According to the community-led programmatic mapping and population size estimation (p-MPSE) activity undertaken as part of the national programme during 2020-2023, the estimated population of MSM amounts to 351,000 (314,000-388,000). This study was conducted across 735 districts in India [1]. Even previously declining STIs like syphilis are currently witnessing an upward trend among MSM [2]. MSM is an umbrella term used to describe a variety of MSM and therefore may transmit or acquire HIV or other STIs, but do not necessarily share the same sexual orientation, sexual identity, or gender identity.
Previously, Section 377 of the Indian Penal Code (IPC) referred to unnatural offences, stating that whoever voluntarily engages in carnal intercourse against the order of nature with any man, woman, or animal shall be punished with imprisonment for life. On 6th September 2018, a Constitution Bench of the Supreme Court delivered a historic judgement in the case of Navtej Singh Johar and Ors v. Union of India, on petitions challenging Section 377 IPC. The Bench declared that adult consensual homosexuality cannot be deemed a crime, thereby invalidating the provision to that extent.
However, there remains an insensitive attitude among some individuals towards this population, making them reluctant to access healthcare services. This situation must change and more studies need to be conducted to ascertain the incidence and prevalence of STIs and HIV among the MSM population in India, so that misconceptions regarding these diseases can be addressed and proper education can be provided. According to the National AIDS Control Organisation (NACO) survey, RPR/VDRL reactivity is higher in Kerala (0.98) compared to Andhra Pradesh (0.26) and Tamil Nadu (0.33) [1].
The purpose of this study was to provide insights into the STI patterns among the MSM population in Kerala and to offer appropriate treatment based on clinical diagnosis, along with related counselling. The aim of the study was to identify the trends of various STIs among the MSM population attending DVL OPD. The primary objective of the study was to identify the association between condom use and STIs, while the secondary objective was to provide appropriate treatment for STIs using syndromic management, colour-coded kits and counselling according to their clinical diagnosis.
Materials and Methods
This hospital-based cross-sectional study was conducted from March 2023 to February 2024 at Karuna Medical College in Chittur, a tertiary care centre in Palakkad, Kerala, India following ethical clearance (KMC/IHEC/06/2023). Study participants were recruited with the assistance of an Non Governmental Organisation (NGO) working with the MSM population, as it is not easy to encourage them to visit the hospital for awareness and health check-ups regarding STIs. NGOs were required to track the partners of cases presented in the outpatient department. A snowball sampling technique was adopted for the study.
Inclusion criteria: Male volunteers aged over 15 years who provided with written consent and who reported peno-oral or peno-anal sexual contact with other men were included in the study.
Exclusion criteria: A male volunteer below 18 years and who did not provide consent were excluded from the study.
Sample size: The study sample size was n=60 based on the above criteria. If erosion or ulcers were present at the contact sites, dark ground microscopy from the discharge, Tzanck smear and Gram stain were conducted. Serological tests for HIV, HBV and syphilis were performed on all study participants. Patients diagnosed were treated according to their diagnoses: syphilis was treated with injection benzathine penicillin (White kit); Acute Gonococcal Urethritis (AGU) was treated with injection ceftriaxone 1 g intravenously as a single dose (Grey kit); NGU was treated with oral doxycycline 100 mg twice daily for seven days and azithromycin 1 g as a single dose (Grey kit); genital HPV infection was treated with topical podophyllin once weekly until resolution; herpes genitalis was treated with oral acyclovir 400 mg thrice daily for five days (Red kit); scabies was treated with 5% permethrin cream once weekly for two weeks, along with antihistamines; CBP was treated with azole cream and an oral fluconazole 150 mg stat dose (Green kit); and genital molluscum was treated using the needling method.
Statistical Analysis
A descriptive analysis of the collected data was conducted using statistical methods. Categorical variables, such as the type of sexual contact, condom usage and STIs, were expressed as frequencies and percentages. The Chi-square test was applied, with p-values of ≤0.05 considered statistically significant.
Results
Among the 60 patients enrolled in this study, 31 were diagnosed with STIs, resulting in a prevalence of 51.7%. The majority of subjects were in the age group of 16-25 years (50%), while the least represented group was those aged over 46 years (5%). Their educational background indicated that 30% had completed secondary education, 26.7% had an intermediate level of education, 23.3% had a degree, 16.7% had completed primary education and the remaining participants were illiterate. The most common profession was manual labour, followed by workers in other professions, students and those unemployed [Table/Fig-1].
Demographic details of study participants.
| Demographic details | n (%) |
|---|
| Age (years) |
| 16-25 | 30 (50) |
| 26-35 | 15 (25) |
| 36-45 | 12 (20) |
| >46 | 3 (5) |
| Education status |
| Illiterates | 2 (3.30) |
| Primary education | 10 (16.70) |
| Secondary education | 18 (30) |
| Intermediate | 16 (26.7) |
| Degree/diploma | 14 (23.3) |
| Occupation |
| Student | 10 (16.7) |
| Sex worker | 18 (30) |
| Labourers | 15 (25) |
| Unemployed | 4 (6.7) |
| Other profession | 13 (21.6) |
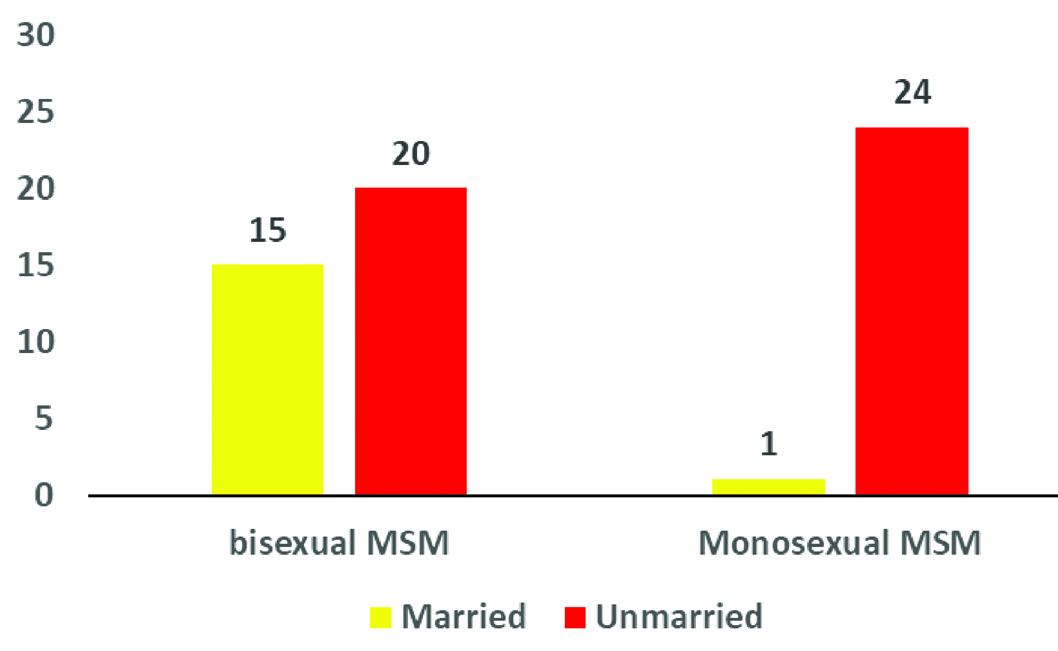
The majority of participants were identified as bisexual (58.3%); however, among unmarried participants, monosexual orientation was more prevalent. This trend highlights the reluctance of young individuals who identify as monosexual to engage in marital relationships [Table/Fig-2].
Marital status and sexual orientation.
It is alarming to observe that out of the 60 study participants, 31 (51.7%) had some form of STDs, with 10 being serologically positive for HIV and seven diagnosed with syphilis. Three cases each of CBP, herpes genitalis and NGU, as well as two cases each of AGU and scabies. Hepatitis B was not detected [Table/Fig-3,4].
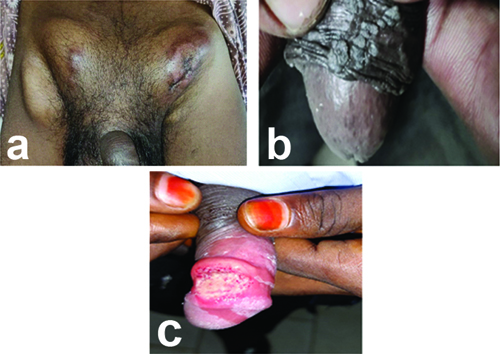
Clinical images of STD’s studied: a) Groove’s sign of lymphogranuloma venereum; b) Genital warts; c) Syphilitic ulcer.
*private-parts held by the patients themselves
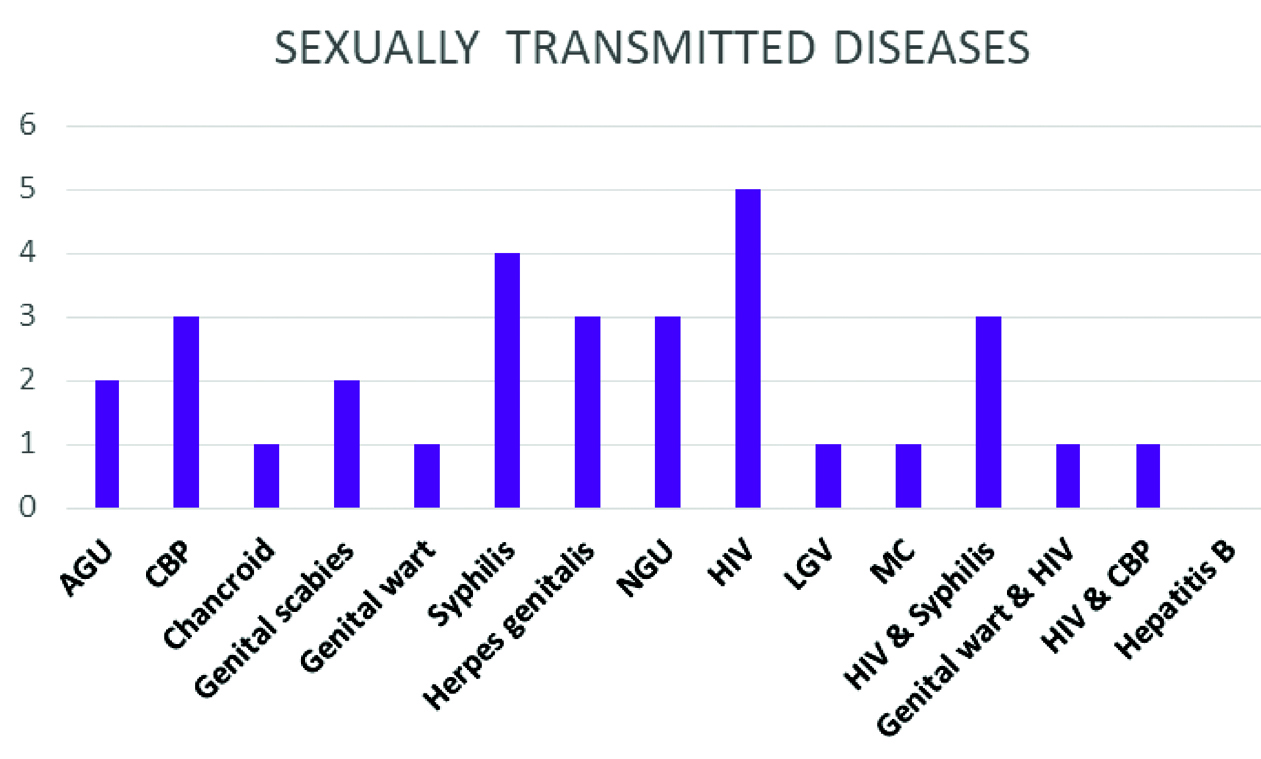
Distribution of STD’s in study participants.
AGU: Acute gonococcal urethritis; CBP: Candidal balanoposthitis; NGU: Non-gonococcal urethritis; HIV: Human immunodeficiency virus; LGV: Lympho granuloma venerum; MC: Molluscum contagiosum
Among the study participants, 52.67% reported playing an ano-receptive role, 25% played an ano-insertive role and the remainder played both receptive and insertive roles. Non usage of condoms was linked to the development of STDs. Among the 31 participants diagnosed with STDs, 20 reported not regularly using condoms, while out of the 29 who were not diagnosed with any STDs, 18 reported regular condom usage. According to the Chi-square test, we obtained a p-value of 0.03, indicating a significant association [Table/Fig-5].
Comparison of condom usage among study participants diagnosed with STD and without STD.
| STD diagnosed | STD notdiagnosed | Chi-square, p-value |
|---|
| Condom non users | 20 | 11 | χ2-4.24p-value=0.03 |
| Condom users | 11 | 18 |
| Total | 31 | 29 |
Discussion
The United Nations General Assembly Special Session on HIV/AIDS Report estimates that there are about 3.1 million MSM in India [3]. In present study, MSM are defined as men who engage in sexual activity with other men and, as a result, may transmit or acquire HIV or other STDs, but do not necessarily share the same sexual orientation, sexual identity, or gender identity. Recent research indicates a synergy between STIs and HIV transmission and acquisition, which, in turn, enhances the transmission or acquisition of HIV among MSM. There has been a global rise in STIs within this population [4,5]. Therefore, there is a need for more studies in this field to raise awareness about STIs among MSM. Present study aimed to contribute to this effort.
In the Indian context, MSM are primarily classified as kothis, who assume a receptive role in peno-oral and anal sex and often display more feminine characteristics; panthis, who are masculine and take on the role of insertive male partners in peno-oral and anal sex; and double deckers, who act as both receptive and insertive partners [6]. Indian literature describes the existence of hijras/aravanis and homosexuality dating back to ancient times. Sculptures and mural paintings in various temples across India also provide evidence of this historical context [7]. Until recently, Section 377 of the IPC in Indian law stated that anyone who voluntarily engages in carnal intercourse against the order of nature with any man, woman, or animal shall be punished with imprisonment for life. However, in a landmark judgment on 6th September 2018, the Supreme Court, after considering the behavioural, sexual and social implications, declared that adult consensual homosexuality cannot be deemed a crime, effectively decriminalising this section [8].
Despite this progress, marginalisation and social stigma persist, leading many individuals to experience low self-esteem, demotivation and engagement in high-risk sexual behaviours, including unprotected sexual intercourse and substance abuse. This ultimately contributes to the surge in STIs and the re-emergence of previously controlled infections.
In the present study, 50% of participants were in the age group of 16-25 years. An 80% of the patients had completed their secondary education and 73% were unmarried [Table/Fig-6] [9-11].
Comparison of demographic profile [9-11].
| Demographic profile | Prajapati AC et al., (2015) [9] | Salve, HR at al., (2015) [10] | Mahapatra T et al., (2015) [11] | Present study, 2025 |
|---|
| Age (years) | Mean | 33.6 years | 31.5 years | 23.4 years | 22.6 years |
| Educational status | Illiterates | 19.3% | 23.9% | 4.21% | 3.3% |
| Marital status | Married | 47.6% | 55.9% | - | 26.6% |
| Unmarried | 50% | 44.1% | - | 73.4% |
| Occupation | Students | | 4.1% | 23.38% | 16.7% |
| Labourers | 11% | 23.5% | - | 25% |
| Male sex workers | - | - | - | 30% |
| Condom usage | Yes | 42.2% | - | 41.6% | 48.3% |
There is an alarming rise in STDs among the younger generation, as noted in previous studies. A study conducted by Thunyapipat C et al., revealed that adolescents and young people who identify as homosexual or bisexual reported high levels of sexual risk behaviour correlated with their usage of online dating apps and websites [12]. Specifically, social network dating—where people meet online—led to a greater likelihood of haphazard, spontaneous sexual encounters, which in turn resulted in impulsive, careless and unplanned sexual activity and behaviours. Youth who have completed secondary education are increasingly gaining opportunities and confidence to identify themselves and their sexual orientation while deliberately staying away from marital relations. According to the majority of participants, one of the main obstacles to disclosing their sexual inclinations is their concern that their families will not accept their sexuality [13].
In present study, a total of 35 participants identified as bisexual MSM and 15 were married against their will to members of the opposite sex, either due to social pressure or reluctance to defy conventional standards. Ultimately, these individuals function as a bridge population in the spread of several STIs.
STIs have been reported more commonly among patients engaged in selling sex (MSW), with a prevalence of 30%. MSWs must satisfy their customers and often have to consent to unprotected sex against their will, making them more susceptible to STIs than other MSM. Among the 31 MSM diagnosed with STIs in present study, more than half were found to have HIV and syphilis. While the incidence of HPV, herpes and AGU showed a decreasing trend, NGU and CBP are on the rise [Table/Fig-7] [1,9].
Comparison of STD’s with previous studies [1,9].
| Clinical diagnosis | Garg T et al., (2004) [1] | Agarwal NP et al., (2014) [9] | Present study |
|---|
| HIV | 4.5% | 23% | 31.5% |
| Syphilis | 27% | 26.9% | 22% |
| HPV | 26% | 23% | 5% |
| Herpes Genitalis | 19% | 11% | 9.5% |
| AGU | 12% | 6% | 5% |
| NGU | 6.6% | - | 9.5% |
| MC | - | 9.62% | 3% |
| CBP | 4.5% | 7.69% | 9.5% |
| Genital Scabies | 6.6% | 1.92% | 5% |
AGU: Acute gonococcal urethritis; CBP: Candidal balanoposthitis; NGU: Non-gonococcal urethritis; HIV: Human immunodeficiency virus; HPV: Human papilloma virus; MC: Molluscum Contagiosum
In India, less than 4% of the general population has any of the four curable STIs; however, the burden of STIs is likely to be significantly higher among subpopulations engaging in high-risk behaviours, such as MSM, Transgender Individuals (TGs), Injection Drug Users (IDUs) and Female Sex Workers (FSWs). Although there is a shortage of research on the incidence of STIs in India’s major demographics, relevant studies are still available; however, these data have not been combined to show the general temporal and spatial trends of STI infections across different key groups [14].
The increased risk of HIV acquisition and transmission may be explained by the damage to the epithelial barrier caused by syphilitic sores. Furthermore, the lesion site is rich in activated lymphocytes and macrophages, which serve as attachment sites for the highly expressed HIV receptors found within the ulcer region and can facilitate HIV infection [15]. Treponema pallidum’s outer membrane lipoproteins enhance the expression of the β-chemokine receptor CCR5 in human monocytes, thereby increasing their vulnerability to HIV infection [16].
Anoreceptive partners are more prone to mucosal tears, which can lead to the acquisition of STIs. In present study, the majority of participants identified as anoreceptive partners. Hence, proper condom usage is essential to prevent the acquisition of STIs. It was observed that the frequency of condom usage among the MSM population is showing a mild increase compared to previous studies conducted in India. A total of 48.3% of study participants reported that they regularly use condoms with a p-value of 0.03 when comparing the variables of those with and without STDs.
There is substantial evidence linking a significant risk of HIV infection to being a receptive partner during unprotected peno-anal intercourse. The medical and public health professions largely agree that latex and polyurethane condoms can greatly reduce the risk of HIV transmission during intercourse when used correctly [17]. Present study supports the notion that proper condom usage provides protection against STIs for the MSM population. We advocate for condom use as a crucial strategy for HIV prevention.
Limitation(s)
The limitations of the study include the relatively small sample size and the limited geographical coverage compared to previous studies.
Conclusion(s)
Unmarried young students represent a relatively high-risk group within the MSM population for acquiring STIs. The promotion of sex education in schools and colleges is essential. An increasing trend of HIV and syphilis among the MSM population has been observed. It is crucial to provide health education starting from schools, focusing on safe sex practices, the importance of avoiding multiple sexual partners, the risks of substance abuse and the regular use of condoms for the youth in our country. Therefore, there is an urgent need to strengthen targeted interventions, along with appropriate management and follow-up for patients and their partners within the MSM population.
AGU: Acute gonococcal urethritis; CBP: Candidal balanoposthitis; NGU: Non-gonococcal urethritis; HIV: Human immunodeficiency virus; HPV: Human papilloma virus; MC: Molluscum Contagiosum