The lips are an important part of an individual’s persona contributing to aesthetics as well as having an important functional role. Various conditions like oncology excision, trauma, and congenital deformities are among the major aetiologies that result in lip deformities compromising the aesthetics as well as function, thus requiring lip reconstruction.
Reconstruction of the lip becomes an especially challenging task due to various anatomic factors. The lack of any substantial fibrous framework increases the risk of anatomic distortion through wound contraction and may lead to poor functional and aesthetic outcomes. The quality (i.e., color, texture, elasticity) of the skin and mucosa of the lips are difficult to match with distant flaps. Hence, local tissues provide the best results. There are various techniques for the lip reconstruction like Gillies fan flap, Karapandzic flap, Bilateral advancement flap, Bernard-Burow flap, Nasolabial flap, Perialarcrescentic advancement flap, Dieffenback method Depressor angulioris flap and free flap. Another technique that has been proven very useful for the reconstruction of lip defects is the use of Abbe-Estlander flap. The conventional Abbe-Estlander flap is composed of skin, muscle, and mucosa with the pedicle containing labial vessels. Hence, the present study was conducted to investigate the versatility of Abbe-estlander flap in lip reconstruction in 10 subjects and to present our experience with regard to aesthetic and functional outcomes.
Materials and Methods
This prospective study was conducted in the Department of Oral & Maxillofacial Surgery, Manipal College of Dental Sciences, Mangalore and KMC Attavar Hospital, Mangalore, Karnataka, India from Jan 2011 to June 2012. Institutional ethical committee approval was taken before conducting this study. Abbe-Estlander flap was used for lip reconstruction in 10 subjects who required lip reconstruction following excision of carcinoma of lip, following traumatic maxillofacial injuries causing lip defects or correction of congenital lip deformities.
Detailed history and clinical examination along with routine investigations (Haemoglobin, BT, CT, Urine analysis, Chest X-ray, ECG) were done and all patients were operated under general anesthesia. All the patients were on IV antibiotics in the immediate postoperative period. Patients were recalled at intervals of three weeks, three months and six months for follow up.
All patients reported with traumatic lip injuries or congenital lip deformities having lip defects of 1/3-1/2 of the lip requiring reconstruction were included in study. Patients having Lip defects less than 1/3 of the lip, and could have been managed by primary closure were excluded from the study. Subjects who were medically unfit for surgery or unwilling to undergo surgery were also not included in current study.
Technique
The partial-thickness Abbe-Estlander flaps in this series were taken from the middle of the lower lip to replace a portion of the upper lip or from the lateral portion of the upper lip to replace a portion of the lower lip. Lip height to the nose or to the labiomental fold was assessed at the preoperative visit so that postoperative lip height could be correlated to the pre-existing anatomy. The surgery generally involved the following considerations:
All flaps originating from the lower lip and moved to the upper lip were arterially based laterally on the same side as the upper-lip defect; all upper-lip flaps were arterially based medially.
Methylene blue vermilion/cutaneous tattoos were placed with a 25-guage needle under loupe magnification after regional anaesthetic block (infraorbital and mental nerves) to ensure perfect alignment of the vermilion-cutaneous borders.
For lower-lip defects, the size of the lip-switch flap was usually half the size of the excisional defect, thereby sharing the lip loss equally between the upper and lower lips.
The Estlander is a lip-switching flap that involves the commissure and pivots the upper lip to the lower lip.
Abbe flaps for upper-lip replacement have always made the full height of the upper lip regardless of the amount of skin being replaced; lower-lip replacement flaps were boxed (not triangular) and tailored at any level necessary.
To ensure viability and to trim the flap subcutaneously, all lip-switch flaps were mobilized under regional block before local anaesthetics with epinephrine was instilled into the adjacent tissues. Viability was constantly ensured during the operation by noting pink coloration and pinpoint bleeding at the distal flap edge after a light rub with a piece of gauze.
The flap was always cut through on the non pedicled side first to locate the position of the artery in relation to the muscle and the vermilion cutaneous border. Although the labial vessel is generally located on top of or just beneath the surface of the orbicularis oris muscle, thin lips or previously operated lips might have the vessel in a precarious position.
Only a cuff of muscle around the vessel was maintained, along with a mucosal pedicle of 1.25 to 1.50 cm. The remainder of the flap was skin and subcutaneous tissue only.
The vermilion was cut through on the pedicled side for 3 to 4 mm to line up the flap vermilion cutaneous border with the recipient vermilion cutaneous border.
A single central pexing suture held all flaps in place before routine closure. No maxillomandibular fixation was ever used.
The skin adjacent to the split Abbe flap was always undermined for a small distance to aid in closure and to provide counter traction, which prevents trapdoor bulking effects.
No drains were used.
All patients were placed on a clear liquid diet for one day, a pureed diet for two days, and then onwards normal diet. Tooth brushing was encouraged. Internal prostheses were always removed. In the office, 2.5 to 3 wk after the reconstruction, the pedicle was injected with 1 to 2 mL lidocaine with epinephrine 1: 2, 00,000. After 10 min, the flap was divided with a No. 10 blade and inset. Mucosal tissue was undermined for closure; however, no significant mucosal adjustments were made. Resorbable sutures were placed in the oral mucosa.
Results
A total number of 10 patients were taken up in the study, age ranging from 35-71 y, mean age being 60 [Table/Fig-1]. Out of 10 patients, 6 (60%) were male and 4 (40%) female [Table/Fig-1]. In all these patients, Abbe-Estlander flap that involved the commissure was used for reconstruction. Supraomohyoid neck dissection on ipsilateral side was done in six patients. In three patients with verrucous carcinoma, only wide excision was done. In the lip bite patient, only reconstruction was done. Abbe-Estlander flap was used in each of the 10 patients to reconstruct the various lip defects. Various sites of the lip defects are shown in [Table/Fig-2] that was reconstructed by using Abbe-Estlander flap. In all the cases single stage except one patient in which two stage, medially based Abbe-Estlander flap was used. The size of the lip-switch flap was usually half the size of the excisional defect. All the patients were evaluated for intra-operative complications like bleeding, difficulty to rotate the flap, difficulty in approximation of margins of flap, infection [Table/Fig-3] and postoperative complications like orocutaneous fistula, fullness or blunting of involved oral commissure, trap-door deformity [Table/Fig-4] before discharging from the hospital. All the patients were recalled at three week, three months and at six months interval to evaluate functional and aesthetic outcomes. All the patients reported for three week follow up only nine patients reported at the time of three months follow up and one patient expired within three months of postoperative due to metastasis to distant organs and six patients reported at the time of six months follow up. In one patient, difficulty to rotate flap (10%) was encountered intra-operatively. In postoperative period, one patient reported with orocutaneous fistula (10%) and one patient had fullness of involved oral commissure (10%) that resulted in permanent unaesthetic oral commissure. Orocutaneous fistula was closed immediately using V-Y closure technique. All the patients had adequate blood supply of flap (100%) [Table/Fig-5].
Distribution of the subjects according to mri pattern and asia grading at initial presentation
| Case no. | Age | Sex | Diagnosis | Treatment done | Complication |
|---|
| 1. | 54 | M | SCC of lower lip involving right commissure | Wide excision and reconstruction with abbe-estlander flap with ipsilateralsupraomohyoid neck dissection | none |
| 2. | 70 | M | SCC of lower lip involving left commissure | Wide excision and reconstruction with abbe-estlander flap with ipsilateralsupraomohyoid neck dissection | Expired within 3 month |
| 3. | 35 | F | Human Lip bite of right half of lower lip | Reconstruction with abbe-estlander flap | none |
| 4. | 58 | M | SCC of lower lip involving right commissure | Wide excision and reconstruction on right side with abbe-estlander with ipsilateralsupraomohyoid neck dissection | Second primary malignant lesion on left buccal mucosa which was reconstructed with nasolabial flap |
| 5. | 56 | F | SCC of lower lip involving right commissure | Wide excision and reconstruction with abbe-estlander flap with ipsilateralsupraomohyoid neck dissection | None |
| 6. | 64 | F | Verrucous carcinoma of lower lip involving right commisure | Wide excision and reconstruction with abbe-estlander flap | None |
| 7. | 65 | M | SCC of lower lip involving left commisure | Wide excision and reconstruction with abbe-estlander flap with ipsilateralsupraomohyoid neck dissection | Orocutaneous fistula |
| 8. | 71 | M | Verrucous carcinoma of lower lip involving left commissure | Wide excision and reconstruction with abbe-estlander flap | Hypertrophic scar |
| 9. | 67 | F | SCC of lower lip involving left commissure | Wide excision and reconstruction with abbe-estlander flap with ipsilateral supraomohyoid neck dissection | Fullness of oral commissure |
| 10. | 69 | M | Verrucous carcinoma of lower lip | Wide excision and reconstruction with abbe-estlander | None |
Different sites on lip of 10 subjects for lip reconstruction
| Site | No. of patients |
|---|
| Middle lower lip | 1 |
| Philtrum of upper lip | 0 |
| Lower lip Involving Right commissure | 4 |
| Lower lip Involving Left commissure | 5 |
| Upper lip involving right commissure | 0 |
| Upper lip involving left commissure | 0 |
| Total | 10 |
Intra operative complications
| Intra Operative Complications | No. | Percent (%) |
|---|
| None | 9 | 90 |
| Bleeding | 0 | 0 |
| Difficulty to rotate the flap | 1 | 10 |
| Difficulty in approximation of margins of flap Trap-door deformity | 0 | 0 |
| Total | 10 | 100 |
Intra Operative Complications
| Post-Operative Complications | No. | Percent (%) |
|---|
| None | 8 | 80 |
| Infection | 0 | 0 |
| Orocutaneous fistula | 1 | 10 |
| Fullness or blunting of involved oral commissure | 1 | 10 |
| Trap-door deformity | 0 | 0 |
| Total | 10 | 100 |
| Adequate Mouth Opening | Yes | 8 (80%) | 9 (100%) | 6 (100%) |
| No | 2 (20%) | 0 (0%) | 0 (0%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Adequate Blood Supply | | 3 weeks | 3 months | 6 months |
| Yes | 10( 100%) | 9 (100%) | 6 (100%) |
| No | 0 (0%) | 0 (0%) | 0 (0%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Adequate oral seal | Yes | 6 (60%) | 9 (100%) | 6 (100%) |
| No | 4 (40%) | 0 (0%) | 0 (0%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Symmetrical Mouth Opening | Yes | 7 (70%) | 8 (88.88%) | 6 (100%) |
| No | 3 (30%) | 1(11.11%) | 0 (0%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
Various clinical characteristics observed in postoperative period
| Symmetrical Lip Movements | Yes | 7 (70%) | 8 (88.88%) | 6 (100%) |
| No | 3 (30%) | 1(11.11%) | 0 (0% |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Speech Problem | Yes | 1(10%) | 0 (0%) | 0 (0%) |
| No | 9 (90%) | 9 (100%) | 6 (100%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Hypertrophic scar | Present | 0 (0%) | 1 (11.11%) | 1 (16.66%) |
| Absent | 10 (100%) | 8 (88.88%) | 5 (83.33%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
| Aesthetic Oral Commissure | Present | 6 (60%) | 8 (88.88%) | 6 (100%) |
| Absent | 4 (40%) | 1 (11.11%) | 0 (0%) |
| Total | 10 (100%) | 9 (100%) | 6 (100%) |
Two patients with inadequate mouth opening (20%), one of them expired within three months of postoperation and in one patient; second procedure (cheiloplasty) was performed [Table/Fig-5]. Four patients had inadequate oral seal (40%) [Table/Fig-5] and one patient had speech problem (10%) which resolved within a period of three months [Table/Fig-5]. Three patients had asymmetric mouth opening (30%) [Table/Fig-5], and asymmetric lip movement (30%) that resolved within a period of three months except one patient [Table/Fig-5]. One patient developed hypertrophic scar (11.11%) at the end of three month [Table/Fig-5] and 60% of patients had aesthetic oral commissure at the end of three week, 88.88% at the end of three months and 100% patients had aesthetic oral commissure at the end of six months period [Table/Fig-6].
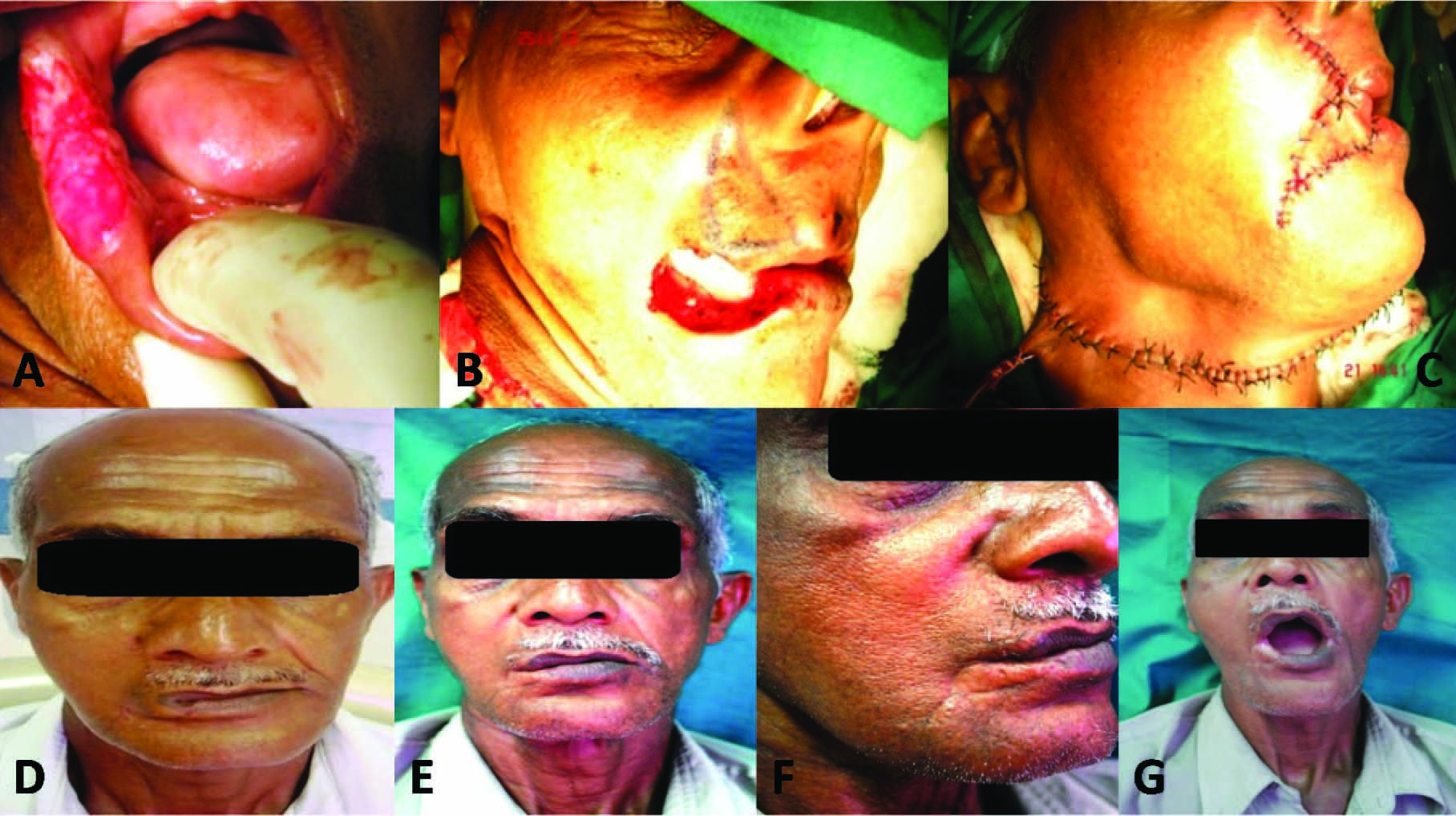
a) Pre operative photograph showing carcinoma of lip; b) surgical defect & flap marking; c) immediate post-operative photograph; d) 3 weeks follow up; e) 3 months follow up; f) 6 months follow up; g) mouth opening at the end of 6 months follow up
Discussion
Reconstruction of the lip for defects from oncological, congenital, post-traumatic, and, rarely, infectious processes has been described for more than 200 y [1,2]. Lip defects can be classified as partial defects that involve only skin or mucosa or they can be classified as full-thickness defects involving skin and muscle, with or without mucosal involvement [3–5]. Lip defects are also classified by location. Defects can be limited to the cutaneous lip or vermilion or involve the both. Upper lip defects can further be divided into those that involve the philtrum, medial lip, or lateral upper lip. Lower lip defects can also be divided into central or lateral, with or without commissural involvement. The size of the defects is also a helpful means of defining the lip defects. Four categories are commonly considered: one third or less of the lip, one third to two thirds of the lip, more than two thirds of the lip, and defects that result in total loss of one lip in combination with defects in the other lip.Microsurgical techniques have greatly enhanced our ability to restore large parcels of tissue in the head and neck, and the lips and perioral region are no exception. Microsurgical techniques are particularly valuable when local tissues are insufficient for adequate repair of large composite defects [4,5].
The best reconstructions use as much local tissue as possible until free tissue transfer is inevitable, at which point the free flap is joined with the local tissues in as much functional manner as possible. Although, variety of techniques have been proposed for the reconstruction of 1/3rd to 2/3rd sized lip defects, none is ideal. It is obvious from the observations made in our present study that Abbe-Estlander flap provides a reliable reconstructive flap. This is supported by the fact that none of our patient had dehiscence or necrosis of the flap. Flanagin[6] used a narrow full-thickness free graft from the lower lip to the upper lip for correction of a flat upper lip. Mild superficial necrosis occurred in all his cases. Multiple functional and aesthetic criteria were used to assess the versatility of Abbe-Estlander flap. The functional criteria were evaluation of mouth opening, presence or absence of lip competence, presence or absence of symmetrical lip movements and the presence or absence of normal speech. The key to optimal restoration of lip function is the reconstitution of the orbicularis oris muscle with its reinnervation [7,8]. The extensive review of literature implies that a two stage procedures is required for restoring adequate mouth opening, but the same was accomplished in our study with single stage alone. Only one patient required a second stage (cheiloplasty) to get adequate mouth opening and enhance oral commissural appearance. Rolda et al., [9] restored the mouth competence and symmetry with a single stage procedure. They did not encounter microstomia in any patient. In literature the major disadvantage of abbe-estlander flaps is microstomia [10].In this study, only one patient suffered from the same. None of patients had persistent speech problems and lip incompetence at three months postoperative. These findings are in consistent with the finding of Zhai et al., [7]. The aesthetic criteria were presence or absence of symmetrical mouth opening, presence or absence of hypertrophic scar and the presence or absence of an aesthetic oral commissure. The best way to achieve a good aesthetic outcome is to use identical or similar tissue for reconstruction of defects [7]. As the Abbe-Estlander flap imports identical tissue for reconstruction, it fulfils the requirements of a good aesthetic outcome. Our study also had good aesthetic results in terms of symmetrical mouth opening and oral competence. Although one patient had a hypertrophic scar but the overall results were satisfactory with regard to cosmetic appearance. Our result is in consistent with the study of Motamedi [11], Bennis and Vegter et al., [12]. This procedure was less mutilating, less stressful and well suited for elderly patients whose general health was not optimal [11]. This flap may represent an alternative to microvascular reconstruction for defects involving up to 1/3rd to 2/3rd of the lip. Because of its rich vascularity [13,14]. It is an ideal flap for the irradiated patient and those that have undergone neck dissection. Although, the major limiting factor is its size, it was successfully used for reconstructing 1/3rd to 2/3rd of lip defects in this study. Zide MF and Fuselier C [15], Yamauchi et al., [16] and Ali Ebrahimi et al., [17] also stated that Abbe flaps for lower-lip defects typically fill defects comprising 30% to 80% of the total lip width. The Abbe-estlander flap technique has several advantages over other techniques such as: 1) It is safe and a reliable flap with an excellent blood supply that affords versatility in flap design even after bilateral neck dissection. 2) Simple to perform, and provides functionally and aesthetically pleasing result for reconstruction of 1/3rd to 2/3rd sized lip defects. 3) Safer and less mutilating for elderly patients with multiple morbidities, who represent a poorer operative risk. 4) Change of appearance is very minimal and very acceptable for the patients. 5) Improves functional results in terms of speech and symmetrical lip movements [10,14,16].
Conclusion
Even though maxillofacial reconstructive surgery has undergone a sea change from the use of traditional flaps to the present day microsurgical free tissue transfer, Abbe-Estlander still holds in a position as a reliable method of lip reconstruction. Our experience with 10 patients with Abbe-Estlander flap reconstruction has been encouraging and the result obtained was extremely satisfactory.