Cervical cancer is the foremost malignancy in Indian women. Amongst female cancer, relative proportion of cancer cervix varied 14 to 24% in Indian women. Cervical cancer considered to be the most common genital cancer in all over the world and it account for 80% genital malignancy in India [1]. In India, incidence of cervical cancer is 23.5/100,000. Globally, more than 5,27,600 new cases are diagnosed each year with 2,65,700 deaths [2]. Fortunately, cervical cancer is both preventable and curable, provided that it is detected at an early stage by screening. The most important method for early diagnosis of cancer cervix is cytology screening. Papanicolaou (PAP) smear (LBC) is a simple, safe, painless and non-invasive method. LBC is effective method for detection of precancerous, cancerous and non-cancerous lesion in the cervix and vagina [3]. Pap smear has reduced the mortality of cervical cancer by up to 70% [4].
It is not possible to launch nationwide cytology screening programme of cervical cancer. So, this has led to the development of low cost technology e.g., visual inspection of the VIA. The attractive features of VIA include low cost, simple application, real time screening of results and accuracy as comparable to good quality LBC, minimal requirements of infrastructure, immediate results, and it can be performed by nursing sisters and trained paramedical workers [5]. So, an alternative technique aimed at eliminating subjects diagnosed by LBC, increasing sensitivity and eliminating the need for second visit, has to be pursued; thus VIA has been chosen for screening of cervical cancer.
Materials and Methods
The present cross-sectional study was conducted in the Department of Obstetrics and Gynaecology, at a tertiary care centre in rural area over the period of three year from July 2015 to June 2018. The protocol of this study was approved by the Institutional Review Board. (585/UPUMS/Dean/2015-2016/EC No. 2014/119). The informed written consent was obtained from every case in this study.
Total 1600 patients who presented to the department were screened for cervical cancer. The average number of women who attended Gynaecology OPD was 150 per day. Among them, women who fulfilled the selection criteria and given the proper consent were randomly selected. The inclusion and exclusion criteria for this study were:
Inclusion criteria: Persistent vaginal discharge, low backache, contact bleeding, postmenopausal bleeding, menstrual disorder and pain in lower abdomen.
Exclusion criteria: Women less than 21 year of age, prior hysterectomy or procedure on cervix, unmarried, pregnancy, obvious malignant growth on cervix, asymptomatic women and exogenous hormone.
About 1600 patients attending Gynaecology Outpatient Department with the following signs and symptoms of minimum duration for six month were included (as mentioned above). After taking informed consent, the cases were subjected to detailed history, physical examination, LBC, visual inspection test and colposcopy followed by biopsy (if required.) Biopsy was taken in patients who had a Reid Score >3. All method was done by senior consultant in same sitting.
Technique of Taking Cervical Smear (LBC)
Patient was laid in dorsal position and Cusco’s speculum was introduced to expose cervix. Any excessive vaginal discharge was wiped away. LBC was taken by a cytobrush which was introduced into the endocervical canal and transformation zone, then twisted at 360° and then withdrawn. The brush was immediately dipped in 95% ethyl alcohol and sent for pathological exam, where reporting was done according to Bethesda classification [5].
Method of doing VIA
Patient was laid in dorsal position. With proper aseptic measures, sterile speculum was introduced to visualise cervix. A 5% acetic acid was applied over cervix with a cotton swab. After one minute cervical changes were noted [Table/Fig-1,2].
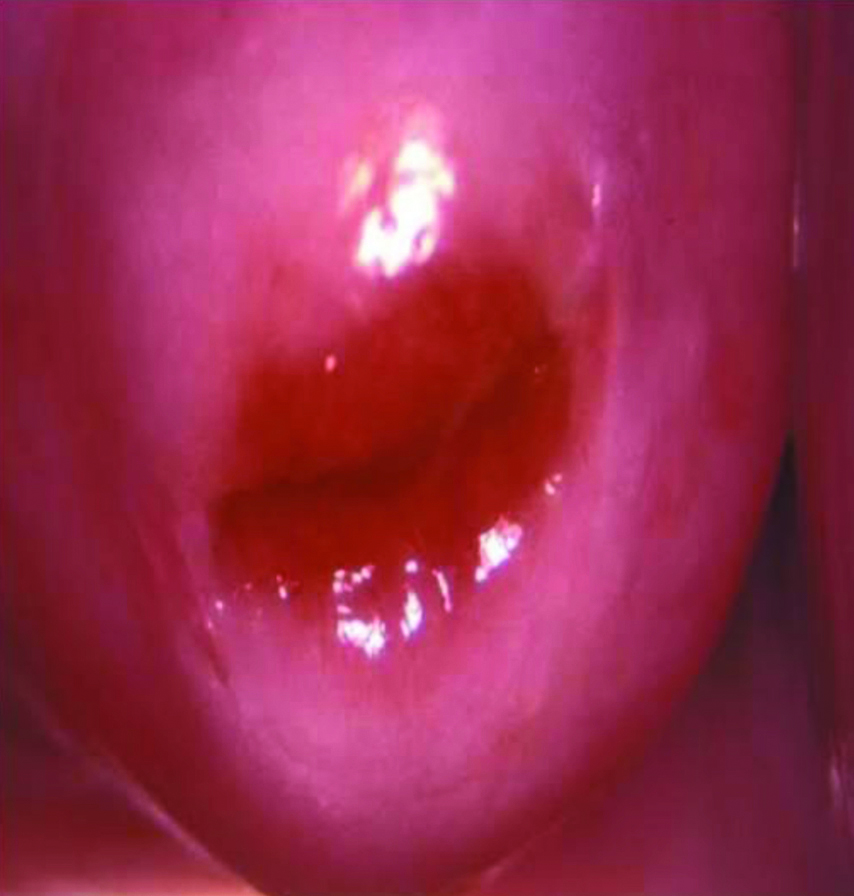
Acetowhite area seen during VIA.
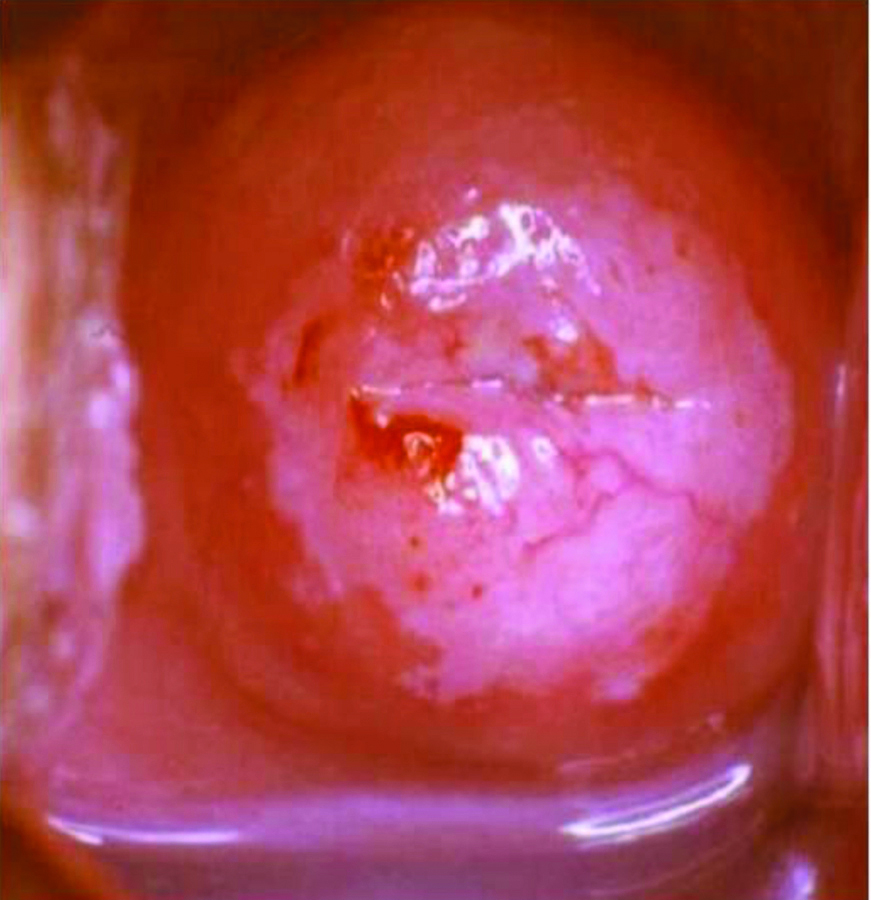
VIA Positive- Distinct and opaque acetowhite area, well defined margin, close to the transformation zone and not far away from the orifice.
VIA Negative- No acetowhite lesions, transport lesions or faint patchy lesions without definite margins and acetowhite lesions far away from the transformation zone.
Techniques of doing Colposcopy
The patient was laid in dorsal position on the examining table and the colposcope was placed towards the patient. The cervix was then exposed with a self-retaining Cusco’s speculum. Excessive discharge was mopped with swabs gently dipped in normal saline and firstly, the examination of the cervix was done under low power magnification. Normal saline dissolves the excessive mucous and provides a refractory medium for better visualisation of the cervix under green filter. The cervix was examined after application of acetic acid and Lugol’s iodine. Interpretation was done under Reid score system [6,7]. Biopsy was taken in patients who had a Reid Score >3.
Statistical Analysis
The sensitivity and specificity of each test are determined and compared. Data entry and analysis were done using Statistical Package For The Social Sciences (SPSS) Inc., Chicago, IL version 11.0.
Results
[Table/Fig-3] shows the distribution of subjects according to age, parity and socioeconomic status. Maximum number of subject were between 31-40 years. The mean age (SD) was 36.30±6.20 years. A 1040 (65%) subjects were multiparous. Total of 66% subject belonged to class III and class IV lower socioeconomic status according to B.G Prasad classification.
Demographic profile of patients.
| Variable | | Percentage (%) |
|---|
| Mean age (36.30±6.20 years) |
| Parity | Primi | 10 |
| Para2 | 25 |
| Multiparous | 65 |
| Socioeconomic status (B.G prasad classification) | I | 8 |
| II | 14 |
| III | 38 |
| IV | 28 |
| V | 12 |
| Total | 100 |
[Table/Fig-4] shows the distribution of subjects according to LBC findings. 23% subjects had normal LBC findings, 17% had inflammatory smear, 24% had Low Grade Squamous Intraepithelial Lesion (LSIL) while 15% had High Grade Squamous Intraepithelial Lesion (HSIL). A 10% had Atypical Squamous cell of Undetermined Significance (ASCUS), 5% had reactive/reparative changes, 4% had koilocytosis, and 2% had smear findings suspension of carcinoma of cervix.
Distribution of subjects according to Liquid Based Cytology (LBC) findings.
| LBC findings | Number of subjects | % |
|---|
| Normal | 368 | 23 |
| Inflammatory | 272 | 17 |
| Reactive/Reparative | 80 | 05 |
| Koilocytosis | 64 | 04 |
| ASCUS | 160 | 10 |
| LSIL | 384 | 24 |
| HSIL | 240 | 15 |
| Suspected carcinoma cervix | 32 | 02 |
| Total | 1600 | 100 |
ASCUS: Atypical squamous cell of undetermined significance; LSIL: Low grade squamous intraepithelial lesion; HSIL: High grade squamous intraepithelial lesion
[Table/Fig-5] shows the distribution of subjects according to visual inspection after acetic acid application. Out of 1600 subjects, 1184 (74%) had Acetowhite area on visual inspection after acetic acid application (positive test) and 416 (26%) had negative VIA test.
Findings of visual inspection after application of acetic acid (VIA).
| Test | VIA | % |
|---|
| Positive | 1184 | 74 |
| Negative | 416 | 26 |
| Total | 1600 | 100 |
[Table/Fig-6] shows the relationship of LBC and biopsy. In present study out of 1600 subjects, 1008 subjects who had colposcopic Reid Index (3-8) were planned for colposcopic guided biopsy. Out of 960 subjects who had abnormal LBC, 688 had biopsy proven preinvasive lesion. So, the Sensitivity and Specificity of LBC was 68.25% and 54.05%, respectively. The PPV of LBC was 71.67 % and the NPV was 50%. The Accuracy of LBC was 63%.
Relation between Liquid Based Cytology (LBC) and biopsy.
| LBC | Biopsy |
|---|
| Done | Not done | Total |
|---|
| Positive | 688 | 272 | 960 |
| Negative | 320 | 320 | 640 |
| Total | 1008 | 592 | 1600 |
[Table/Fig-7] depicts the relationship of VIA and biopsy. In present study, out of 1600 subjects, 1008 subjects who had colposcopic Reid index (3-8) was planned for colposcopic guided biopsy. Out of 1184 subjects who had VIA positive, 928 had biopsy proven preinvasive lesion. So, the Sensitivity and Specificity of VIA was 92.06% and 56.76%, respectively. The PPV was 78.38% and the NPV was 80.77%. The accuracy of VIA 79% is higher than LBC 63%.
Relation of VIA and biopsy results.
| VIA | Biopsy |
|---|
| Done | Not Done | Total |
|---|
| Positive | 928 | 256 | 1184 |
| Negative | 80 | 336 | 416 |
| Total | 1008 | 592 | 1600 |
[Table/Fig-8] shows the comparison between VIA and LBC. The Sensitivity, Specificity, PPV, NPV and accuracy of VIA is more than LBC.
Comparison of both screening modalities.
| Sensitivity | Specificity | PPV | NPV | Accuracy |
|---|
| LBC | 68.25% | 54.05% | 71.67% | 50.0% | 63% |
| VIA | 92.06% | 56.76% | 78.38% | 80.77% | 79% |
PPV: Positive pedictive value; NPV: Negative predictive value; LBC: Liquid based cytology; VIA: Visual inspection after application of acetic acid
Discussion
According to 2012 United States Preventive Services Task Force (USPSTF) guidelines, for average-risk women aged 30-65 years, the USPSTF now recommends high-risk Human Papillomavirus (hrHPV) testing alone every five years as an alternative to screening with cervical cytology alone every three years or screening with a combination of cytology and Human Papillomaviruses Deoxyribonucleic Acid (HPV DNA) testing every five year [8]. In the present study, maximum numbers of cases were in the age group of 31-40 years. The mean age was 36.30±6.20 years. In Hegde D et al., study most of women age group between 20-50 years were included [9]. In study done by Goel A et al., most subjects belonged to age group of 30 to 34 years, whereas Khan M et al., studied age range of 25 to 65 years [10,11]. Kenney W et al., conducted a screening programme in the age group of 35 to 65 years [12]. In Sachan PL et al., study most women were in the age range of 30-50 years [13]. According to Huy NVQ et al., most of patients belonged to age group of 30-39 years [14].
In present study, maximum numbers of subjects were multiparous. Similar study by Kulasingam S et al., showed the mean parity was 4.2 in patients with invasive cancer [15]. Kustagi P and Fernandez P showed the prevalence of Cervical Intraepithelial Neoplasia (CIN) was significant higher in parity of >2 [16]. In study done by Sachan PL et al., most women were multiparous [13]. According to Huy NVQ et al., most of patients were multiparous [14]. Most of the subjects in present study belonged to low socio-economic status (class-III and IV of BG Prasad classification). Two large case control studies held in Spain and Colombia in 2003 have reported a high prevalence of dysplasia among women in low socio-economic status [17,18]. Results of Indian studies is seen in [Table/Fig-9] [18-20]. In present study, 23% subjects had normal pap smear findings. LSIL, HSIL and suspected carcinoma cervix were found in 24%, 15% and 02% subjects, respectively. Denny L et al., reported that the incidence of abnormal pap smear is 8.2% [21]. University of Zimbabwe/Jhpiego cervical cancer project found that 14.6% of women in their study had an abnormal pap smear. Megevand E et al., noted an abnormal pap smear in 13% of their study population [22]. Results of various studies depicted in [Table/Fig-10] [9,13,23-26].
Comparison of present study findings against published literature [18-20].
| Study | Socio-economic status |
|---|
| Bhattacharyya AK et al., [19] | Low |
| Sherwanti RK and Khan T [18] | Low |
| Vaidya A [20] | Low |
| Present Study | Low |
Comparison of Liquid Based Cytology (LBC) finding against published studies [9,13,23-26].
| Study | LBC finding |
|---|
| ASCUS | LSIL | HSIL |
|---|
| Sachan PL et al., [13] | 2.9% | 5.09% | 0.48% |
| Hegde D et al., [9] | - | 6.6% | 2.6% |
| Verma A et al., [24] | 1% | 5.5% | 2.5% |
| Saha D et al., [23] | 5.92% | 1.74% | 0.35% |
| Padmini CP et al., [25] | 8% | 5% | 3% |
| Nayani ZS and Hendre PC [26] | - | 8.6% | 3.8% |
| Present study | 10% | 24% | 15% |
ASCUS: Atypical squamous cell of undetermined significance; LSIL: Low grade squamous Intraepithelial lesion; HSIL: High grade squamous intraepithelial lesion
In present study, acetowhite areas were seen in 74% subjects. According to Goel A et al., study VIA positive rate was 12.5% [10]. Loiudice I et al., reported positive VIA positive in 25.4% in their study [27], whereas Slawson et al., and Megevand E et al., reported an incidence of abnormal VIA of 4.2 and 3.13%, respectively in their study [22]. In present study, Sensitivity of VIA was 92.06% and specificity was 56.76%. In a study done by Sankaranarayanan R et al., Sensitivity of VIA to detect CIN was 88.6% and Specificity was 86.5% [28]. Diagnostic value of VIA were tabulated in [Table/Fig-11] [2,14,19,29]. In present study, Sensitivity, Specificity, PPV and NPV of LBC was 68.25%, 54.05%, 71.67 % and 50%, respectively. In study by Hegde D et al., Sensitivity, Specificity, PPV and NPV of LBC was 50%, 97%, 97.5% and 96.09% respectively [9]. Dignostic value of LBC were tabulated in [Table/Fig-12] [2,9,10,14,30].
Comparison of Diagnostic accuracy of VIA against published studies [2,14,19,29].
| Study | Sensitivity | Specificity | PPV | NPV | Accuracy |
|---|
| Vahedpoor Z et al., [29] | 94.6% | 81.6% | 78.8% | 95.4% | - |
| Sinha P et al., [2] | 93.3% | 60% | 36.8% | 97.3% | 66.7% |
| Huy NVQ et al., [14] | 88.8% | 43.8% | 51.2% | 83.3% | 63.4% |
| Bhattacharyya AK et al., [19] | 89% | 87% | 32% | 99% | 87% |
| Present study | 92.06% | 56.76% | 78.38% | 80.77% | 79% |
PPV: Positive pedictive value; NPV: Negative predictive value
Comparison of Diagnostic accuracy of LBC against published studies [2,9,10,14,29,30].
| Study | Sensitivity | Specificity | PPV | NPV | Accuracy |
|---|
| Sinha P et al., [2] | 93.8% | 72.9% | 48.4% | 97.7% | 77.3% |
| Hedge D et al., [9] | 83% | 98% | 97.9% | 80.80% | - |
| Goel A et al., [10] | 50% | 97% | - | - | - |
| Huy NVQ et al., [14] | 58% | 85.2% | 83.3% | 61.3% | 69.9% |
| Vahedpoor Z et al., [29] | 29.7% | 85.5% | 59.8% | 62.6% | |
| Singh KN and More S [30] | 70.02% | 97.2% | 51.2% | 97.1% | |
| Present study | 68.25% | 54.05% | 71.67% | 50% | 63% |
PPV: Positive pedictive value; NPV: Negative predictive value
In present study, the Sensitivity, Specificity, PPV, NPV and accuracy of VIA is more than LBC. The reason for these variations in the diagnostic value of LBC and VIA in different studies may be due to considering different diagnostic criteria, difference in considering the positive tests results and differences in the studied population. VIA is a low cost, simpler, single visit approach and easier method than LBC and does not require laboratory facilities. Therefore, it can be recommended for primary screening program in low resource settings.
Limitation(s)
In present study, most of the patient from rural area which may be act as a confounding factor. Secondary triage procedures like human paplilloma virus testing and colposcopy should also be performed which was not done.
Conclusion(s)
VIA is a more sensitive then pap smear screening modality, so it should be used in routine as screening modality for cervical cancer, High incidence of cervical cancer may be attributed to the lack of awareness among the people and the lack of effective screening program. This leads to reporting of very advanced cases of cervical cancer cervix where mortality and morbidity is very high.
ASCUS: Atypical squamous cell of undetermined significance; LSIL: Low grade squamous intraepithelial lesion; HSIL: High grade squamous intraepithelial lesion
PPV: Positive pedictive value; NPV: Negative predictive value; LBC: Liquid based cytology; VIA: Visual inspection after application of acetic acid
ASCUS: Atypical squamous cell of undetermined significance; LSIL: Low grade squamous Intraepithelial lesion; HSIL: High grade squamous intraepithelial lesion
PPV: Positive pedictive value; NPV: Negative predictive value
PPV: Positive pedictive value; NPV: Negative predictive value