An intrathoracic gossypiboma is a rare condition. We are reporting a case of intrathoracicgossypiboma which was misdiagnosed as a recurrent aspergilloma. In our patient, the gossypiboma manifested as a pleural- based extra pulmonary mass which had a large contact area with the pleura and it displayed an extra pulmonary location. A retained surgical swab (gossypiboma) is a rare but an important complication of an intra- thoracic surgery. The diagnosis is usually overlooked, as in our case, resulting in delay of treatment, complications and a prolonged hospitalization.
Intra-thoracic foreign body, Surgical pack, Bronchopleural fistula, Aspergillum
INTRODUCTION
A gossypiboma or a textiloma is a non-absorbable surgical material with a cotton matrix, around which a foreign body reaction occurs. A retained surgical sponge (gossypiboma) is a rare but a serious complication of surgery, with an estimated incidence in 1/1,000 to 1/10,000 surgeries [1].
An intrathoracic gossypiboma is extremely rare, with only a handful of reported cases, most of which are associated with pulmonary surgeries [1–5]. Almost all the surgical sponges contain a radiopaque marker, usually a barium sulfate filament.The diagnosis of an intrathoracic gossypiboma can be easily missed because of its rare occurrence and low index of suspicion [1].
Here, we are reporting a case of an intrathoracic gossypiboma which was misdiagnosed as a recurrent aspergilloma.
CASE REPORT
A 39 year old, normotensive, nondiabetic, non- smoking, male patient presented to our Out Patients Department with the complaints of persistent cough and haemoptysis which were there since 2007. He was diagnosed of right primary pulmonary tuberculosis in 1999. He had received a course of antituberculous treatment for 6 months. From 2001, he started having dry cough and generalized weakness. On investigation, he was found to have an aspergilloma in the tubercular cavity [Table/Fig-1]. He underwent a right upper lobectomy in Dec 2002. The patient was symptom free for 3 years post-surgery, when he again started having cough with expectoration from 2005. He was treated symptomatically at different hospitals since then, without any relief. Contrast enhanced computerized tomography scans which were done repeatedly, showed an opacity in the right upper zone [Table/Fig-2].
Air–crescent sign seen in right lung apex
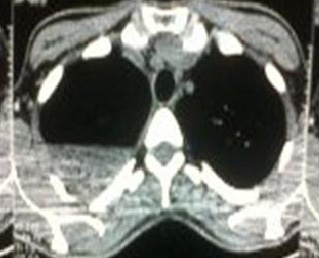
Fibrotic streaks seen in right lung apex
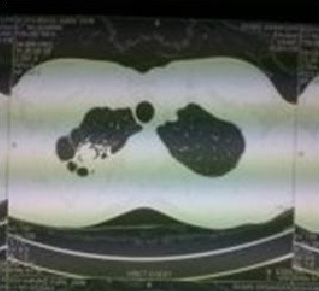
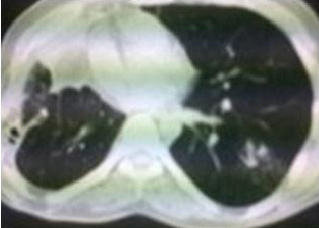
A diagnosis of recurrent aspergillum was made and the patient was treated with various anti- fungal agents with short spells of symptomatic relief. In April 2011, contrast enhanced computerized tomography of the chest was done, which showed a pleural based cavitatory lesion with locules of gas in the right antero- lateral chest wall, which measured 0.4 x 13 cms. The distal part of the collection was abutting the right pulmonary artery. The middle lobe of the right lung was also reported as collapsed. In view of the previous history and the above mentioned findings, a radiological diagnosis of a recurrent aspergillum was formed [Table/Fig-3 & 4]. The patient was planned for right poster lateral thoracotomy with excision of the fungal ball with or without pneumonectomy.
Cystic area seen close to right anterior chest wall
CT Scan showing pleural based opacity with mottled air lucencies
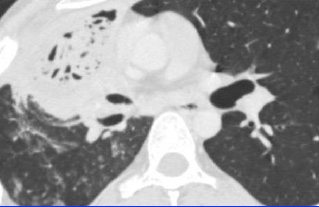
The pre-operative investigations showed
Hb = 12.0,Pcv = 29.5, TLC = 7170 N 60, Platelet = 256000
PT = 13/12, APTT = 24/24, RBS = 90
Urea = 26, Creatinine = 0.9
Chest X- Ray - Middle and upper zone opacity on right side.
Minimal effusion.
ECG =Normal study
2D Echo =Normal size Left Ventricle
LVEF = 60%
On opening the thorax, dense adhesions were found between the right lung, the pleura, the mediastinal structures and the diaphragm. The visceral pleura were thickened, with the lung being densely adherent to the mediastinal pleura. At thoracotomy, a purulent, crumpled and putrid, retained cotton fibre swab was discovered from the right pleural cavity space in the right upper lobe of the lung, in close proximity to the right principal bronchus. The distal part of the cotton fibre swab was abutting the right pulmonary artery, along with the collapse of the right middle lobe [Table/Fig-5,Table/Fig-6]. The cotton fibre swab was densely adherent to the lung and the right bronchus was intermediate with the enfolding of the lung parenchyma, over the swab. A careful, sharp dissection was done, decortication of the right lower lobe and the middle lobe and a rib resection flap were done and an intercostals drain was put. There was no evidence of a bronchopleural fistula.
Saggital view showed collapsed middle lobe apex and and opacity in the upper zone
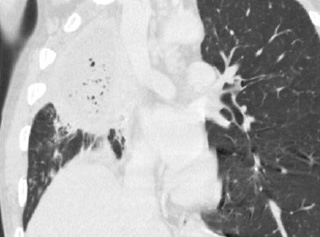
Pleural based collection abutting right pulmonary artery
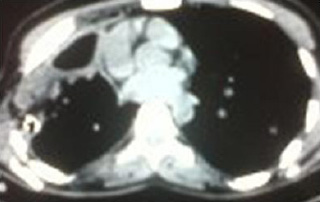
The post-operative chest X- ray revealed complete expansion of the right lung. The purulent material which was drained from the pleural space did not grow any fungus on incubation. On the third post-operative day, there was evidence of an air leak, which was managed conservatively. The bronchopleural fistula persisted for 3 months with conservative management. The repair of the bronchopleural fistula was done with a pectoralis major myocutaneous flap. The recovery was uneventful and there was no evidence of a bronchopleural fistula.
DISCUSSION
The word “gossypiboma” (Latin gossy- pium = cotton) refers to sponges, towels or other instruments (laparotomy pads, cotton swabs and buds, drains, needles, haemostats and forceps) which are inadvertently forgotten within the human body during surgical procedures [2]. Though this term specifically describes the foreign bodies with a cotton matrix, it may be employed for any kind of retained surgical material. Being first described in 1884 3, its occurrence has several remarkable aspects which include the risk of complications (abscesses, fistulas, perforations, adhesions, migrations within the contiguous organs, or remobilization through the vessels) and possible legal consequences [4–6].
The clinical presentation of the Retained Surgical Foreign Bodies (RSFBs) may be acute or delayed. While many RSFBs are identified and retrieved immediately or shortly after a surgical wound closure , some may go unnoticed for years or even decades.
Gossypibomas vary in radiological manifestations according to their location and the chronicity of the retained gauze, the type of foreign body reaction and the presence of a radiopaque marker. On plain chest radiographs, a gossypiboma is manifested as an unusual opacity or as an atypical mass, which generally does not change over time. Computerized axial tomography is the best method for detecting a sponge and for evaluating the complications [6]. The typical computerized axial tomography feature of a retained gauze is a predominantly high- attenuating, central mass with a spongiform pattern of air bubbles and a hyper dense, well-enhancing rim [6–8]. Several hypotheses on the origin of the air bubbles have been suggested. The air bubbles had been interpreted as an infection or even an abscess [9,10]. Recently, the air bubbles have been believed to be caused by the gas which is trapped within the synthetic fibres of the surgical gauze which may have been inadvertently left in place during a previous surgery. It has also been suggested that the air can remain inside or that it can decrease over a period of time [9]. However, our case suggested a different hypothesis for the origin of the air bubbles. Our case showed the presence of a bronchopleural fistula in the immediate postoperative period which was suggestive of the presence of the communications between the cavity and the bronchus. Park et al., reported a similar case of a 59 year old man where the air crescent which was within the gossypiboma resulted from the communications between the mass and the adjacent bronchioles in the same way as in the development of the air bubbles [11]. There are relatively few descriptions of the imaging characteristics of the intra- thoracic swabs. The computerized axial tomography appearances of a retained intra- thoracic swab are variable because of the many potential anatomical sites in the thorax where swabs may be left. Several features should alert the radiologist to the possibility of a retained swab. The highly unusual, multilayered appearance which is shown on computerized axial tomography should not be attributed to a simple lung abscess (a loculated empyema) and it would be unlikely to be mistaken for any other mass or tumour. The predominantly high attenuation central “nidus” represents the swab (without the presence of a radiopaque marker), and again, it would not be a feature of a simple abscess. The low attenuation layer outside this represents the pus which surrounds the swab and, in our case, the air- fluid level indicated the communication of the mass with the bronchial tree.
CONCLUSION
Gossypibomas are rarely seen following thoracic surgeries, and the patients are usually asymptomatic for a long period after the initial operation.Computerized axial tomography is the best method for detecting a sponge and for evaluating the complications. Adequate preventive measures should be taken to avoid all the deleterious consequences of RSFBs, which include the need for a re- operation.
[1]. Karabulut N, Herek D, Kýroglu Y, CT features of intrathoracic gossypiboma (textiloma)Diagn Interv Radiol 2011 17:122-24. [Google Scholar]
[2]. Patel AM, Trastek VF, Coles DT, Gossypibomas mimicking echinococal cyst disease of the lungChest 1994 105:284-85. [Google Scholar]
[3]. Wilson CP, Foreign bodies left in the abdomen after LaparotomyGynecology 1884 Tr 9:109-12. [Google Scholar]
[4]. Catalano D, Lapiccirella G, Erosion of the duodenal wall caused by the migration of a retained surgical sponge into the duodenal lumenRadiologe 1987 27:301-02. [Google Scholar]
[5]. Kester NL, Hassien JD, Pulmonary embolism caused by a surgical spongeAJR 1992 158:757-58. [Google Scholar]
[6]. Yamato M, Idol K, Izutsu M, Narimatsu Y, Hiramatsu K, CT and ultrasound findings of surgically retained sponges and towelsCAT 1987 11:1003-06. [Google Scholar]
[7]. Sheehan RE, Sheppard MN, Hansell DM, Retained intra- thoracic surgical swab: CT appearancesJ Thorax Imaging 2000 15:61-64. [Google Scholar]
[8]. Catalano O, Nunziata A, An unusual thoracic opacity Gossypiboma (retained surgical foreign body)Radiologe 1997 37:763-64. [Google Scholar]
[9]. Kopka L, Fischer U, Gross AJ, Funke M, Oestmann JW, Grabbe E, CT of retained surgical sponges (textilomas): pitfalls in detection and evaluationJ Comput Assist Tomogr 1996 20:919-23. [Google Scholar]
[10]. Schmitt R, Helmberger T, Spindler-Thiele S, Loitzsch RM, Sonography and computed tomography in intraperitoneally retained abdominal drapesRofo 1992 157:520-22. [Google Scholar]
[11]. Park HJ, Im SA, Chun HJ, Park SH, O JH, Lee KY, Changes in CT appearance of intrathoracic gossypiboma over 10 yearsBr J Radiol 2008 Feb 81(962):e61-63. [Google Scholar]