Introduction
Adhesive capsulitis is a self-limiting regional skeletal condition of uncertain aetiology characterised by a progressive loss of both active and passive mobility of the glenohumeral joint in the shoulder complex. It begins insidiously with shoulder pain and dysfunction in middle aged and elderly population. Adhesive capsulitis predominantly affects the older population, affecting both the sexes; however, female patients are affected more.
Aim
To find the effect on pain, Range of Motion (ROM) and disability in subjects with adhesive capsulitis treated with hot pack along with caudal glide versus hot pack along with antero-posterior glide mobilisation.
Materials and Methods
The study, quasi experimental, was conducted on 80 subjects which were further divided into two groups with 40 subjects in each groups. Subjects were evaluated for pain, ROM and disability index. Group A received antero-posterior glide mobilisation with the hot pack, whereas Group B received caudal glide mobilisation with hot pack for thrice a week for total three weeks completing a total of nine sessions. The statistical analysis was done using one-way ANOVA and post-hoc analysis and Independent t-test was used for calculating within and between group differences. The parameters that were measured were Visual Analogue Scale (VAS), ROM, Shoulder Pain and Disability Index (SPADI).
Results
The p-value after three weeks between the groups was 0.02, 0.0001, and 0.014 for VAS, ROM and disability. There was significant difference in the pre and post values in both Group A and Group B. Post-treatment values of VAS (p=0.0001), ROM (p=0.0001), and SPADI (p=0.0001) in Group B were showed more improvement than the post-treatment values of VAS, ROM and SPADI in Group A.
Conclusion
Caudal glide mobilisation is more effective in improving pain, abduction ROM and SPADI index in patients with adhesive capsulitis.
Introduction
Adhesive capsulitis is a self-limiting regional skeletal condition of uncertain aetiology characterised by a progressive loss of both active and passive mobility of the glenohumeral joint in the shoulder complex [1]. The incidence of adhesive capsulitis in the general population is around 3% to 5% but as elevated as 20% in patients with diabetes. It is estimated that 70% of patients with adhesive shoulder capsulitis are women [2]. The risk factors associated with adhesive capsulitis include diabetes mellitus, prolonged shoulder immobility, thyroid disease, hypertension, hypercholesterolemia and postoperative heart diseases and other systemic diseases [3].
Loss of motion of greater than 25% in atleast two planes, a 50% loss of passive External rotation, or less than 30° of External rotation are indicative of a patient with Frozen shoulder [4]. Identifying risk factors for a disease is one of the methods used to gain and understand the aetiology of adhesive capsulitis. In a long-term study of the natural history of frozen shoulder, concluded that the disease is self-limiting; however, many patients suffer for more than three years with an average duration of 30.1 months. A disability of this duration can obviously place severe emotional and economic hardship on the affected individuals [5]. In long term patients, the pain and restricted shoulder motion induces disability, severe emotional and economic hardship on the afflicted person. Most patients are unwilling to suffer this pain, prolonged disability, and sleep deprivation without seeking treatment [6].
In adhesive capsulitis, there is global loss of both passive and active range of motion of the glenohumeral joint with external rotation usually being the most restricted physiologic movement [7]. Most of the adhesive capsulitis patients initially experience a phase of pain, which progresses to a freezing phase when glenohumeral motion is lost, followed by a thawing phase in which pain gradually subsides and most of the lost motion returns. Based on the symptoms, adhesive capsulitis is divided in three stages: Stage I (freezing stage) is mainly characterised by pain usually lasting 2-9 months. In Stage II (frozen stage); pain gradually subsides and ROM decreases but stiffness is marked, lasting 4-12 months. In Stage III (thawing phase); constitute gradual relief from the symptoms and recovery of range of motion pain and lasts from 5 to 24 months [8].
There is currently no gold standard for diagnosis, nor have validated diagnostic criteria been published in the literature [9,10]. With respect to physical therapy, a variety of interventions are used; these include heat or ice applications, modalities, mobilisations, exercises, Proprioceptive Neuromuscular Facilitation (PNF) among other [11].
Choosing a mobilisation technique is dictated by the “concave-convex rule”: if a convex surface moves on a concave surface, rolling and gliding movements of the joint surfaces must occur in the opposite directions, and in the same direction if the joint surface configuration is reversed [12,13]. Accordingly, as the humerus abducts, its head rolls superiorly, but glides in an inferiorly direction unless restrained by the inferior glenohumeral ligament. The caudal glide mobilisation involves an inferiorly directed force on the abducted proximal humerus to generate an inferior translation of the head of the humerus. For this reason, the caudal mobilisation is recommended by many authors as the appropriate technique to treat glenohumeral abduction hypo mobility [14].
According to the “circle stability concept,” the primary restraint to the translation of the humeral head is part of the joint capsule and ligaments located in the direct path of translation [15]. Applying the antero-posterior mobilisation at a joint angle close to its end range might be a good alternative for treating abduction hypo mobility since the inferior glenohumeral ligament is preferentially stressed in this position. During the antero-posterior glide mobilisation, a posteriorly directed force is applied by the therapist to the head of the humerus, causing it to translate posteriorly. For this reason, anterior-posterior glide and caudal glide are frequently employed by physical therapists to mobilise the shoulder joint. During the antero-posterior glide mobilisation, a posteriorly directed force is applied by the therapist to the head of the humerus, causing it to translate posteriorly [14].
In addition to mobilisation techniques, heating modalities are also used as an adjuvant therapy for managing patients with adhesive capsulitis [16]. Heat has been used therapeutically for thousands of years. It offers immediate relief and can increase circulation to speed the healing process after the injury [17]. Moist heat appears to be more advantageous in pain relief than other dry heat modalities such as electric heat pads [18].
A study investigating the effects of superficial thermal agents and shoulder stretching exercises in normal subjects found that the use of superficial heat in combination with low-load long-lasting stretching created more extensive changes in the extensibility of soft tissue than did stretching alone. The authors proposed that a superficial thermal agent can lead to muscle relaxation, thus reducing the resistance to stretches within and around the muscle, and as a result increasing the ROM of the shoulder [16,19]. This study may help to identify and treat the cause for pain, loss of Range of Motion (ROM), and shoulder disability using the better technique. The aim of this study was to compare the effect of two different mobilisation techniques along with hot pack treatment in improving the abduction range of motion in patients with adhesive capsulitis.
Materials and Methods
The study design was quasi-experimental pre and post study design, the study setting was the In-Patient and Out Patient Department of Orthopaedics, Kempegowda Institute of Medical Sciences, (KIMS) Hospital and RI, Bangalore and the Out Patient Department of Physiotherapy at Kempegowda Institute of Physiotherapy (KIPT), Bangalore. The total study Period was one year, April 2018 to April 2019.
The ethical clearance was obtained from the Institutional Ethical Committee members with Ethical approval no-KIPT/592/A/17-18 Dated: 23-03-2018, with informed consent obtained from all the study samples, acquired sample size was 88 with a 10% dropout. Net sample size 80.
Inclusion and Exclusion criteria: Subjects who fulfill the inclusion criteria were assigned into two groups. Subjects between the age range of 40-60 years, who had symptoms atleast for 1 month, were diagnosed cases of adhesive capsulitis freezing stage and had painful restriction more than 50% of shoulder abduction movement and showed capsular pattern of movement restriction were selected. Of the 80 selected samples 42 were female and 38 were male. Subjects diagnosed with any previous history of shoulder surgery, Tuberculosis (TB) shoulder, cancer shoulder, chronic arthritis, administration of corticosteroid injection to the affected shoulder within last two months, any other shoulder problem or pregnant women were excluded from the study. All subjects were evaluated before starting the treatment for pain, shoulder abduction range of motion, and shoulder disability.
No blinding was done, Group A was given antero-posterior glide performed at the rate of 2-3 glides/second for 30 seconds. About five such sets were given in every session, thrice a week for total three weeks [Table/Fig-1].
Antero-posterior glide mobilisation.
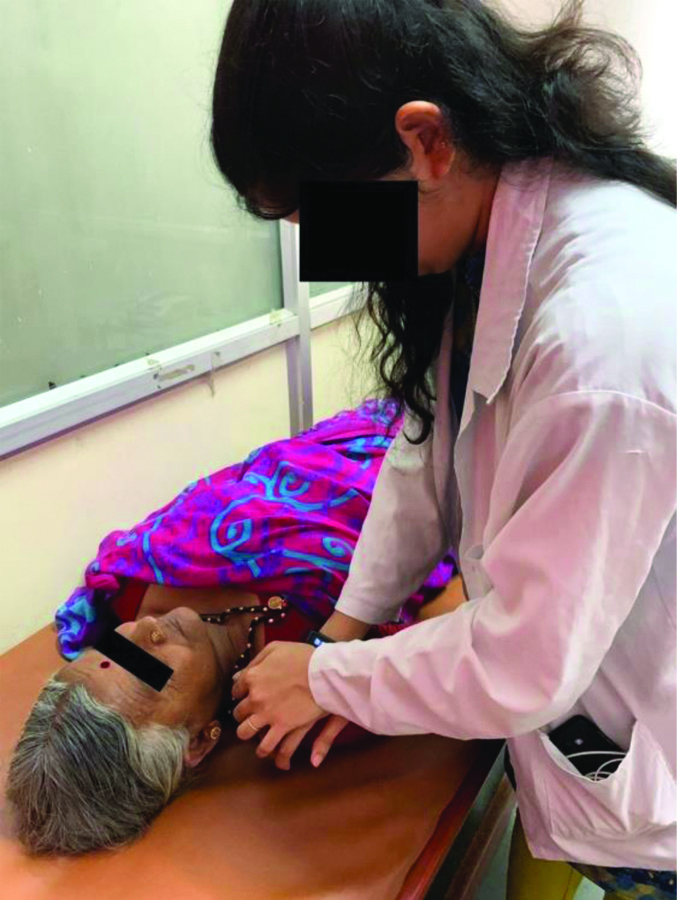
Group B was given caudal glide performed at the rate of 2-3 glides/second for 30 seconds. About five such sets were given in every session, thrice a week for three weeks [Table/Fig-2].
Caudal glide mobilisation.
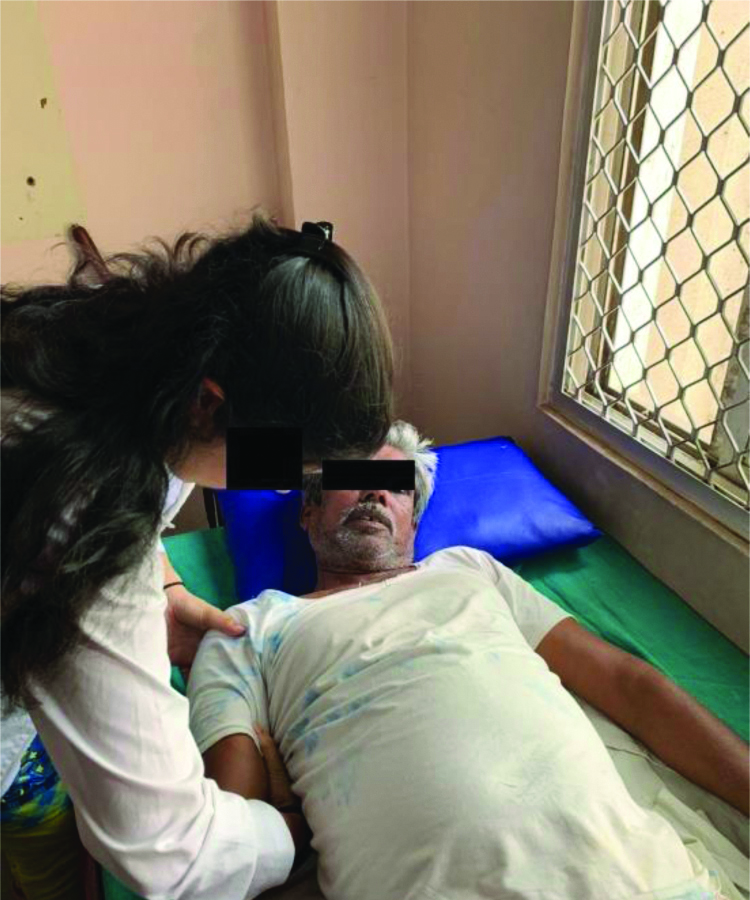
All subjects re-evaluated post one week and post three weeks of the treatment. Outcome measures included the evaluation of pain using VAS, shoulder abduction ROM using a full-circle goniometer and shoulder disability index using Shoulder Pain And Disability Index (SPADI) [20,21].
Statistical Analysis
Data was analysed using the Statistical Package for the Social Science (SPSS) 19.0 (SPSS Inc., Chicago, IL) and level of significance was set at p<0.05. Descriptive statistics was performed to find out the mean and standard deviation of the respective groups. ANOVA test followed by Post-hoc analysis was used within the groups to find out the statistical significance. Independent t-test was used between the groups to find out the significance.
Results
The mean age of the subjects were 53.15±6.74 in Group A and 51.7±6.07 in Group B, (p-value=0.30) which was statistically not significant [Table/Fig-3].
Comparison of Age between Group A and Group B.
| Groups | Mean | SD |
|---|
| Group A | 53.15 | 6.74 |
| Group B | 51.7 | 6.07 |
| p-value (t-test) | 0.30 |
Both Group A and Group B comprised of 52.5% males and 47.5% females. t-test analysis showed that the p-value was 1, i.e., data was not statistically significant, hence, both the groups are comparable. (p>0.05) [Table/Fig-4].
Gender Distribution between Group A and Group B.
| Groups | Number | Percentage (%) |
|---|
| Group A | Males | 21 | 52.5 |
| Females | 19 | 47.5 |
| Group B | Males | 21 | 52.5 |
| Females | 19 | 47.5 |
| p-value | 1 |
The comparison of VAS after ANOVA followed p-value after ANOVA followed by post-hoc within Group B was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant [Table/Fig-5].
Comparison of VAS within Group A and Group B.
| Group A | Group B |
|---|
| Pre-treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post three weeks |
|---|
| Mean | 8.4 | 7.47 | 6.25 | 8.1 | 7.2 | 5.72 |
| Standard deviation | 0.90 | 0.96 | 0.98 | 0.92 | 1.01 | 1.15 |
| p-value (ANOVA) | 0.0001* | 0.0001* |
| p-value (Pre-treatment vs Post one week) | 0.0001* | 0.0001* |
| p-value (Pre-treatment vs Post three weeks) | 0.0001* | 0.0001* |
| p-value (Post one week vs post three weeks p-value (t-test) | 0.0001* | 0.0001* |
Statistical analysis within the Group A and Group B was performed using ANOVA followed by post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
The p-value in comparison of ROM after ANOVA p-value after ANOVA followed by post-hoc within Group B was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant [Table/Fig-6].
Comparison of abduction Range of Motion (ROM) within Group A and Group B.
| Group A | Group B |
|---|
| Pre-treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post one weeks |
|---|
| Mean | 72.85 | 82.27 | 99.45 | 74.37 | 90.65 | 123.52 |
| Standard deviation | 10.97 | 11.39 | 11.97 | 11.20 | 11.80 | 13.78 |
| p-value (ANOVA) | 0.0008* | 0.0001* |
| p-value (Pre-treatment vs Post one week) | 0.0001* | 0.0001* |
| p-value (Pre-treatment vs Post three weeks) | 0.0001* | 0.0001* |
| p-value (Post one week vs Post three weeks) | 0.0001* | 0.0001* |
Statistical analysis within the Group A and Group B was performed using ANOVA followed by post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0008, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
The comparison of SPADI score after ANOVA followed by Post- hoc p-value after ANOVA followed by post-hoc within Group B was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant [Table/Fig-7].
Comparison of SPADI Score within Group A and Group B.
| Group A | Group B |
|---|
| Pre-treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post three weeks |
|---|
| Mean | 83.16 | 77.45 | 68.56 | 82.67 | 74.74 | 65.06 |
| Standard deviation | 5.97 | 6.06 | 6.04 | 4.64 | 5.20 | 6.48 |
| p-value (ANOVA) | 0.0001* | 0.0001* |
| p-value (Pre-treatment vs Post one week) | 0.0001* | 0.0001* |
| p-value (Pre-treatment vs Post three weeks) | 0.0001* | 0.0001* |
| p-value (Post one week vs Post three weeks) | 0.0001* | 0.0001* |
Statistical analysis within the Group A and Group B was performed using ANOVA followed by Post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
The p-value after independent t-test between pre-treatment of Group A and Group B was 0.14, post one week between Group A and Group B was 0.22 and post three weeks between Group A and Group B was 0.02; of which the p-value post three weeks of treatment between both groups was statistically significant. Group A showed an improvement of 25.5% after three weeks, Group B showed an improvement of 29.6%; hence, Group B showed more improvement than Group A [Table/Fig-8].
Comparison of VAS between Group A and Group B.
| Group A | Group B |
|---|
| Pre-treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post three weeks |
|---|
| Mean | 8.4 | 7.47 | 6.25 | 8.1 | 7.2 | 5.72 |
| Standard deviation | 0.90 | 0.96 | 0.98 | 0.92 | 1.01 | 1.15 |
| Percentage improvement | 25.5% | 29.6% |
| p-value (Group A vs Group B Pre-treatment) | 0.14 |
| p-value (Group A vs Group B Post one week) | 0.22 |
| p-value (Group A vs Group B Post three weeks) | 0.02* |
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant
The p-value after independent t-test between pre-treatment of Group A and Group B was 0.54, post one week between Group A and Group B was 0.001 and post three weeks between Group A and Group B was 0.0001; of which the p-values post one week and post three weeks of treatment between both groups were statistically significant. Group A showed an improvement of 36.5% after three weeks, Group B showed an improvement of 66.08%; hence, Group B showed more improvement than Group A [Table/Fig-9].
Comparison of abduction ROM between Group A and Group B.
| Group A | Group B |
|---|
| Pre-Treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post three weeks |
|---|
| Mean | 72.85 | 82.27 | 99.45 | 74.37 | 90.65 | 123.52 |
| Standard deviation | 10.97 | 11.39 | 11.97 | 11.20 | 11.80 | 13.78 |
| Percentage improvement | 36.5% | 66.08% |
| p-value (Group A vs Group B Pre-treatment) | 0.54 |
| p-value (Group A vs Group B Post one week) | 0.001* |
| p-value (Group A vs Group B Post three weeks) | 0.0001* |
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant
Group A showed an improvement of 17.5% after three weeks, Group B showed an improvement of 19.3%; hence, Group B showed more improvement than Group A [Table/Fig-10].
Comparison of SPADI Scores between Group A and Group B.
| Group A | Group B |
|---|
| Pre-treatment | Post one week | Post three weeks | Pre-treatment | Post one week | Post three weeks |
|---|
| Mean | 83.16 | 77.45 | 68.56 | 82.67 | 74.74 | 65.06 |
| Standard deviation | 5.97 | 6.06 | 6.04 | 4.64 | 5.20 | 6.48 |
| Percentage improvement | 17.5% | 19.3% |
| p-value (Group A vs Group B Pre-treatment) | 0.68 |
| p-value (Group A vs Group B Post one week) | 0.03* |
| p-value (Group A vs Group B Post three weeks) | 0.014* |
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant; p-value after independent t-test between pre-treatment of Group A and Group B was 0.68, post one week between Group A and Group B was 0.03 and post three weeks between Group A and Group B was 0.014; of which the p-values post one week and post three weeks of treatment between both groups were statistically significant
Discussion
The mean age in Group A (antero-posterior glide mobilisation group) was 53.15±6.74 and in Group B (caudal glide mobilisation group) was 51.7±6.07. Sarkari E et al., also had conducted a study on the same age group adhesive capsulitis patients. As per the gender distribution analysis, Group A had 52.5% female subjects and 47.5% male subjects [22]. The study further concluded that although antero-posterior glide mobilisation is effective in increasing the abduction range of motion, it is not as effective as the traditional caudal glide mobilisation.
Similarly, Group B had 52.5% female subjects and 47.5% male subjects; the female subjects were more in number than male subjects. In a similar study conducted by Yang JL et al., in the year 2007, the number of female subjects exceeded the number of male subjects [23].
The results from the present study showed that there is a significant improvement in the VAS scores of the subjects before the treatment and after three weeks of treatment. In a similar study done by Agarwal S et al., significant improvement was noted in VAS scores after the intervention of caudal glide and antero-posterior glide mobilisation [24].
A study by Vermeulen HM et al., conducted in the year 2006, showed significant improvement in abduction ROM in the post values after using caudal glide and antero-posterior glide mobilisation [25]. Similarly in the present study, there were significant improvements in the pre and post values of the abduction ROM after the three week protocol.
In 2012, Kumar A et al., conducted a study and concluded that there was significant improvement in the SPADI scores after giving mobilisation techniques in subjects with adhesive capsulitis [26]. The present study also showed similar results. The SPADI scores improved significantly after three weeks of using the mobilisation techniques. However, more significant results were observed in Group B than Group A in regard to VAS, abduction ROM and SPADI. Yet another study by Nicholson GG, also concluded that shoulder abduction range of motion significantly improved in the subjects with adhesive capsulitis who were given mobilisation techniques [27].
Thermotherapy is generally soothing and psychologically relaxing, thereby favourably modifying emotional response to pain and further reducing painful muscle spasm [19].
The detailed mechanical behaviour and biomechanical changes that occur with caudal glide mobilisation are not very clear. The tissue targeted for stretching during caudal glide procedure is believed to be the caudal glenohumeral ligament as the head of the humerus glides downward relative to the glenoid fossa. This is based on the concave-convex rule. Antero-posterior glide can effectively be used to increase abduction range when given at the end of the available range. It can also be used as a substitute to caudal glide, though caudal glide in the most effective [22].
Limitation(s)
The number of subjects in the present study was less. Further studies can comprise a larger sample size. The current study was not of long duration. To study the long term effect of the techniques, future studies can be undertaken for longer period of time. There was no inclusion of control group in the present study. Control group can be added for further accuracy in the study. The age variation in this study was of 20 years, ranging from 40 years to 60 years. The patient’s that were built in the study were variable. Reducing age variation could be recommended for further research. Since, adhesive capsulitis is a self-limiting disease; the actual improvement throughout the treatment in this study could not be evaluated. Proper strengthening program was not followed after mobilisation sessions due to lack of time. Further studies may include a proper strengthening program for better prognosis of the subjects.
Conclusion(s)
The study showed that both antero-posterior glide mobilisation and caudal glide mobilisation were effective in improving VAS score, shoulder abduction ROM and SPADI score. It also established that caudal glide is more effective than antero-posterior glide mobilisation in improving abduction ROM in patients with adhesive capsulitis.
Statistical analysis within the Group A and Group B was performed using ANOVA followed by post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
Statistical analysis within the Group A and Group B was performed using ANOVA followed by post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0008, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
Statistical analysis within the Group A and Group B was performed using ANOVA followed by Post-hoc and independent t-test; *p<0.05 statistically significant; p-value after ANOVA followed by post-hoc within Group A was 0.0001, p-value after independent t-test among pre-treatment, post one week and post three weeks was 0.0001; all of which were statistically significant
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant
Statistical analysis between Group A and Group B was performed using independent t-test and percentage improvement; *p<0.05 statistically significant; p-value after independent t-test between pre-treatment of Group A and Group B was 0.68, post one week between Group A and Group B was 0.03 and post three weeks between Group A and Group B was 0.014; of which the p-values post one week and post three weeks of treatment between both groups were statistically significant
[1]. Nevieaser RJ, Neviaser TJ, The frozen shoulder. diagnosis and managementClin Orthop Relat Res 1987 223:59-64.10.1097/00003086-198710000-00008 [Google Scholar] [CrossRef]
[2]. Le HV, Lee SJ, Nazarian A, Rodriguez EK, Adhesive capsulitis of the shoulder: Review of pathophysiology and current clinical treatmentsShoulder Elbow 2017 9(2):75-84.10.1177/175857321667678628405218 [Google Scholar] [CrossRef] [PubMed]
[3]. Milgrom C, Novack V, Weil Y, Jaber S, Radeva-Petrova DR, Finestone A, Risk factors for idiopathic frozen shoulderIsr Med Assoc J 2008 10(5):361-64. [Google Scholar]
[4]. Skirven TM, Osterman AL, Fedorczyk J, Amadio PC, Rehabilitation of the Hand and upper extremityMosby. set. (6th ed.) 2011 6(2):901182 [Google Scholar]
[5]. Weiser HI, Painful primary shoulder mobilisation under local anesthesiaArch Phys Med Rehabil 1977 58(9):406-08. [Google Scholar]
[6]. Mao CY, Jaw WC, Cheng HC, Frozen shoulder: correlation between the response to physical therapy and follow-up shoulder arthrographyArch Phys Med Rehabil 1997 78(8):857-59.10.1016/S0003-9993(97)90200-8 [Google Scholar] [CrossRef]
[7]. Diercks RL, Stevens M, Gentle thawing of the frozen shoulder: A prospective study of supervised neglect versus intensive physical therapy in seventy-seven patients with frozen shoulder syndrome followed up for two yearsJ Shoulder Elbow Surg 2004 13(5):499-502.10.1016/j.jse.2004.03.00215383804 [Google Scholar] [CrossRef] [PubMed]
[8]. Inayat F, Ali NS, Shahid H, Younus F, Prevalence and determinants of frozen shoulder in patients with diabetes: A single center experience from PakistanCureus 2017 9(8):e154410.7759/cureus.1544 [Google Scholar] [CrossRef]
[9]. Loew M, Heichel TO, Lehner B, Intraarticular lesions in primary frozen shoulder after manipulation under general anesthesiaJ Shoulder Elbow Surg 2005 14(1):16-21.10.1016/j.jse.2004.04.00415723009 [Google Scholar] [CrossRef] [PubMed]
[10]. Ramirez J, Adhesive capsulitis: diagnosis and managementAm Fam Physician 2019 99(5):297-300. [Google Scholar]
[11]. Carette S, Moffet FN, Tardfiff J, Bessette L, Morin F, Frémont P, Intraarticular corticosteroid, supervised physiotherapy, or a combination of the two in the treatment of adhesive capsulitis of the shoulderArthritis Rheum 2003 48(3):829-38.10.1002/art.1095412632439 [Google Scholar] [CrossRef] [PubMed]
[12]. Mangus BC, Hoffman LA, Hoffman MA, Altenburger P, Basic principles of extremity joint mobilisation using a kaltenborne approachJournal of Sport Rehabilitation 2002 11(4):235-50.10.1123/jsr.11.4.235 [Google Scholar] [CrossRef]
[13]. Kaltenborn F, Manual Mobilisation of the Joints Vol 1: The Extremities 1989 4th Edition [Google Scholar]
[14]. Hsu AT, Ho L, Ho S, Hedman T, Joint position during anterior-posterior glide mobilisation: Its effect on glenohumeral abduction range of motionArch Phys Med Rehabil 2000 81(2):210-14.10.1016/S0003-9993(00)90143-6 [Google Scholar] [CrossRef]
[15]. Blasier RB, Goldburg RE, Rothman ED, Anterior shoulder stability: Contribution of rotator cuff forces and the capsular ligaments in a cadaver modelJ Shoulder Elbow Surg 1992 1(3):140-50.10.1016/1058-2746(92)90091-G [Google Scholar] [CrossRef]
[16]. Lentell G, Hetherrington T, Eagan J, Morgan M, The use of thermal agents to influence the effectiveness of a low-load prolonged stretchJ Orthop Sports Phys Ther 1992 16(5):200-07.10.2519/jospt.1992.16.5.20018796753 [Google Scholar] [CrossRef] [PubMed]
[17]. Petrofsky J, Lohman E III, Lee S, Cuesta ZDL, Labial L, Louciulescu R, Effects of contrast bath on skin blood flow on the dorsal and plantar foot in people with type ii diabetes and age-matched controlsPhysiother Theory Pract 2007 23(4):189-97.10.1080/0959398070120929517687732 [Google Scholar] [CrossRef] [PubMed]
[18]. Petrofsky J, Berk L, Alshammari F, Lee H, Hamdan A, Yim Je, The effect of moist air on skin blood flow and temperature in subjects with and without diabetesDiabetes Technol Ther 2012 14(2):105-16.10.1089/dia.2011.012822017463 [Google Scholar] [CrossRef] [PubMed]
[19]. Tepperman PS, Devlin M, The therapeutic use of local heat and coldCan Fam Physician 1986 32:1110-14. [Google Scholar]
[20]. Conroy DE, Hayes KW, The effect of joint mobilisation as a component of comprehensive treatment for primary shoulder impingement syndromeJ Orthop Sports Phys Ther 1998 28(1):03-14.10.2519/jospt.1998.28.1.39653685 [Google Scholar] [CrossRef] [PubMed]
[21]. Breckenridge JD, McAuley JH, Shoulder Pain and Disability Index (SPADI)J Physiother 2011 57(3):19710.1016/S1836-9553(11)70045-5 [Google Scholar] [CrossRef]
[22]. Sarkari E, Dhakshinamoorthy P, Multani NK, Comparison of caudal and anteroposterior glide mobilisation for the improvement of abduction range of motionJournal of Exercise Science and Physiotherapy 2006 2:59-65. [Google Scholar]
[23]. Yang JL, Chang CW, Chen SY, Wang SF, Lin JJ, Mobilisation techniques in subjects with frozen shoulder syndrome: Randomized multiple-treatment trialPhys Ther 2007 87(10):1307-15.10.2522/ptj.2006029517684085 [Google Scholar] [CrossRef] [PubMed]
[24]. Agarwal S, Raza S, Moiz JA, Anwer S, Alghadir AH, Effects of two different mobilisation techniques on pain, range of motion and functional disability in patients with adhesive capsulitis: A comparative studyJ Phys Ther Sci 2016 28(12):3342-49.10.1589/jpts.28.334228174448 [Google Scholar] [CrossRef] [PubMed]
[25]. Vermeulen HM, Rozing PM, Obermann WR, le Cessie S, Vliet Vlieland TP, Comparison of high-grade and low-grade mobilisation techniques in the management of adhesive capsulitis of the shoulder: Randomized controlled trialPhys Ther 2006 86(3):355-68.10.1093/ptj/86.3.35516506872 [Google Scholar] [CrossRef] [PubMed]
[26]. Kumar A, Kumar S, Aggarwal A, Kumar R, Das PG, Effectiveness of Maitland Techniques in Idiopathic Shoulder Adhesive CapsulitisISRN Rehabilitation 2012 2012:71023510.5402/2012/710235 [Google Scholar] [CrossRef]
[27]. Nicholson GG, The effects of passive joint mobilisation on pain and hypomobility associated with adhesive capsulitis of the shoulderJ Orthop Sports Phys Ther 1985 6(4):238-46.10.2519/jospt.1985.6.4.23818802309 [Google Scholar] [CrossRef] [PubMed]