A Rare Case of Primary Supraclavicular Lymphadenitis due to Cryptococcus Neoformans in an HIV Infected Patient
Anuradha Sood1, Lata R Chandel2, Smriti Chauhan3, Kamlesh Thakur4, S.C Jaryal5
1Assistant Professor, Department of Microbiology,Dr Rajendra Prasad Government Medical College, Kangra, Himachal Pradesh, India.
2Senior Resident, Department of Microbiology,Dr Rajendra Prasad Government Medical College, Kangra, Himachal Pradesh, India.
3Medical Officer, Department of Microbiology,Dr Rajendra Prasad Government Medical College, Kangra, Himachal Pradesh, India.
4Professor & Head, Department of Microbiology,Dr Rajendra Prasad Government Medical College, Kangra, Himachal Pradesh, India.
5Associate Professor, Department of Microbiology,Dr Rajendra Prasad Government Medical College, Kangra, Himachal Pradesh, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Smriti Chauhan, Medical Officer, Department of Microbiology, Dr Rajendra Prasad Government Medical College, Kangra at Tanda, Himachal Pradesh, India.
Phone: +919418070808,
E-mail: drsmriti123@gmail.com
Cryptococcosis caused by encapsulated yeast Cryptococcus neoformans most commonly presents as disease of the central nervous system. Cryptococcus is a non–mycelial budding yeast found in soil, pigeon droppings and their nesting places. The three ‘classic’ virulence factors of cryptococci are: polysaccharide capsule, melanin production and growth at 37°C. Here, we present a rare case of cryptococcosis affecting left supraclavicular lymph node in a Human Immunodeficiency virus (HIV) infected individual. Culture of fine needle aspirate of the lymph node yielded Cryptococcus neoformans which was identified by standard microbiological techniques. Meyer’s mucicarmine stain imparted a typical rose burgundy colour to the capsule. Unusual characteristics of the isolate included poorly developed capsule and the presence of yeast in chains resembling pseudo-hyphae. This case highlights the importance of microbiological techniques for diagnosis and prompt treatment of cryptococcosis.
Lymph node, Cryptococcus neoformans, Hypocapsular variant
Case Report
A 27-year-old female, presented to the outpatient department of Medicine at Dr Rajendra Prasad Government Medical College on February 2012, with chief complaints of low grade fever, cough and significant weight loss of two months duration. On general physical examination bilateral cervical lymphadenopathy and enlargement of the left supraclavicular lymph node (3cm ×3cm) was evident. Oral thrush was also present while other vital signs were within normal limits. On systemic examination she had moderate splenomegaly. Routine haematological as well as biochemistry investigations were within normal limits. Sputum examination was negative for acid fast bacilli. On chest X-ray left hilar lymphadenopathy was seen. From the site of oral thrush Candida albicans was isolated and identified.
Giemsa stained Fine Needle Aspiration Cytology (FNAC) of left supraclavicular lymph node revealed 5-15μm spherical yeast cells with narrow-based budding, scattered lymphocytes and epitheloid cells. The yeast cells were poorly encapsulated, engulfed inside macrophages and present in chains closely resembling pseudo-hyphae. The aspirate of FNAC was subjected to culture on Sabouraud’s Dextrose Agar medium (SDA). After 48 hours white to cream, smooth and non-mucoid colonies were isolated [Table/Fig-1]. The growth was identified as Cryptococcus neoformans based on the findings of Gram Stain, biochemical tests (i.e, hydrolysis of Christensen’s urea agar, inositol and nitrate assimilation) and negative germ tube test. On India ink preparation yeast cells with a thin, narrow capsule was demonstrated. This was further confirmed by Meyer’s mucicarmine stain as it imparted a typical rose burgundy colour to the capsule [Table/Fig-2]. There was no increase in the size of the capsule even when it was sub-cultured in 1% peptone solution and on chocolate agar at 370C in a CO2 incubator [1].
Based on the above findings, the patient was referred to Integrated Counselling and Testing Centre (ICTC). After counselling and obtaining an informed consent, blood of the patient was collected for HIV testing. Serology was reactive for HIV-1. Cerebrospinal fluid examination by India ink, culture and antigen detection for cryptococcus was negative. Sputum and stool examination were negative for other opportunistic microorganisms. The patient was treated with amphotericin B 0.7mg/kg /day intravenously. With treatment her lymphadenopathy subsided. However the patient refused to undergo a repeat FNAC to confirm microbiological cure. She was further referred to Anti-Retroviral Centre for CD4 cell count and antiretroviral treatment.
Culture of Cryptococcus neoformans showing white to cream, smooth and non-mucoid colonies
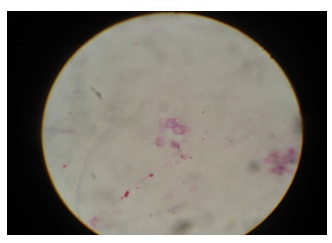
Meyer’s mucicarmine stain showing a typical rose burgundy colour of the capsule of Cryptococcus neoformans (X400)
Discussion
Few fungi are pathogenic to humans. Cryptococcosis has emerged as the second most common fungal infection after candidiasis in HIV infected individuals and potentially the most serious one [1]. C. neoformans is a basidiomycetous fungus that is ubiquitous in the environment. It is found in soil, on flowers of trees like Eucalyptus and in excreta of wild and domestic birds. Because of its ubiquity, it has been suggested that most people are exposed to C. neoformans early in life.
In immune-competent human hosts, the usual primary infection is pulmonary and most often subclinical. On the other hand, in immunosuppressed individuals cryptococcal infection commonly manifests as meningoencephalitis, pneumonia, skin lesions, eye lesions, bone and joint involvement. Rare manifestations include lymphadenopathy, endocarditis, hepatitis, lesions of gastrointestinal tract, pyelonephritis and prostatitis. Its usual route of entry into humans is through inhalation of non or poorly encapsulated form of the organism.
Cryptococcus neoformans is known for its predilection to the CNS and about 70-90% of the patients present with subacute meningitis or meningoencephalitis [2]. This patient however, did not show any central neurological signs and symptoms. Cryptococcal lymphadenitis is an uncommon form of extra pulmonary cryptococcosis in patients with AIDS [3-4]. Only few cases have been reported worldwide [5-6]and from India [3-4]. Cryptococcal lymphadenitis in the absence of AIDS is extremely rare. Such cases are initially suspected of a diagnosis of lymphoma or tuberculosis [7]. This further necessitates the need of tissue diagnosis to ensure earliest appropriate treatment.
C. neoformans’ virulence is mediated predominantly by a polysaccharide capsule which provides a physical barrier that interferes with normal phagocytosis and clearance by the immune system. Usually the size of capsule is several times the size of the yeast cell. The capsule size and morphology has been seen to vary under different growth conditions. There have been reports of isolation of cryptococci having smaller capsules from patients with AIDS [6].
Absence of pseudohyphae have been used to differentiate Cryptococcus species from yeasts like Candida. However, the presence of pseudohyphae, as demonstrated in our case, has been recently observed by other workers also. This is a rare case of involvement of the left supraclavicular lymph node in which Cryptococcus neoformans isolate showed atypical features like poorly developed capsule and the presence of yeast cells in chains similar to pseudohyphae.
Conclusion
Our diagnosis in this exceptional case helped the physicians to initiate prompt and specific treatment. This highlights the importance of culture and other microbiological techniques in such cases.
[1]. J Chander, Textbook of Medical Mycology 2002 2nd EditionNew DelhiMehta Publishers:231-49. [Google Scholar]
[2]. TG Mitchell, JR Perfect, Cryptococcosis in the era of AIDS’100 years after the discovery of Cryptococcus neoformansClinical Microbiological Reviews. 1995 8(4):515-48. [Google Scholar]
[3]. AK Sainath, M Ahuja, I Shaik, Cryptococcal Lymphadenitis on fine needle aspiration CytologyPeople’s Journal of Scientific Research 2012 5(2):33-5. [Google Scholar]
[4]. P Bhuyan, K Pattnaik, A Kar, RC Brahma, S Mahapatra, Cryptococcal lymphadenitis in HIV: a chance diagnosis by FNACDiagn Cytopathol 2013 41(5):456-8. [Google Scholar]
[5]. ES Jacobson, TJ Tingler, PL Quynn, Effect of hypertonic solutes upon the polysaccharide capsule in Cryptococcus neoformansMycoses 1989 32(1):14-23. [Google Scholar]
[6]. EJ Bottone, M Toma, BE Johansson, GP Wormser, Poorly encapsulated Cryptococcus neoformansfrom patients with AIDS. I: Preliminary observationsAIDS Res 1986 2(3):11-18. [Google Scholar]
[7]. F Bao, H Tan, W Liu, Y Li, H Li, Pediatric cryptococcal lymphadenitis in the Absence of AIDS: Case report and literature reviewCase Reports in Pediatrics 2013 Article ID 563081. [Google Scholar]