 x 8.1 cms in the lower pole suggestive of ruptured AML [Table/Fig-2]. CT brain revealed multiple calcified sub ependymal nodules [Table/Fig-3].
CT abdomen showing bilateral renal AML with large intratumoural bleed on right side
CT brain showing calcified Sub ependymal nodules
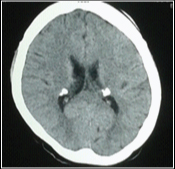
A diagnosis of TS with bilateral, multifocal renal AML with Wunderlich’s syndrome was made. Patient was transfused 2 pints of packed RBCs. Exploratory laprotomy and enucleation of tumour in right kidney along with the haematoma was done. Histopathology showed a well encapsulated globular soft tissue mass measuring 15 x 11x 8cm weighing 850g, with the haematoma measuring 8x8 cm with compressed renal tissue on one side. Cut surface showed yellow to tan tumour mass with areas of haemorrhage.
Microscopy revealed a tumour composed of areas of mature adipose tissue, thick walled, hyalinised blood vessels and bundles of smooth muscles with perivascular epitheloid cells [Table/Fig-4]. No evidence of nuclear atypia or increased mitoses seen. Immunohistochemistry with HMB-45 showed immunoreactivity in the perivascular epitheloid cells [Table/Fig-5]. The diagnosis of renal AML was made. Patient recovered uneventfully and was discharged from the hospital on the 5th postoperative day. At 6 months follow up, there was neither evidence of tumour recurrence on same side nor evidence of an obvious increase in size of nodules in the opposite kidney.
Angiomyolipoma showing fat, hyalinised blood vessels and smooth muscles (H&E, x100)
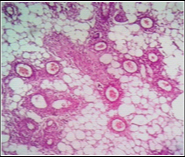
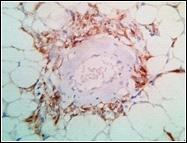
Perivascular epitheloid cells showing HMB-45 immuno reactivity (IHC, x100)
Discussion
Tuberous sclerosis (TS) or Bournville-Pringle disease is a relatively rare autosomal dominant disorder with variable penentrance affecting approximately 1 in 10,000 population [1,2]. Classically the disease is described as a clinical triad of adenoma sebaceous, mental retardation and seizures. The pathophysiology can include glial tumours of brain, adenoma sebaceus of skin, rhabdomyoma of heart and hamartomatous tumours of thyroid, retina, liver, pancreas, lung, kidney, adrenals and ovaries [1,2]. Three types of renal involvement have been described in TS: a) Renal AML (40-80%); b) Cystic disease (occasionally); c) Renal cell carcinoma, with the most common renal lesion being AML [3]. A rare concurrence of Bilateral RAML and Renal cell carcinoma was reported by Khallouk A et al., in a 35-year-old man with TS [4].
Histologically AML is a benign renal neoplasm composed of mixture of 3 tissue types- benign smooth muscle in sheets and bundles, thick walled muscular blood vessels which lack elastic lamellae and mature fat [1]. One of the most feared complications of renal AML is Wunderlich’s syndrome, occurring in 10% of patients. By definition, Wunderlich’s syndrome is a spontaneous non traumatic bleeding into the sub capsular and or peri renal space, and is characterized by the classic triad of symptoms of acute abdominal pain, a palpable mass and hypovolemic shock [5], as seen in the present case. Similar cases of Wunderlich’s syndrome have been described in the literature which are tabulated below [Table/Fig-6].
Table showing cases of Wunderlich’s syndrome from the literature
| Author | Age of patient | Sex of patient | Laterality | Association with TS | Year of reporting | Maximum diameter of index lesion |
|---|
| Khan AS et al.,[1] | 29 | F | Bilateral | Present | 2003 | 40 cm |
| Mongha R et al., [5] | 32 | F | Bilateral | Present | 2008 | Not mentioned |
| Nabi N et al., [6] | 47 | F | Bilateral | Present | 2007 | Not mentioned |
| Medda M et al., [7] | 50 | F | Unilateral | Absent | 2009 | 22 cm |
| Kushwaha R et al.,[8] | 35 | F | Unilateral | Present | 2010 | 15 cm |
| Lin CY et al., [9] | 57 | F | Unilateral | Absent | 2011 | Huge |
| Vaddi et al., [10] | 25 | F | Bilateral | Present | 2011 | Not mentioned |
| Ploumidis A et al., [11] | 32 | F | Unilateral | Absent | 2013 | 7.6 cm |
AML occur as isolated sporadic entities and in association with TS [1]. They are typically large, multifocal, bilateral and occur in younger patients when associated with TS. In 70 to 80% of patients with AML without TS, a more pronounced female predominance is found and most patients present later in life, during fifth or sixth decade [5]. These findings are supported by the literature review shown in the [Table/Fig-6]. Benign and malignant renal tumours, renal infections, nephritis, vascular lesions like PAN, anatomical lesions like cysts and hydronephrosis, previously undiagnosed haematological conditions are the common causes of Wunderlich’s syndrome [12]. The commonest cause of renal haemorrhage is an AML [12]. Lesions greater than 4 cms, multicentric lesions and those associated with TS have increased risk of haemorrhage [1,7].
AML’s can exhibit areas of hypercellularity with atypia, posing specific diagnostic challenges. In such cases sarcomas including fibrosarcoma, leiomyosarcoma, liposarcoma, and sarcomatoid renal cell carcinoma need to be considered in the differential diagnosis depending on the predominant component present. Positive immunoreactivity for HMB-45 is characteristic of AML and positive in 100% of tumours, thus clinching the diagnosis [13].
Malignant transformation of AML, if it does occur is extremely rare. Two such cases were reported by Takahashi N et al., in the absence of association with TS. AML with many perivascular epitheloid cells should be classified as epitheloid AML. Malignant AML is considered to be a transformation of benign epitheloid AML. Diagnosis of malignancy can be made only on the basis of presence of metastases. On IHC, malignant AML are negative for epithelial markers (EMA, Keratin), but are positive for HMB-45 [14].
In general, asymptomatic AMLs with a diameter of 4 cm or smaller can be followed up. For larger and symptomatic tumours, surgical intervention should be considered [7]. Nephron sparing approach such as angio-embolisation or partial nephrectomy is preferable, especially in TS with bilateral, and multiple AML [15] as was done in the present case.
Conclusion
Renal AML are unusual lesions that behave in a benign fashion, however when associated with TS, can result in life threatening haemorrhage. So, an early diagnosis and timely treatment is important in these cases to prevent life threatening complications. Regular follow up of smaller lesions for progression and a thorough search for hamartomas in other sites, which are a part of tuberous sclerosis complex, is warranted. Patients and the relatives have to be educated about the pathology of the disease and to report immediately in case of appearance of sudden abdominal pain /haematuria.
[1]. Khan AS, Bakshi GD, Siddiqui AQ, Jaggi S, Thakare VA, Ellur S, Massive bilateral renal angiomyolipomatois in tuberous sclerosisBombay Hosp J 2003 45:477-80. [Google Scholar]
[2]. Gomez MR, Phenotype of tuberous sclerosis complex with a revision of diagnostic criteriaAnn N Y Acad Sci 1991 615:1-7. [Google Scholar]
[3]. Nasir K, Ahamad A, Giant renal angiomyolipoma and pulmonary lymphangiomyomatosisSaudi J Kidney Dis Transpl 2010 21(2):314-19. [Google Scholar]
[4]. Khallouk A, Ahallal Y, Doublali M, Tazi MF, Mellas S, Fassi MJE, Concurrent bilateral renal angiomyolipoma and renal cell carcinoma in a patient with tuberous sclerosis complexRev Urol 2009 11(4):216-18. [Google Scholar]
[5]. Mongha R, Bansal P, Dutta A, Das RK, Kundu AK, Wunderlich’s’s syndrome with hepatic angiomyolipoma in tuberous sclerosisIndian J Cancer 2008 45(2):64-66. [Google Scholar]
[6]. Nabi N, Shaikh AH, Khalid SE, Tuberous sclerosis with bilateral renal angiomyolipoma and Wunderlich’s’s syndromeJ Coll Physicians Surg Pak 2007 17(11):706-07. [Google Scholar]
[7]. Medda M, Picozzi SCM, Bozzini G, Carmignani L, Wunderlich’s’s syndrome and haemorrhagic shockJ Emerg Trauma Shock 2009 2(3):203-05. [Google Scholar]
[8]. Kushwaha R, Dhawan I, Arora R, Gupta K, Dhupia JS, Multifocal renal angiomyolipoma presenting as massive intraabdominal haemorrhageIndian J Pathol microbiol 2010 53(2):340-41. [Google Scholar]
[9]. Lin CY, Lin YH, Wu FZ, Pan HB, Wunderlich’s’s syndrome in spontaneous angiomyolipoma bleedingNDT Plus 2011 4:211-12. [Google Scholar]
[10]. Vaddi SP, Reddy VP, Devraj R, Wunderlich’s’s syndrome in a Tuberous sclerosis PatientIndian J surg 2011 73(3):227-29. [Google Scholar]
[11]. Ploumidis A, Katafigiotis I, Thanou M, Bodozoglou N, Athanasiou L, Ploumidis A, Spontaneous Retroperitoneal hemorrhage( Wunderlich syndrome) due to Large Upper Pole Renal Angiomyolipoma: Does Robotic- Assisted Laproscopic Partial Nephrectomy Have a role in Primary Treatment?Case Rep Urol 2013 2013:498694 [Google Scholar]
[12]. Albi G, Del Campo L, Taggaro D, Wunderlich’s’s syndrome: Causes, diagnosis and radiological managementClin Radiol 2002 57(9):840-45. [Google Scholar]
[13]. Kulkarni B, Desai SB, Dave B, Tongaonkar HB, Kulkarni JN, Chinoy RF, Renal angiomyolipomas-a study of 18 casesIndian J Pathol microbiol 2005 48(4):459-63. [Google Scholar]
[14]. Takahashi N, Kitahara R, Hishimoto Y, Ohguro A, Hashimoto Y, Suzuki T, Malignant transformation of renal angiomyolipomaInt J Urol 2003 10:271-73. [Google Scholar]
[15]. Cakan M, Demirel F, Yalcinkaya F, Altug U, Bilateral nephron-sparing surgery for giant bilateral renal angiomyolipomas associated with tuberous sclerosis complexJournal of Ankara University Faculty of Medicine 2006 59(2):83-85. [Google Scholar]