Many individuals experience significant stress due to lifestyle changes, which can contribute to suicidal ideation. This stress often stems from personal issues such as family conflicts, work pressures, or socio-economic challenges and can lead individuals to contemplate ending their lives [1]. Frequently, this tragic decision involves the ingestion of poisons readily available in the commercial market, with rodenticides being among the most commonly used substances in India [2]. Rodenticide poisoning occurs when humans or animals ingest toxic substances intended to eliminate rodents. These poisons can inflict severe damage and can be fatal if not addressed promptly. Rodenticide poisons are primarily classified into two categories: 1) Anticoagulants and 2) Non Anticoagulants. Anticoagulant rodenticides, such as brodifacoum and bromadiolone, function by inhibiting vitamin K-dependent clotting factors (Factors II, V, VII, IX). Non anticoagulant rodenticides, notably Bromethalin, pose even greater risks as they disrupt the central nervous system, leading to symptoms such as tremors, seizures and potentially respiratory failure [3]. In cases of suspected poisoning, it is imperative to seek immediate medical intervention. Treatment typically involves administering antidotes and supportive care to manage symptoms effectively. Additionally, management may include fluid therapy, oxygen support, blood transfusions and plasmapheresis. Severe cases necessitate hospitalisation for continuous monitoring and symptom management [4].
Histomorphological examination of tissue under a microscope is crucial for identifying the extent of damage to vital organs caused by rodenticide poisoning. This analysis provides valuable insights for clinicians to offer effective symptomatic treatment and expedite patient recovery. Therefore, the objective of this study was to find the histomorphological changes in the heart, lungs, liver, kidneys, spleen and brain in cases of rodenticide poisoning victims.
Materials and Methods
This cross-sectional study was conducted in the Department of Pathology using medicolegal autopsy specimens obtained from the Department of Forensic Medicine at Government Medical College and Hospital, Krishnagiri,Tamil Nadu, India. The study was carried out retrospectively over a one-year period from June 2023 to June 2024, following approval by the Institute’s Ethical Committee under number 55062024. The study encompassed all medicolegal autopsies conducted by the Forensic Department of Government Medical College and Hospital, Krishnagiri, during the specified period.
Inclusion criteria: Cases where the cause of death was identified as rat poison ingestion were included in the study.
Exclusion criteria: Cases involving other types of poisoning or those with fully autolysed tissues in which cell morphology could not be determined under the microscope after processing the tissue were excluded from this study.
Sample size: The sample size was determined using the convenience sampling technique, calculated via Solvin’s formula:
X=N/1+Ne2, X=30/1+1(0.05)2, X=30Given the adequacy of cases, the study proceeded with the collection of detailed crime history, clinical history and autopsy findings. Upon completion of the autopsy procedures, the relevant organs were dispatched to the Pathology Department for microscopic examination by forensic experts. The specimens analysed included the heart, lungs, kidneys, liver, spleen and brain, which perform vital functions in every individual and are the organs most likely to be damaged in poisoning cases. All the aforementioned organs were preserved in 10% formalin before and after the gross examination, and sections were taken from the specimens for further processing. Finally, histopathological sections were stained with routine H&E.
The following parameters were studied, which included the incidence of rodenticide poisoning, age, sex, fatality duration and histomorphological findings of vital organs, all of which were tabulated.
Both macroscopic and microscopic observations were meticulously documented in a case study format. The microscopic findings were examined by two pathologists to minimise interobserver variability. Conclusions were derived from a comprehensive analysis of both macroscopic and microscopic data, and the findings were systematically compiled and tabulated.
Statistical Analysis
For statistical analysis, data was entered into Excel and analysed using SPSS version 25.0, and expressed in frequency and percentage. Cross-tabulations were performed to analyse the parameters related to organ-specific findings in rodenticide poisoning.
Results
During the one-year study period, from June 2023 to June 2024, our department processed specimens from 450 medicolegal autopsies, of which 180 cases (40%) were attributed to poisoning [Table/Fig-1]. Among the 450 autopsy cases, which include both poisoning and non poisoning cases, death due to rodenticide poisoning was found in 32 cases [Table/Fig-2]. Of the 180 cases of poisoning in this study, 32 cases (17.78%) [Table/Fig-3] were specifically due to rodenticide poisoning, while the remaining 148 cases (82.22%) [Table/Fig-4] were attributed to other poisons. The age of the subjects ranged from 11 to over 61 years, with the study cohort comprising 12 females (37.50%) and 20 males (62.50%), indicating a higher prevalence among males [Table/Fig-5]. Among them, the younger age group between 11-20 years had 10 cases (31.25%), followed by the older age group between 50-60 years with eight cases (25.0%) being victims of this poison [Table/Fig-6]. The fatality rate, as detailed in [Table/Fig-7], demonstrates an increased rate of mortality associated with delayed hospitalisation following poison ingestion.
Showing the incidence of poisoning cases among the total number of post-mortems.
| Cases | n (%) |
|---|
| Total number of post-mortems done=450 |
| Number of poisoning cases | 180 (40) |
Showing the incidence of cases poisoned with rodenticide among the total number of post-mortems done.
| Cases | n (%) |
|---|
| Total number of post-mortems done=450 |
| Number of rodenticide poisoning cases | 32 (7.11) |
Showing the number of cases with rodenticides among the number of poisoning cases.
| Cases | n (%) |
|---|
| Total number of poisoning cases | 180 (40) |
| Number of rodenticide poisoning cases | 32 (17.78) |
Showing the number of poisoning cases other than rodenticides during the year.
| Cases | n (%) |
|---|
| Total number of poisoning cases | 180 (40) |
| Number of poisoning cases other than rodenticides | 148 (82.22) |
Showing the sex incidence of these cases.
| Sex | n (%) |
|---|
| Male | 20 (62.50) |
| Female | 12 (37.50) |
Showing the age incidence from the study group cases.
| Age group (years) | n (%) |
|---|
| 0-10 | - |
| 11-20 | 10 (31.25) |
| 21-30 | 6 (18.75) |
| 31-40 | - |
| 41-50 | 2 (6.25) |
| 51-60 | 8 (25) |
| 61 and above | 6 (18.75) |
Showing the fatal period in study cases.
| Fatal period | n (%) |
|---|
| Within half an hour | - |
| ½-1 hr | - |
| 1-2 hrs | - |
| 2-4 hrs | - |
| 4-8 hrs | 2 (6.25) |
| 12-24 hrs | 5 (15.62) |
| 1-2 days | 9 (28.12) |
| 3 days and above | 16 (50) |
The primary organs examined in all cases included the heart, lungs, liver, kidneys, spleen and brain. Histopathological examination of the specimens revealed congestion in most organs. Despite the common finding of congestion, significant morphological changes were observed in specific organs under the microscope, as depicted in [Table/Fig-8].
Histomorphological findings of various organs in rodenticide poison.
| Organ and findings | Out of 32 cases in each organ, n (%) |
|---|
| Liver |
| Steatosis | 12 (37.50) |
| Submassive hepatic necrosis | 8 (25) |
| Acute hepatic necrosis (fulminant hepatitis) | 6 (18.75) |
| Chronic Venous Congestion (CVC) | 4 (12.50) |
| Cholestasis | 2 (6.25) |
| Kidney |
| Acute tubular necrosis | 18 (56.25) |
| Chronic venous congestion | 14 (43.75) |
| Lungs |
| Diffuse alveolar haemorrhage | 12 (37.50) |
| Pulmonary oedema | 4 (12.50) |
| Emphysema | 2 (6.25) |
| Chronic Venous Congestion (CVC) | 14 (43.75) |
| Spleen |
| Diffuse splenic haemorrhage | 2 (6.25) |
| Chronic venous congestion | 30 (93.75) |
| Brain |
| Normal | 20 (62.50) |
| Congestion | 11 (34.37) |
| Cerebral haemorrhage | 1 (3.12) |
| Heart |
| Atherosclerosis | 7 (21.88) |
| Normal | 25 (78.12) |
On gross examination, the liver exhibited congestion in most cases. Microscopic examination of the liver showed acute hepatic necrosis (fulminant necrosis) [Table/Fig-9], which occurs at the late stage of rodenticide poisoning and acts as an indicator of end-stage liver disease. However, submassive necrosis [Table/Fig-10] of hepatocytes occurs before fulminant necrosis, indicating partial necrosis of hepatocytes in periportal areas. In this study, most of the liver specimens showed features of steatosis [Table/Fig-11], which is the accumulation of triglycerides due to hepatic dysfunction in the early stages of poisoning. Finally, in a few cases, cholestasis was observed, which also results from the accumulation of bile pigment due to hepatocytic injury.
Histopathological picture of liver shows massive necrosis of hepatocytes sparing the bile duct indicates acute hepatic necrosis (H&E; X40).
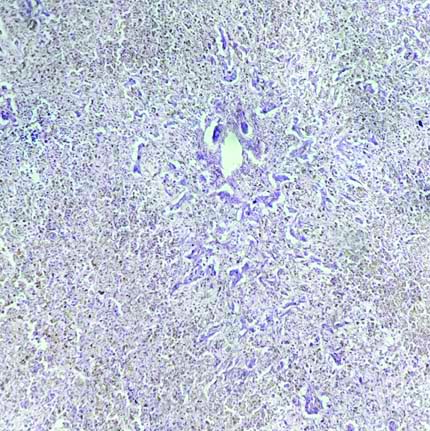
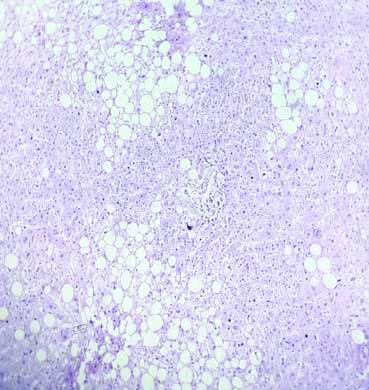
Histopathological picture of liver shows focal necrosis hepatocytes surrounded by normal liver parenchyma in submassive necrosis (H&E; X40).

The histopathological picture of the liver shows hepatocytes with fatty changes in hepatic steatosis (H&E; X10).
The kidneys displayed a pale cortex and congested medulla, which denotes acute tubular necrosis grossly in most cases, while the rest of the cases showed congestion. The kidneys predominantly exhibited acute tubular necrosis under microscopic examination as a direct effect of poison on renal tubular epithelial cells [Table/Fig-12].
The histopathological picture from the kidney shows renal tubules exhibiting marked necrosis of tubular epithelial cells in acute tubular necrosis (H&E; X40).
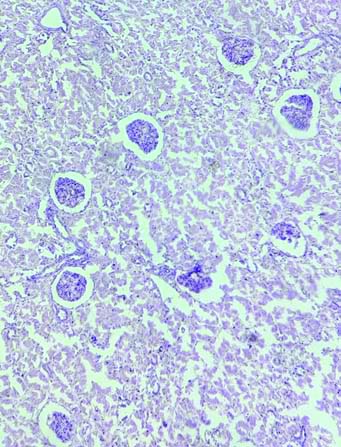
The lungs typically showed congestion grossly in most of the specimens, with some exhibiting heavy congestion and frothy secretion upon dissection. Under the microscope, notable findings in the lungs included diffuse alveolar haemorrhage [Table/Fig-13], emphysema [Table/Fig-14], pulmonary oedema [Table/Fig-15], and chronic venous congestion.
Histopathological picture from lung shows diffuse alveolar haemorrhage (H&E; X10).

Histopathological picture from lung shows dilated alveoli with emphysematous changes (H&E; X10).
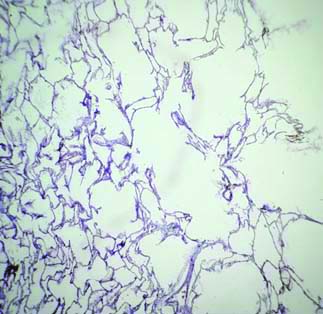
Histopathological picture from lung shows alveoli filled with fluid in pulmonary oedema (H&E; X40).
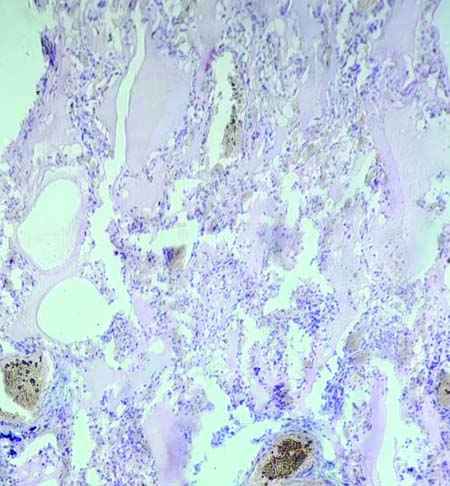
The spleen specimens displayed congestion both grossly and microscopically, with one showing splenic haemorrhage under the microscope.
On gross examination of the heart specimens, most exhibited pinpoint haemorrhages on their external and cut surfaces, associated with congestion. However, under microscopic examination of the sections from the heart, including the ventricles, aorta, and coronaries, most showed normal findings, with a few exhibiting age-related atherosclerotic changes that were not specific to this study.
Brain specimens were largely normal both grossly and microscopically, except for one case that revealed cerebral haemorrhage.
Discussion
This study indicates a higher prevalence of poisoning among males compared to females and revealed that individuals in the teenage, middle-aged, and elderly categories are particularly susceptible. Furthermore, the study highlights that delayed treatment following poison ingestion correlates with an increased fatality rate.
In the present study, the liver emerged as the most frequently affected organ due to its critical role in detoxifying poisons. Substances such as brodifacoum or bromadiolone, found in rat killer poisons, inhibit vitamin K epoxide reductase, leading to coagulopathy and subsequent liver damage. This results in extensive necrosis of liver cells while sparing the bile ducts [5]. In this study, submassive hepatic necrosis was observed in 25.0% of cases, which was consistent with the 28% reported by Sankappa PS et al., steatosis was found in 37.50% of cases, aligning with the 33% reported by the same study [6]. However, there is a discrepancy regarding acute hepatic necrosis, which was observed in 18.75% of cases in this study compared to 62% in the study by Das S et al., [7].
The kidneys were the second most affected organ. Toxins such as Alpha-Naphthylthiourea (ANTU) or bromethalin, present in rodenticide agents, directly damage the renal tubules, causing acute tubular necrosis. The extent of necrosis can be either diffuse or patchy, depending on the quantity of poison ingested by the individual. Regarding renal findings, acute tubular necrosis was observed in 56.25% of cases in this study, which was consistent with the finding of 44% reported by Das S et al., [7].
In the lungs, substances like zinc phosphide, present in rat killer poison, cause damage to the alveolar capillaries, leading to fluid loss, which results in pulmonary oedema and alveolar haemorrhage [8]. The observation of diffuse alveolar haemorrhage in 37.50% of cases in the present study was consistent with findings from Das S et al., who found 30% and Mothakapalli J et al., who reported a rate of 37.6% [7,9]. Additionally, the incidence of emphysema at 6.25% aligns with the 7.1% reported by Sankappa PS et al., Other organs, including the spleen and brain, displayed intraparenchymal haemorrhage, likely resulting from the indirect anticoagulant effects of the rodenticide [6].
Limitation(s)
The limitation of this study was that cases where the cause of death was not known could not be included in the study group.
Conclusion(s)
The liver and kidneys are the most commonly affected organs in rat poison cases, as they play key roles in detoxification and excretion, whereas other organ such as lung, spleen, brain and heart are least affected. Early treatment targeting the primary organs involved in rodenticide poison can significantly increase survival rates of affected individual. Additionally, incorporating yoga after treatment can prevent suicidal tendencies and improve mental health issues like depression and anxiety. Yoga techniques like mindfulness meditation and breathing exercises offer cognitive and emotional benefits to the patients.