An isolated fallopian tube torsion is a rare, often difficult to diagnose, but significant cause of acute lower abdominal pain in women of the reproductive age group. It is rare in the perimenopausal age group. We are presenting a literature review and the case of a 47 years old woman who presented with a sudden onset of acute lower abdominal
pain . Her clinical examination revealed an 8x8 cm, tender, cystic mass in the left lower quadrant, with positive cervical movement tenderness. MRI revealed a gross hydrosalpinx with a small left ovarian cyst. With a diagnosis of left adnexal torsion, an emergency laparotomy was performed, which revealed an isolated left fallopian
tube torsion which necessitated a left salpingo-oophorectomy. A tubal torsion should be suspected in females with acute lower abdominal pain, of any age group, especially in those with predisposing
factors like pelvic infections, tumours and surgeries which include tubal ligation. Laparoscopy is the preferred modality for the diagnosis and treatment of a tubal torsion.
INTRODUCTION
An isolated torsion of the fallopian tube is extremely rare, which occurs in 1 in 1.5 million women [1]. The first case of tubal torsion was described by Bland-Sutton in 1890 [2]. It is seen in the reproductive age group of 21-40 years [3] and rarely in the perimenopausal age group [1, 4, 5].
This condition is rarely diagnosed preoperatively and by the time a surgery is undertaken, the affected adnexa is usually damaged. Making a differential diagnosis between an adnexal and a tubal torsion is very difficult. A definitive diagnosis is always made after a laparoscopic or a surgical exploration. An early diagnosis and treatment is required to prevent complications.
CASE REPORT
A 47 year old perimenopausal woman presented with an acute onset of pain in the lower abdominal quadrant of 3 days duration, which was of a moderate degree, gradually progressive, colicky in nature and non-radiating. There were no other symptoms. She was Para 2 living 2, both being normal vaginal deliveries. Her menstrual cycles were regular. She had undergone a bilateral tubal ligation 15 years ago. She had no other significant past medical and surgical histories.
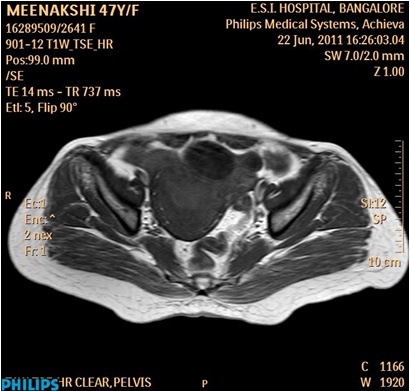
On examination, the patient was found to be conscious and oriented and with stable vital signs. Her abdominal examination revealed tenderness in the suprapubic, left lumbar and the iliac fossa regions without a rebound tenderness or guarding. A mobile, tender, cystic mass with an irregular surface, which measured about 8x8 cm, was felt in the left lower quadrant of the abdomen. All the borders of the mass could be felt, except the lower one. Her vaginal examination revealed that the tender mass was in the anterior and the left fornix, which was different from the uterus. Cervical motion tenderness was present. A provisional diagnosis of a left adnexal torsion was made. On investigating, ultrasound of the abdomen revealed a convoluted complex cystic mass in the left adnexal region. All the haematological parameters were normal, except for ESR, which was raised. Her urine pregnancy test was negative and CA-125 was normal. As the patient’s general condition was stable, an MRI was done, which revealed a gross, left sided hydrosalpinx of a maximum diameter of 3.4 cm and a small, left haemorrhagic ovarian cyst of 3.7x2.9cm with a bulky uterus and with minimal free fluid in the POD [Table/Fig-1].
MRI of abdomen and pelvis showing left sided hydrosalpinx and ovarian cyst.
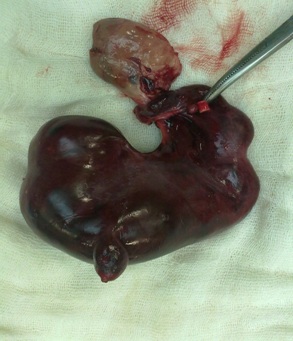
On the next day, as the patient’s general condition worsened, an emergency exploratory laparotomy was done. On table, the findings were as follows:A grossly enlarged, necrotic, left fallopian tube which measured 4x10 cm, with haemorrhagic contents was twisted on its own axis (three times), distal to the site of ligation of the tube. The uterus was bulky, with a normal right ovary and an elongated fallopian tube. The left haemorrhagic ovarian cyst of 3x4 cm was adherent to the left tube. A left salpingo-oophorectomy was done and it was sent for a histopathological examination (which was consistent with the fallopian tube with haemorrhage and the ovary-corpus haemorrhagicans) [Table/Fig-2]. The postoperative period was uneventful.
Left hematosalpinx with torsion and ovarian cyst.
DISCUSSION
An isolated torsion of the fallopian tube may occur in the reproductive age group, which is rare in the premenarcheal [6], perimenopausal [1, 5, 6] or in the menopausal age groups [3, 4, 7]. This variation is because, most of the risk factors for tubal torsion occur in the reproductive age group [1]. Its incidence is 1 in 1.5 million women [1, 7]. The diagnosis is difficult pre-operatively, due to a lack of pathognomonic clinical and imaging findings.
The exact cause of this torsion is unknown. Regad [7] surveyed 201 cases of fallopian tube torsion and found a normal appearance in only 24% cases. Youssef et al., [7] classified the causes of tubal torsion as extrinsic and intrinsic [Table/Fig-3] [1, 7, 8].
Causes of fallopian tube torsion.
| Intrinsic | Extrinsic |
|---|
| 1. Congenital tubal anomalies: Excessive length and tortuosity of the tube/mesosalpinx, hydatids of Morgagni | 1. Changes in the neighbouring organs: Tumors of the ovary or paraovaian, omental or other adhesions to part of the tube, uterine enlargement by pregnancy or tumor. |
| 2. Acquired pathology: Hydro/hematosalpinx, tubal neoplasms, tubal surgery (tubal ligation). | 2. Mechanical factors: Movements and contractions of the neighbouring hollow viscus, sudden body position changes(Sellheim theory), or trauma to the abdominal wall. |
| 3. Physiological abnormalities: Autonomic dysfunction and abnormal peristalsis of the fallopian tube, tubal spasm. | 3. Haemodynamic abnormalities: Pelvic venous congestion at the time of ovulation or premenstrual period. |
The mechanism of tubal torsion: [1], [7–10] In the presence of 732predisposing factors, the adnexal veins and the lymphatic vessel are prone to a mechanical blockage, leading to a local oedema and a pelvic congestion. The subsequent enlargement of the adnexa predisposes to a partial or a complete torsion, along with the formation of a hydrosalpinx [1, 9, 10]. If there is an associated compromise in the arterial supply, it leads to a haemorrhagic infarction and a haematosalpinx [1, 5, 11, 12]. Rarely, does autoamputation of the tube [13] occur.
The torsion of the fallopian tube is usually unilateral and it occurs most commonly on the right side. This may be due to the presence of the sigmoid colon on the left side (it prevents the adnexal movement) [1] or the slow venous flow on the right side (this results in congestion) [8].
In our case, the underlying cause of the tubal torsion with the haematosalpinx was unclear. The possible causes are elongated tubes, a prior tubal ligation, an associated ovarian cyst and pelvic adhesions [1, 5, 7, 8, 12]. This case was unusual, as it was a rare presentation of a tubal torsion on the left side, which occurred in the perimenopausal age group.
The clinical presentation: [1, 8, 10] Commonly, the patients present with a sudden onset of lower abdominal pain which is colicky in nature, which often radiates to the flank or thigh. On pelvic examination, a tender adnexal mass may be present, with a positive cervical motion tenderness . The laboratory studies are usually within the normal range.
The imaging findings in torsion are non-specific and a clinical correlation is very important. Ultrasound [3, 4, 10] may reveal an elongated, convoluted, cystic mass which tapers as it nears the uterine cornu, with the typical beads-on-a string sign [14] and demonstration of the ipsilateral ovary as separate from the mass. Doppler may be helpful and it shows a high impedence or the absence or reversal of the diastolic flow (obstruction to the blood flow in a mesosalpinx) in a tubular structure, especially that in one with a history of tubal ligation can be indicative of a diagnosis [10]. A whirlpool sign may be specific of a tubal torsion, if it is elicited. Because of the dual blood supply, the presence of the blood flow in the Doppler may not exclude the torsion [14]. MRI may add useful information by suggesting the bloody nature of the tubal contents [14] and it may depict the haemorrhage as related to an irreversible disease.
The differential diagnosis of tubal torsion includes both gynaecological and non gynaecological conditions [1, 4, 5]. The gynaecological conditions include torsion or rupture of the ovarian cysts, PID, ectopic pregnancies and ruptured corpus luteal cysts. The non-gynaecological causes include appendicitis, cystitis, biliary/ renal colic, perforation of the hollow viscus, intestinal obstruction, mesenteric lymphadenitis and strangulated hernias.
Management [1, 4, 7, 8, 14]: Laparoscopy is the gold standard procedure for both the diagnosis and the treatment of tubal torsions. However, a surgery (laparotomy) is often performed. A patient with a tubal torsion without any ischaemic damage can be successfully treated by laparoscopic tubal detorsion (which is preferred in the reproductive age group) [1, 7]. If the tube is gangrenous, a malignancy can be suspected and if the tube is diseased or if the patient has completed her family [7], a laparoscopic salpingectomy is preferred.
CONCLUSION
Fallopian tube torsion is rare in perimenopausal women, but it should be included in the differential diagnosis of an acute lower abdominal pain in women, especially in those with predisposing factors. An early diagnosis and an early intervention can maximize the tubal salvage. Laparoscopy remains the gold standard for the same.
[1]. Shukla R, Isolated torsion of the hydrosalpinx: a rare presentationBr J Radiol 2004 77:784-86. [Google Scholar]
[2]. Bland-Sutton T, Salpingitis and some of its effectsLancet 1890 2:1146 [Google Scholar]
[3]. Masroor I, Khan N, Torsion of fallopian tube,fimbrial cystJ Pak Med Assoc 2008 58:571-73. [Google Scholar]
[4]. Samiee H, Asgari Z, Mahdavi A, Khoshideh M, Taslimi S, Karimi M, Isolated fallopian tube torsion:A case report and review of literatureJournal of Family and Reproductive Health 2010 4:87-89. [Google Scholar]
[5]. Malhotra V, Dahiya K, Nanda S, Malhotra N, Isolated torsion of the fallopian tube in a perimenopausal woman: A rare entityJournal of Gynecologic Surgery 2012 28:31-33. [Google Scholar]
[6]. Goktolga U, Ceyhan T, Ozturk H, Gungor S, Isolated torsion of fallopian tube in a premenarchal 12-year-old girlJ. Obstet Gynaecol Res 2007 33:215-17. [Google Scholar]
[7]. Krissi H, Shalev J, Hava IB, Langer R, Herman A, Kalpana B, Fallopian Tube Torsion: Laparoscopic Evaluation and Treatment of a Rare Gynecological EntityJ. Am Board Fam Med 2001 14:274-77. [Google Scholar]
[8]. Krissi H, Orvieto R, Dicker D, Dekel A, Rafael ZB, Torsion of a fallopian tube following Pomeroy tubal ligation:a rare case report and review of literatureEuropean Journal of Obstetrics and Gynecology and Reproductive Biology 1997 72:107-09. [Google Scholar]
[9]. Bernardus RE, Vander Slikke JW, Roex AJ, Dijkhuizen GH, Stolk JG, Torsion of the fallopian tube ;some considerations on its etiologyObstet Gynecol 1984 64:675-78. [Google Scholar]
[10]. Bertolotto M, Serafini G, Toma P, Zappetti R, Migaleddu V, Adnexal torsionUltrasound Clin 2008 3:109-19. [Google Scholar]
[11]. Furui T, Imai A, Yokoyama Y, Tamaya T, Hematosalpinx and torsion of the fallopian tube in a virgin girlGynecol Obstet Invest 1993 35:123-25. [Google Scholar]
[12]. Fallopian tube torsion and hematosalpinx in a menopausal womanEur J. Obstet and Gynec and Reproductive Biology 2008 140:276-77. [Google Scholar]
[13]. Sankaran S, Shahid A, Odejinmi F, Autoamputation of the fallopian tube after chronic adnexal torsionJournal of Minimally Invasive Gynecology 2009 16:219-21. [Google Scholar]
[14]. Coudray AJ, Naggara IT, Chereau E, Rouzier R, Darai E, Bazot M, A case of isolated torsion of the fallopian tube: an added value of magnetic resonance imagingEuropean Journal of Radiology Extra 2011 79:e1-e4. [Google Scholar]