Alveolar Bone Expansion for Implant Placement in Compromised Aesthetic Zone – Case Series
Jumshad B Mohamed1, Md Nazish Alam2, Gurudeep Singh3, S.N Chandrasekaran4
1Assistant Professor, Department of Periodontics and Implant Dentistry,Sree Balaji Dental College & Hospital, Chennai, Tamil Nadu, India.
2Senior Lecturer, Department of Periodontics and Implant Dentistry,Sree Balaji Dental College & Hospital, Chennai, Tamil Nadu, India.
3Professor, Department of Periodontics and Implant Dentistry,Sree Balaji Dental College & Hospital, Chennai, Tamil Nadu, India.
4Professor & HOD, Department of Periodontics and Implant Dentistry,Sree Balaji Dental College & Hospital, Chennai, Tamil Nadu, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Jumshad B. Mohamed, Assistant Professor, Department of Periodontics & Implant Dentistry, Sree Balaji Dental College & Hospital, Chennai - 600100 Tamil Nadu, India.
Phone: +919884325366,
E-mail:Jumshad77@gmail.com
Implant placement and restoration of compromised alveolar ridges in the aesthetic zone has always been a challenge to the oral implantologists. The use of bone expanders and bone condensers without the use of traditional drilling sequences in this scenario is becoming popular because of its predictable results. Xenograft along with Platelet-rich fibrin (PRF) used as scaffold also provides growth factors to accelerate both soft and hard tissue healing as well as regeneration. The paper highlights this combined approach in the placement of implants in compromised alveolar ridges with good results. All implants were successfully restored and followed up for one year.
Osteotomes, Platelet-Rich Fibrin, Dental Implants
Case Report
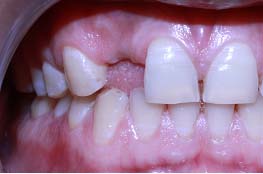
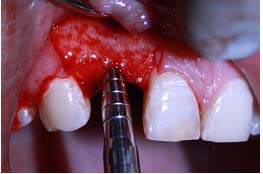
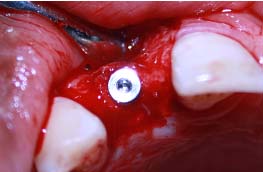
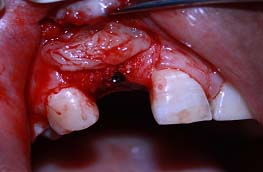
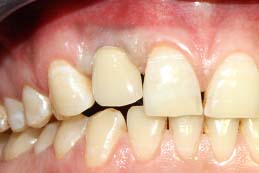
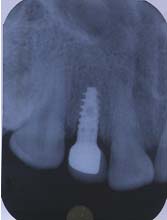
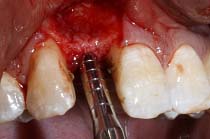
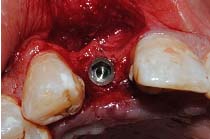
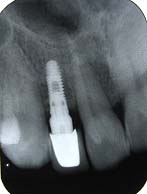
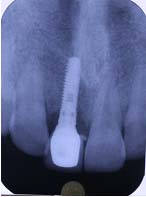
Case 1: A 24-year-old male patient presented to the Department Of Periodontics and Implant Dentistry for management of partially edentulous area in the maxillary anterior region in relation to tooth no.12 [Table/Fig-1a]. After clinical and radiographic evaluation the patient was given the option of dental implant versus crown and bridge, the patient opted for the former. After induction of local anaesthesia, a paracrestal incision was given using Bard Parker scalpel #15 and a full thickness flap was elevated. Due to deficient bone, osteotomy was initiated using a sharp pilot D-shaped expander followed by condensation of the osteotomy site using bone condensers [Table/Fig-1b]. Following the osteotomy dental implant$ of size 3.5x 11.5 mm was placed [Table/Fig-1c] achieving primary stability. On the facial aspect xenograft* and PRF [Table/Fig-1d] was placed for augmentation of deficient region and sutured using 3-0 silk sutures. Post-operative instructions and medications were prescribed for five days and the patient was reviewed after 24 hours. Every month clinical follow-up was done along with intraoral periapical radiographs. The implant was perfectly ossteointegrated within the confines of the bone with in a period of 3 months following which second stage surgery was performed for healing abutment placement. Final prosthesis was placed and reviewed clinically and with radiographic evaluation every 3 months for 1-year period [Table/Fig-1e,1f]. Excellent aesthetics was achieved.
Case 2: A 37-year-old male patient presented to the Department Of Periodontics & Implant Dentistry for management of partially edentulous area in the maxillary anterior region in relation to tooth no.12. After clinical and radiographic evaluation the patient was given the option of dental implant versus crown & bridge, the patient opted for the former. Same surgical protocol followed as the first case and dental implant$ size 3.5x13 mm [Table/Fig-2a,2b] was placed followed by xenograft* and PRF. The implant was perfectly ossteointegrated within the confines of the bone with in a period of 3 months following which second stage surgery was performed for healing abutment placement. Final prosthesis was placed and reviewed clinically and with radiographic evaluation [Table/Fig-2c] every 3 months for 1- year period.
Case 3: A 26-year-old male patient presented to the Department Of Periodontics & Implant Dentistry for management of partially edentulous area in maxillary anterior region in relation to tooth no.11. After clinical and radiographic evaluation the patient chose placement of dental implant. A dental implant$ size 3.5x13 mm was placed [Table/Fig-3a,3b] followed by xenograft* and PRF. The implant was perfectly ossteointegrated in 3 months’ time when second stage surgery was performed for healing abutment placement. Final prosthesis was placed and reviewed clinically and with radiographic evaluation [Table/Fig-3c] every 3 months for 1- year period.
Partially edentulous ridge
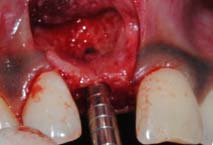
Condensation of prepared osteotomy
Platelet-rich fibrin placed over Xenograft
Prosthetic rehabilitation
Osteotomy site condensation
Osteotomy site condensation
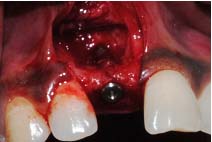
Dental implant placementn
Discussion
The technique discussed in this article have been derived from a combination of techniques suggested by Hom Lay Wang and Carl Misch [1] where their aim was augmentation of deficient alveolar ridge and correction of osseous defects around dental implants along with Tatum’s expansion techniques. Elimination of the drilling sequence prevents excessive bone loss and wash out of growth factors which helps in regeneration. Abstaining from drilling also prevents heat generation thereby avoiding bone necrosis and also aid in decreasing the healing duration of the site. PRF is a matrix of autologous fibrin in which are embedded a large quantity of platelet and leukocyte cytokines during centrifugation [2,3]. The presence of cytokines within the fibrin mesh allows for their progressive release over time period of 7-11 days which is the life span of platelet following which the network of fibrin disintegrates [4]. The PRF membrane acts like a fibrin bandage [5], which significantly serves as a matrix to accelerate the healing of the wound edges and surfaces [6]. The PRF provides post-operative protection to the surgical site and also helps to accelerate the integration and remodelling of the grafted biomaterial [3,7]. The fibrin clot plays an important mechanical role, with the PRF membrane maintaining and protecting the grafted biomaterials and PRF fragments serving as biological connectors between bone particles [8,9]. The integration of this fibrin network into the regenerative site facilitates cellular migration, particularly for endothelial cells necessary for the neoangiogenesis [2], vascularisation, and survival of the graft. The platelet cytokines (PDGF, TGF, IGF-1) are gradually released as the fibrin matrix is resorbed, thus creating a perpetual process of healing [10]. The presence of leukocytes and cytokines in the fibrin network can play a significant role in the self regulation of inflammatory and infectious phenomenon within the grafted material [11]. The clinical application of PRF helps in the integration and remodelling of both soft tissues as well as hard tissues. A major disadvantage could be the shorter duration of action of the fibrin matrix, which is about 7-10 days which signifies the life span of the platelets.
Conclusion
With ever increasing patient acceptance and demand for implant retained prosthesis, Implantologists very often face the scenario of deficient and compromised anterior ridges in majority of cases where extensive ridge augmentation followed by implant placement is advocated. This involves a lot of time and expense as well as increased number of clinical visits. Promising results along with optimal aesthetics have been achieved by this technique wherein implants are placed followed by guided bone regeneration (GBR) with bone graft and PRF in a single visit. This tremendously reduces the time as well as the expenditure involved. We would advocate this technique as an alternative to augmentation by block bone grafts or GBR involving the use of expensive membranes; though further clinical trials comparing with other bone augmentation techniques are recommended.
[1]. HL Wang, C Misch, RF Neiva, “Sandwich” bone augmentation technique: rationale and report of pilot casesInt J Periodontics Restorative Dent 2004 Jun 24(3):232-45. [Google Scholar]
[2]. DM Dohan, J Choukroun, A Diss, SL Dohan, AJ Dohan, J Mouhyi, B Gogly, Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part I: technological concepts and evolutionOral Surg Oral Med Oral Pathol Oral Radiol Endod 2006 101:e37-44. [Google Scholar]
[3]. J Choukroun, F Adda, C Schoeffler, A Vervelle, Une opportunité en paroimplantologie: le PRFImplantodontie 2001 42:55-62. [Google Scholar]
[4]. A Simonpieri, M Del Corso, G Sammartino, DM Dohan Ehrenfest, The relevance of choukroun’s platelet-rich fibrin and metronidazole during complex maxillary rehabilitations using bone allograft. Part I: A new grafting protocolImplant Dent 2009 18:102-11. [Google Scholar]
[5]. BS Vence, GA Mandelaris, DP Forbes, Management of dentoalveolar ridge defects for implant site development: An interdisciplinary approachCompend Cont Ed Dent. 2009 30(5):250-62. [Google Scholar]
[6]. VLW Gabling, Y Açil, IN Springer, N Hubert, J Wiltfang, Platelet-rich Plasma and Platelet-rich fibrin in human cell cultureOral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009 108:48-55. [Google Scholar]
[7]. DM Dohan, J Choukroun, A Diss, SL Dohan, AJ Dohan, J Mouhyi, B Gogly, Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part II: platelet-related biologic featuresOral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006 101:e45-50. [Google Scholar]
[8]. Toffler Michael, Toscano Nicholas, Holtzclaw Dan, Corso Marco Del, Dohan David, Ehrenfest Introducing Choukroun’s Platelet Rich Fibrin (PRF) to the reconstructive surgery milieuThe Journal of Implant & Advanced Clinical Dentistry. 2009 1(6):21-32. [Google Scholar]
[9]. A Simonpieri, M Del Corso, G Sammartino, DM Dohan Ehrenfest, The relevance of choukroun’s platelet-rich fibrin and metronidazole during complex maxillary rehabilitations using bone allograft. Part II. Implant surgery, prosthodontics, and survivalImplant Dent 2009 18:220-29. [Google Scholar]
[10]. Z Mazor, M Peleg, AK Garg, J Luboshitz, Platelet-rich plasma for bone graft enhancement in sinus floor augmentation with simultaneous implant placement: patient series studyImplant Dent. 2004 13:65-72. [Google Scholar]
[11]. SJ Froum, SS Wallace, DP Tarnow, SS Cho, Effect of platelet-rich plasma on bone growth and osseointegration in human maxillary sinus grafts: Three bilateral case reportsInt J Periodontics Restorative Den 2002 22:45-53. [Google Scholar]