The treatment of intertrochanteric fractures, especially unstable fractures in the elderly remains a challenge for orthopaedists [1]. There is no consensus on the ideal implant for its treatment. The main goal of treatment is a stable fixation that promotes early postoperative mobilisation and better healing. Evidence indicates that intramedullary nail is one of the best implants available for its fixation and hence, better clinical outcomes [2]. Intertrochanteric fractures are relatively common among the elderly, 90% of such fractures occurring in those aged over 65 years [3]. Most elderly patients with intertrochanteric fractures have osteoporosis [3]. This type of geriatric fracture has relatively high mortality and causes severe impairment of function [4]. So, the main aim of surgery is early mobilisation of the patient. Unstable intertrochanteric fractures are those with significant disruption of the posteromedial cortex due to comminution, reverse oblique fractures or those with the subtrochanteric extension [5].
It is crucial to use a less invasive implant which allows early weight-bearing and has low complication rates. The selection of an implant is mainly decided by the fracture pattern (stable or unstable). Though there are many implant designs for the fixation of these types of fractures, most of them have many demerits such as mechanical disadvantages, less hold on the osteoporotic bone and early failures. PFNA devices have been introduced recently as an intramedullary option and PFNA-2 is its newer design [6]. These devices were developed to achieve better fixation strength, particularly in the presence of osteoporosis.
PFNA has many advantages such as shorter operative time, minimal fluoroscopy time, minimal blood loss and early weight-bearing [7]. Other advantages are fewer chances of implant failure, easier helical blade insertion (compared with a cumbersome lag screw and de-rotation screw insertion in PFN), lesser chances of postoperative hip pain, and better performance than any other implant [8].
This study was proposed to determine the role and result of unstable intertrochanteric fractures treated with PFNA-2 in geriatric patients. Moreover, in this study, the authors focused on the impact of fracture type, according to the AO classification and role of restoration of radiological parameters in the overall anatomical and functional results. It was hypothesised that unstable fractures according to the AO classification treated with PFNA-2 would show a greater sta-bility and better functional outcome.
Materials and Methods
A prospective analytical study was conducted on 35 patients with intertrochanteric femur fracture operated with PFNA-2 implant between January 2018 to December 2018 at Government Medical College, Kozhikode, Kerala, India. The study was approved by the Institutional Ethical Committee (Ref.No:GMCKKD/ RP 2018/IEC/53). Written informed consent was obtained from all subjects before enrollment in the study. Sample size was calculated according to 4pq/d2 formula.
Inclusion and Exclusion criteria: Patients with types 31-A2.2, 31-A2.3, 31-A3.1, 31-A3.2, 31-A3.3 (unstable intertrochanteric femur fracture) as per AO classification [9], and aged more than 60 years were included. Patients with stable fractures, not willing or unable to follow-up for one year, died before final follow-up, pathological fractures (except osteoporosis), polytrauma patients, unfit for surgery and those with previous implant in the injured hip were excluded.
Closed reduction under fluoroscopic guidance was used as the method of reduction of the fracture. Injection cefazolin was the prophylactic antibiotic used within an hour of skin incision and it was continued for the first 48 hours. Further continuation of antibiotic was decided based on the healing status of surgical wound. TAD was used to evaluate the placement of the helical blade in the femoral head and the quality of fixation [10]. The quality of reduction was also assessed by taking the difference of neck-shaft angle between operated and normal hip. A difference of less than 5° was graded as excellent, between 5 and 10° as good, and >10° as poor [11]. The MB software in the hospital’s computed radiographic system was used to measure the values for avoiding bias. Active range of motion exercises and partial weight-bearing mobilisation was started on the first postoperative day. All the complications were noted. The Radiographic Union Score for Hip (RUSH) score for the assessment of union based on the presence of bridging callus at the fracture site was used. Osteoporosis was assessed using Singh index and it was treated with oral ibandronate150 mg monthly for six months in all the cases [12]. The final follow-up was carried out at 12 months with a Modified Harris Hip Score (MHHS) [13].
Statistical Analysis
The results were assessed using Student’s t-test, and Chi-square test. A p-value of less than 0.05 was considered significant. The results were entered in MS Excel spreadsheets, and statistical analysis was performed using Statistical Package for Social Sciences (SPSS) version 16.0.
Results
There were 35 patients with a mean age of 65.6 years (range=60-84). In 28 patients, fractures were caused by a trivial fall and in the rest by road traffic accidents. Most of the patients (24, 68.57%) belonged to ASA Class 3 (American Society of Anesthesiologists Classification). Patient’s demographics and preoperative data are shown in [Table/Fig-1].
Demographic and preoperative data.
| Variables | Values |
|---|
| Age (Years) | 60-84 (65.6) |
| Sex (Male: Female) | 22:13 |
| Side (Right: Left) | 17:18 |
| *AO/OTA Fracture type (Number of patients) |
| 31-A2.2 | 18 |
| 31-A2.3 | 17 |
| Medical Co-morbidities |
| Cardiovascular diseases | 18 |
| Diabetes | 14 |
| Hypertension | 35 |
| Neurological illness | 1 |
| Renal disease | 1 |
*AO/OTA denotes Association for Osteosynthesis/Orthopaedic trauma association
Patients with good fracture reduction, i.e., neck-shaft angle difference less than 5 degrees, had better functional outcomes (p-value <0.019). There was a significant association between TAD and functional outcome (p-value=0.001). All surgeries were carried out within a mean of 7.84 days (range 3-14 days) from the date of injury. Closed reduction under fluoroscopic guidance was possible in all cases [Table/Fig-2].
a) Preoperative radiographs of a 65-year-old female with a right AO-OTA 31-A2.2 multi-fragmentary trochanteric fracture; b) Clinical photograph of surgical exposure and; c) Shows peroperative X ray pictures.
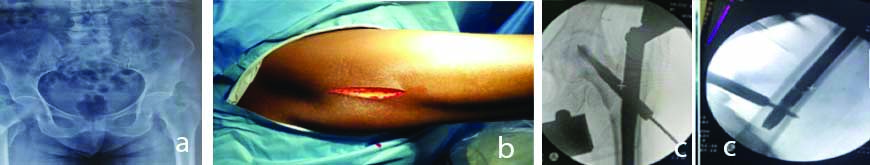
Mean operative time (skin-to-skin) was 55 minutes (range=30-90 minutes). The commonly used PFNA-2 nail was 10 mm in diameter, which was used in 28 patients. In the remaining patients, 9 mm nails were used. The most frequently used nail length was 200 mm and commonly used blades were between 90-105 mm.
The fracture reduction was evaluated in the first postoperative radiographs [Table/Fig-3] and subsequently at third month and after one year [Table/Fig-4]. The mean hospital stay was 8.8 days (range=4-18). Sutures were removed on 10th postoperative day. In the mean follow-up period of 12 months, functional results according to modified HHS were found to be excellent in 6 (17.1%) patients, good in 14 (40%) patients, fair in 12 (34.3%) patients, and poor in 3 (8.6%) patients. The average HHS in this study was 81.6. Patients with delay in surgery had poor HHS which was statistically significant (p-value=0.036).
Fracture reduction assessment with radiological parameters.
| Fracture reduction assessment | Number of patients | Percentage |
|---|
| *TAD <25mm | 34 | 97.1 |
| Neck-shaft angle difference <5° | 22 | 62.9 |
| Neck-shaft angle difference <5°-10° | 12 | 34.3 |
| Neck-shaft angle >10° | 1 | 0.35 |
| Centre-centre placement of helical blade not achieved | 30 | 85.7 |
*TAD denotes Tip apex distance
Radiographs of a 65-year-old female with a right AO-OTA 31-A2.2 trochanteric fracture. (a) Immediate postoperative view (b) One month follow-up X-ray shows healing (c) and (d) six months and one year follow-up X-rays which shows healed fractures; the patient was able to walk with no crutch and no pain or discomfort from two months after surgery.
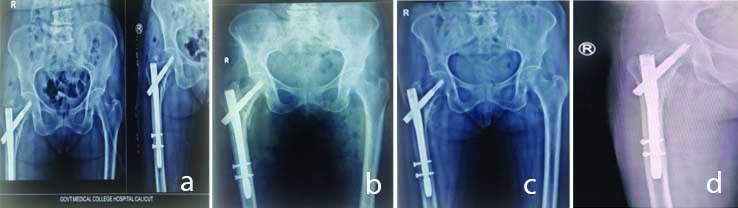
The relationship between functional outcome with operating time did not show significance (p-value=0.888) [Table/Fig-5]. The mean time of union, based on RUSH score, was about 14.11 weeks (Range:12 to 18 weeks). There is a linear relationship between functional outcome and age [Table/Fig-6]. Younger patients had better clinical and functional scores (p=0.001). In this study, there were 6 cases (17.1%) with excellent results and most of them were younger and who had type 31-A2.2 and 31-A2.3 fractures with no postoperative complications.
The relationship between operating time and functional outcome.
| Time | Excellent % | Good % | Fair % | Poor % |
|---|
| <60 min | 17.2 | 41.4 | 34.5 | 6.9 |
| 61-90 min | 16.7 | 33.3 | 33.3 | 16.7 |
Relationship between functional outcome and age.
| Age (years) | *HHS outcome |
|---|
| Excellent | Good | Fair | Poor |
|---|
| 60-69 | Number | 6 | 8 | 4 | 2 |
| % within age | 30% | 40% | 20% | 10% |
| 70-79 | Number | 0 | 5 | 5 | 0 |
| % within age | 0% | 50% | 50% | 0% |
| >80 | Number | 0 | 1 | 3 | 1 |
| % within age | 0% | 20% | 60% | 20% |
*HHS denotes Harris hip scores The younger patients had better clinical and functional scores (p=0.001)
There were implant-related complications such as lateral cortex nail impingement in two patients, screw back out in three patients, and fracture at the tip of the nail in one patient. Two patients with varus collapse and screw back out, were treated by exchange nailing. Longer nail was used for exchange nailing in those with fracture at the tip of the nail. Other postoperative complications are shown in [Table/Fig-7] and all were managed promptly. There was no statistical correlation between wound infection and clinico-radiological outcomes in this study (p-value=0.098).
Postoperative complications.
| Complications | Number of patients | Percentage | Treatment offered |
|---|
| Chest Infection | 2 | 5.714 | Antibiotics and Nebulisation |
| Urinary tract infection | 1 | 2.86 | Antibiotics |
| Deep vein thrombosis | 1 | 2.86 | Anticoagulants |
| Superficial wound infection | 1 | 2.86 | Antibiotics and wound care |
| Varus collapse and screw back out | 2 | 5.714 | Exchange nailing |
| Fracture at the tip of the nail | 1 | 2.86 | Exchange nailing with Longer nail |
Discussion
Unstable intertrochanteric fractures are a challenging situation for an average orthopaedic surgeon. Among the many implants designed for its treatment, based on different biomechanics, PFNA is being accepted in a big way [7,14,15]. The second version of PFNA-2 was designed with a flattened lateral surface, decreased mediolateral nail angle, and decreased proximal nail diameter to address the issues such as lateral cortex impingement reported with PFNA [8].
This study shows that stable type fractures had better clinical and functional outcomes which was statistically significant. Urgent surgical intervention is necessary for all geriatric hip fractures, as it not only avoids the development of many known complications such as hypostatic pneumonia, catheter sepsis, cardiorespiratory failure, bedsores but also allows early rehabilitation and mobilisation [8]. Most patients in this series were operated within eight days following admission in the hospital (85.7%). But in some patients operative procedure was delayed due to medical co-morbidities. In this study, patients with delay in surgery had poor HHS which was statistically significant. Delay in surgery prolongs the immobilisation period thereby, deteriorating the patient’s condition physically, physiologically, and psychologically [8]. Most of the surgeries performed in this series were completed within 60 minutes. The average surgical time as reported by others authors was 58.4 minutes [8]. In this study, the relationship between functional outcomes with operating time did not have much significance.
The RUSH score have been used for the the RUSH score for the assessment of union based on the presence of bridging callus at the fracture site and the average time of union in majority of our patients was about 14 weeks.
In this study, patients with good fracture reduction, i.e., neck-shaft angle difference less than 5 degrees with normal side had better functional outcomes. Quality of fixation was assessed using TAD [16] and there was a significant association between TAD and functional outcome.
Present study shows a linear relationship between functional outcome and age, where younger patients had better clinical and functional scores. Another important finding noticed was most patients with fair and poor results were older, with postoperative complications or those having more unstable types of fractures. Here, fixation of intertrochanteric fractures in elderly with PFNA-2 provides a good outcome with very few complications, high union rate, and early postoperative mobilisation. The complication rates were comparable to another study [17]. There was only one patient of superficial wound infection.
Limitation(s)
The sample size was limited. Studies with larger sample size over a large population would make the consensus clear and to affirm the recommendation of PFNA 2 for management of intertrochanteric fractures.
Conclusion(s)
PFNA-2 is a dependable implant for the fixation of unstable intertrochanteric fractures in the elderly. It has good to excellent outcomes and takes less operative time with low complication rates. The age of the patient is an important factor in predicting functional outcome. The operating time did not have much significance on functional outcome. The proper operative technique to maintain the neck-shaft angle difference of fewer than 5 degrees and TAD <25 mm are important for achieving fracture stability and to avoid major complications.
*AO/OTA denotes Association for Osteosynthesis/Orthopaedic trauma association
*TAD denotes Tip apex distance
*HHS denotes Harris hip scores The younger patients had better clinical and functional scores (p=0.001)