Anaesthetic Management of a Patient with Dilated Cardiomyopathy for Fracture Femur Surgery-A Case Report
Koramutla Pradeep Kumar1, Gudaru Jagadesh2
1Assistant Professor, Department of Anesthesiology, Balaji Institute of Surgery Research and Rehabilitation for Disabled,, Tirupati, Andhra Pradesh, India.
2Professor and Head, Department of Orthopaedics, and Director,Balaji Institute of Surgery Research and Rehabilitation for Disabled, Tirupati, Andhra Pradesh, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Koramutla Pradeep Kumar, Assistant Professor, Department of Anesthesiology, Birrd (T), Tirupati-517507, Andhra Pradesh, India.
Phone: +919440012363,
E-mail:drpradeep9@gmail.com
Dilated cardiomyopathy (DCM) is defined as impairment of the ventricular function of the myocardium. The management of a patient with dilated cardiomyopathy, who undergoes a non-cardiac surgery, is always a challenge for an anaesthesiologist, as this situation is associated with a high mortality rate. We are reporting the successful anaesthetic management of a patient with severe dilated cardiomyopathy for fractured femur surgical repair under graded epidural anaesthesia.
Epidural anaesthesia, DCM
Case Report
A 75-year-old patient who presented with a fractured femur neck was posted for surgery. His previous medical records revealed that he was a known case of dilated cardioyopathy and chronic kidney disease, stage III. He was hospitalized and he had received treatment for the same problem, 6 months back. After admission, the patient was subjected to the required investigations and his laboratory reports revealed; random blood glucose of 148 mg/dL, urea- 84mg/dL, serum creatinine 3.0 mg/dL, serum sodium 127mmol/L, serum potassium 5.8 mmol/L, and Hb 8.0 gm/dL. Heart rate was 37/min and it was regular. Systolic and diastolic blood pressures were 170 mmHg and 60 mmHg respectively. His respiratory rate was 18/min. SOB was class 2. On auscultation, normal vesicular breaths and no added sounds were heard. The pre-operative ECG showed supraventricular bradycardia, abnormal left axis deviation, left ventricular hypertrophy with repolarization abnormality and a complete heart block. Echocardiography reports revealed; global hypokinaesia, severe LV systolic dysfunction, ejection fraction of 20%, Grade 1 diastolic dysfunction, mild mitral regurgitation, tricuspid regurgitation and pulmonary arterial hypertension. Left atrium was 33mm, left ventricle was 65/60, IVSD was 11/11, PWD was 8/12, RV =200mm, MV=2+mr, AOV= 1+AR, AJV=180cm/sec. 2+ TR RVSP =40+RAP, PJV were normal. All valves were normal. He was on treatment with telmisartan 40mg and lasilactone. His chest X-ray revealed enlarged cardiac borders [Table/Fig-1]. Cardiologist advised biventricular pacing, but the patient was not willing to undergo the same pre-operatively. However, the procedure was planned at the time of surgery, after taking a high risk consent. Regional anaesthesia was planned, it was particularly Graded as epidural and the reason for selection was explained to the patient, which is a routine practice in our institute. Epidural anaesthesia was chosen as it produces changes in the preload and afterload, that mimic pharmacological goals in the treatment of this disease [1] . Epidural anaesthesia also produces minimal effects on the heart rate, and contractility. Blood volume was maintained with colloids at 1.0ml/kg/hr. Intraoperatively, there were no haemodynamic changes [Table/Fig-2]. Invasive monitoring was done by assessing intraarterial blood pressure, arterial oxygen saturation (sPo2) 5 lead ECG monitoring. CVP line was placed for assessing the volume status. Pre-operatively, anaemia was corrected by transfusing packed cells. Under aseptic preparations, epidural space was identified at L3-L4 by using loss of resistance technique and an 18 G epidural catheter was advanced and it was fixed at 9 cm. 2% lignocaine and 0.5% bupivacaine were given alternately (3 ml), to attain a sensory level of upto T10. Total dose which was required was 10ml. After 10 minutes, the patient was positioned for surgery in supine position, on a surgical table. Intra operatively, epidural infusion of bupivacaine 0.5% was started, at a rate of 5ml/hr. Inotropes (dobutamine, dopamine) were used. A vasopressor, phenylephrine, was kept ready, but it was not used, as there was no drop in blood pressure. Intraoperatively, blood loss was assessed by collection of blood in suction bottle and the soaked gauze pieces and same was corrected by transfusion with packed cells. The total duration of the surgery was approximately 90 min. No significant changes were observed in blood pressure and heart rate. Post-operatively, blood pressure was maintained, there were no complaint of chest pain, sweating or dyspnoea. Post-operative complications were not remarkably noticed, and the patient was discharged. The patient was advised regular OPD follow ups, which were well taken care of accordingly.
Discussion
Anaesthetic management of patients with cardiomyopathy, with reduced systolic function, is challenging and it may be associated with high mortality [2] . Dilated cardiomyopathy (DCM) is defined as a deterioration of the function of the myocardium, either caused by left ventricular or biventricular dilatation or due to impaired systolic function of one or both ventricles, with impaired ventricular contractility [3] . These patients are often at a risk of dysrhythmias or sudden cardiac death[4] . The anaesthesiologist should have a thorough knowledge on its pathophysiology, clinical features, diagnostic evaluations and the treatment modalities. This has to be followed by a careful planning, for the provision of safe anaesthesia. Several types of treatment given for dilated cardiomyopathy aim at improving systolic function. The patient should be initially managed medically. The key haemodynamic features of DCM are elevated filling pressures, failure of myocardial contractile strength, and a marked inverse relationship between afterload and stroke volume [5] . Biventricular pacing, cardioplasty or cardiac transplant may be required to improve cardiac function [4]. Anaesthetic management needs to be customized for those with LVEF which is below 45%. A pre-operative hydration may not be desirable, as it may lead to congestive heart failure. Fluid management is critical. Choice of anaesthesia should be planned and it should be aimed at having only minimal haemodynamic fluctuations. Regional anaesthesia, particularly, a Graded epidural can be planned, in order to avoid fluctuations in blood pressures, as most of these patients tend to be dehydrated, because of the use of diuretic drugs. This further causes hypotension. However, this dehydration is generally beneficial for these patients, as it improves limited cardiac function. Anaesthetic drugs, with their vasodilator properties, can become hypotensive. Yamaguchi et al., reported a case of total prostectomy which was done under continuous epidural anaesthesia and total intravenous venous anaesthesia (TIVA) by using ketamine and propofol in a patient of DCM [4] . Cases of fracture neck femur which was done under plain epidural have not been reported. Biventricular pacing devices are often used in patients with cardiomyopathies, to improve systolic function. An interventricular conduction defect with a wide QRS complex is indicative of a asynchrony of the two ventricles [Table/Fig-2] . In our case, biventricular asynchrony was seen. Biventricular pacing (BVP) is beneficial for such patients with severe cardiomyopathy, in those with moderate to severe congestive heart failure with an EF of < 30% and in ventricular asynchrony. Use of vasoactive or inotropic drugs may be required frequently, to counteract the negative effects of the anaesthetics on cardiac function, and in this case, these drugs were also required to prevent haemodynamic changes. Our case was distinct from other cases, in that epidural anaesthesia was safely provided, while general anaesthesia is used by others [6,7] . There were no changes in heart rate and blood pressure and ventricular pacing was not required in the perioperative period. This showed that epidural anaesthesia had only a minimal effect on heart rate and contractility and that in patients with global hypokinaesia and complete heart block, regional anaesthesia could be safely given.
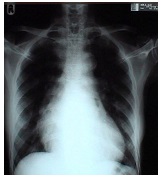
Chest X-ray showing enlarged cardiac borders
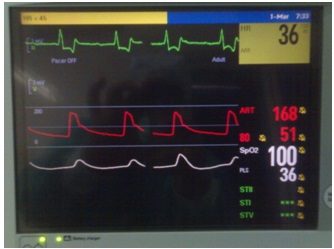
Snapshot of intraoperative monitoring
Conclusion
The management of a patient with dilated cardiomyopathy, who undergoes a noncardiac surgery, is always a challenge for the anaesthesiologist, as it is associated with high mortality. Patients with dilated cardiomyopathy can be effectively managed under regional anaesthesia. Anaesthesia planning, pre-operative assessment, optimizing cardiac status, post-operative monitoring are vital parameters which have to be considered for reducing the mortality. It is essential that anesthesiologists must understand the underlying pathophysiology, for a better management of these patients, as they may present at any time for anaesthesia.
[1]. RK Stoelting, SF Dierdorf, Cardiomyopathy. In: Stoelting RK (Ed). Anaesthesia and Coexisting Disease 1993 23rd EditionNew YorkChurchill Livingstone:97-102. [Google Scholar]
[2]. WG Dec, V Fuster, Review Article- Idiopathic dilated Cardiomyopathy. N Engl J Med. 1994 Dec 8 331(23):1564-75. [Google Scholar]
[3]. Report of the WHO/ISFC task force on the definition and classification of cardiomyopathies. Br Heart J. 1980 44:672-3. [Google Scholar]
[4]. S Yamaguchi, K Wake, M Mishio, Y Okuda, T Kitajima, [Anesthetic management of a patient with dilated cardiomyopathy under total intravenous venous anaesthesia with propofol and ketamine combined with continuous epidural analgesia]Masui. 1999 48:1232-4. [Google Scholar]
[5]. I Nicoletti, R Tomei, G Zanotto, E Dalla Vecchia, E Zorzi, C Vassanelli, The beneficial effect of biventricular pacing on ventricular tachycardia in a patient with non-ischemic cardiomyopathy.Int J Cardiol. 2008 126(2):29-31. [Google Scholar]
[6]. H Kaur, R Khetarpal, S Aggarwal, Dilated cardiomyopathy: an anaesthetic challenge.J Clin Diagn Res. 2013 7(6):1174-6. [Google Scholar]
[7]. T Nakamura, K Ikeshita, M Shimizu, W Miyake, Y Ikeda, A Asada, [Anesthetic management for mitral valve replacement in a patient with mitral stenosis and dilated cardiomyopathy]Masui. 2011 60(2):220-3. [Google Scholar]