A high potency, long acting and/or the extended use of oral corticosteroids, particularly in children, may cause suppression of the hypothalamo-pituitary-adrenal axis. However, the iatrogenic Cushing’s syndrome in the infantile age group is rare and only few patients have been reported to date in the literature. Here, we are reporting a case of iatrogenic Cushing’s syndrome in a 5-month-old male child, whose parents brought him to the hospital for puffiness of the face and overweight.
Infant, Iatrogenic cushing’s syndrome, Oral corticosteroid
INTRODUCTION
Iatrogenic Cushing’s syndrome may occur due to the overuse of potent oral and topical steroids [1–2]. Oral Betamethasone is being prescribed unnecessarily for innocuous conditions like common cold. Ignorant mothers also misuse betamethasone for their babies to make them chubby. These babies develop Cushing’s syndrome, immuno-suppression and serious infections like pneumonia and meningitis. We are reporting a case of iatrogenic Cushing’s syndrome in a 5-month-old infant which had occurred due to the prolonged usage of very high-potent synthetic oral corticosteroid drops (betamethasone dipropionate) which was prescribed irrationally by a quack.
Children have greater risks of systemic side effects of oral steroids as they have significant impact on various metabolisms. For this reason, these products should better not be purchased from the drugstore without a prescription. Also, the information about the usage period and the probable side effects of product should be given to the parents.
CASE REPORT
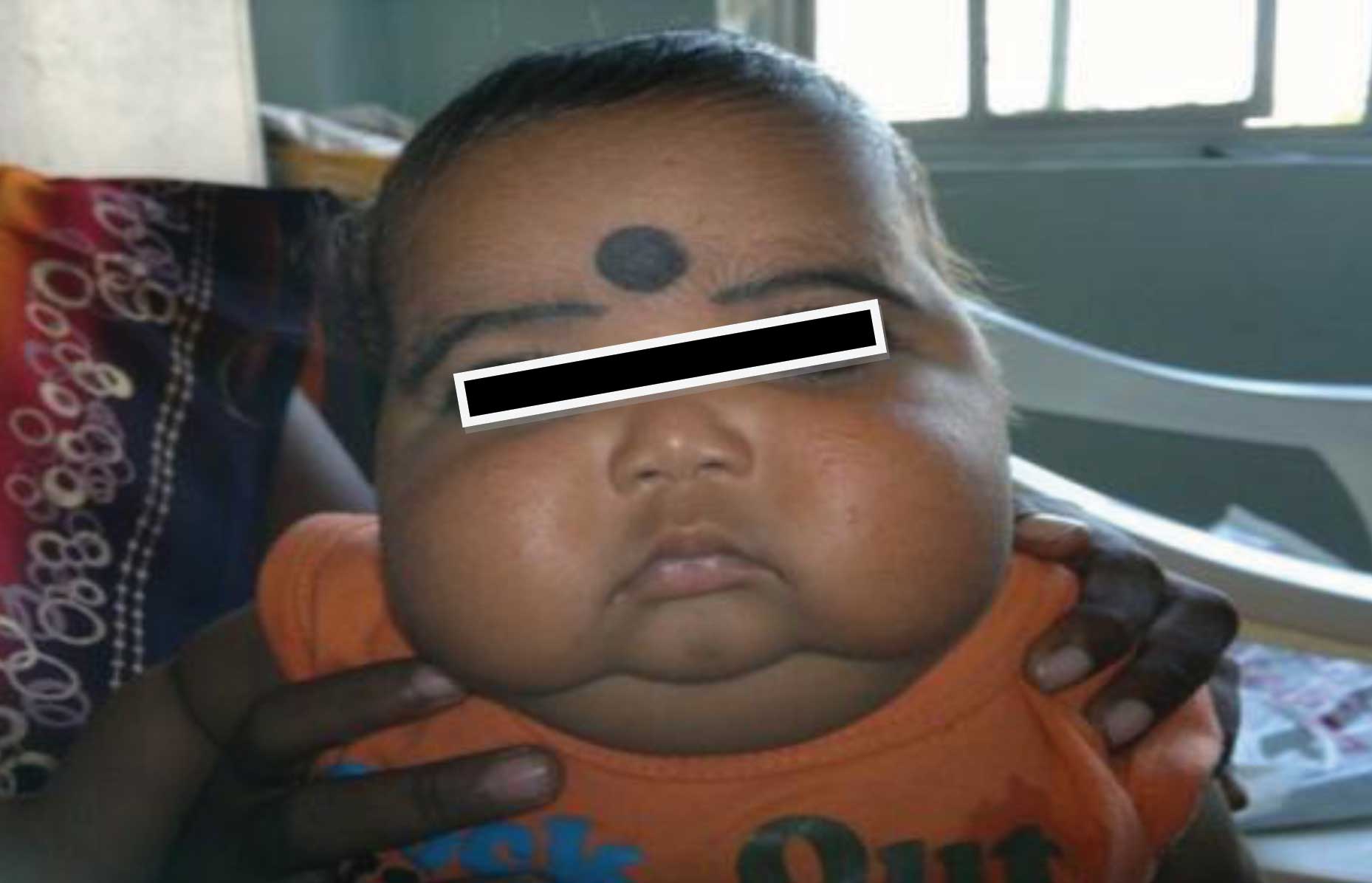
A 5-month-old male child was brought to our hospital with a 3-month history of overweight. His family history revealed that he was the second living child. He had one healthy elder sister who was aged four years. His sister and other members of his family had no similar disease. On physical examination, his blood pressure was found to be 96/60 mmHg (90th-95th centile for height and age) and his heart rate was 94/min. His weight was 6.5 kg (25–50th percentile), his length was 59 cm (<5th percentile), and his head circumference was 41 cm (10–25th percentile). He had Cushingoid facies, truncal obesity, a buffalo hump and paper-thin skin, and crops of fine papules on his face, which were suggestive of steroid acne [Table/Fig-1].
Cushingoid facies of child after 4 months of oral betamethasone drops (note the fine papules of steroid acne over the cheeks)
On laboratory examination – his fasting plasma glucose was found to be 89mg/dL (normal: 70-100mg/dL), his sodium was 139 mEq/L(normal: 130-145mEq/L), his potassium was 4.9 mEq/L (normal: 3.5 – 5.0mEq/L), total cholesterol was 324mg/dL (normal: <170mg/dL), triglycerides were 344mg/dL(normal: <150mg/dL), HDL-C cholesterol was 70mg/dL (normal: > 45mg/dL and LDL-C (low density lipoprotein - cholesterol)- was 185 mg/dL(normal: < 130mg/dL). His morning 8.00 am cortisol level was very low, 0.91 μg/dl(normal: 20 μg/dL).
When his parents were questioned about the details of his history, we learned about the usage of the betamethasone dipropionate oral drops (0.3mg/day equivalent to 7.5mg/day of hydrocortisone or 22mg/m2/day). It was used 2 times in a day (morning and evening) for the past 4 months for cold. This product was purchased from a drugstore with the prescription of quack. The parents were not informed about the period and the possible side effects of the product.
The dose of the steroid was reduced to a physiological dose of 15 mg/m2/day of hydrocortisone and a stress advice was given. We planned to taper off the dose of the steroids by monitoring the 8.00 am cortisol and by checking the recovery of HPA axis periodically.
DISCUSSION
Oral corticosteroids have been ordered extensively in the medical practice by many doctors for various diseases. If the information about their side effects is not given to the parents, the extended use of the high-potency corticosteroids in children may cause severe systemic side effects. The systemic side effects include hypertension, dyslipidaemia, Cushing’s syndrome, hypothalamopituitary- adrenal axis suppression, a failure to thrive, glaucoma, cataract, skin atrophy, striae and a predisposition to bacterial and fungal infections [3].
An extensive and a prolonged misuse of potent steroid preparations in children may cause the suppression of ACTH [4–5]. Puffiness of the face, paper-thin skin with striae, crops of fine papules on the face and hypertension were the positive physical signs of Cushing’s syndrome in our patient. In the present case, Cushing’s syndrome had developed due to an irrational use of a steroid by a quack.
Traditionally, the withdrawal schemes begin by reducing the glucocorticoid incrementally from supraphysiologic to physiologic doses. The physiologic dose is approximately 5 to 7.5 mg a day of prednisone, 15 to 20 mg a day of hydrocortisone, or the equivalent. During this phase of withdrawal, the patients are not at a risk for adrenal insufficiency, nor do most experience the symptoms of the withdrawal syndrome. Therefore, the greatest concern at this time will be exacerbation of the underlying disease. Once a patient is on a replacement dose of glucocorticoid, several approaches can be taken. Many practitioners like to switch to hydrocortisone if possible, in order to take advantage of the short half-life of this medication. This switch may allow the HPA axis more opportunity to recover.
During this stage of withdrawal, it is appropriate to begin checking the morning cortisol levels, which can be useful as a screening test for the basal adrenal sufficiency. A cortisol level which is drawn at approximately 8 a.m. that measures less than 3μg/ dL, indicates a deficient basal cortisol secretion and the need for a continued replacement therapy. If the morning cortisol level is greater than 20μg/dL, the patient can be assumed to have a recovered HPA axis and can be withdrawn entirely from the glucocorticoid therapy [6].
The patients who have cortisol levels that fall between 3 and 20 μg/dL may have sufficient basal cortisol production but they may still be lacking in a sufficient capacity to respond to the significant physiologic stress. In this case, an insulin tolerance test, a CRH stimulation, or an overnight metyrapone test would be reasonable for the assessment of the HPA axis.
For the patients who have been on a long-term glucocorticoid therapy, the risk for an adrenal insufficiency can continue for months. The suppression can be seen for up to 9 months or for even a year. Therefore, the patient and the physician must discuss the potentially prolonged nature of the steroid therapy withdrawal and approach the problem with patience and, sometimes, determination.
The child who has been mentioned above, represents only the tip of the iceberg and a large number of other babies with a steroid usage go undetected. Guidelines for dispensing over the counter steroids are lacking in the developing countries [7]. The irrational prescriptions of steroids as treatment for common cold, both by the practitioners of allopathy and alternative systems of medicine are increasing. Kshirsagar et al., estimated that more than 30% of the prescriptions of the medical practitioners were irrational [8]. Complementary and alternative medicine practitioners, who are untrained medically, prescribe allopathic medicines openly, and even prohibited drugs are available without prescription [9].
Apart from the irrational prescriptions, the health awareness among the general public is also lacking to the extent, that the rapid weight gain which is caused by steroids, which is basically a side effect, is mistaken for good health. As a result, multiple vials of this drug are bought everyday over the counter. In order to reduce this problem, doctors should undergo continuing medical education programs which highlight the harmful effects of steroid misuse. The government can enact stringent laws for restricting the over the counter dispensing of harmful drugs by untrained persons.
[1]. Siklar Z, Bostancı I, Atli Ö, Dallar Y, An infantile Cushing syndrome due to misuse of topical steroidPediatrDermatol. 2004 21:561-63. [Google Scholar]
[2]. Teelucksingh S, Balkaran B, Ganeshmoorthi A, Arthur P, Prolonged childhood Cushing’s syndrome secondary to intralesional triamcinolone acetonideAnn Trop Paediatr. 2002 22:89-91. [Google Scholar]
[3]. West DP, Micali G, Principles of Paediatric Dermatological Therapy. In: Harper J, Oranje A, Prose N, editorsTextbook of Pediatric Dermatology 2000 1stBlackwell Science Ltd:1731-42. [Google Scholar]
[4]. Bertrand J, Saez JM, Adrenal steroids: Biochemistry and Physiology. In: Bertrand J, Rappaport R, Sizonenko PC, editorsPediatric endocrinology 1993 2ndBaltimoreWilliams and Wilkins:283-304. [Google Scholar]
[5]. Allen DB, Safety of inhaled corticosteroids in childrenPediatr Pulmonol. 2002 33:208-20. [Google Scholar]
[6]. Krasner AS, Glucocorticoid-induced adrenal insufficiencyJAMA 1999 282(7):671-76. [Google Scholar]
[7]. Hui JYH, Woo PCY, Lo SS, Chan JCS, Over the counter medication and its effectsLancet 2002 359:1120 [Google Scholar]
[8]. Kshirsagar MJ, Langade D, Patil S, Patki PS, Prescribing patterns among medical practitioners in Pune, IndiaBull World Health Organ 1998 76:271-75. [Google Scholar]
[9]. George R, Abraham R, Private health in IndiaLancet 2002 359:1528 [Google Scholar]