One of the greatest assets for the geriatric edentulous population is to have a beautiful smile, and the ability to chew well with a complete denture prosthesis that is adequately retentive. Lack of retention with maxillary denture can affect not only the personality but also the behavior of the individual [1-3]. A well-constructed, accurately fitting denture aids significantly to meet the mind of the patient by comforting them, while lack of retention can lead to rejection towards the rehabilitation [3]. One of the factors affecting complete denture success is the relationship between the dentures and its supporting and limiting structures [4]. The distal limit and border seal of maxillary denture is established by successfully incorporating posterior palatal area in the impression [5].
According to Glossary of Prosthodontic terms 9, PPS is defined as “that portion of the intaglio surface of a maxillary removable complete denture, located at its posterior border, which places pressure, within physiologic limits, on the PPS area of the soft palate; this seal ensures intimate contact of the denture base to the soft palate and improves retention of the denture” [6,7]. A correctly incorporated PPS helps in providing retention, prevents food accumulation beneath the denture base, reduces gag reflex, makes the distal border less conspicuous to tongue and provides a mechanism to compensate for denture warpage during processing [5,8,9].
Previous studies have reported the following as the most common methods to establish PPS: 1) Arbitrary technique (cast scraping method); 2) Winkler’s conventional technique (using temporary record base to transfer the vibrating lines along with scoring of the master cast); 3) Boucher’s conventional technique (by transferring the vibrating lines onto the custom tray and recording the seal during border molding under pressure along with master cast scoring); 4) Boucher’s conventional technique without master cast scoring; 5) Fluid wax technique (made during final impression using mouth temperature wax) [10,11].
The PPS is recorded by locating the anterior and posterior vibrating lines in the patient’s mouth followed by transferring it on to the master cast [12,13]. The well documented technique for locating vibrating line includes pronunciation of “ah” sound, Valsalva maneuver (nose blowing) and palpation method [14-16].
Literary works reported variation in concepts for determining PPS among US predoctoral dental curriculum, but some concepts were dominant with respect to scoring of the cast (95%), butterfly pattern of PPS carving (75%) and one-line vibrating concept of recording PPS area (80%) [17]. An educational survey conducted in Pakistan (2010) on the same, revealed no conceptual difference in training methods of PPS among different government and private dental colleges [18]. Another study conducted in Chennai showed arbitrary scraping of posterior palatal area as the most commonly followed method. The study also highlighted the variation in recording techniques of PPS among dental practitioners and dental students [19].
However, surveys relating the influence of faculty experience on evolving concepts of PPS among dental colleges have not been documented in Indian literature. Therefore, this study aimed to determine the commonly used methods in teaching PPS philosophy across various government and private dental colleges of Karnataka and also, if the teaching methods were standardised among various cadres of the faculty.
Materials and Methods
A descriptive, cross-sectional survey was conducted for a period of 75 days between August 2019 to November 2019 using a prevalidated close ended English language questionnaire [17]. Ethical approval for the present study was obtained from University Ethics Committee for Human Trial, MSRUAS at MS Ramaiah University of Applied Sciences, Bengaluru (UECHT/2016-2018/PG). The questionnaire was created online (www.docs.google.com) and sent by e-mail to the faculty members of the Department of Prosthodontics across 44 dental colleges of Karnataka state. These faculty members were categorised as: Group 1 with teaching experience ranging from 2-7 years, Group 2 had 7-12 years of experience and Group 3 were into teaching for more than 12 years [Table/Fig-1].
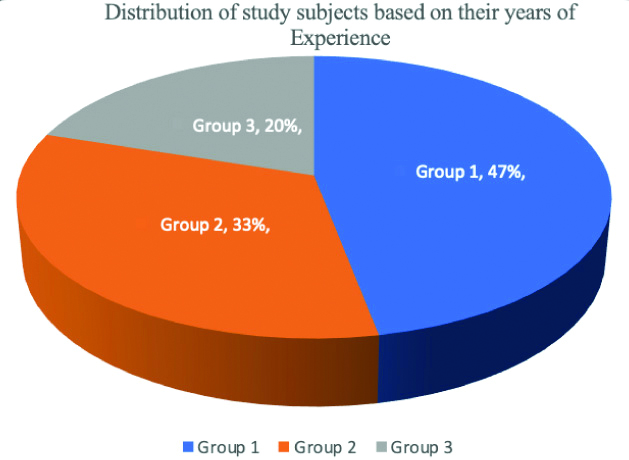
Distribution of study participants based on their years of experience.
Group 1: 2-7 years 47% (94/200); Group 2: 7-12 years 33% (66/200); Group 3: >12 years-26 years 20% (40/200)
Inclusion Criteria
Faculty with MDS degree in Prosthodontics and a minimum teaching experience of 2 years.
Faculty only from dental colleges of Karnataka was included in the study.
Exclusion Criteria
Private practitioners were not included in the study.
Faculty members who were eligible but did not give consent were excluded from the study.
The sample size was calculated to be 195.92 which was rounded off to 200 based on 95% confidence level and 5% margin of error to provide a power of at least 80. Anticipating a non-response rate of approximately 15% in online surveys, the sample size was inflated to 230. The prevalidated questionnaire had seven close-ended questions [17]. Three questions were added (Questions 5, 6 and 10) to the existing questionnaire resulting in a total of ten close ended questions. A pilot test was carried out to internally validate the modified questionnaire using Lawshe’s method in the following way. The questionnaire was distributed among 15 prosthodontic staff members (experts). Every question was to be ranked by the staff as essential, essential but not so important or not essential on a 3-part spectrum. Responses which indicated “essential’ for all items were determined and Content Validity Ratio (CVR) was calculated. Questions with a score of 0.7 and above were included in the study whereas question having score less than 0.7 were excluded. Consistency of the questionnaire was evaluated using Cronbach’s alpha value with a mean score of 0.82.
In the survey, the first four questions (Questions 1, 2, 3 and 4) were related to knowledge of the posterior palatal vibrating lines and the relation of the maxillary denture to those lines. The next two questions (Questions 5 and 6) were associated with currently used methods and materials in recording the PPS. The subsequent three questions (Questions 7,8 and 9) were linked to practice and design of carving the seal area on the maxillary master cast. The final question (Question 10) was associated with the need for clear-cut standardised methods in teaching and learning PPS. The respondents had to answer all the questions by choosing only one response for each device. All responses remained anonymous throughout the survey and prior informed consent was obtained from the participants. The responses were directed to the site (google drive) for evaluation and data was recorded using Microsoft excel 2013.
Statistical Analysis
The analysis of data was done using Statistical Package for Social Sciences (SPSS) for Windows Version 22.0 Released 2013. Armonk, NY: IBM Corp., Descriptive analysis of all the explanatory and outcome parameters was done using mean and standard deviation for quantitative variables, frequency and percentages for categorical variables. The inferential data analysis tests employed were:
a) Chi-Square Goodness of Fit test to compare the overall differences in the responses by the study participants; and
b) Independent Chi-Square test to compare the differences in the responses based on teaching experience of the study participants.
The level of significance (p-value) was set at p<0.05.
Results
A total of 200 prosthodontic faculty members responded, out of which 47% (94/200) respondents had a teaching experience of 2 to 7 years and were categorised as Group 1, whereas 33% (66/200) with a teaching experience of 7 to 12 years were assigned to Group 2. Finally, 20% (40/200) of faculty with teaching experience of greater than 12 years were allotted to Group 3 [Table/Fig-2].
Comparison of overall differences in distribution of responses among the participants.
| Comparison of the overall differences in distribution of responses among the participants using Chi-square goodness of fit test |
|---|
| Sl. | Questions | Responses | n | % | χ2 value | p-value |
|---|
| Q1 | Which method is currently taught for locating the vibrating line? | Phonation | 23 | 11.5% | 103.720 | <0.001** |
| Phonation and nose blowing | 77 | 38.5% |
| Phonation and fovea palatini | 8 | 4.0% |
| Phonation, nose blowing and fovea palatini | 92 | 46.0% |
| Others | 0 | 0.0% |
| Q2 | What concept is currently being taught for number of vibrating lines? | One line | 46 | 23.0% | 58.320 | <0.001** |
| Two lines | 154 | 77.0% |
| Q3 | If you teach one vibrating line concept, where do you place the termination of maxillary denture in relation to vibrating line? | On vibrating line | 146 | 73.0% | 254.200 | <0.001** |
| Anterior to vibrating line | 17 | 8.5% |
| Posterior to vibrating line | 33 | 16.5% |
| Others | 4 | 2.0% |
| Q4 | If you teach two vibrating line concept, where do you place the termination of maxillary denture in relation to vibrating line? | On posterior vibrating line | 116 | 58% | 179.080 | <0.001** |
| Anterior to vibrating line | 15 | 7.5% |
| Posterior to vibrating line | 68 | 34% |
| Half way between anterior and posterior lines | 1 | 0.5% |
| Q5 | Which method is currently taught for incorporating the posterior palatal seal? | Arbitrary technique (Cast scraping method) | 10 | 5.0% | 262.250 | <0.001** |
| Winkler’s conventional technique | 8 | 4.0% |
| Boucher’s conventional technique (with master cast scoring) | 49 | 24.5% |
| Boucher’s conventional technique (without master cast scoring) | 126 | 63.0% |
| Fluid wax technique | 7 | 3.5% |
| Others | 0 | 0.0% |
| Q6 | What is your material of choice if you are using fluid wax technique? | IOWA wax | 2 | 1% | 1.571 | 0.67 |
| Korrecta wax | 3 | 1.5% |
| Adaptol | 1 | 0.5% |
| H-L physiologic past | 1 | 0.5% |
| Others | 0 | 0.0% |
| Q7 | Are you currently teaching your students to carve postpalatal seal on maxillary cast? | Yes | 67 | 33.5% | 21.780 | <0.001** |
| No | 133 | 66.5% |
| Q8 | What pattern or shape of postpalatal seal are you currently teaching? | Butterfly | 135 | 67.5% | 239.080 | <0.001** |
| Single bead | 2 | 1.0% |
| Double bead | 2 | 1.0% |
| According to palpation | 61 | 30.5% |
| Others | 0 | 0.0% |
| Q9 | What is the depth of postpalatal seal carved in maxillary master cast? | 0.5-1 mm (Considering compressible tissue) | 89 | 44.5% | 249.050 | <0.001** |
| 1-1.5 mm (Considering compressible tissue) | 100 | 50.0% |
| 1-1.5 mm (Do not consider compressible tissue) | 4 | 2.0% |
| Entire depth of compressible tissue | 3 | 1.5% |
| Half the depth of compressible tissue | 4 | 2.0% |
| Q10 | Do you feel the need to standardise and simplify the existing method of recording PPS? | Yes | 120 | 60.0% | 8.000 | 0.005* |
| No | 80 | 40.0% |
p<0.05* statistically significant; p<0.001** statistically highly significant
The overall differences in distribution of responses is presented in [Table/Fig-2] and comparison of responses related to years of experience in [Table/Fig-3].
Comparison of responses based on years of experience of study participants.
| Comparison of differences in the responses based on the years of experience of study participants using Independent Chi-Square Test |
|---|
| Sl. | Questions | Responses | Group 1 | Group 2 | Group 3 | χ2 value | p-value |
|---|
| n | % | n | % | n | % |
|---|
| Q1 | Which method is currently taught for locating the vibrating line? | Phonation | 9 | 9.6% | 13 | 19.7% | 1 | 2.5% | 10.482 | 0.11 |
| Phonation and nose blowing | 40 | 42.6% | 22 | 33.3% | 15 | 37.5% |
| Phonation and fovea palatini | 3 | 3.2% | 4 | 6.1% | 1 | 2.5% |
| Phonation, nose blowing and fovea palatini | 42 | 44.7% | 27 | 40.9% | 23 | 57.5% |
| Others | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% |
| Q2 | What concept is currently being taught for number of vibrating lines? | One line | 19 | 20.2% | 21 | 31.8% | 6 | 15.0% | 4.756 | 0.09 |
| Two lines | 75 | 79.8% | 45 | 68.2% | 34 | 85.0% |
| Q3 | If you teach one vibrating line concept, where do you place the termination of maxillary denture in relation to vibrating line? | On vibrating line | 71 | 75.5% | 46 | 69.7% | 29 | 72.5% | 1.921 | 0.93 |
| Anterior to vibrating line | 6 | 6.4% | 8 | 12.1% | 3 | 7.5% |
| Posterior to vibrating line | 15 | 16.0% | 11 | 16.7% | 7 | 17.5% |
| Others | 2 | 2.1% | 1 | 1.5% | 1 | 2.5% |
| Q4 | If you teach two vibrating line concept, where do you place the termination of maxillary denture in relation to vibrating line? | On posterior vibrating line | 48 | 51.1% | 34 | 51.5% | 34 | 85.0% | 17.371 | 0.008* |
| Anterior to vibrating line | 6 | 6.4% | 7 | 10.6% | 2 | 5.0% |
| Posterior to vibrating line | 39 | 41.5% | 25 | 37.9% | 4 | 10.0% |
| Half way between anterior and posterior lines | 1 | 1.1% | 0 | 0.0% | 0 | 0.0% |
| Q5 | Which method is currently taught for incorporating the posterior palatal seal? | Arbitrary technique (Cast scraping method) | 6 | 6.4% | 3 | 4.5% | 1 | 2.5% | 85.642 | <0.001** |
| Winkler’s conventional technique | 6 | 6.4% | 1 | 1.5% | 1 | 2.5% |
| Boucher’s conventional technique (with master cast scoring) | 5 | 5.3% | 16 | 24.2% | 28 | 70.0% |
| Boucher’s conventional technique (without master cast scoring) | 77 | 81.9% | 44 | 66.7% | 5 | 12.5% |
| Fluid wax technique | 0 | 0.0% | 2 | 3.0% | 5 | 12.5% |
| Others | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% |
| Q6 | What is your material of choice if you are using fluid wax technique? | IOWA wax | 0 | 0.0% | 1 | 0.5% | 1 | 0.5% | 4.200 | 0.65 |
| Korrecta wax | 1 | 0.5% | 0 | 0.0% | 2 | 1.0% |
| Adaptol | 0 | 0.0% | 0 | 0.0% | 1 | 0.5% |
| H-L physiologic past | 0 | 0.0% | 0 | 0.0% | 1 | 05% |
| Others | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% |
| Q7 | Are you currently teaching your students to carve postpalatal seal on maxillary cast? | Yes | 17 | 18.1% | 20 | 30.3% | 30 | 75.0% | 41.253 | <0.001** |
| No | 77 | 81.9% | 46 | 69.7% | 10 | 25.0% |
| Q8 | What pattern or shape of postpalatal seal are you currently teaching? | Butterfly | 71 | 75.5% | 41 | 62.1% | 23 | 57.5% | 7.513 | 0.28 |
| Single bead | 0 | 0.0% | 1 | 1.5% | 1 | 2.5% |
| Double bead | 1 | 1.1% | 1 | 1.5% | 0 | 0.0% |
| According to palpation | 22 | 23.4% | 23 | 34.8% | 16 | 40.0% |
| Others | 0 | 0.0% | 0 | 0.0% | 0 | 0.0% |
| Q9 | What is the depth of postpalatal seal carved in maxillary master cast? | 0.5-1mm (Considering compressible tissue) | 55 | 58.5% | 26 | 39.4% | 8 | 20.0% | 22.364 | 0.004* |
| 1-1.5mm [Considering compressible tissue] | 36 | 38.3% | 35 | 53.0% | 29 | 72.5% |
| 1-1.5mm (Do not consider compressible tissue) | 1 | 1.1% | 2 | 3.0% | 1 | 2.5% |
| Entire depth of compressible tissue | 2 | 2.1% | 1 | 1.5% | 0 | 0.0% |
| Half the depth of compressible tissue | 0 | 0.0% | 2 | 3.0% | 2 | 5.0% |
| Q10 | Do you feel the need to standardise and simplify the existing method of recording PPS? | Yes | 58 | 61.7% | 51 | 77.3% | 11 | 27.5% | 25.922 | <0.001** |
| No | 36 | 38.3% | 15 | 22.7% | 29 | 72.5% |
p<0.05* statistically significant; p<0.001** statistically highly significant
In relation to question 1, results showed that the most common method taught for locating vibrating line is phonation-nose blowing-fovea palatine (46.0%), followed by phonation-nose blowing (38.5%). The difference between the responses was statistically highly significant (p<0.001) [Table/Fig-2]. However, there was no statistical significance (p=0.11) when the responses were compared according to years of experience [Table/Fig-3].
With respect to question 2, the survey revealed that, 77% of faculty taught two-line concept for marking the vibrating line and only 23% preferred one-line concept. The difference was statistically highly significant (p<0.001) for the concept of vibrating lines [Table/Fig-2]. When the responses were compared with teaching experience the trend was similar in that, majority of the faculty taught two lines concept in all three groups, the difference being statistically non significant (p=0.09) [Table/Fig-3].
With respect to question 3, which emphasises on one-line concept of vibrating line, most of the faculty preferred to terminate the maxillary denture on the vibrating line (73%) which was statistically highly significant (p<0.001) when compared to terminating the border posterior to vibrating line (16.5%) or anterior to vibrating line (8.5%) [Table/Fig-2]. Comparison of responses from the three groups based on teaching experience revealed no statistical difference (p=0.93) for termination of maxillary denture in relation to vibrating line [Table/Fig-3].
Question 4 emphasises on two-line concept of vibrating line. In this, most of the faculty preferred to terminate the maxillary denture on the posterior vibrating line (58%) which was statistically highly significant (p<0.001) when compared to others borders [Table/Fig-2]. Comparison of faculty responses revealed 85% of Group 3 preferred terminating maxillary denture on posterior vibrating line as compared to Group 2 (51.5%) and Group 1 (51.1%). This difference was statistically significant (p=0.008) [Table/Fig-3].
Question 5 of the survey, revealed that most of the faculty preferred to teach Boucher’s conventional method without master cast scoring (63%) followed by Boucher’s conventional technique with master cast scoring (24.5%). The least preferred methods were arbitrary scrapping of master cast (5%), followed by Winkler’s conventional technique (4%), and fluid wax technique (3.5%). The difference was statistically highly significant with p-value at 0.001 [Table/Fig-2]. Comparison of faculty responses revealed that Group 1 and Group 2 preferred Boucher’s conventional technique without master cast scoring (81.9% and 66.7%, respectively) while Group 3 faculty preferred Boucher’s conventional technique with master cast scoring (70%). This difference was statistically highly significant (p<0.001) [Table/Fig-3].
In sixth question, 1.5% faculty members preferred Korrecta wax over the other waxes to record PPS area followed by IOWA wax (1%), Adaptol and H-L physiologic past (0.5%), where the value was p=0.65 and not statistically significant [Table/Fig-2]. Faculty members across all groups unequivocally advocated use of Korrecta wax (p=0.65) [Table/Fig-3].
With respect to the seventh question, majority of the faculty (66.5%) do not advocate carving PPS on maxillary cast, which was found to be statistically highly significant (p<0.001) in comparison to those who advocated carving (33.5%) [Table/Fig-2]. Comparison of faculty showed that 81.9% of faculty in Group 1, followed by 69.7% in Group 2, do not support carving PPS; whereas 75% of Group 3 favoured carving PPS area on the cast. This difference was statistically highly significant at p<0.001 [Table/Fig-3].
With regard to question 8, overall 67.5% of the faculty preferred butterfly shaped PPS, followed by 30.5% who preferred to palpate the PPS to determine its shape. This difference was statistical highly significant (p<0.001) [Table/Fig-2]. Based on faculty experience, no statistical difference (p=0.28) was found within the groups [Table/Fig-3].
In response to question 9, 50% of total faculty members carved PPS up to a depth of 1-1.5 mm considering the compressibility of the tissues, followed by 44.5% who preferred 0.5-1 mm carving considering compressible tissue whereas only 1.5% preferred carving PPS to the entire depth of compressible tissue. This difference was statistically highly significant at p<0.001 [Table/Fig-2]. When the responses were compared with teaching experience, majority of Group 3 faculty (72.5%) favoured scoring of master cast up to 1-1.5 mm considering the compressibility of the tissues with a statistical difference of 0.004 as compared to other groups [Table/Fig-3].
In question 10, 60.0% of the overall faculty members felt the need to simplify and standardise the existing methods. The Chi-Square Goodness of Fit test showed a statistically significant difference in opinions (p=0.005) [Table/Fig-2]. Also, a difference in opinion was noted related to years of experience. Mainly faculty from Group 2 (77.3%) and Group 1 (61.7%) felt the need to simplify the existing methods as against very few in Group 3 (27.5%). This difference was again found to be statistically highly significant at p<0.001 [Table/Fig-3].
Discussion
The technique preferred by a practitioner generally depends upon individual preference and experience [19]. Thappa D et al., in 2016 said, locating and recording PPS, is a highly controversial topic, as the literature provides various methods to record the same [20]. Therefore, this survey was conducted with the aim to identify the most common concept and methods of teaching PPS among Prosthodontic faculty belonging to dental colleges of Karnataka. In the present study, the participants had a teaching experience ranging from a minimum of two years to a maximum of 26 years. The common method taught for locating the vibrating line by most of the faculty was a combination of phonation-nose blow-fovea palatine (46.0%). Based on the educational survey carried by Rashedi B and Petropoulos VC, 80% predoctoral dental schools in US taught a combination of phonation with other methods for determining the location of vibrating line [17]. Previous survey by Chen MS et al., also showed similar results, where, 51.8% of dental schools taught phonation and other techniques as the method of choice for locating vibrating line [21].
This survey revealed that two-line concept of vibrating line is the most commonly taught among dental colleges of Karnataka. Accordingly, 77% of the faculty members follow two-line concept of identifying vibrating line and also terminate their maxillary denture on posterior vibrating line. A survey carried out by Rashedi B and Petropoulos VC, revealed that, 80% of the dental schools in US taught one-line concept for identifying the vibrating line [17]. However, the present survey disclosed that, two-line concept of vibrating line was most commonly followed by all three groups of faculties. This may be attributed to improvement in understanding and replication of the boundaries of PPS anatomy which contributes immensely to the retention of complete dentures [22-24]. Limbu IK and Basnet BB acknowledged that two vibrating line concept is prevalent in India and Nepal [20,25].
In one-line concept of identifying the vibrating line, 73% of participants believe in termination of maxillary denture on vibrating line. This is in accordance with surveys conducted by Rashedi B and Petropoulos VC, and Chen MS et al., where, 77% and 64.3% of the schools, respectively, terminate the distal end of maxillary denture on vibrating line [17,21]. In two-line concept of identifying the vibrating line, this survey found 58% of faculty members terminate the maxillary denture on posterior vibrating line. Similar studies by Rashedi B and Petropoulos VC, and Chen MS et al., observed 50% and 46.2% of colleges respectively, terminated the distal end of the maxillary denture on the posterior flexion line [17,21]. In the current survey faculty across all three groups, indisputably advocated termination of distal end of the denture base on vibrating line while following one-line concept and on posterior vibrating line when advocating two-line concept.
Literature shows variation in the method of recording PPS across the globe. Studies conducted across different countries suggest arbitrary technique (cast scraping method) to be the most common method taught for establishing PPS [17,19,21]. Alaa’a MS investigated the effectiveness of arbitrary scraping method used for establishing PPS and concluded that scraping method offers effective retention in the PPS area and can be considered as a safe procedure [26]. On the contrary, recent evidence from literature suggests that scraping technique is considered as one of the least accurate method [19,23]. As the depth and width of cast scoring can be subjective, the possibility of over-compression or under-compression of posterior palatal tissues has reduced the popularity of scraping method among current teaching protocols [23,27]. Khafoor MQ stated recording PPS is the clinician’s responsibility rather than the technicians [28].
The present survey revealed that Boucher’s conventional technique without scoring of master cast was most commonly taught to record PPS (63%). While, 81.9% of Group 1 and of Group 2 (66.7%) were against master cast scoring, 70% of faculty from Group 3 preferred master cast scoring. This difference in teaching protocol within the groups was statistically highly significant (<0.001). The difference among faculty may be attributed to changing concepts as revealed by recent comparative studies which discard scoring of master cast [28,29]. Khafoor MQ stated physiological methods offered better retention and minimised chances of over compression of tissues [28]. These variations in teaching may create ambiguity among students regarding the appropriate method to be employed while recording PPS.
Majority of the faculty considered Korrecta wax (1.5%) as the material of choice while advocating fluid wax technique. According to Binti NS et al., 44% participants preferred Korrecta wax over other mouth temperature waxes [19]. Butterfly shape of PPS was most commonly advocated among the faculty which is in accordance to a survey where, 75% of dental schools taught butterfly shape of PPS [17]. Faculty members across all groups unequivocally advocate use of Korrecta wax and carving of PPS in butterfly shape.
Overall, the concept of carving PPS on the master cast was not predominant across dental colleges in Karnataka, which is contradictory to findings of other studies done in US, Canada and Chennai [17,19,21]. Although there is a difference in findings between earlier studies and the present survey, the influence of teaching experience had not been taken into consideration in previous studies. Interestingly, faculty belonging to Group 3 (with higher teaching experience) seemed to prefer carving of master cast whereas faculty belonging to Group 1 and 2 avoided carving of master cast. Recent scientific evidence also suggests that carving of master cast tends to over compress the palatal tissue [23,27,28]. The younger generation of faculty seems to have progressed by accepting a more physiological method to record PPS when compared with their experienced counterparts.
A common consent of carving PPS up to a depth of 1-1.5 mm based on tissue compressibility was noticed among majority of teaching faculty which is in accordance with previous studies [17,18]. Rashedi B and Petropoulos VC, Hussain SZ et al., and Chen MS et al., showed that 91%, 83.33% and 93.9% of study population respectively, carved PPS up to a depth of 1-1.5 mm considering tissue compressibility [17,18,21]. When faculty experience was taken into account, variations were noted in the depth of postpalatal seal carved in maxillary mastercast. This is in accordance with the study done by Krysinski ZJ and Prylinski M which concluded that the individual’s clinical experience influence the depth of carving PPS [30]. The Group 1 (58.5%) and Group 2 (39.4%) faculty preferred carving master cast to a depth of 0.5-1mm based on the compressibility of the tissue as compared to very few in Group 3 (20%). This evolving school of thought depicts a shift towards being conservative when carving PPS area.
More than half of the participants (60.0%) agreed to the need of uncomplicated and a standardised method to record PPS, which was found to be statistically significant (p=0.005). Analysis of responses based on teaching experience revealed that majority of faculty members belonging to Group 2 and Group 1 favoured the need to standardise the teaching methods. Though Boucher’s conventional technique without scoring of master cast is the dominant method according to our survey, it does not find a place in the present curriculum [7,9,13]. It is considered a physiologic technique and is very commonly followed in our country whereas other techniques are not preferred because of their built-in differences and disadvantages [23,27-29]. Comparative studies done with respect to measurement of retention offered by various methods concluded that fluid wax and functional method using low fusing compound offers highest retention [28,29]. The existing dilemma can be solved by conducting comparative clinical studies that evaluate retention offered by Boucher’s conventional method without cast scoring as against other methods. It may also be suggested to include in the teaching curriculum, newer methods that are physiologic, simple and easy to standardise. Eliminating cast scoring methods may help in further simplification. This in turn can promote better teaching and improved learning outcomes.
Limitation(s)
The present study was conducted among various Prosthodontic faculty members belonging to dental colleges of Karnataka. As teaching methods can be subjective, an Indian survey with a similar focus and a larger sample size will help in generalising the results.
Conclusion(s)
The teaching concepts of PPS vary with experience among Prosthodontic faculty of Karnataka. It is clear that the younger faculty have progressed and adjusted to concepts that are physiologic when compared to their counterparts. Though a sizeable majority followed Boucher’s method without scoring of master cast to achieve PPS, senior faculty with greater than 12 years of experience advocated master cast scoring unlike their junior colleagues who were against scoring. Ambiguity was also evident regarding the depth of scoring the master cast, termination of maxillary denture with respect to vibrating lines and the necessity to standardise the existing concepts of PPS. It is evident that there is no consensus in the teaching concepts and methods within different cadres of faculty. Hence, it may be suggested to include PPS recording methods that are standardised and unambiguous in the teaching curriculum.
p<0.05* statistically significant; p<0.001** statistically highly significant
p<0.05* statistically significant; p<0.001** statistically highly significant