Doppler Sonography and 3D CT Angiography of Acquired Uterine Arteriovenous Malformations (AVMs): Report of Two Cases
Senthil Kumar Aiyappan1, Upasana Ranga2, Saveetha Veeraiyan3
1Associate Professor, Department of Radiodiagnosis and Imaging,Saveetha Medical College and Hospital, Thandalam, Kancheepuram, Tamilnadu, India.
2Associate Professor, Department of Radiodiagnosis and Imaging,Saveetha Medical College and Hospital, Thandalam, Kancheepuram, Tamilnadu, India.
3Professor, Department of Radiodiagnosis and Imaging,Saveetha Medical College and Hospital, Thandalam, Kancheepuram, Tamilnadu, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Senthil Kumar Aiyappan, Associate Professor, Department of Radiodiagnosis and Imaging, Saveetha Medical College and Hospital, Thandalam, Kancheepuram, Tamilnadu-602105, India.
Phone: 9941501392,
E-mail:senthilkumarpgi@yahoo.co.in
Uterine Arteriovenous Malformations (AVMs) are rare but life threatening causes of abnormal vaginal bleeding. Accurate clinical and radiological diagnosis is essential because uterine instrumentation that is often used for management of other sources of abnormal bleeding, can lead to massive hemorrhage. Timely diagnosis and early proper treatment can markedly reduce the associated disease mortality. Ultrasound with colour and spectral doppler is the initial imaging modality of choice. Three-dimensional computed tomography (CT) angiography can determine the actual extent of the vascular malformation and helps in pre-interventional planning noninvasively. Uterine AVM can be either congenital or acquired in nature with latter being more common. We hereby report two cases of acquired AVMs diagnosed by color doppler sonography and confirmed by three-dimensional CT angiography. Both the cases reported here had previous history of dilation and curettage for abortion. Clinically one patient presented with profuse uterine bleeding and another with meno-metrorrhagia and both cases underwent surgical removal of uterus.
Doppler ultrasound, Arteriovenous malformations, CT angiography, Abnormal uterine bleeding, Embolization
Case Report
Case 1
A 38-year-old G3 P2, presented with history of recurrent meno-metrorrhagia for the past 2 months. She gave previous history of missed abortion at 12 weeks gestational age three years back for which dilation and curettage (D & C) was performed. No other significant past medical or surgical history could be elicited. General examination of the patient was normal. Per-vaginal examination showed slightly enlarged pulsatile uterus with normal vulva and cervix. Gray–scale ultrasound showed presence of tubular anechoic lesions in uterus which showed low impedance, high velocity color flow [Table/Fig-1] on doppler images. Color mosaic pattern was observed representing turbulent flow. Peak systolic velocity was 98cm/sec with resistive index of 0.33. These findings could represent arteriovenous malformation of uterus. Three-dimensional CT angiography was requested to confirm the diagnosis, rule out extra uterine involvement and to localize feeder vessels. CT angiography was performed in 64-slice multi-detector CT which showed bunch of dilated vascular channels within the uterus. The arterial supply was from uterine arteries on both sides which appeared dilated [Table/Fig-2a,b]. Patient refused transcatheter arterial embolization for economic reasons; hence hysterectomy was done after ligation of bilateral internal iliac arteries. Histopathology of the hysterectomy specimen confirmed the diagnosis of uterine AVMs.
Case 2
A 54-year-old G 2 P2, presented with profuse vaginal bleeding for the past 3 days. She had undergone curettage for retained products of conception 2 years back. No other significant past medical of surgical history could be elicited. General examination of the patient showed pulse rate of 104 beats / min with blood pressure of 90 / 60mm Hg. Emergency transvaginal ultrasound showed presence of bunch of vascular channels replacing uterus[Table/Fig-3a,b]. These vascular channels showed turbulent color flow with peak systolic velocity of 110cm / sec and low resistive index of 0.27. One of these vascular channels showed disproportionate dilatation suggestive of aneurysm formation [Table/Fig-3a,b]. Patient was shifted immediately for CT angiography to confirm the diagnosis of uterine AVM and to localize feeding vessels. CT angiography showed presence of bunch of dilated vascular channels replacing uterine cavity with aneurysm formation in one of vascular channel likely flow related aneurysm [Table/Fig-4a,b]. The arterial feeders were from bilateral uterine arteries which appeared dilated. Although few of the other branches of both internal iliac arteries were dilated, they did not supply the AVM. Patient underwent hysterectomy after ligation of bilateral internal iliac arteries. Histopathology of the hysterectomy specimen confirmed the diagnosis of AVMs.
Transabdominal pelvic doppler ultrasound image showing multiple vascular channels within uterus showing colored mosaic pattern (white arrow) suggestive of arterio-venous malformation
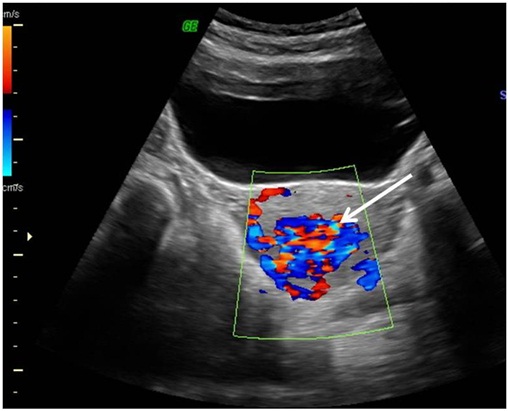
Coronal volume rendered and maximum intensity projection CT angiography images of abdomen showing tortuous vascular channels within uterus (white arrows) with arterial feeders from bilateral uterine arteries (black arrows)
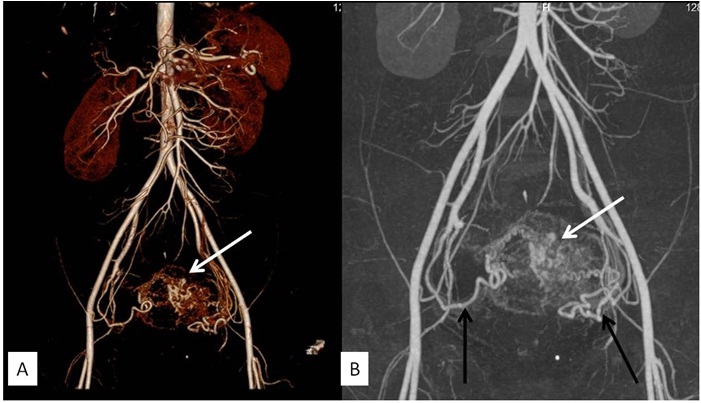
Transvaginal B mode and color doppler ultrasound images showing large anechoic structures (white arrow) within uterine cavity and wall replacing uterus which shows turbulent color flow (white arrows) suggestive of arterio-venous malformation. In addition a large disproportionately dilated vascular channel is noted in fundal region of uterus suggestive of aneurysm (black arrows) formation
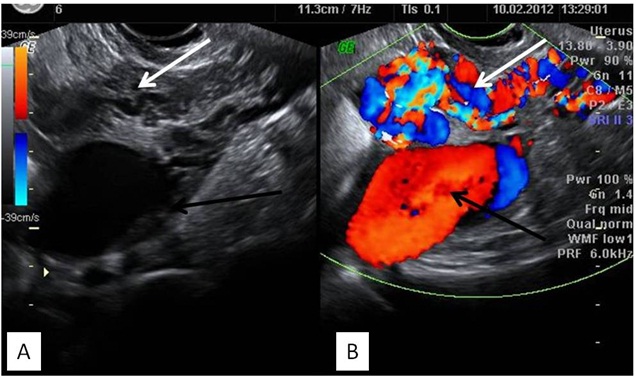
Coronal maximum intensity projection and sagittal multiplanar reformatted CT angiography images of abdomen showing dilated tortuous vascular channels replacing uterus (white arrows) with arterial feeders from bilateral uterine arteries. In addition aneurysm (black arrow) is also seen in fundal region of uterus
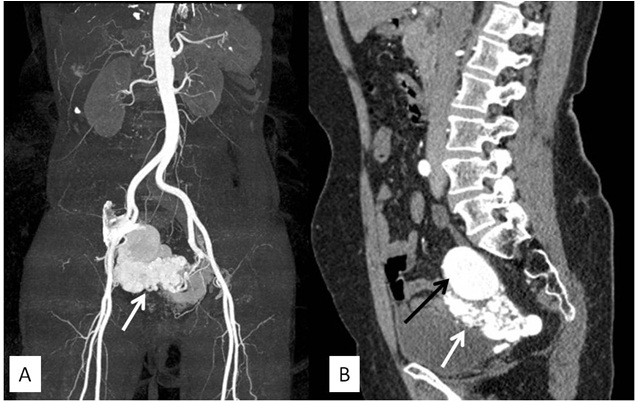
Discussion
AVMs are one of the rare causes for abnormal uterine bleeding (AUB) [1,2]. The true incidence of uterine AVMs is not known, however the reported cases are on the rise due to the increasing availability of imaging modalities like ultrasound, CT and magnetic resonance imaging (MRI) [1–3].
Uterine AVMs are classified broadly into congenital and acquired, of which acquired AVMs are more common, as in our cases [1,2]. Abnormal differentiation of primitive vascular structures during embryogenesis leads to development of congenital uterine AVM. The common causes for acquired AVMs are iatrogenic resulting 188from prior dilation and curettage, uterine surgery or therapeutic abortion, direct uterine trauma, uterine malignancy and gestational trophoblastic disease [3,4]. Both the cases reported here gave previous history of dilation and curettage. The difference between congenital and acquired AVMs are that congenital AVMs have multiple feeding arteries with a central nidus and many draining veins, contrary to acquired AVMs which have multiple small arteriovenous fistulae between intramural arterial branches and myometrial venous plexus [1,2].
Uterine AVM have been reported in ages ranging from 18 years to 72 years. The incidence of uterine vascular malformations are relatively higher in patients after abortion than in postpartum or outpatient groups as reported in a study [5]. Affected patients usually present with menorrhagia or menometrorrhagia, like in our cases[3]. Few cases may present with heavy uterine bleeding requiring transfusion.
The diagnosis of uterine AVM is clinically important as therapeutic uterine instrumentation like D & C which is done in cases of retained products of conception, may aggravate the bleeding in cases of uterine AVM [3].
The initial imaging modality of choice for uterine AVM is sonography with color and spectral doppler analysis [6]. It also helps in ruling out other conditions causing AUB like retained products of conception, trophoblastic disease, sarcoma of uterus, uterine artery pseudoaneurysm and pelvic varicose veins. In both the cases reported here, sonography with color doppler accurately suggested the diagnosis of uterine AVM. Gray scale ultrasound of uterine AVM commonly shows heterogeneous myometrium with multiple hypo to anechoic tubular structures. In few cases, grey scale ultrasound may show focal inhomogeneity or a mass resembling leiomyoma or a polyp. Application of color doppler sonography will reveal abnormal hypervascularity within the lesion with color mosaic of aliasing and flow reversal. Spectral doppler ultrasound shows low resistive index values with high velocity flow [6].
The role of three-dimensional CT angiography is to define the extent of involvement, to rule out extrauterine involvement, to differentiate between congenital and acquired uterine AVM non-invasively and to delineate the feeder vessel / uterine arteries [7,8]. In both the cases reported here, CT angiography helped in answering all the questions posted above. In patients considered for embolization, CT angiography can reduce the study time, radiation dose and contrast required for the procedure and it is also useful for anatomical conceptualization to the gynaecologist in patients planned for surgery [9]. MRI shows presence of flow voids in the region of vascular malformation and MR angiography provides the details about the vascular supply and drainage. However MRI is a costly radiological investigation and acquisition time is relatively longer for MRI and MR angiographic images compared to CT angiography. Hence CT angiography is preferred in unstable patients with heavy bleeding, those who cannot afford MRI and when MRI is contraindicated. Digital subtraction angiography (DSA) though gold standard, is usually reserved for patient planned for transcatheter embolization, because of its invasive nature.
Past medical history is also important in patients presenting with AUB and can suggest the possibility of uterine AVM in proper clinical setting. Both the cases reported here gave similar past history of dilation and curettage and in both cases ultrasound with doppler and three-dimensional CT angiography helped in confirming the diagnosis and planning the treatment.
Hence a complete clinical history combined with radiological investigations like color doppler ultrasonography and CT angiography can help in making accurate diagnosis at the earliest and reducing patient mortality. The treatment options for uterine AVMs include surgery and transcatheter uterine artery embolization [2,6]. Transcatheter uterine artery embolization has become an effective alternative to surgical intervention for uterine AVMs with major advantage of maintaining child bearing capacity [6]. Hysterectomy is preferred if patient does not want future pregnancies or when transcatheter embolization fails [1]. Since both our patients had completed their family and were economically poor to afford transcatheter uterine artery embolization, they underwent hysterectomy.
Therefore, in any patient with unexplained uterine bleeding, color doppler ultrasonography should be performed at the earliest to facilitate accurate diagnosis. Three-dimensional CT angiography helps in confirming the diagnosis of uterine AVM and provides valuable cross sectional anatomical details in patients planned for surgery or embolization.
[1]. MK Hoffman, JW Meilstrup, DP Shackelford, PF Kaminski, Arteriovenous malformations of the uterus: an uncommon cause of vaginal bleedingObstet Gynecol Surv 1997 Dec 52(12):736-40. [Google Scholar]
[2]. P O’Brien, A Neyastani, AR Buckley, SD Chang, Uterine Legiehn GM, arteriovenous malformations: from diagnosis to treatmentJ Ultrasound Med 2006 5(11):1387-92. [Google Scholar]
[3]. D Timmerman, J Wauters, S Van Calenbergh, D Van Schoubroeck, G Maleux, T Van Den Bosch, Color Doppler imaging is a valuable tool for the diagnosis and management of uterine vascular malformationsUltrasound Obstet Gynecol 2003 21(6):570-7. [Google Scholar]
[4]. E Mungen, YZ Yergok, AA Ertekin, AR Ergur, E Uçmakli, S Aytaçlar, Color doppler sonographic features of uterine arteriovenous malformations: report of two casesUltrasound Obstet Gynecol 1997 10(3):215-9. [Google Scholar]
[5]. H Yazawa, S Soeda, T Hiraiwa, M Takaiwa, S Hasegawa-Endo, M Kojima, Prospective evaluation of the incidence of uterine vascular malformations developing after abortion or deliveryJ Minim Invasive Gynecol 2013 May- Jun 20(3):360-7. [Google Scholar]
[6]. J Maldonado, C Perez, W Rodriguez, AJR Teaching file: Profuse vaginal bleeding seven weeks following induced abortionAJR Am J Roentgenol 2008 191(6):S79-82. [Google Scholar]
[7]. NA Wani, F Shaheen, T Kousar, T Gojwari, Uterine arteriovenous malformation diagnosed with multislice computed tomography: A case reportJ Reprod Med. 2010 55((3-4)):166-70. [Google Scholar]
[8]. T Umezu, A Iwase, T Ota, K Suzuki, A Nakagawa, T Nakahara, Threedimensional CT angiography is useful for diagnosis of postabortion uterine hemorrhage: 3 case reports and review of the literatureJ Minim Invasive Gynecol17(2):246-51. [Google Scholar]
[9]. MS Gulati, SB Paul, A Batra, D Sarma, V Dadhwal, J Nath, Uterine arteriovenous malformations: the role of intravenous ‘dual-phase’ CT angiographyClin Imaging. 2000 24(1):10-4. [Google Scholar]