Knee OA is the most common type of arthritis, and its incidence is increasing due to rising life expectancy and obesity rates [1]. India, with a large population over 55 years old, is expected to face a significant economic burden due to OA, with the population aged 60 years and over predicted to reach 323 million by 2050 [2]. Despite the high burden of OA in India, there is a lack of published information on its epidemiology and long-term treatment outcomes, making resource allocation decisions challenging for healthcare administrators and policymakers [3]. Non invasive treatment methods for OA aim to improve patients’ quality of life by managing pain, improving function and modifying the disease process and cartilage degeneration [4]. These methods include medications such as analgesics [5], steroid and non steroid anti-inflammatory drugs [6], glucosamine/chondroitin supplementation [7], and hyaluronic acid injections [8]. However, chronic OA pain is often not effectively managed with current treatments [9].
TKA is a common treatment for knee arthritis that is refractory to conservative management, but 8-34% of patients experience chronic pain after the procedure [10]. GNRFA has emerged as an alternative to conservative therapy and TKA [10]. RFA dates back as far as 1931 when it was used for the ablation of the Gasserian ganglion in treating trigeminal neuralgia. The technique of thermal RFA was initially documented in 1960 [11] and subsequently utilised in the 1970s for treating back pain by targeting the spinal facet joints [12]. This technique destroys nerves by increasing the temperature of the surrounding tissue to around 80°C-90°C using radiofrequency probes [13]. On the other hand, pulsed RFA, which was first developed in 1998, is a method of removing tissue without causing its destruction. Pulsed RFA is accomplished by alternating prolonged periods of inactivity that allow for the dissipation of heat with short bursts of high-voltage electrical current [14]. The periodic electrical supply prevents damage to the tissue, allowing the target tissue to stay at a temperature below 42°C. Choi WJ et al., first proposed using RFA as a treatment for Ganglion Cysts (GNs) in knee OA [15]. GNRFA is a widely used in surgery for addressing knee pain caused by arthritis. Given that classic RFA is still the most commonly employed RFA technique, it is crucial to assess its effectiveness in alleviating knee pain caused by degenerative OA in patients with severe OA who are unwilling to undergo TKA. Hence, the present study was undertaken with the aim to investigate the effectiveness of RFA of genicular nerves in reducing knee pain due to degenerative OA. The study also evaluates functional outcomes, analgesic use and quality-of-life improvements following RFA.
Materials and Methods
The present prospective interventional study was conducted on 38 knees with chronic pain due to degenerative OA at the Department of Orthopaedic Surgery and Pain and Palliative Care Unit, JSS Medical College and Hospital in Mysore, Karnataka, India over a period of one year from July 2022 to June 2023. The study commenced after obtaining Ethical Clearance (JSS/MC/PG/IEC-139/2022-23) from the institutional ethical committee.
Inclusion criteria: Patients over 50 years old with degenerative knee OA (Kellgren-Lawrence grading III and above) [16,17] who did not respond to conservative treatments after six months. Patients who were not suitable for surgery due to medical co-morbidities or a high Body Mass Index (BMI), as well as advanced OA patients unwilling to undergo TKA were included in the study.
Exclusion criteria: Patients with neuropathic knee joints, chronic inflammatory arthritis, psychological issues, uncontrolled diabetes mellitus, bleeding disorders, implantable defibrillators or pacemakers and active knee infections were excluded from the study.
Sample size calculation: The sample size of 30 was calculated based on a retrospective review of Outpatient Department (OPD) records, focusing on the approximate prevalence of patients over 50 years old with degenerative knee OA (Kellgren-Lawrence grading III and above) who were not suitable for surgery. This calculation was made using a 95% confidence level and the formula for sample size calculation:
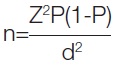
Where n is the sample size, Z is the statistic corresponding to the level of confidence, P is the expected prevalence (with p approximately equal to 50%), and d is the precision.
Patients who fulfilled the inclusion criteria were selected for the study after signing a written consent form. The study participants were randomly selected using simple random sampling. Relevant clinical data were recorded in a structured proforma, and the clinical profiles of the patients were evaluated according to the proforma.
The study comprised a comprehensive assessment of participants, including a thorough medical history, physical examination of the knee, X-ray, laboratory tests like Prothrombin time/international normalised ratio, HBsAg, HIV, HCV, Electrocardiogram (ECG), symptom measurement, and review of adverse events. An X-ray of the knee was taken under weight-bearing conditions, and the grading of OA was done using the Kellgren-Lawrence grading scale [16,17]. The study was divided into multiple visits, specifically Visit 1, Visit 2, and so on, scheduled at baseline, 1st month, 3rd months, and 6th months postprocedure, with each visit being analysed separately. The treatment involved a single procedure, followed by further follow-up. No study drug supplies or administration were required, and any complications or drug interactions during or after the procedure were meticulously recorded. Additionally, no concomitant therapy was permitted. The instruments used in the study included the Avanos medical radiofrequency generator and the Avanos radiofrequency 100 mm needle with a 10 mm active tip, manufactured by Avanos Medical, Inc., USA (formerly Halyard Health, Inc).
During the procedure, patients were positioned supine with their knee flexed at approximately 30°. Local anaesthesia was administered via subcutaneous lidocaine injections at the cannula insertion sites. A 100 mm, 20-gauge RF cannula (DIROS) with a 10 mm active tip was inserted percutaneously at three specific locations: the junction of the femoral shaft and lateral epicondyle (Superior Lateral Genicular Nerve), the medial aspect of the distal femoral diaphysis (Superior Medial Genicular Nerve), and the junction of the tibial diaphysis and medial condyle (Inferior Medial Genicular Nerve). The cannula tips were confirmed to be in the correct position using fluoroscopic imaging and sensory/motor testing. Using the RF generator, radiofrequency thermocoagulation was then performed at 60°C for 70 seconds, 70°C for 80 seconds, and 80°C for 90 seconds, followed by the injection of 20 mg of methylprednisolone through the cannula to prevent post-procedural pain and neuritis [18].
Patients were assessed and followed-up for pain using the NRS from 0 to 10 and the number of analgesic pills consumed per day. Functional outcomes and quality of life were assessed using the WOMAC [19] before and after the intervention on day one, at one month, at three months and at six months. The WOMAC score is closely related to quality of life, as it assesses the impact of OA on a patient’s daily life. A higher WOMAC score indicates greater functional impairment and reduced quality of life. The WOMAC [19] is a 24-item, condition-specific questionnaire that assesses the symptoms and functional limitations associated with knee OA. Since the study was conducted using a single-blinded method, all patients underwent RFA of the genicular nerve of the affected knee performed by a single pain clinician who was blinded to the patient details. The pain evaluation at baseline and during the study intervals was carried out by a different clinician who conducted the study.
Statistical Analysis
Statistical analysis was conducted using RStudio Desktop Version 4.3.0. Descriptive analysis included frequencies for categorical variables, while continuous variables were presented as means or medians with Interquartile Range (IQR), depending on their distribution. The Friedman test was used to study the effectiveness of RFA of genicular nerves in reducing knee pain due to degenerative OA, and the pairwise Wilcoxon test with Bonferroni correction was used to compare statistical significance between different pairs. A p-value <0.05 was considered statistically significant.
Results
[Table/Fig-1] shows the demographic characteristics of the study population (N=38). The results revealed that the mean age of the study participants was 66.18 years. Among the 38 participants, 23 (60.5%) were females and 15 (39.5%) were males. A total of 24 (63.16%) subjects had normal alignment, while 14 (36.84%) subjects had deformities. Furthermore, 32 (84.2%) subjects had intra-articular swelling, and 11 (28.95%) study participants exhibited joint line tenderness.
Demographic and characteristics of the study population (N=38).
| Characteristic | Summary statistics |
|---|
| Age (years), Mean±SD | 66.18±9.15 |
| Gender, n (%) |
| Female | 23 (60.5) |
| Male | 15 (39.5) |
| Alignment, n (%) |
| Normal | 24 (63.16) |
| Varus deformity | 14 (36.84) |
| Intra articular swelling, n (%) |
| Yes | 32 (84.2) |
| No | 6 (15.8) |
| Joint line tenderness, n (%) |
| Yes | 11 (28.95) |
| No | 27 (71.05) |
All 38 patients had a negative posterior drawer test, indicating no evidence of posterior cruciate ligament instability. Additionally, 37 patients exhibited quadriceps atrophy, a common finding in OA patients. The valgus stress test, anterior drawer test, Apley’s grinding test, McMurray’s test, and varus stress test were all negative in all 38 patients, suggesting no significant ligamentous instability or meniscal damage.
[Table/Fig-2] shows the clinical parameters of the study population (N=38). The results indicated that coronary heart disease was absent in all 38 (100%) subjects. Nine (23.63%) subjects were diabetic, 22 (57.89%) subjects experienced pain in the left knee, and 16 subjects reported pain in the right knee. Ischaemic heart disease was present in one subject, 18 (47.36%) subjects were hypertensive, and one subject had hyperthyroidism.
Clinical parameters of study population (N=38).
| Characteristic | n (%) |
|---|
| Coronary heart disease |
| No | 38 (100) |
| Diabetic miletus (The haemoglobin A1C (HbA1c): 6.5% or higher) |
| Yes | 9 (23.68) |
| No | 29 (76.32) |
| Chief complaints |
| Pain left knee | 22 (57.9) |
| Pain right knee | 16 (42.10) |
| Ischaemic heart disease |
| Yes | 1 (2.63) |
| No | 37 (97.37) |
| Hypertension |
| Yes | 18 (47.37) |
| No | 20 (52.63) |
| Hyperthyroidism |
| Yes | 1 (2.63) |
| No | 37 (97.37) |
[Table/Fig-3] shows a comparison of the number of analgesic pills taken per day at different time points. A statistically significant difference was observed in the median number of analgesic pills taken per day at different time points (p-value <0.05). Subsequent Bonferroni post-hoc testing revealed a statistically significant difference in the median number of analgesic pills taken per day when comparing the “Before Procedure” time point to other time points (p-value <0.05).
Comparison of number of analgesic pills per day at different time points.
| Number of analgesic pills per day at | Median (IQR) | p-value (Overall) | p-value (Before procedure vs. other time points) |
|---|
| Before procedure (baseline) | 1 (1,1) | <0.001 | - |
| After procedure | 0 (0,1) | <0.001 |
| After 1 month | 0 (0,0) | <0.001 |
| After 3 months | 0 (0,0) | <0.001 |
| After 6 months | 0 (0,0) | <0.001 |
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range
[Table/Fig-4] shows a comparison of the WOMAC score at different time points. A statistically significant difference was observed in the median WOMAC score at different time points (p-value <0.05). The Bonferroni post-hoc test further demonstrated that the median WOMAC score exhibited a statistically significant difference when compared to the time point before the procedure (p-value <0.05).
Comparison of WOMAC score at different time points.
| WOMAC score at | Median (IQR) | p-value (Overall) | p-value (Before procedure vs. other time points) |
|---|
| Before procedure (baseline) | 87 (82,88) | <0.001 | - |
| After procedure | 21 (19,23) | <0.001 |
| After 1 month | 19 (17,20) | <0.001 |
| After 3 months | 16.5 (15,17) | <0.001 |
| After 6 months | 14 (13,15) | <0.001 |
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index
[Table/Fig-5] shows a comparison of the pain score (NRS at rest) at different time points. A statistically significant difference was found in the median pain level (NRS at rest) at different time points (p-value <0.05). The Bonferroni post-hoc test revealed that the median pain level (NRS at rest) exhibited a statistically significant difference when compared to the time point before the procedure (p-value <0.05).
Comparison of pain score (pain (NRS at rest) at different time points.
| Pain (NRS at rest) | Median (IQR) | p-value (overall) | p-value (Before procedure vs. other time points) |
|---|
| Before procedure (baseline) | 7 (7,80) | <0.001 | - |
| After procedure | 3 (3,4) | <0.001 |
| After 1 month | 3 (2,3) | <0.001 |
| After 3 months | 2 (2,3) | <0.001 |
| After 6 months | 2 (2,3) | <0.001 |
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; NRS: Numeric rating scale
[Table/Fig-6] shows a comparison of the pain score (NRS with movement) at different time points. A statistically significant difference was observed in the median pain level (NRS with movement) at different time points (p-value <0.05). The Bonferroni post-hoc test indicated that the median pain level (NRS with movement) displayed a statistically significant difference when compared to the time point before the procedure (p-value <0.05). None of the participants documented any complications during the follow-up period.
Comparison of pain score (NRS with movement) at different time points.
| Pain (NRS with movement) | Median (IQR) | p-value (Overall) | p-value (Before procedure vs. other time points) |
|---|
| Before procedure (baseline) | 9 (8,9) | <0.001 | - |
| After procedure | 4 (4,5) | <0.001 |
| After 1 month | 4 (3,4) | <0.001 |
| After 3 months | 3 (3,4) | <0.001 |
| After 6 months | 3 (3,4) | <0.001 |
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; NRS: Numeric Rating Scale
Discussion
The present study investigated the efficacy of conventional RFA in managing chronic refractory knee pain associated with OA. The results showed a significant reduction in the usage of pain-relieving medication and an improvement in quality of life and patient satisfaction. Additionally, RFA provided sustained pain relief and enhanced functionality without significant adverse effects. The study enrolled 38 knees with chronic pain due to degenerative OA, with a mean participant age of 66.18±9.15 years, comprising 60.5% females and 39.5% males. The majority of participants (63.16%) had normal knee alignment, while 36.84% had varus deformity. Intra-articular swelling and joint line tenderness were observed in 84.2% and 28.95% of participants, respectively. Present study results correspond to a similar study conducted by Ahmed A and Arora D, which reported the mean age of the patients as 61.50±6.75 years; another study by de Sire A et al., reported an average age of 68.8±13.7 years [20,21].
By applying radiofrequency current near the genicular nerves, this procedure can block pain signals from the knee, providing relief and improving knee function for patients with knee OA or post-TKA pain [22]. The current technique of using conventional RF to target genicular nerves with fluoroscopic guidance was originally revealed by Choi WJ et al., and it provided significant knee pain relief for over 50% of participants for 12 weeks with no side-effects [15]. The current study similarly found a significant reduction in analgesic pill usage and pain levels (as measured by the NRS) at various time points after the procedure. The results showed a statistically significant difference in pain levels and analgesic usage before and after the procedure, indicating the effectiveness of the treatment. In line with present study, Konya ZY et al., found a significant decrease of 75% in the median Visual Analogue Scale (VAS) ratings when measured at 1, 3, and 6 months. At the end of the 6-month follow-up period, a significant proportion of patients (93.75%) had VAS values equal to or less than 4 [23]. Furthermore, similar to the present study, this study found that, concurrently with the effective pain relief achieved, there was a notable reduction in the use of painkillers and a considerable improvement in overall quality of life, with no significant adverse effects observed.
The various studies, in concurrence with the present study, consistently demonstrate the efficacy of RFA of genicular nerves in reducing pain and improving functional outcomes in patients with knee OA. de Sire A et al., found a significant decrease in pain levels, as measured by the numeric pain rating scale, from 7.48±1.74 to 3.63±1.68 (p-value <0.001) after ultrasound-guided RFA [21]. Additionally, they observed notable enhancements in overall functioning and health-related quality of life outcomes (p-value <0.05). Similarly, Ahmed A and Arora D, reported significant improvements in pain intensity at rest, during movement, and while weight-bearing from baseline to one month and six months after RFA (p-value <0.05) [20]. Mean pain scores decreased from 8.75-9.0 to 2.38-4.63 at one month and 3.13-4.63 at six months. Furthermore, a controlled study by Sari S et al., demonstrated that radiofrequency neurotomy significantly decreased pain (VAS-pain) at one month (p-value <0.001) and three months (p-value <0.001) compared to intra-articular injection [24]. Similarly, Santana Pineda MM et al., demonstrated that radiofrequency neurotomy of genicular nerves significantly decreased pain and resulted in 88% of participants experiencing a 50% or greater improvement in VAS scores at one month, 64% at six months, and 32% at 12 months [25].
A study by El-Hakeim EH et al., compared the efficacy of radiofrequency neurotomy of genicular nerves with conventional analgesics in managing pain and found significant differences in VAS scores between the two groups at two weeks, three months, and six months [26]. Additionally, both groups demonstrated significant improvements in VAS scores throughout the follow-up period compared to their pre-treatment values. In another similar study, Iannaccone F et al., found that GNRFA resulted in a 67% improvement in pain relief after three months in patients with chronic knee OA [27]. The average pain score decreased to 2.9 out of 10. At six months, 95% of patients who experienced pain relief at three months continued to experience alleviation, with an average pain score of 3.3 and 64% pain alleviation. In contrast, Vanneste T et al., reported a very low percentage of pain relief; the primary outcome was achieved in four out of 23 patients treated with conventional RF (17%), which reduced pain in the OA and persistent postsurgical pain population [28]. Fogarty AE et al., compared RFA with hyaluronic acid injection and found that the probability of treatment success was 1.8 times higher [29]. Wu BP et al., compared cooled and traditional thermal RFA and reported that genicular nerve t-RFA was associated with a higher probability of treatment success and a greater degree of pain relief at one month after the procedure compared to c-RFA in propensity score-matched patients with chronic knee pain [30].
Similar to the present study, a study by Ahmed A and Arora D, showed a considerable improvement in the WOMAC score, which decreased from 77.75±4.34 at the beginning to 38.38±5.82 and 39.25±5.12 after one and six months, respectively (p-value <0.05) [20]. The procedure resulted in a substantial enhancement in the quality of life, as indicated by a statistically significant p-value of <0.05. Additionally, in the study by San S et al., patients who underwent RF neurotomy of the genicular nerve reported a significant reduction in WOMAC total scores in the first month (p-value <0.001) compared to the group that underwent intra-articular injections [24]. Similarly, Santana Pineda MM et al., found that the application of radiofrequency neurotomy on the genicular nerves resulted in a substantial decrease in disability (measured using the WOMAC Index) for most subjects, without any negative incidents [25]. El-Hakeim EH et al., reported significant changes when comparing pretreatment values with values during the entire follow-up period regarding the total WOMAC index in both groups, with a significant difference in the total WOMAC index at the sixth month [26].
Regarding safety, the present study participants did not document any complications during the follow-up period. The safety of the technique is also supported by similar studies conducted by Choi WJ et al., and Konya ZY et al., that involved the knee joint [15,23].
Limitation(s)
The limitation of the present study was that, due to the 6-month follow-up period, it was not possible to ascertain the longevity of the observed effects.
Conclusion(s)
The significant reduction in daily analgesic intake, WOMAC scores, and pain scores (NRS at rest and with movement) following GNRFA indicates excellent treatment outcomes. This study confirms that GNRFA is a safe, effective, and efficient treatment modality, offering functional improvement and analgesia for patients with chronic knee OA. RFA of the genicular nerves is a valuable intermediate treatment option for OA patients who rely heavily on analgesics or are unsuitable for surgery. Additionally, RFA has emerged as a promising treatment for patients experiencing persistent pain after TKR. As a minimally invasive and cost-effective procedure with a favourable safety profile, RFA is gaining popularity as a viable treatment choice for managing chronic knee pain in OA patients, providing significant pain relief and functional improvement for those debilitated by knee OA.
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; NRS: Numeric rating scale
p-value (overall) from Friedman test; p-value (Before procedure vs. other time points) from pairwise Wilcoxon test with Bonferroni correction; IQR: Interquartile range; NRS: Numeric Rating Scale