Gallbladder Cancer Presenting with Brain and Bone Metastasis: Case Report
Raghvendra Gupta1, Manish Singh2, Shilpi Karmakar3, Saurabh Karmakar4
1Lecturer, Department of Surgery, G.S.V.M. Medical College, Kanpur, India.
2Lecturer, Department of Surgery, G.S.V.M. Medical College, Kanpur, India.
3Junior Resident, Department of Surgery, G.S.V.M. Medical College, Kanpur, India.
4Assistant Professor, Department of Pulmonary Medicine, Era’s Lucknow Medical College, Lucknow, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Shilpi Karmakar, 117/H-2/189, Pandu Nagar, Kanpur, Uttar Pradesh-208005, India.
E-mail: doc_next_door@yahoo.com
Although gallbladder cancer is a rare disease worldwide, north India has one of the highest incidences of this disease. We report a case of asymptomatic gall bladder cancer with brain metastasis. The patient presented with a scalp lump as the sole presenting feature, with no symptoms attributable to abdominal malignancy. Previously, the lump had been incised by a local practitioner who had probably misdiagnosed it as an abscess.
Asymptomatic, Osteolytic lesion, Skull
Case Report
A 50-year-old woman presented to Department of General Surgery of G.S.V.M. Medical College with a painless scalp lump. She had noticed a small lump while combing her hair, three months back. It had progressively increased to its present size but was asymptomatic except for the cosmetic defect, so she ignored it. She had no history of trauma, abdominal pain, nausea, vomiting, anorexia, yellowish discolouration of eyes, headache or dizziness. She had no history of smoking, chewing tobacco or any other addictions. Her past history was not significant.
Her medical history, on perusal of records revealed that she had gone to an unqualified local practitioner, a day prior to attending our centre. He had suspected it to be an abscess and had incised the lump. The patient revealed that bleeding started, so the wound was dressed and she was referred to our Department immediately.
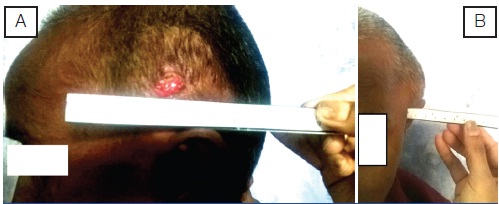
On examination, a well defined swelling was noted on the left temporal region. On inspection, the lump was measuring approximately 4cm x4 cm with a bulge of 2 cm in centre, with well defined margins and overlying skin was normal. A horizontal scar due to incision, and surrounding granulation tissue was present. On palpation, the lump was spherical in outline, had a normal surface temperature, and was non tender, firm, mobile over the underlying bone, with well defined margins [Table/Fig-1a&b]. Her hemogram revealed low haemoglobin of 7gm/dl and rest parameters were within normal limits. Her biochemical investigations and coagulation profile were within normal limits.
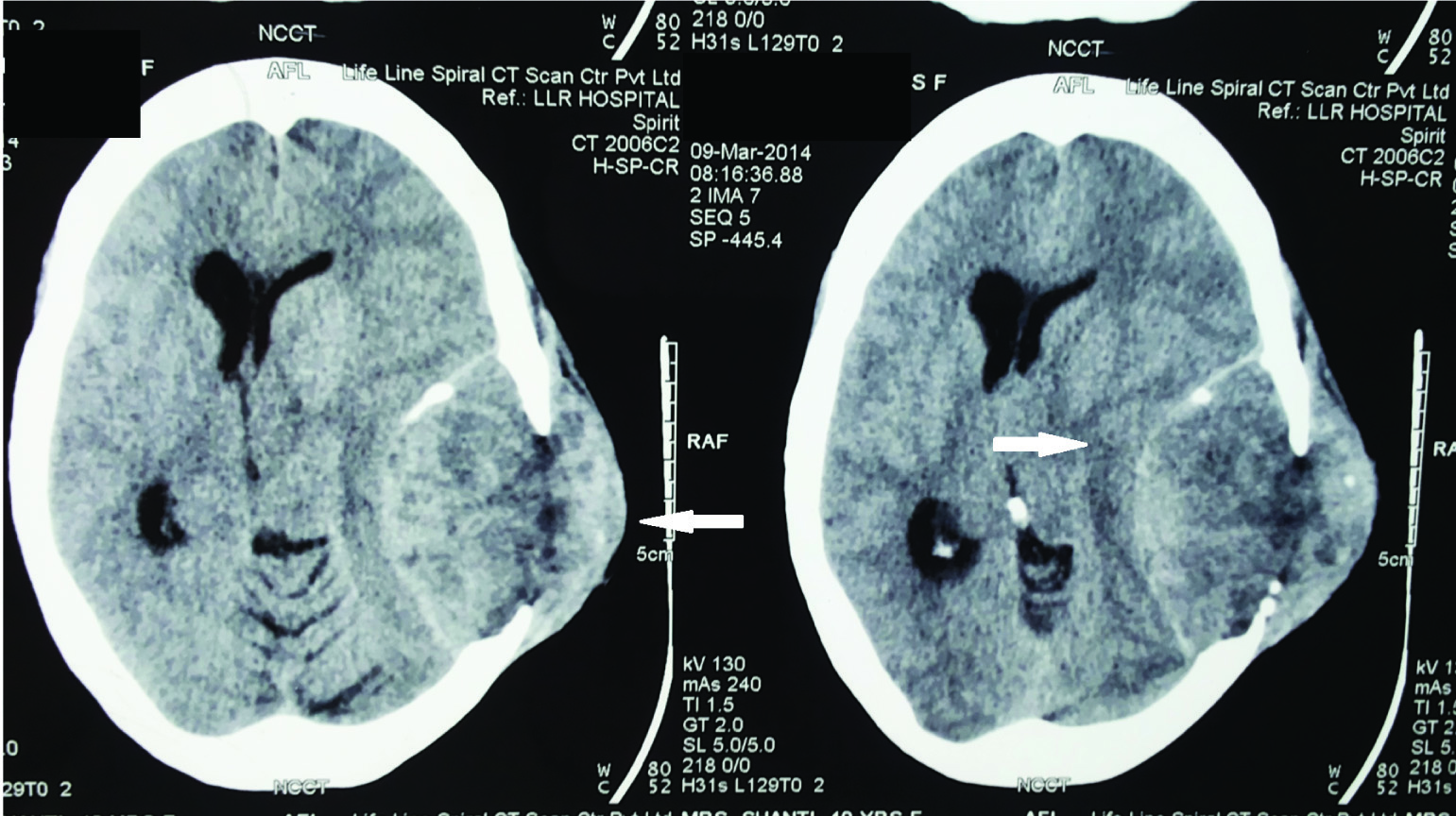
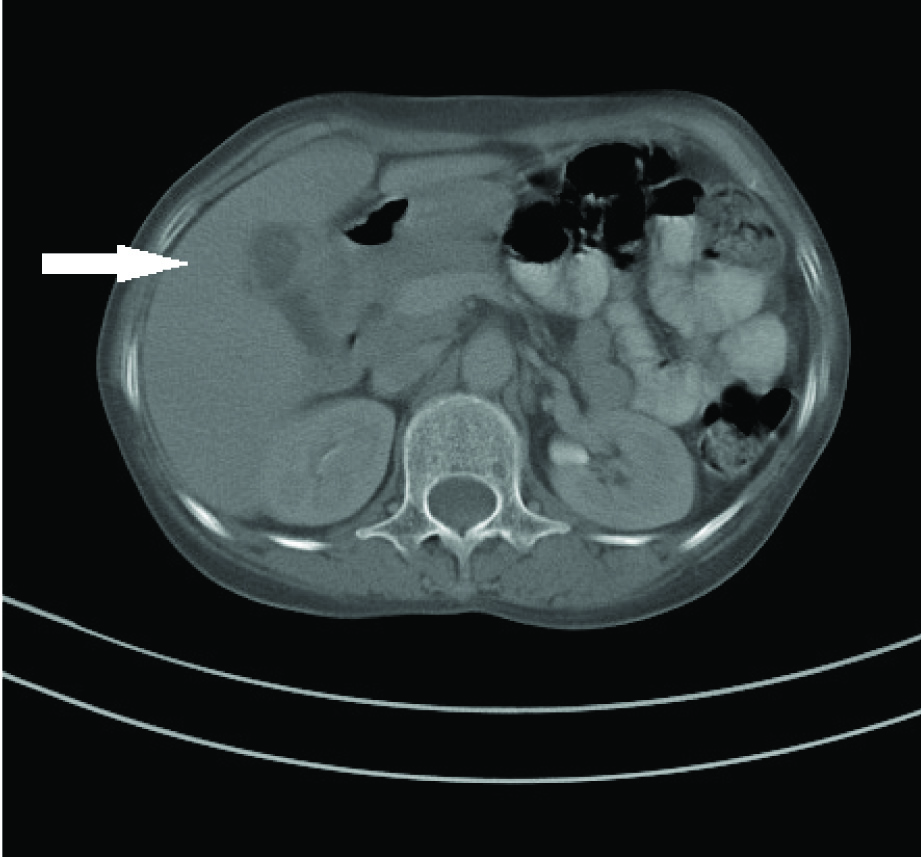
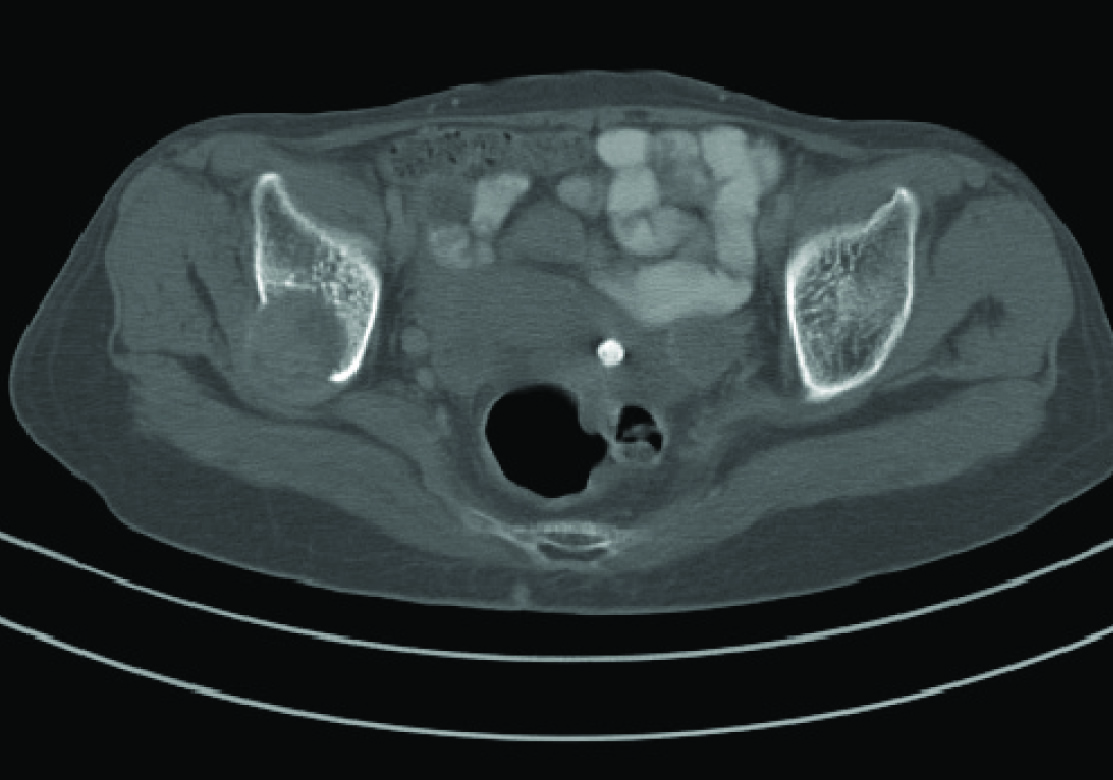
A Computed Tomogram (CT) of the head revealed a large mass lesion in temporo-parietal region eroding the skull and extending into the scalp [Table/Fig-2]. A Fine Needle Aspiration Cytology of the lump revealed clusters of atypical epithelial cells with pleomorphic nuclei and prominent nucleoli with the cells forming acini and ill defined papillae. The cytopathology was suggestive of metastatic Reportadenocarcinoma. A workup was done for the primary site of malignancy. Chest x ray PA view was normal. A helical CT of the abdomen revealed a gallbladder mass in the fundus [Table/Fig-3]. An osteolytic lesion was seen in the right iliac bone [Table/Fig-4]. There was no focal lesion in the liver and the portal tract and biliary tree was normal in appearance.
The serum carcinoembryonic antigen level was 4.93ng/ml .We diagnosed it as a case of gallbladder cancer TxNxM1 Stage IV B. We planned an Oncology referral and cholecystectomy but she didn’t turn up for admission and was lost to follow-up.
Discussion
Gallbladder cancer is a rare malignancy [1]. However, there is a high prevalence in regions of North India and among Asian Indian (native and migrants) ethnicity [2]. Early onset of gall stone in women and late presentation of patients for surgery has been implicated as cause of high prevalence of gallbladder cancer in north Indian population [1].
Gallbladder lacks a muscularis mucosa and submucosa and has a direct venous drainage through the liver parenchyma. Thus gallbladder cancer has a propensity for early metastasis and direct invasion into the liver and a tendency to seed the peritoneal cavity, biopsy tracts and laparoscopic-port sites [3]. One third of patients present with metastasis at the time of diagnosis and only 10%-30% of the patients have resectable tumours at presentation [4]. The median survival is less than 6 months after diagnosis.
Gallbladder cancer is asymptomatic, initially it might be detected incidentally on cholecystectomy specimen of patients presenting with cholelithiasis [5]. The diagnosis of gallbladder cancer is missed after cholecystectomy for gallstones in up to 7% patients [6]. In later stages, nonspecific symptoms like abdominal pain, weight loss, fever and jaundice maybe present. Invasion of biliary tract leads to jaundice. If tumour is located in the body or fundus of the gallbladder, then extension can occur into the liver or adjacent colon/small bowel can lead to local pain or bowel obstruction. Liver is the most common site of metastasis. Extraabdominal metastasis is rare and is to the lung followed by the brain [7].
Ultrasonography is used for screening; however it is unreliable for staging and for early lesions [8]. Helical computed tomography (CT) scan provides better imaging and reveals liver metastases and enlarged celiac, perihepatic and interaortocaval lymph nodes. On USG, CT or MRI the presence of a large gallbladder mass that nearly fills or replaces the lumen, is highly suggestive of gallbladder carcinoma [9]. Magnetic Resonance (MR) scan with MR cholangiography is sensitive for small hepatic metastases and common bile duct involvement. Endoscopic retrograde cholangiography or percutaneous cholangiog helps define resectability and provides palliative options [3].
Surgical resection is the mainstay of therapy. Palliation is done with percutaneous trans-hepatic biliary drainage (PTC) and endoscopic retrograde cholangiopancreatiography (ERCP). Chemotherapy and radiotherapy decrease the risk of locoregional failure. 5 FU is chemotherapeutic agent of choice and is given with adjuvant radiotherapy for locally advanced disease.
There are only five case reports of gallbladder cancer metastasis to the bones in the English Language literature [10]. Also, there’s only a single case report of gallbladder cancer metastasis to both brain and bones [10]. Our patient presented with a scalp lump [Table/Fig-1a&b], which on further workup revealed brain and bone metastasis [Table/Fig-2&4] of gallbladder cancer [Table/Fig-3]. In the previously described case, Win et al., used F18-FDG PET/CT scan for detection of metastasis of gallbladder cancer [10]. In our case, a Computed Tomography revealed the site of primary malignancy; which we believe is an adequate radiological modality for workup in developing country like ours. High index of suspicion leads to early detection and improves prognosis for aggressive malignancies, like gallbladder cancer. The purpose of presenting this case is not only to report a rare site of metastasis of gallbladder cancer but also to raise awareness among clinicians regarding this disease as a possible differential in diagnosis of scalp lumps.
A frontal and a lateral view of the scalp lump
Mass lesion in temporo-parietal region of the brain. The dura has been breached and the mass is eroding into the skull and scalp
CT Abdomen showing the mass replacing the gallbladder fundus and lumen
A soft tissue osteolytic lesion in the right iliac bone
Conclusion
Gallbladder cancer is potentially aggressive and rapidly invasive malignancy. Clinicians should be aware of the presentation and sites of metastasis of this malignancy. A high index of suspicion and early detection would lead to better prognosis and improve the outcome.
[1]. VK Kapoor, AJ McMichael, Gallbladder cancer: an ‘Indian’ diseaseNatl Med J India 2003 16:209-13. [Google Scholar]
[2]. RJ Mc Claine, SA Ahmad, AM Lowy, Surgical management of Gallbladder Cancer. In: Fuller CD, editors. Biliary Tract and Gallbladder Cancer: Diagnosis and Therapy 2009 1st EditionNYDemos Medical Publishing:16-17. [Google Scholar]
[3]. DL Bartlett, Y Fong, Gallbladder Cancer. In: Blumgart LH, Fong Y, Jarnagin WR,editors. American Cancer Society Atlas of Clinical Oncology Series 2001 1st EditionHamiltonBC Decker:213-24. [Google Scholar]
[4]. P Jeyaraj, TT Sio, MJ Lott, An unusual case of isolated, serial metastases of gallbladder carcinoma involving the chest wall, axilla, breast and lung parenchymaRare Tumors 2013 5:e7 [Google Scholar]
[5]. X de Aretxabala, I Roa, L Burgos, H Losada, JC Roa, J Mora, Gallbladder cancer: an analysis of a series of 139 patients with invasion restricted to the subserosal layerJ Gastrointest Surg 2006 10:186-92. [Google Scholar]
[6]. SS Saluja, M Gulati, PK Garg, H Pal, S Pal, P Sahni, Endoscopic or percutaneous biliary drainage for gallbladder cancer: a randomized trial and quality of life assessmentClin Gastroenterol Hepatol 2008 6(1):944-50. [Google Scholar]
[7]. S Singh, R Bhojwani, A Singh, A Bhatnagar, RK Saran, AK Agarwal, Skeletal metastasis in gall bladder cancerHPB 2007 9:71-72. [Google Scholar]
[8]. A Furlan, JV Ferris, K Hosseinzadeh, AA Borhani, Gallbladder carcinoma update: multimodality imaging evaluation, staging, and treatment optionsAJR Am J Roentgenol 2008 19:1440-47. [Google Scholar]
[9]. A Rodríguez-Fernández, M Gómez-Río, A Medina-Benítez, JV Moral, C Ramos-Font, JM Ramia-Ángel, Application of modern imaging methods in diagnosis of gallbladder cancerJ Surg Oncol 2006 93:650-64. [Google Scholar]
[10]. AZ Win, CM Aparici, Rare case of gallbladder cancer presenting with metastasis to bone and brain in an African American male discovered by F18-FDG PET/CTJournal of Biomedical Graphics and Computing 2013 3:24-29. [Google Scholar]