Rippled Pattern Extraocular Sebaceous Carcinoma: A Rare Case Report with Brief Review of Literature
Amita K.1, Vijayshankar S.2, Shobha S.N.3
1 Associate Professor, Department of Pathology, Adichunchanagiri Institute of Medical Sciences, Karnataka, India.
2 Associate Professor, Department of Pathology, Adichunchanagiri Institute of Medical Sciences, Karnataka, India.
3 Assistant Professor, Department of Pathology, Adichunchanagiri Institute of Medical Sciences, Karnataka, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr Amita K., Associate Professor, Department of Pathology, Adichunchanagiri Institute of Medical Sciences B.G. Nagara. Mandya District-571448, Karnataka, India.
Phone: 09901429624,
E-mail: dramitay@rediffmail.com
Sebaceous carcinoma (SC) is a highly aggressive malignant adnexal tumor of sebaceous gland origin, accounting for less than 1% of cutaneous. Extraocular sebaceous carcinomas are more aggressive than their ocular counterpart with a predilection for the skin of head and neck, trunk, salivary glands and extremities in decreasing order of frequency. Rippled effect literally means “gradually spreading effect”. In histopathology it describes the unique arrangement of tumor cells in palisading pattern. The tumors in which rippled effect has been reported include adnexal tumors like trichoblastoma, trichomatricoma, trichoblastoma with sebaceous differentiation, trichoblastoma with apocrine differentiation, sebaceoma, basal cell carcinoma, fibrohistiocytic tumors, mesenchymal tumors and melanocytic tumors. We report the first case of extra ocular sebaceous carcinoma with rippled effect with emphasis on the fact that differentiation from other tumors demonstrating rippled effect is important in view of different treatment protocols.
Extraocular, Sebaceous carcinoma, Rippled pattern
Case Report
A 61–year–old male presented with slowly growing swelling over the ala of nose, of 6 months duration. There was no history of fever, weight loss or diminished appetite. Local examination revealed a dome–shaped swelling measuring 2.5 x 1.5 cm. There was no evidence of any lymphadenopathy. Clinically, a diagnosis of a benign lesion of nose was made. A complete local excision was performed and specimen sent for histopathology.
Gross: Specimen consisted of a single globular skin covered mass measured 2.5 x 1.5 x 0.5 cm. Area of focal ulceration was noted. Cut surface was solid, lobulated and grey white [Table/Fig-1A].
(A) Gross image showing solid, white and lobulated cut surface.(B) Hematoxylin and eosin (H & E) section showing an atrophic epithelium and a subepithelial tumor. [H & E, x 40]
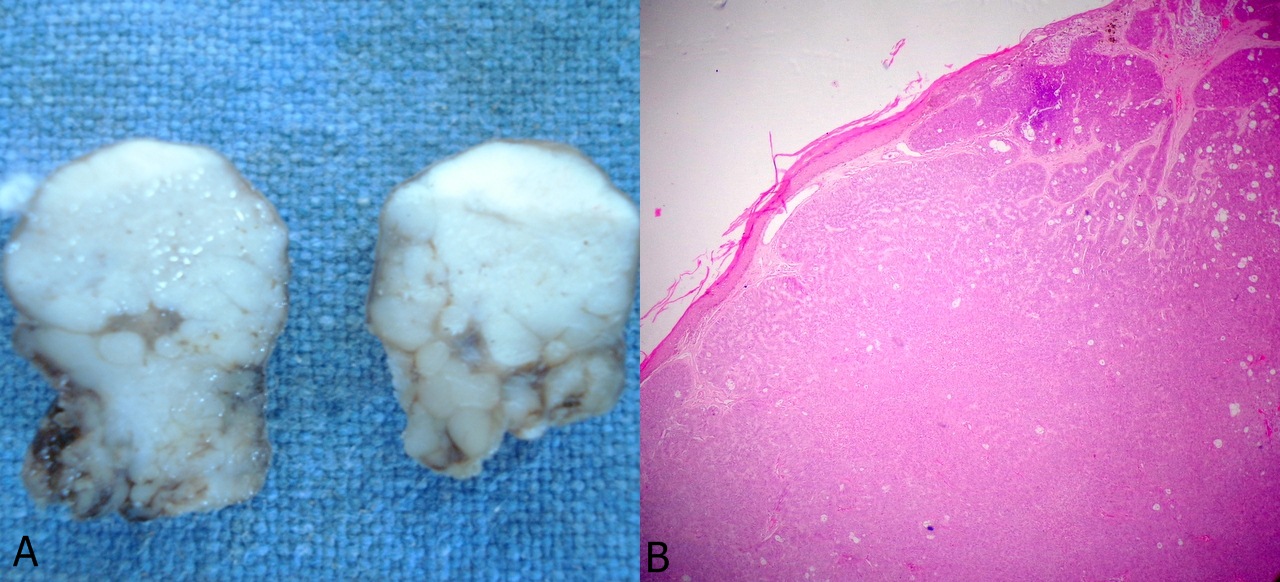
Histopathology sections showed skin which was atrophic, with focal ulceration. Sub–epithelium showed an asymmetric, poorly circumscribed tumour comprising of cells arranged in lobules of varying sizes, separated by fibrous stroma [Table/Fig-1B]. The tumour cells were typically arranged in palisading pattern, resembling waves of water–rippled pattern [Table/Fig-2A]. The individual cells were moderately pleomorphic, elongated with scant eosinophilic cytoplasm, nucleus with vesicular chromatin, overcrowding and prominent eosinophilic nucleoli. Centres of the lobules showed occasional sebaceocytes with multi–vacuolated cytoplasm and starry nuclei. [Table/Fig-2B and C] Infiltration was seen deep in the dermis. The centre of lobules showed necrosis [Table/Fig-2D].
(A) Tumour nodules of varying sizes are seen. Note: the tumour cells typically arranged in palisading pattern resembling waves of water–rippled pattern. [H & E, x 40] Inset in (A)-Higher power view of the palisading. [H & E, X 100]; (B) Section depicts varying sized lobules with occasional sebaceocytes with multi vacuolated cytoplasm and starry nuclei. [H&E, × 40]; (C) - Higher power view of the sebaceous differentiation along the nuclear crowding, Vesicular nuclei and prominent nucleoli. [H & E, x 100] Inset in (C) - Higher power view showing vesicular nucleus with prominent eosinophilic nucleoli. [H & E, x 100]; (D) - Section depicting necrosis in the centre of the lobules. [H & E, × 100]
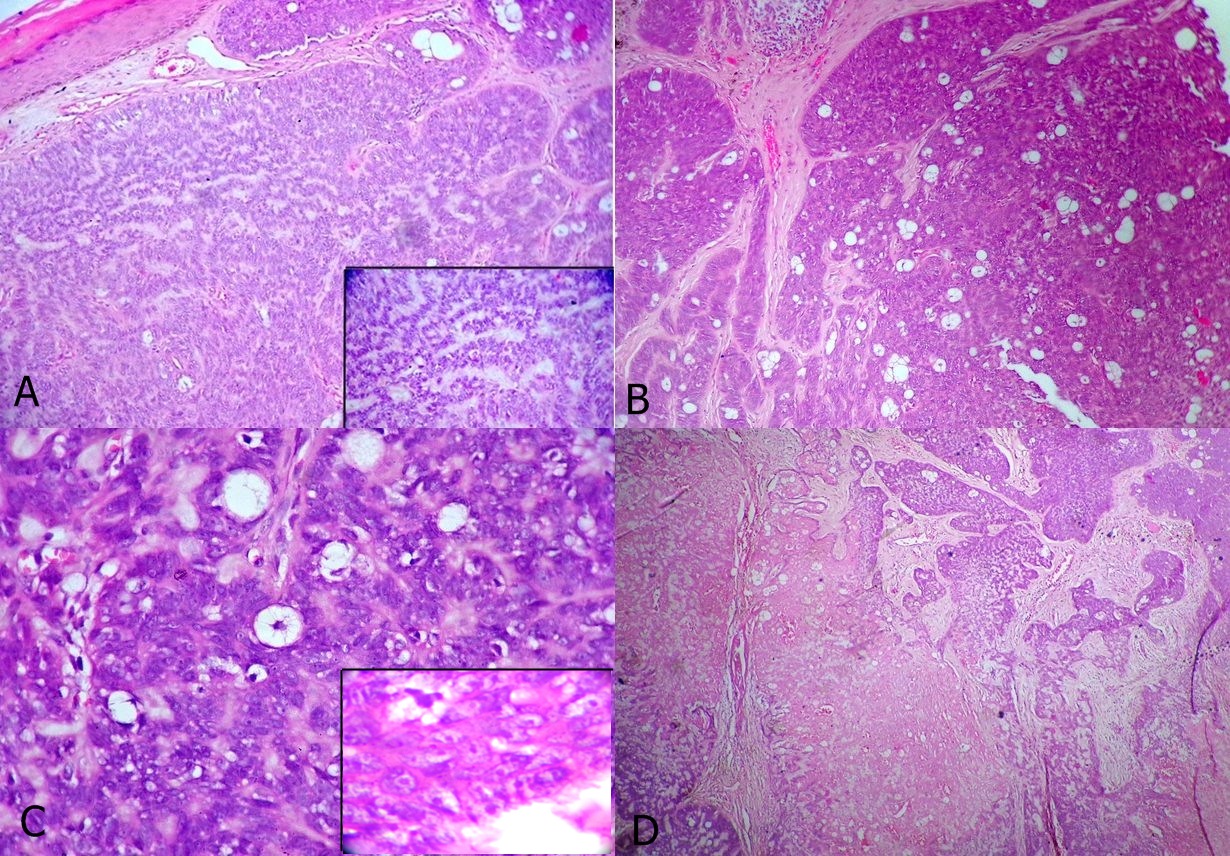
Hence, a final diagnosis of sebaceous cell carcinoma with rippled pattern was made. A thorough investigation was done, to rule out any internal malignancy.
Discussion
Sebaceous Carcinoma (SC) is a highly aggressive malignant adnexal tumour of sebaceous gland origin, accounting for less than 1% of cutaneous malignancies [1]. Topographically, it can occur at ocular or extra ocular sites. The extra ocular sites being the skin of head and neck, trunk, salivary glands and extremities in decreasing order of frequency. Extra ocular tumours are historically thought to be uncommon and less aggressive than their ocular counterparts. A recent large scale study has drawn attention to the fact that extra ocular SCs are more aggressive and that they occur in increasing frequency, accounting for two thirds of all the cases [2].
‘Rippled effect’ literally means “gradually spreading effect”. In histopathology, this term was first pronounced by Hashimoto et al in 1989, wherein he pertinently used it for describing the unique arrangement of tumour cells in palisading pattern, in the form of parallel rows of cells, forming ribbons, separated by extracellular matrix, resembling a verocay body formation [3]. He described it in association with trichoblastomas. There have not been many case reports on this unique pattern in the literature. Other than trichoblastomas, tumours in which rippled pattern has been reported include other adnexal tumours like sebaceomas, basal cell carcinomas, fibrohistiocytic tumours, mesenchymal tumours and melanocytic tumours [4].
Adnexal tumours in which rippled pattern has been documented include mainly trichogenic tumours as trichoblastomas (5 cases), trichomatricomas (1 case), trichoblastomas with sebaceous differentiation (1 case), trichoblastomas with apocrine differentiation (1 case) and sebaceomas. Ansai et al., 2009, in a large study of eighty cases of sebaceomas, documentated that 26.3% of sebaceomas demonstrated rippled pattern [5]. Till date, there is no case report on sebaceous carcinomas with rippled patterns. Histopathologically, focal presence of rippled pattern does not pose much difficulty in diagnosis. However, when the pattern is seen throughout the tumour, diagnosis becomes a challenge, as was in our case. In such cases, distinction from trichoblastomas with sebaceous differentiation, sebaceomas with rippled pattern on the benign spectrum and basal cell carcinomas with sebaceous differentiation at the other end, holds implications with respect to the biologic behaviour, treatment planning and prognosis [5].
Trichoblastomas and trichoblastomas with sebaceous differentiation are benign tumours of follicular derivation, which closely resemble sebaceomas, so much that some authors consider it difficult to distinguish between the two entities [6]. However, trichoblastomas exhibit some unifying features like formation of hair germ papillae, palisading at the periphery and a trichogenic stroma, which clinches the diagnosis [5]. Sebaceomas, in turn, are characterized by the presence of small duct like spaces with cuticular keratin, sebaceocytes with vacuolated cytoplasm, starry nuclei and pseudo rosettes in carcinoid like pattern [5]. Distinction of SCs from sebaceomas is based on both architectural and cytologic features. Sebaceomas demonstrate sharp circumscription and good symmetry, while SCs are assymetrical, poorly circumscribed with deep infiltration and superficial ulceration. On cytology, prominent eosinophilic nucleoli, atypia and en mass centrilobular tumour necrosis favour a SC [7].
The pathogenesis of rippled growth pattern remains a matter of speculation. As has been proposed for verocay bodies, the overexpressions of laminin and phospholipids lead to cell to cell adhesion, resulting in the unifying appearance. However, absence of extracellular matrix production in SC mystifies the hypothesis [3]. SC has been more frequently associated with Muir torre syndrome as compared to other sebaceous lesions. Hence, thorough investigation is indicated, to rule out an internal malignancy [4].
Treatment should aim at wide surgical excision with regional lymph node removal. Prognosis of extra ocular tumours is worse.
Conclusion
We reported the first case of extra ocular sebaceous carcinoma with rippled pattern, with emphasis on the fact that its differentiation from other tumours demonstrating rippled pattern is important in view of different treatment protocols.
[1]. Al-Shobaili HA, Alghamdi KM, Al-Ghamdi WA, Cystic sebaceous carcinoma: is it a constant pathognomonic marker for Muir-Torre syndrome?J Drugs Dermatol 2007 6:540-43. [Google Scholar]
[2]. Dasgupta T, Wilson LD, Yu JB, A retrospective review of 1349 cases of sebaceous carcinomaCancer 2009 115:158-65. [Google Scholar]
[3]. Hashimoto K, Prince C, Kato I, Ito M, Tazawa T, Pelachyk JM, Rippled pattern trichomatricoma: histological, immunohistological and ultrastructural studies of an immature hair matrix tumorJ Cutan Pathol 1989 16:19-30. [Google Scholar]
[4]. Biswas A, Setia N, Bhawan J, Cutaneous Neoplasms With Prominent Verocay Body–Like Structures: The So-called “Rippled PatternAm J Dermatopathol 2011 33:539-50. [Google Scholar]
[5]. Ansai S, Kimura T, Rippled-pattern sebaceoma: a clinicopathological studyAm J Dermatopathol 2009 31:364-66. [Google Scholar]
[6]. Misago N, Narisawa Y, Rippled-pattern sebaceomaAm J Dermatopathol 2001 23:437-43. [Google Scholar]
[7]. Misago N, Mihara I, Ansai S, Narisawa Y, Sebaceoma and Related Neoplasms with Sebaceous Differentiation. A Clinico pathologic Study of 30 CasesAm J Dermatopathol 2002 24:294-304. [Google Scholar]