The drug utilization research is increasing and it is being carried out in health setups, in order to study the use of drugs in a society. This has immense medical social and economic consequences. Drug utilization studies are needed to identify the trends as well as to set the priorities, not only in the interest of the regulatory control, but also as a basis of the planning program of education and information [1].
It has been proved that cardiovascular diseases are the most frequent cause of morbidity and mortality throughout the world [2,3]. The risk of cardiovascular diseases is being frequently monitored. But the studies on inpatients are rare and incomplete [4]. Hence, we decided to do a drug utilization study on cardiovascular emergencies. A prescription based survey is considered to be one of the most effective methods which have been used to assess and evaluate the prescribing attitude of physicians [4,5]. Therefore, that was the method which we adopted for this study.
METHODS
Prior approval from the institutional ethical committee was obtained to undertake the present study. Permission from the concerned authorities of the Department of Medicine was also obtained for the data collection. This study was undertaken to determine the drug utilization trends in cardiovascular emergencies. It was conducted in the Department of Medicine in a government hospital which was attached to the Government Medical College, Miraj, India. An attempt was also made to associate the prescription data with the age, sex, diagnosis and the investigations.
During the period of the study (four months), two hundred and forty three (243) patients were studied, who were admitted into the Intensive Care Unit (ICU) of the Department of Medicine as cardiovascular emergency cases. Their data was collected regularly from the ICU and then from the General Ward of Medicine, without interfering with their treatment.
The age, sex, diagnosis (only cardiovascular) and the drugs which were prescribed were recorded for each patient. Also, the brand names and the generic names of the prescribed drugs were noted. The collected data was analyzed to study-
The drug utilization trends.
Quantitatively, the drug utilization in terms of the DDD and the prescribing prevalence.
The most common cardiovascular emergencies which were treated.
The outcome of each patient with a cardiovascular emergency until discharge.
Correlation of the clinical outcome with the treatment. i.e. the protocol which was followed in the hospital for the cardiovascular emergencies was in accordance with the guidelines which were described in the standard literatures [2].
The collected data was used to find the prescribing indicators [6] like.
The average no. of drugs per prescription.
The percentages of the drugs which were prescribed by their generic names.
The percentages of the drugs with antibiotics which were prescribed.
The percentages of the drugs with injections prescribed.
The percentages of the drugs which were prescribed from the essential drugs list or the formulary.
As the patients were admitted to the ICU, followed by the ward, the drugs which were administered to the patients were directed by supervised nursing staff. Hence, patient care indicators [6] like the average consultation time, the average dispensing time, the percentages of the drugs which were actually dispensed, the percentages of the drugs which were adequately labelled and the patients' knowledge on the correct dosage, were not considered.
The quantification of the drugs which were used was done by using the Anatomical Therapeutic Chemical (ATC) classification and the Defined Daily Dose (DDD) system. The Defined Daily Dose (DDD) concept was developed to overcome the objection against the traditional units of the measurements of the drug consumption [7,8]. The DDD for a given drug was established on the basis of the assumed average use per day of the drug which was used for its main indication in an adult. It is expressed as DDD per thousand persons per day (DDD/1000/day) and it provides a rough estimation of the consumption.
The results which were obtained were expressed in terms of the DDD /1000 persons/day [4,8]. The DDD/1000 persons/ day is expressed as follows [8].
Total no. of dosage units prescribed
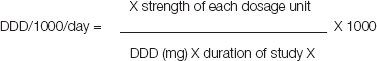
total sample size.
The prescribing prevalence of the individual drugs was also calculated and expressed in terms of the percentage of the prescribing frequency.
Prescribing prevalence of No. of prescriptions for that drug

Prescriptions were considered as the written orders for the drugs which were given by the doctor for one day in the patients' case paper records.
Exclusion Criteria
The patients who died or were discharged against medical advice within 24 hours of their admission were excluded in this drug utilization study.
RESULTS
In the present study, we recorded the drug treatment which was received by the patients with cardiovascular emergencies. The total number of patients was two hundred and forty three (243). Outof these 243 patients, 129 (53.1%) had myocardial infarction, 96 (39.5%) patients suffered from ischaemic heart disease and the incidence of arrhythmias of various types was (7.4%). It was also seen that males (64.43%) had a higher incidence of cardiovascular emergencies than females (34.57%) [Table/Fig-1].
| Age group | I.H.D | M.I. | Cardiac Arrhythmia | Total | Percentage |
|---|
| M | F | M | F | M | F | M | F | M | F |
|---|
| 31-40 | 6 | 6 | 3 | 0 | 3 | 0 | 12 | 6 | 4.93 | 2.46 |
| 41-50 | 12 | 3 | 24 | 3 | 0 | 3 | 36 | 9 | 14.81 | 3.7 |
| 51-60 | 15 | 3 | 15 | 9 | 3 | 0 | 33 | 12 | 13.58 | 4.93 |
| 61-70 | 15 | 18 | 30 | 30 | 3 | 6 | 48 | 54 | 19.75 | 22.22 |
| 71-80 | 12 | 0 | 9 | 0 | 0 | 0 | 21 | 0 | 8.64 | 0 |
| 81-90 | 6 | 0 | 3 | 0 | 0 | 0 | 9 | 0 | 3.7 | 0 |
| 91-100 | 0 | 0 | 0 | 3 | 0 | 0 | 0 | 3 | 0 | 1.234 |
| Total | 66 | 30 | 84 | 45 | 9 | 9 | 159 | 84 | 65.43 | 34.57 |
| Percentage | 27.16 | 12.34 | 34.56 | 18.51 | 3.7 | 3.7 | 65.43 | 34.57 | | |
(Note: IHD ischemic heart disease, M.I.-myocardial infarction, M-male, F-female)
[Table/Fig-1] also shows that the incidence of cardiovascular emergencies was higher in the patients of the age group of 61-70 years (102 out of 243). In the ages in between 51-70 years, the incidence of cardiovascular emergencies was found to be nearly equal in both males (81 out of 243) and females (66 out of 243). The incidence of cardiovascular emergencies was less in females in the age group of 31-50 years (5.53%) than in the age group of 51-70 years (27.15%). [Table/Fig-2] shows that hypertension (46.91%) was the most common associated disease in cardiovascular emergencies. It was also the most common risk factor for cardiovascular morbidity & mortality.
Information about the associated disease
| Associated Disease→ | HTN | DM | CCF | IHD | LVF | SVT | Br. Asthma | TIA |
|---|
| Emergencies ↓ |
|---|
| Myocardial infarction | 48 | 18 | 9 | 21 | 12 | 0 | 6 | 0 |
| Ischemic heart disease | 54 | 15 | 12 | 0 | 9 | 6 | 0 | 3 |
| Arrhythmia | 12 | 3 | 9 | 3 | 0 | 0 | 0 | 0 |
| Total | 114 | 36 | 3 | 24 | 21 | 6 | 6 | 3 |
| Percentage | 46.91 | 14.81 | 12.34 | 9.87 | 8.64 | 2.46 | 2.46 | 1.23 |
(Note: HTN- hypertension, DM-Diabetes mellitus, CCF- congestive cardiac failure, IHD-ischemic heart disease, LVF-left ventricular failure, SVT-Supra ventricular tachycardia, Br. Asthma-bronchial asthma, TIA-Transient ischemic attack)
In this present study, a total of 61 drugs was prescribed, out of which 29 drugs were prescribed for cardiovascular diseases, while 17 drugs were antibiotics, in 1410 prescriptions. The average no of drugs which was prescribed was 9 per prescription. We also observed that out of 61 drugs, nearly 46% of the drugs i.e. 28 were prescribed by their generic names. A total of 88% prescriptions contained injectable drugs. Of the 29 drugs which were prescribed for cardiovascular diseases, 17 relevant drugs were compared.
[Table/Fig-3] shows that Isosorbide Dinitrate was most commonly prescribed (91.90%), followed by Aspirin (90.21%) and Clopidogrel (80.85%). In the group of Angiotensin Converting Enzyme inhibitors, Enalapril was prescribed regularly (37.87%). HMG CoA reductase inhibitors (Atorvastatin) were prescribed (52.76%) more as compared to ACE inhibitors (38.93%) and ?blockers (Metoprolol and Atenolol) (25.53%). The least commonly prescribed drug was Prazosin (ά blocker) 0.42%.
Percentage prescribing prevalence and DDD/1000/Day
| Drugs | ATC Classification | No. of prescriptions | Percentage prescribing prevalence | DDD | Observed DDD/1000/Day | Expected DDD/1000/Day |
|---|
| Isosorbiddinitrate | C01DA08 | 1296 | 91.91 | 60 mg O | 22.456 | 44.019* |
| Glyceryltrinitrate | C01DA02 | 21 | 1.489 | 5 mg P | 4.553 | 0.7083* |
| Aspirin | B01AC06 | 1272 | 90.21 | 1 tab O | 55.153 | 42.906 |
| Clopidogrel | B01AC04 | 1140 | 80.85 | 75 mg O | 56.769 | 39.668* |
| Dalteparin | B01AB04 | 783 | 55.53 | 2.5IU P | 105.241 | 25.602* |
| Enalapril | C09AA02 | 534 | 37.87 | 10 mg O | 6.327 | 17.70* |
| Metoprolol (O) | C07AB02 | 201 | 14.255 | 0.15 gm O | 3.272 | 10.1194* |
| Amlodipine | C08CA01 | 90 | 6.382 | 5 mg O | 4.857 | 3.137 |
| Atenolol | C07AB03 | 159 | 11.27 | 75 mg O | 2.158 | 5.262* |
| Digoxin (P) | C01AA05 | 63 | 4.468 | 0.25 mg P | 2.226 | 2.023 |
| Digoxin(O) | C01AA05 | 39 | 2.765 | 0.25 mg O | 1.214 | 1.124 |
| Furosemide (O) | C03CA01 | 93 | 6.595 | 40 mg O | 4.857 | 2.9346 |
| Furosemide(P) | C03CA01 | 507 | 35.955 | 40 mg P | 0.379 | 11.030* |
| Amiodarone | C01BD01 | 105 | 6.595 | 0.2 gm O | 10.625 | 0.7083* |
| Atorvastatin | C10AA05 | 744 | 52.76 | 10 mg O | 25.602 | 23.9829 |
| streptokinase | B01AD01 | 51 | 3.617 | 1.5 MU P | 0.1619 | 0.2023 |
| Prazosin | C02CA01 | 6 | 0.425 | 5 mg O | 0.303 | 1.6191* |
(Note: O=oral, P-parenteral ATC -Anatomical Therapeutic Classification *- statistically significant p< 0.5 %
From the same table, it is also clear that the DDD/1000/day of Dalteparin (105.24) was the highest. Aspirin (55.15) and Clopidogrel (56.76) were most commonly used. The drug consumption rate of diuretics (5.22) nitrates (27.00) and statins (25.60) was nearly equal.
DISCUSSION
From the above observations, we could see that 9 drugs per prescription were justifiable, as they were prescribed for cardiovascular emergencies. It was also observed that 75% of the drugs which were used, out of the 61 drugs, were from the essential drug list [9]. As the expected no. of drugs which was prescribed per patient and the injectable prescriptions which were used were high because they were used in emergencies, these therapies require multidrug prescriptions.
There are some drugs which should be always given by the injectable route of administration, like Adrenaline, Dalteparin, Heparin, Streptokinase and Pethidine, etc in emergencies. As nearly 75% of the drugs were from the essential drug list, this may be one of the reasons for getting good outcomes.
The prescription of the drugs was expressed as both DDD/1000/day and prescribing prevalence. The DDD methodology does not indicate the exact number of patients who have been treated with drugs. This concept assumes that every person who is prescribed a particular drug is taking the specific DDD every day, ignoring the alteration of the dosage for each disease and the patient related factors. The variations in the dosage pattern, the duration of the study, the scattering of the population over different age groups, etc. can therefore contribute to the difference in the audit report, with the use of the DDD methodology to determine the prevalence of the prescriptions [7,8,10].
After comparing the drugs under the parameter of the observed and expected DDD/1000/days, it was observed that there were some drugs like Digoxin, Atenolol, Atorvastatin, Furosemide and Streptokinase which did not show any significant difference. Other drugs like nitrates, Daltaparin, Amlodipine, Amiodarone, and Prazosin, showed a significant difference in the utilization study.
The expected DDD/1000/days was calculated, based on the prevalent guidelines of the WHO, assuming that these guidelines were followed scrupulously [7]. Thus, the significant difference indicated a guideline incongruent prescribing behaviour, which was statistically significant.
It was observed that the most common cardiovascular emergencies which had to be treated were myocardial infarction and ischaemic heart disease. It was also seen that these emergencies were more common in males than in females, before the age of 50 years but after the age of 50 years, this disparity was not seen and the incidences were nearly equal in both. Here, we also noted that most of the patients of cardiovascular emergencies had preceding associated diseases like Diabetes mellitus and hypertension.
The reasons for these incidences of the above two emergencies are multifactorial. Some of these high risk factors included a high fatty and energy rich diet, smoking, alcoholism and a sedentary life style, in addition to associated risk factors like obesity, insulin resistance and type 2 Diabetes mellitus [2,11].
The utilization of nitrates, anticoagulants, antiplatelet agents and hypolipidaemic drugs was high and it is in accordance with the standard guidelines which were mentioned for the treatment of such emergencies. The use of the ACE-inhibitors was higher than that of the ?-blockers and the calcium channel blockers. This was for keeping up with the increased use of ACE-inhibitors because of their beneficial effect on the morbidity and mortality in myocardial infarction and ischaemic heart disease patients, even after a long-term use. Also, the ACE-inhibitors had a beneficial effect against fibrosis and cardiac remodelling [12]. These observations correlated with those of various studies like the study of Martinez et al., [13] which showed that an increase in the use of ACE-I and a decrease in the calcium channel blockers were recorded in between 1982-1994. Similarly, our findings correlated with those of other studies like the study of Doubeni et al., [14].
The only lacuna was the relatively low use of the β-blockers though they had a higher beneficial effect in the prevention of events like myocardial infarction. Therefore, it may be necessary to increase the prescription of the ?-blockers further.
CONCLUSIONS
In conclusion, the protocol of the management which was followed by the college in the treatment of cardiovascular emergencies was competent enough, as the clinical outcome of the patients was favourable. 100% patients of arrhythmia and 90% and 96% patients of myocardial infarction and ischaemic heart disease were discharged and followed-up by giving proper treatment. But, there was a guideline incongruent prescribing behaviour which was statistically significant, for which there is a need to conduct a large scale study.
(Note: IHD ischemic heart disease, M.I.-myocardial infarction, M-male, F-female)
(Note: HTN- hypertension, DM-Diabetes mellitus, CCF- congestive cardiac failure, IHD-ischemic heart disease, LVF-left ventricular failure, SVT-Supra ventricular tachycardia, Br. Asthma-bronchial asthma, TIA-Transient ischemic attack)
(Note: O=oral, P-parenteral ATC -Anatomical Therapeutic Classification *- statistically significant p< 0.5 %