The basic requirement in Fine Needle Aspiration Cytology ( FNAC) is a rapid diagnosis, for which adequate sampling is an essential factor. There is a lot of inordinate delay if the sample adequacy has to be determined after the entire procedure of fixation and staining, which defeats the purpose of the entire procedure. An early assessment of the sample adequacy on unstained smears avoids an undue delay and patient revisits. It also facilitates the selection of the slides for special staining techniques and immunocytochemistry, without having to destain the slides. A naked eye examination helps in the assessment of the sample adequacy when the aspirate is not haemorrhagic. But haemorrhagic and fluid aspirates cannot be assessed for sample adequacy on gross examination. In such cases, an unstained smear examination by using light microscopy is useful. Besides which, the option of choosing a special stain whenever necessary, remains open.
Repeated passes during subsequent visits may induce secondary changes which may interfere with the interpretation. This can be avoided by assessing the sample adequacy during the initial visit.
Materials and Methods
The present study had three groups. Group I included 200 cases with heamorrhagic and fluid aspirates as were observed under a microscope by observer A, a Professor of Pathology with 27 years of experience. Group II included 100 cases out of the 200 cases from Group I, which were observed by observer B, an Assistant Professor of Pathology with 5 years of experience [Table/Fig-1 & 2]. Group III included 80 cases out of the cases from Group II and they were observed by observer C, a junior resident with 2 years of experience in microscopy.
The condensor of the microscope was lowered for the examinations of these unstained smears. The results were compared with assessment of aspirate adequacy on stained smears, analysed statistically and the ‘p’ value was calculated.
Results
200 cases with haemorrhagic and fluid aspirates were included in the study.
Observer A analyzed all the 200 cases in Group I. There were 174 (84%) adequate smears and 26 (13%) inadequate smears among the 200 unstained smears which were seen by Observer A [Table/Fig-3].
Unstained smear from FNA of lymph node 100X, low power)
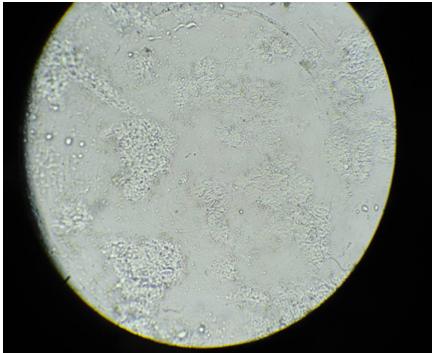
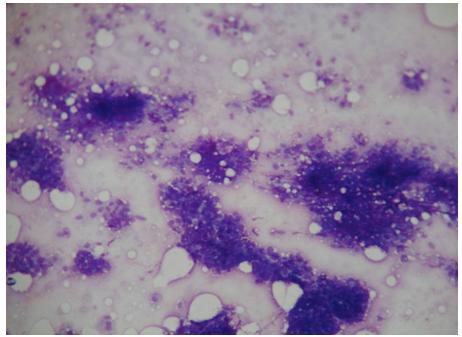
Stained smear of the same aspirate from lymph node (100X, low power)
Results of evaluation of unstained smears of Group I by Observer A compared with stained smears.
| Unstained Smears | Stained Smears-Adequate | Stained Smears-Inadequate |
|---|
| Adequate-174 (87%) | 170(97.7%) | 4(2.3%) |
| Inadequate-26 (13%) | 4(15.4%) | 22(84.6%) |
| Total-200 | 174(87%) | 26(13%) |
Results of evaluation of unstained smears of Group II by Observers A and B compared with stained smears
| Results | Unstained Observer A | Smears Observer B | Stained Smears |
|---|
| Adequate | 82 | 86 | 83 |
| Inadequate | 18 | 14 | 17 |
Results of evaluation of unstained smears of Group III by Observers A, B and C compared with stained smears.
| Result | Un Observer A | Stained Observer B | Smears Observer C | Stained Smears |
|---|
| Adequate | 66 | 62 | 67 | 65 |
| Inadequate | 14 | 18 | 13 | 15 |
| 80 | 80 | 80 | 80 |
Analysis of results of evaluation of unstained and stained Group III smears by Observers A,B and C.
| Observer | Unstained (80) | Stained Smears: Adequate (65) | Stained Smears: Inadequate (15) |
|---|
| A | Adequate: 66 Inadequate: 14 | Adequate: 65 Inadequate:00 | Adequate: 01 Inadequate: 14 |
| B | Adequate: 62 Inadequate: 18 | Adequate: 62 Inadequate:03 | Adequate: 00 Inadequate: 15 |
| C | Adequate: 67 Inadequate: 13 | Adequate: 65 Inadequate:00 | Adequate: 02 Inadequate: 13 |
When these were compared with the stained smears, 170(97.7%) smears proved to have adequate material and 4(2.3%) were found to be falsely positive for adequacy.
Out of the 26 unstained smears which were found to be inadequate, after staining, 22(84.6%) were confirmed as inadequate and 4(15.4%) were found to be falsely negative for adequacy.
The analysis of Group II cases was done by comparing the evaluations of the unstained smears which were done by Observers A and B with those of the stained smears [Table/Fig-4]. Observer A had evaluated 1 smear as falsely negative (inadequate). Observer B had evaluated 3 smears as false positive smears.
The analysis of Group III cases was done by comparing the evaluations of the unstained smears which were done by Observers A, B and C with those of the stained smears [Table/Fig-5 & 6]. Observer A had reported 1 false positive smear and no false negative smear. Observer B had reported no false positive smears, but had reported 3 false negative smears. Observer C had reported 2 false positive smears and no false negative smears.
Observer A had reported 1 false positive smear in which the cellular material was entangled with fibrin. Observer B had reported 3 false negative smears and Observer C had reported 2 false positive smears, probably due to an improper screening.
The statistical analysis revealed a ‘p’ value of <0.001 between the observers and between the stained and unstained smears.
Discussion
Despite being a familiar cytological technique, unstained smear examination has been limited to the examination of urine, semen, vaginal smears and other body fluids [1-3]. A gross examination which is based on the granularity or the particulate nature of the aspirate is sufficient to assess the specimen adequacy in a majority of the cases [4]. However, bloody aspirates may appear to be inadequate on gross evaluation and they may subsequently show adequate material on staining.
Rapid staining methods like Diff-Quik and Toluidine blue stain can be used for preliminary evaluation of the aspirated samples before sending the patient. With Diff-Quik staining, the stain is less intense than the MGG stain. Following Toluidine blue staining, a restaining is necessary. The ultrafast Papanicolaou stain gives a rapid assessment of the FNAs and it offers an excellent cytologic detail.
Very few published studies are available in the literature regarding the efficacy of using unstained smears for evaluating the adequacy of the needle aspirations. Prayaga A.K. and Vijaya K, in their study, found the unstained smear evaluation to be an effective technique for determining the adequacy of needle aspirations. They found no statistically significant difference between the analyses which were done by a consultant and a junior resident [4].
The present study established the fact that the unstained smear evaluation with a reduced illumination under light microscopy, is an effective technique for determining the sample adequacy, even in the hands of a less experienced pathologist. In India, in resource constrained areas and peripheral rural health units, where consultant pathologist services are not available, the referring doctor can be sensitized to assess the adequacy of the sample on unstained smears before dispatching them to the consultant pathologist.
The specific advantage of the technique includes avoidance of the interpretation problems due to tissue reaction, following multiple passes, since aspiration induced artifacts may occur as a consequence of repeated aspirations [5,6]. In addition, undue delay in reporting, which is due to sample inadequacy, is avoided.
Besides these advantages, the option of using the smears for special staining and immunocytochemistry, is retained.
Conclusion
Unstained smear examination is an extremely effective tool in the evaluation of the sample adequacy in cytological smears and it offers specific advantages by way of a rapid diagnosis and avoidance of the inordinate delay which is associated with assessing the sample adequacy after using cytological staining techniques. It is surely worthy of being recommended for the routine practice.