Isoniazid Induced Cutaneous Leukocytoclastic Vasculitis in Extra Pulmonary Tuberculosis (Pott’s Spine): A Case Report
Sowmya Bondalapati1, Dharma Rao V2, Dilip Rampure3, Rama Rao S4
1Post Graduate, Department of General Medicine,Mamata Medical College,Khammam, Andhra Pradesh, India.
2Professor, Department of General Medicine,Mamata Medical College,Khammam, Andhra Pradesh, India.
3Professor and Head, Department of General Medicine,Mamata Medical College,Khammam, Andhra Pradesh, India.
4Professor, Department of General Medicine,Mamata Medical College,Khammam, Andhra Pradesh, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Sowmya Bondalapati, C/o Pokuri Ramarao, Flat no 101, Sri Nilaya Estates, Ameerpet, Hyderabad, India. Phone : +917893434333, E-mail : kishpokuri@yahoo.com
Anti-tuberculosis drugs frequently result in cutaneous adverse reactions but Isoniazid is known to have least toxic potential for cutaneous reactions. We report a rare case of Isoniazid induced cutaneous leucocytoclastic vasculitis. A 64-year-old male was diagnosed to have Pott’s spine with multiple vertebral body involvement (D8-12 vertebrae). Subsequently, he was treated with first line anti-TB drugs i.e., Isoniazid, Rifampicin, Pyrazinamide and Ethambutol. On the fourth day of treatment with Anti Tuberculosis Treatment (ATT), the patient developed an erythematosus rash over right upper limb not associated with itching or pain, non-blanchable macules and papules over bilateral shins on lower limbs, petechiae on both forearms and hyper pigmented, scaly rash over right axilla and buttocks. The skin biopsy report was consistent with cutaneous leukocytoclastic vasculitis. Although rare, Isoniazid among anti-tuberculosis drugs should be considered as potential cause of drug-induced cutaneous leukocytoclastic vasculitis in the differential diagnosis of erythematosus rash with petechiae.
Anti tuberculosis drugs, Isoniazid, Leucocytoclastic vasculitis, Pott’s spine
Case Report
A 64-year-old male patient was admitted to the tertiary care hospital with complaints of low grade fever with evening rise of temperature, low back ache since three months; pain and swelling in bilateral ankle and knee joints since two months. Low back ache was mechanical and progressive in nature, exacerbated on carrying weights. Pain and swelling in bilateral ankle and knee joints; initially started in left knee followed by right knee and then progressed to both ankle joints and the patient was unable to carry out daily self care activities without support. The patient had significant weight loss in the past six months. He was diagnosed with pulmonary Koch’s 15 y back and was treated with ATT drugs as per DOTS (Directly Observed Treatment Strategy) regimen under RNTCP (Revised National Tuberculosis Control Programme). The lab values and Radiological findings were shown in [Table/Fig-1].
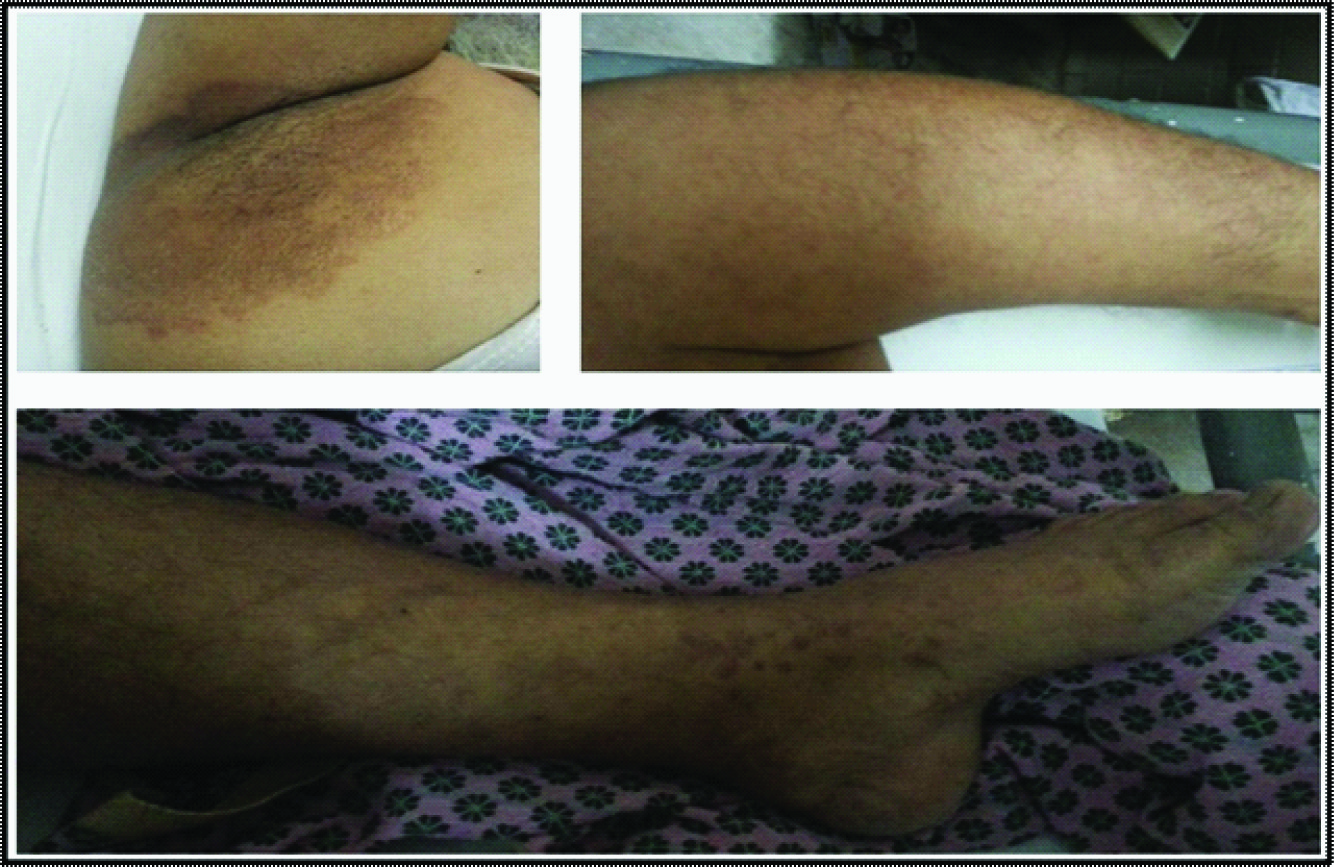
Once the diagnosis of Pott’s spine was under suspicion, the patient was put on empirical Anti Tuberculosis Treatment (ATT) for a therapeutic trial. Anti-tuberculosis therapy with Isoniazid 300mg, Rifampicin 600mg, Pyrazinamide 1500mg and Ethambutol 800mg once daily was initiated. Post treatment on day four, the patient developed rash over right upper limb not associated with itching or pain, palpable purpura over bilateral shins on lower limbs, non blanchable macules, papules and petechiae over both the forearms and hyper pigmented, scaly rash over axilla and buttocks [Table/Fig-2]. A skin biopsy from a purpuric lesion over his shin showed perivascular and interstitial infiltration of neutrophils with extravasation of erythrocytes and fibrin deposition which is characteristic of leukocytoclastic vasculitis.
All anti-tuberculosis drugs were stopped after the development of rash due to a clinical suspicion of drug-induced adverse cutaneous reaction. Patient was then immediately treated with an oral antihistamine and topical corticosteroids. There was progressive improvement of the vasculitis lesions and the rash resolved within one week leaving post-inflammatory hyper pigmentation on axilla and lower limbs. Later, we performed rechallenge with low doses of each anti-tuberculosis drug after nine days of resolution of rash, Sectionas depicted in [Table/Fig-3]. No cutaneous adverse reactions were observed after rifampin (300 mg), ethambutol (400 mg) and pyrazinamide (750 mg). However, after rechallenge with low dose isoniazid (100 mg), new purpuric lesions reappeared on right axilla, both forearms and lower limbs. This time the skin lesion resolved after three days of treatment with oral antihistamine and topical corticosteroids. Consequently, he was treated with other first line anti-tuberculosis agents (excluding isoniazid) at regular doses for Pott’s spine and NSAIDs like naproxen 500mg twice daily and celecoxib 100mg once daily for joint pains without recurrence of the skin rash during his stay in the hospital.
Lab values and radiological findings of the patient
| Hemoglobin 10.8g/dL | Urine analysis results showed no evidence of proteinuria or hematuria. |
| Total WBC count 11800 cells/mm3 (Differential count revealed neutrophils 78%, lymphocytes 18%, monocytes 2%, eosinophils 1% and basophils 1%) | Rheumatoid factor, ANA and ANCA test results were negative. |
| Platelet count 2.2 lakhs cells/mm3 | HBsAg, anti HCV and anti-HIV test results were also negative. |
| Renal Parameters: Blood Urea Nitrogen 44mg/dl Serum creatinine 1.1mg/dL | Abdominal ultrasound revealed grade II fatty liver and mild hepatosplenomegaly |
| Liver Function Tests: Total bilirubin 1.4 mg/dL Direct bilirubin 1.1mg/dL AST: 47 U/L ALT: 44U/L Alkaline phosphatise: 186 U/L γ-glutamyl transferase: 86 U/L Albumin: 2g/dl | CT Lumbar spine has shown spondylosis with mild anterolisthesis @ L5-S1 and ill-defined lytic destruction of D11 Vertebral body with mild adjacent paravertebral soft tissue thickening suggestive of abscess |
| Serum ADA levels were 12 IU/L | Bone scan revealed involvement of D8-12 vertebrae with an abscess consistent with tuberculosis of spine. |
| Sputum AFB staining and Mycobacterium tuberculosis cultures using Lowenstein Jensen media were negative. | CECT Abdomen reveals lytic lesions in D7, 8, 9 and 12 levels and a collection at D9 level suggestive of Pott’s spine. |
| The serum levels of IgG, IgA, IgM, and complement levels C3 and C4 were within normal limits | MRI Dorsolumbar spine shows evidence of multiple vertebral body involvement without spinal cord compression. |
Leucocytoclastic vasculitis over axilla, forearm and lower limb
Response to rechallenge with anti-tuberculosis drugs
| ATT Medication | Dosage and dosing schedule | Cutaneous manifestations |
| Isoniazid (H) | 100 mg once daily | Vasculitis rash reappeared |
| Rifampicin (R) | 300 mg once daily | None |
| Pyrazinamide (Z) | 750 mg once daily | None |
| Ethambutol (E) | 400 mg once daily | None |
Discussion
Leukocytoclastic vasculitis (LCV), also known as hypersensitivity vasculitis and hypersensitivity angiitis, is a histopathologic term commonly used to denote a small-vessel vasculitis [1]. According to Chapel Hill Consensus Conference system classification [1]cutaneous leukocytoclastic vasculitis is classified as small vessel vasculitis. Histologically, the characteristic lesion is an angiocentric inflammatory process associated with leukocytoclasia (neutrophil fragmentation) and fibrinoid necrosis. The pathophysiological mechanism involved is the deposition of immune complexes, usually immunoglobulin M and G that activate the complement pathways, leading to the production of chemotactic factors and the expression of adhesion molecules [2]. Although, immune complexes are involved in the pathogenesis of leukocytoclastic vasculitis, other autoantibodies such as antineutrophil cytoplasmic antibody (ANCA), other inflammatory mediators, and local factors that involve the endothelial cells and adhesion molecules play an important role [2]. However, the exact mechanisms remain unknown. In cases of cutaneous leukocytoclastic vasculitis, Mycobacterium tuberculosis is not found in the vessel wall, which differentiates it from cutaneous tuberculosis, in which microorganisms are seen in biopsy samples. The mechanism of injury proposed for this type of vasculitis is deposition of immune complexes in the vascular wall rather than direct aggression of the tubercle bacillus [2].
Between one third and one half of the cases of cutaneous vasculitis are idiopathic, and the most common drugs that can cause cutaneous vasculitis are antibiotics, particularly beta-lactam drugs, NSAIDs, and diuretics [3]. The most common manifestation of cutaneous vasculitis is palpable purpura on the legs. Urticarial lesions may develop in some patients with LCV; in rare cases, this type of lesion predates the purpuric lesions. The urticarial lesions are of a different character than typical urticaria [3]. We report an unusual clinical presentation of LCV following treatment with anti-tuberculosis drugs in a Pott’s spine patient.
Cutaneous leukocytoclastic vasculitis is a rare complication of antituberculosis medication. Cutaneous adverse drug reactions (CADR) to anti-tuberculosis drugs ranges from urticaria, pustules, pruritus, maculopapular exanthems, morbiliform rash, fixed drug eruptions, erythema nodosum and erythematosus rash like erythema multiforme – minor and major, Steven Johnson’s syndrome and toxic epidermal necrolysis. These cutaneous adverse drug reactions have been reported in up to 5.7% of patients treated with ATT [4].
Three main forms of this combination of pulmonary tuberculosis and vasculitis are present [5-7].
Pulmonary tuberculosis/cutaneous leukocytoclastic vasculitis;
Pulmonary tuberculosis/Henoch-Schönlein purpura; and
Pulmonary tuberculosis/vasculitis secondary to ATT
However, our present case does not fit in either of these forms as this is a case of extra pulmonary TB (pott’s spine) and cutaneous LCV secondary to ATT (isoniazid).
In contrast to tuberculosis related vasculitis, the skin lesions of ATT-induced vasculitis typically improve upon withdrawal of the suspected medication and can be controlled with the administration of antihistamines and corticosteroids [6]. Similarly, our patient had a cutaneous adverse reaction that improved when the causative drug was withdrawn and recurred after rechallenge i.e., with isoniazid. Moreover, there was no cause of the vasculitis except isoniazid, and the pathological findings were compatible with leukocytoclastic vasculitis, although the pathogenic mechanism remains unclear. Risk factors for severe ATT induced CADRs include Asian origin, older age, female gender, diabetes mellitus, previous anti-tuberculosis therapy, history of hepatitis, concomitant hepatotoxic drugs and positive HIV test [8]. Our patient had three risk factors: he was Asian, age > 60 y and had received ATT previously 15 y back.
Causality assessment using Naranjo scale to determine the relationship between isoniazid and leucocytoclastic vasculitis in the present case was “DEFINITE CAUSALITY” (Score of 10 on Naranjo ADR probability scale) [9]. Whereas, causality assessment using WHO UMC scale (World Health Organisation- Uppsala Monitoring Center) revealed that the association of isoniazid and the incidence of LCV in this case was “CERTAIN”. Several studies revealed the causal relationship between the first line anti TB drugs and the skin lesions and their onset but no specific mechanism was documented [10].
Conclusion
With this case report, we aim to create awareness and vigilance about rare, but potentially serious drug reaction like cutaneous leukocytoclastic vasculitis that can occur with isoniazid in a patient with Pott’s spine. Therefore, timely diagnosis of cutaneous ADR and necessary remedial actions may decrease the incidence and morbidity. Further studies are needed to elucidate the specific mechanism of the combination of extra pulmonary tuberculosis (pott’s spine) and cutaneous leukocytoclastic vasculitis with isoniazid.
Acknowledgements
The authors thank the Department of Pathology for reporting the skin biopsy and Department of Radiology for reporting CT and MRI spine. Last but not the least; we thank our patient, who allowed us to publish this case.
[1]. JC Jennette, RJ Falk, Small-vessel vasculitisN Engl J Med 1997 337(21):1512-23. [Google Scholar]
[2]. NM Johnson, MW McNicol, EJ Burton-Kee, JF Mowbray, Circulating immune complexes in tuberculosisThorax. 1981 36(8):610-17. [Google Scholar]
[3]. MC Sneller, CA Langford, AS Fauci, The Vasculitis Syndromes. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, editors. Harrison’s Principles of Internal Medicine. 2005 16th EditionNew YorkMcGraw-Hill:2002-04. [Google Scholar]
[4]. WC Tan, CK Ong, SC Kang, MA Razak, Two years review of cutaneous adverse drug reaction from first line anti-tuberculous drugsMed J Malaysia 2007 62:143-46. [Google Scholar]
[5]. M Carvalho, RL Dominoni, D Senchechen, AF Fernandes, IP Burigo, E Doubrawa, Cutaneous leukocytoclastic vasculitis accompanied by pulmonary tuberculosisJ Bras Pneumol 2008 34:745-48. [Google Scholar]
[6]. CH Chan, YW Chong, AJ Sun, GB Hoheisel, Cutaneous vasculitis associated with tuberculosis and its treatment.Tubercle. 1990 71:297-300. [Google Scholar]
[7]. J Barbagallo, P Tager, R Ingleton, RJ Hirsch, JM Weinberg, Cutaneous tuberculosis: diagnosis and treatment.Am J Clin Dermatol 2002 3:319-28. [Google Scholar]
[8]. T Schaberg, K Rebhan, H Lode, Risk factors for side-effects of isoniazid, rifampin and pyrazinamide in patients hospitalized for pulmonary tuberculosisEur Respir J 1996 9:2026-30. [Google Scholar]
[9]. CA Naranjo, U Busto, EM Sellers, P Sandor, I Ruiz, EA Roberts, A method for estimating the probability of adverse drug reactionsClin Pharmacol Ther 1981 30:239-45. [Google Scholar]
[10]. JH Kim, JI Moon, JE Kim, GS Choi, HS Park, Cutaneous leukocytoclastic vasculitis due to anti-tuberculosis medications, rifampin and pyrazinamidAllergy Asthma Immunol Res 2010 2:55-58. [Google Scholar]