Brain Abscess as A Complication of Chronic Thromboembolic Pulmonary Hypertension – A Rare Case Report
Lakshmi K1, Santhanam R2, Chitralekha S3
1 Assistant Professor, Department of Microbiology, Sree Balaji Medical College and Hospital, Chennai, India.
2 Associate Professor, Department of Neurosurgery, Sree Balaji Medical College and Hospital, Chennai, India.
3 Professor, Department of Microbiology, Sree Balaji Medical College and Hospital, Chennai, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Santhanam R, Associate Professor, Department of Neurosurgery, Sree Balaji Medical College and Hospital, No 7, CLC Works Road, Chromepet, Chennai – 600044, Tamil nadu, India.
Phone: 9445349440,
E-mail: drsanthanam79@yahoo.co.in
A brain abscess is a life threatening condition which can occur as a complication of various clinical conditions. An intra–cerebral abscess which occurs as a complication of pulmonary arterial hypertension is extremely rare. The present report has described such an uncommon case of an intra–cerebral abscess in a chronic pulmonary thrombo embolism patient with pulmonary hypertension. A–34–year old male who was a known case of chronic pulmonary thrombo embolism with pulmonary artery hypertension, who was diagnosed 6 months back, presented to the Out Patients Department (OPD) with headache and vomiting. He had right homonymous hemianopia. Contrast MRI (Magnetic Resonance Imaging) of brain showed a peripherally enhancing lesion in the left temporo-occipital lobe, with oedema and a mass effect. Left parieto–occipital craniotomy and excision of the abscess was done. Staphylococcus aureus was isolated from the aspirated pus.
Brain abscess, Chronic thromboembolic pulmonary hypertension, MRI
Introduction
A brain abscess is a serious life threatening infection of brain parenchyma [1]. It results from a spread of infection from contiguous non-neuronal tissue, haematogenous seeding or a direct introduction into the brain [2]. Predisposing factors which have been identified include congenital heart disease with a right to left shunt, infections of the middle ear, mastoid, paranasal sinuses, orbit, face and scalp, penetrating skull injuries and comminuted skull fractures or intracranial surgeries [3]. But a brain abscess which occurs as a complication of pulmonary hypertension is very rare. Chronic thromboembolic pulmonary hypertension (CTEPH) itself is a very rare disorder, with an incidence of less than 0.5% of all thromboembolic diseases [4]. Thromboembolic manifestations can occur in severe pulmonary hypertension cases, which are mostly under diagnosed. To the best of our knowledge, a brain abscess as a complication of CTEPH, has not been reported in the literature.
Case Report
A 34–year–old male presented to the Neurology OPD with complaints of severe headache which was there since 10 days and vomiting for past 72 hours. Six months ago, he had been admitted to the hospital with exertional dyspnoea, with clinical features which were suggestive of acute pulmonary embolism. His complete blood picture, liver and renal function tests, blood gas analysis and coagulation profiles were normal. An echocardiogram was performed, which showed pulmonary hypertension with a pressure of about 70 mm Hg (expected normal pressure limit was 20 to 30 mm Hg). A ventilation-perfusion (V/Q) scan visualised an obstructive thrombus in the right proximal pulmonary artery. A conventional pulmonary angiogram showed changes which reflected the findings of the perfusion lung scan. A CT angiogram showed right pulmonary artery major emboli. The measured pulmonary trunk pressure was 66 mm Hg. He was diagnosed as a case of thromboembolic pulmonary hypertension and was started on anticoagulants and sildenafil citrate. His symptoms responded to the treatment.
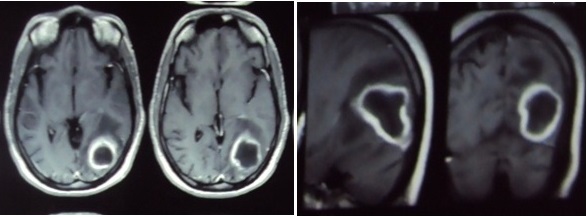
In the present admission, he had developed headache and had frequent episodes of vomiting since 10 days. He did not have any seizures or loss of consciousness. There was no history of fever or ear discharge. On examination, he did not have pallor, but had clubbing of the nails in both the hands and feet; he was conscious, alert and oriented. Both his pupils were reacting; optic fundi showed papilledema and he had right homonymous hemianopia. Clinically, an intra–cerebral haemorrhage or venous sinus thrombosis with a venous infarct was suspected. However, contrast MRI of brain showed a peripherally enhancing lesion in the left temporo occipital lobe, with oedema and a mass effect [Table/Fig-1 and 2]. Left parieto– occipital craniotomy and excision of the brain abscess were done. The aspirated pus was sent to the Microbiology Laboratory. Direct smear gram staining was done and cultures were put up in Nutrient agar, Blood agar and Mac Conkey’s agar plates. The culture media were incubated at 370C for 24 hours. Staphylococcus aureus was isolated from the culture. The organism was identified by using standard techniques. An antibiotic susceptibility test was performed on Muller–Hinton agar by Kirby–Bauer method. The isolated S. aureus from the sample was found to be susceptible to cephalosporins, chloramphenicol, piperacillin, quinolones and penicillin. The organism was resistant to erythromycin.
MRI Brain showing left temporo occipital peripherally well enhancing lesion with central cavitation and peri–lesional edema
Discussion
A brain abscess is a rare infection of the brain parenchyma. According to the literature, 14-25% of brain abscesses are of unknown aetiology [5]. Brain abscesses usually arise from haematogenous dissemination of organisms from distant sites. Cerebral abscesses had been found in cases of chronic lung infections like bronchiectesis, lung abscesses, and acute bacterial endocarditis. In these conditions, the right to left cardiac shunt allows organisms to migrate from venous to systemic circulation. A brain abscess can also occur as a complication of hepatopulmonary syndrome which co–exists with interstitial pneumonia [6]. Congenital heart disease in children which predisposes to brain abscesses, accounts for 6-50 % of brain abscess cases [7]. Haemorrhagic telangiectasis is another condition in which a haematogenous brain abscess can occur as a complication. Sometimes, brain abscesses can arise in cases of otitis, sinusitis or mastoiditis through emissary veins. The other causes include trauma, dental sepsis, surgery and facial infections.
Rare causes of brain abscesses have been reported in literature. Brain abscesses have been recognised as a complication of cystic fibrosis [8]. Herskovitz et al., in [9], reported brain abscesses as a complication of tongue piercing.
Brain abscesses are one of the main complications of pulmonary arteriovenous malformations [10]. However, a brain abscess which occurs as a complication of pulmonary artery hypertension is extremely rare. Bronchial artery hypertrophy is observed in most of the patients with CTEPH and haemoptysis has been reported as a complication in such patients [11]. An intracranial haemorrhage which occurs as a complication of anticoagulants which are used in a patient with chronic pulmonary thromboembolism is a strong differential diagnosis, when this patient presents with features of a raised intracranial pressure and focal neurological deficits.
The most common organisms which are isolated from brain abscesses are various strains of Streptococci, that account for approximately 60-70% of all brain abscess formations [12]. Staphylococcus species was the second most common organism which was isolated in previous studies [13]. It was found to be more in cases which were caused by trauma and postsurgical infections. In this patient, Staphylococcus aureus was isolated from the material which was aspirated from the abscess. The organism was found to be susceptible to methicillin.
To conclude, a brain abscess is a serious infection which can be life threatening. Hence, it must be diagnosed early and treated aggressively. Since it is very uncommon in patients with chronic pulmonary embolism with pulmonary hypertension, a high index of suspicion for intracerebral abscesses is required, when they present with raised intra–cranial pressure features and focal neurological deficits. An immediate surgical intervention must be carried out if it is necessary. Samples must be collected by taking sterile precautions and they must be plated on appropriate culture media promptly, for an early detection of the causative agents. Antibiotic susceptibility testing helps in proper management of such cases.
[1]. Brook I, Brain abscess in children; microbiology and managementJ Child Neurol 1995 10(4):283-8. [Google Scholar]
[2]. Goodkin HP, Harper MB, Pomeroy SL, Intracranial abscess in children: Historical trends at Children’s hospital, BostonPediatrics 2004 111(8):1765-70. [Google Scholar]
[3]. Takeshita M, Kagawa M, Yonetani H, Izawa M, Yato S, Nakanishi T, Monma K, Risk factors for brain abscess in patients with congenital cyanotic heart diseaseNeurol Med Chir 1992 32(9):667-70. [Google Scholar]
[4]. Moser KM, Auger WR, Fedullo PF, Jamieson SW, Chronic thromboembolic pulmonary hypertension: Clinical picture and surgical treatmentEur Respir J 1992 5:334-42. [Google Scholar]
[5]. Pit S, Jamal F, Cheak FK, Microbiology of cerebral abscess: a four year study in MalaysiaJ Trop Med Hyg 1993 96(3):191-06. [Google Scholar]
[6]. Yanagihara T, Moriwaki A, Seki N, Akata K, Imanaga T, A brain abscess as a complication of hepatopulmonary syndrome coexisting with interstitial pneumoniaNihon Kokyuki Gakkai Zasshi 2011 49(7):534-07. [Google Scholar]
[7]. Mathisen GA, Johnson PJ, Brain abscess: state of the art clinical articleClin Infect Dis 1997 25:763-81. [Google Scholar]
[8]. Rabkin CS, Blaser MJ, Brain abscess: A complication of cystic fibrosis in adultsAnn Neurol 1984 15:608-10. [Google Scholar]
[9]. Herskovitz MY, Goldsher D, Finkelstein R, Bar-Lavi Y, Constantinescu M, Telman G, Multiple brain abscesses associated with tongue piercingArch Neurol 2009 66(10):1292 [Google Scholar]
[10]. Gossage JR, Kanj G, Pulmonary arteriovenous malformations: a state of the art reviewAm J Respir Crit Care Med 1998 158:643-661. [Google Scholar]
[11]. Reesink HJ, van Delden OM, Kloek JJ, Jansen HM, Reekers JA, Bresser P, Embolization for hemoptysis in chronic thromboembolic pulmonary hypertension: report of two cases and a review of the literatureCardiovasc Intervent Radiol 2007 Jan-Feb 30(1):136-09. [Google Scholar]
[12]. Mandell GL, John E, Dolin R, Principle and practice of infections diseases 1995 4th edNew York (NY)Churchill Livingstone [Google Scholar]
[13]. Al-Rashdi Fatima M., Al-Ismaily Latifa K., Devi Kokkuvayil L., Common bacteria isolated from brain abscessesNeurosciences 2004 9(3):196-198. [Google Scholar]