Ovarian Gonadoblastoma with Dysgerminoma in a Young Girl with 46, XX Karyotype: A Case Report
Deepa V Kanagal1, Kishan Prasad2, Aparna Rajesh3, Rohan G Kumar4, Sara Cherian5, Harish Shetty6, Prasanna Kumar Shetty7
1 Associate Professor, Department of Obstetrics and Gynaecology, K.S. Hegde Medical Academy.
2 Associate Professor, Department of Pathology, K.S. Hegde Medical Academy.
3 Associate Professor, Department of Obstetrics and Gynaecology, K.S. Hegde Medical Academy.
4 Assistant Professor, Department of Surgery, K.S. Hegde Medical Academy.
5 Post Graduate, Department of Obstetrics and Gynaecology, K.S. Hegde Medical Academy.
6 Professor and HOD, Department of Obstetrics and Gynaecology, K.S. Hegde Medical Academy.
7 Professor, Department of Obstetrics and Gynaecology, K.S.Hegde Medical Academy.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Deepa V. Kanagal, No. 104, Dune Apartments, Kadri, Shivbagh, Mangalore, Karnataka, India.
Phone: 09980164615,
E-mail: deepakanagal@yahoo.co.in
Gonadoblastoma is a rare gonadal tumour consisting of a mixture of germ cells and sex cord stromal derivatives resembling immature granulosa and Sertoli cells. It usually arises in various types of gonadal dysgenesis containing Y chromosome like pure or mixed gonadal dysgenesis. Occurrence in phenotypically and chromosomally normal women is very rare. We report here a case of gonadoblastoma with dysgerminoma in a 14–years–old girl who presented with a huge tumour, virilisation and normal 46XX karyotype. Association of dysgerminoma is seen in 50% cases of gonadoblastomas. Elevated tumour markers like hCG and alpha Fetoprotein may make the diagnosis challenging.
Gonadoblastoma, Dysgerminoma, 46XX Karyotype, Tumour
Introduction
Gonadoblastomas are rare gonadal tumours, almost always arising from a dysgenetic gonad with a Y chromosome [1]. Most patients have 46XY karyotype or various forms of mosaicism [2]. However, rare cases with normal 46, XX karyotype have been reported.
They have a distinctive histological appearance which distinguishes them from any other gonadal neoplasm and were first described by Scully in 1953 [1]. They are composed of germ cells intimately admixed with sex cord derivatives resembling immature Sertoli and granulosa cells [3].
In 50%–60% of cases gonadoblastomas are associated with malignant germ cell tumours, mostly presenting as pure dysgerminoma or less frequently as immature teratoma, Yolk sac tumour, embryonal carcinoma or choriocarcinoma [4]. Scully reviewed 74 gonadoblastoma cases and found that approximately half of the tumours were overgrown by dysgerminoma as coexisting germ cell tumour [1].
Because of its extreme rarity, we present this case of gonadoblastoma with dysgerminoma in a 14 year old girl with normal karyotype.
Case Report
A 14–years–old girl presented to us with distension of abdomen, excessive hair growth over the body and hoarseness of voice. All these complaints were from the past 3 months. She had attained menarche 2 years back and had menstruated only 4 to 5 times.
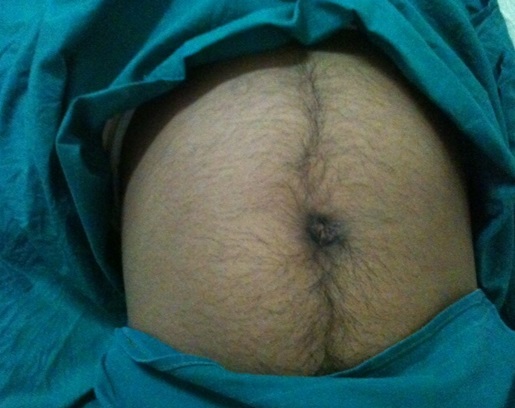
On examination, the girl was short statured with hirsutism. Her built was moderate. There was excessive hair growth over the face, chest, abdomen, thighs and gluteal region. There was associated clitoromegaly. Breast development and pubic hair were normal. Per abdomen examination revealed a huge intra–abdominal mass occupying the whole abdomen [Table/Fig-1]. The mass had a variable consistency with irregular surface. Ultrasound showed a vascular solid tumour with calcification. CT scan revealed associated ascites and para aortic lymph node enlargement [Table/Fig-2]. Tumour markers showed an elevation of LDH. There was also a gross elevation of beta hCG and testosterone levels. Karyotyping revealed a normal 46XX karyotype. With the probable diagnosis of germ cell tumour, mostly dysgerminoma, she was taken for an exploratory laparotomy.
Tumour occupying the whole abdomen with hirsutism
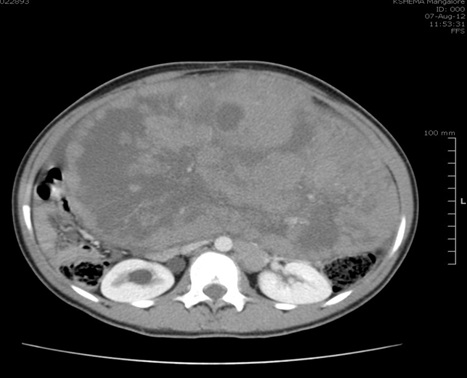
CT showing tumour,enlarged paraaortic lymph nodes
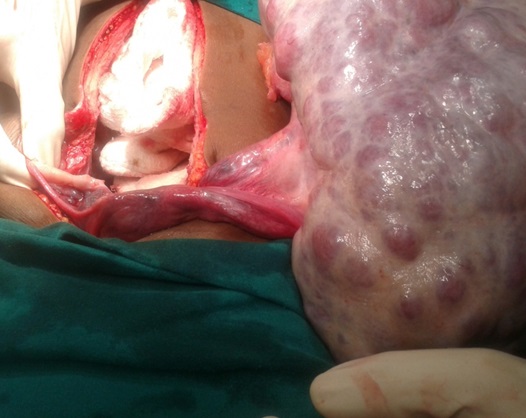
On laparotomy, a huge left ovarian tumour of 30x25x10cm was found. The right ovary was streaky [Table/Fig-3]. There was minimal ascites and enlargement of para aortic lymph nodes. Left Salphingo oophorectomy, pelvic lymphadenectomy, left para aortic lymph node excision, infra–colic omentectomy and right ovarian wedge biopsy was done. Histopathology revealed the presence of predominantly dysgerminoma [Table/Fig-4] and also the presence of gonadoblastoma consisting of nests of intimately admixed germ cells and sex cord stromal derivatives, resembling immature Sertoli/Leydig cells and granulosa cells [Table/Fig-5 & 6]. The granulosa cells formed Call Exner like hyaline bodies [Table/Fig-7]. The germ cell components were similar to dysgerminoma with large, round vesicular nuclei, prominent nucleoli and clear cytoplasm.
Left ovarian Tumour, Right streak ovary with the uterus
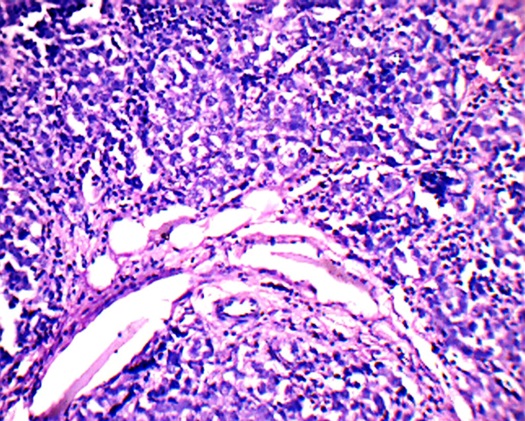
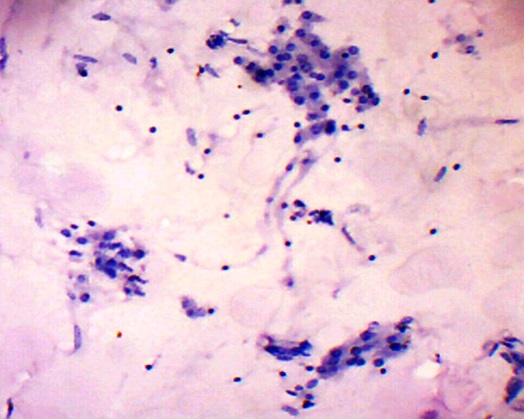
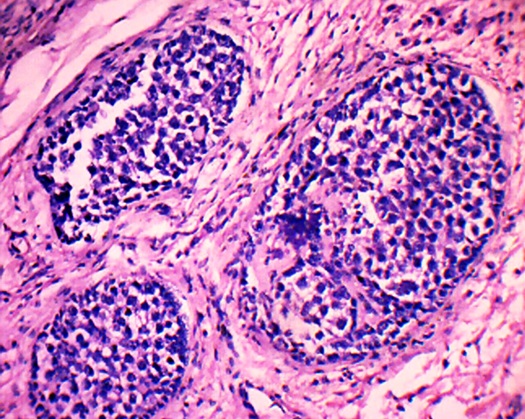
Granulosa with Call Exner bodies
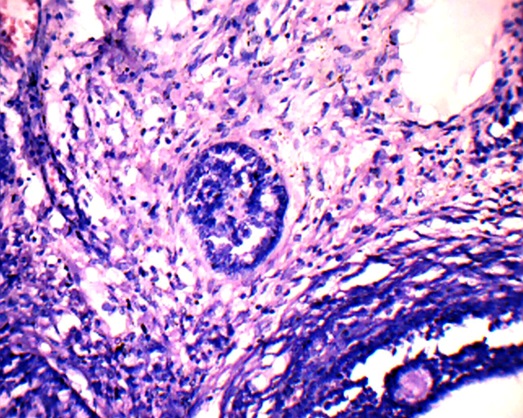
Our patient received combination chemotherapy and the levels of beta hCG, LDH and testosterone reduced after surgery and chemotherapy and her menstrual cycles became regular. Hirsutism reduced, but the voice change persisted. She is on regular follow up and is doing well after twenty months of surgery. There was no evidence of tumour in the other ovary which was left behind.
Discussion
Gonadoblastomas are unusual mixed germ cell sex cord neoplasms usually occurring in dysgenetic gonads. They are found in 25%–30% of patients with XY gonadal dysgenesis and in 15%–20% of 45X/46XY individuals [5]. Only a very small fraction of gonadoblastomas develop in 46XX females with no evidence of Y chromosome. Around 80% of the patients with ovarian gonadoblastoma are phenotypic females and majority of them are virilised. Gonadoblastoma tissue can produce both testosterone and oestrogen. Virilisation is due to the ectopic steroid hormone production by the tumour and it disappears after radical excision of the tumour [3]. This happened in our case too.
In its typical presentation, a pure gonadoblastoma is a small tumour. Considerable size variation has been described with diameters varying from those beyond detection by naked eye up to 8 cm [3]. Esin et al., reported a case of gonadoblasotma of 0.5 cm and stated it to be the smallest in a 46 XX patient [2]. When gonadoblastoma is replaced by a malignant germ cell tumour, it may reach huge dimensions [1]. In our case, the tumour was large due to the overgrowth of dysgerminoma.
The tumour is composed of germ cells and also sex cord stromal derivatives resembling granulosa and Sertoli cells. Sometimes these tumours contain stromal elements indistinguishable from lutein or Leydig cells [1]. This basic histology of gonadoblastoma may be altered and distorted by hyalinization, calcification (81%) and overgrowth by dysgerminoma (50%) [6].
Esin S et al., in their literature search from pubmed, reported 7 cases of gonadoblastoma in women with normal karyotype from 1990 to 2007 including their case. All cases were in young females, the youngest being 10 years old and the oldest 27. All had coexisting germ cell tumour, being common dysgerminoma [2]. Gonadoblastomas have been described in pregnant women too. [6,7] Germ cell tumours frequently produce serum markers such as hCG, LDH and AFP. Elevated serum hCG levels are present in 3% of dysgerminomas [8]. The peptide hormones inhibin and Antimullerian Hormone (AMH) both produced by the granulosa cells are potential candidates for diagnosis and follow up of granulosa cell tumours [9].
Our patient was 14 years old and is the second youngest to be reported with the largest tumour. She also presented with high hCG values probably from the associated germ cell tumour. Antimullerian hormone and inhibin were not done in our patient as presence of sex cord stromal derivatives was not suspected.
Yilmaz et al., described bilateral gonadoblastoma with dysgerminoma in a 20–years–old girl who was managed with bilateral salphingo-oophorectomy followed by chemotherapy. The patient was free of disease five years after initial therapy [10].
Prognosis of pure gonadoblastoma and when associated with dysgerminoma is excellent [11]. Presence of other germ Cell tumours like yolk sac tumour makes the prognosis unfavourable. Chemotherapy may be needed after surgery. Obata et al., described a 10–years–old girl with 46XX karyotype with bilateral gonadoblastoma coexistant with dysgerminoma on one side and dysgerminoma and yolk sac tumor on the other side [12]. Their patient received 10 courses of chemotherapy and was free of relapse after 2 years of surgery. Erdemoglu and Ozen described a pure endodermal sinus tumor and dysgerminoma in a 19–years–old 46 XX female which measured 25x22x20 cm. who underwent fertility conserving surgery, did not receive any chemotherapy and was doing fine after six months of surgery [13].
For patients with dysgenetic gonads, bilateral oophorectomy and hysterectomy are recommended. In cases with a 46 XX karyotype, the necessity of bilateral gonadectomy is less clear and rareness of the situation makes it difficult to decide the appropriate treatment [2].
In our case, a wedge biopsy of the other ovary which was streaky did not show the presence of tumour, hence we did not remove the other ovary. This may be helpful in young women to conserve fertility. FISH or PCR in peripheral blood or from excised tumour could be done to detect low grade mosaicism. This was not done in our case due to lack of facility.
To conclude, the significance of this report is that it describes the very rare case of gonadoblastoma in phenotypically and cytogenetically normal menstruating women. Occurrence of gonadoblastoma in abnormal gonads may not be the absolute rule. More and more cases are being reported in phenotypically and genotypically normal females. Conservative surgery by retaining the other ovary may be helpful to preserve the future reproductive function of the lady.
[1]. Scully RE, Gonadoblastoma – a review of 74 casesCancer 1970 25:1340-56. [Google Scholar]
[2]. Esin S, Baser E, Kucukozkan T, Magden HA, Ovarian gonadoblastoma with dysgerminoma in a 15-year-old girl with 46, XX karyotype: case report and review of the literatureArch Gyanecol Obstet 2012 285:447-51. [Google Scholar]
[3]. Syrjanen KJ, Erzen M, Ovarian gonadoblastoma and related tumours: classification, histopathology and cellular sources of hormone productionCME Journal gyneconcol 2004 9:13-25. [Google Scholar]
[4]. Gelincik I, Ozen S, Bayram I, Left ovarian gonadoblastoma with yolk sac tumour in a young womanIndian j pathol microbial 2010 53(2):345-46. [Google Scholar]
[5]. Kim MJ, Ahn HJ, Kim JY, Kim KR, Gonadoblastoma Overgrown by Dysgerminoma in Women with 46,XX Karyotype – A Report of Two CasesKorean J Pathol 2003 37:66-70. [Google Scholar]
[6]. Erhan Y, Toprak AS, Ozdemir N, Tiras B, Gonadoblastoma and fertilityJ Clin Pathol 1992 45(9):828-29. [Google Scholar]
[7]. Gorosito M, Pancera B, Sarancone S, Nocito AL, Gonadoblastoma: an unusual ovarian tumourAnn Diagn Pathol 2010 14(4):247-50. [Google Scholar]
[8]. Scully R, Young R, Clement R, Tumors of the ovary, mal-developed gonads, fallopian tube, and broad ligament, 1998; fasicle 23Atlas of tumour pathologyvol 3Washington, DCArmed Forces Institute of Pathology [Google Scholar]
[9]. Geerts I, Vergote I, Neven P, Billen J, The role of inhibins B and antimullerian hormone for diagnosis and follow-up of granulosa cell tumoursInt J Gynecol Cancer 2009 19(5):847-55. [Google Scholar]
[10]. Yilmaz B, Gungor T, Bayramoglu H, Soysal S, Mollamahmutoglu L, Bilateral ovarian gonadoblastoma with coexisting dysgerminoma in a girl with 46, XX karyotypeJ Obstet Gynaecol Res 2010 36(3):697-700. [Google Scholar]
[11]. Kurman RJ, Blaustein’s pathology of the female genital tract 2011 6th ednNew YorkSpringer [Google Scholar]
[12]. Obata NH, Nakashima N, Kawai M, Kikkawa F, Mamba S, Tomoda Y, Gonadoblastoma with Dysgerminoma in One Ovary and Gonadoblastoma with Dysgerminoma and Yolk Sac Tumor in the Contralateral Ovary in a Girl with 46XX KaryotypeGynecol Oncol 1995 58:124-28. [Google Scholar]
[13]. Erdemoglu E, Ozen S, Ovarian gonadoblastoma with yolk sac tumour in a young 46, XX female: case reportEur J Gynacec Oncol 2007 6:0392-2936. [Google Scholar]