Complete edentulous patients with mandibular bone resorption often show dissatisfaction with their conventional complete dentures. Bone resorption after the loss of dental elements reduces the basal area for support of conventional complete dentures resulting in poor retention, compromising prosthetic stability and patient comfort. In addition, in cases of severe bone resorption, the use of conventional complete dentures can also cause discomfort, given the “migration” of the mental foramen of the buccal bone plate to the crest of the ridge [1].
Implant supported prosthetic rehabilitation could reestablish the comfort and bring a confident smile to patients, allowing them to eat properly and to lead a social life free of traumas and complexes. The treatment options with implants for completely edentulous patients are overdentures and fixed complete dentures, also known as protocol [2]. Choosing between an overdenture and a fixed denture (protocol) depends on the placement of implants at appropriate sites and in sufficient number, taking into account the local anatomy (bone) and the patient’s socioeconomic background [3,4]. For example, an overdenture could be a cost-benefit treatment for elderly patients with compromised health, when extensive surgical procedures are not recommended. Moreover, this type of rehabilitation would be an alternative for edentulous patients with poor retention of complete lower dentures and low bone quality and quantity for placement of four or more implants [5,6].
Besides anatomical and financial aspects, patientś perception about their oral health has been considered by prosthodontists to be a relevant factor for choosing the rehabilitation treatment plan. Therefore, by means of Visual Analog Scales (VAS) and questionnaires, such as the OHIP-EDENT, studies have assessed patients self-perception about their oral rehabilitation with implants [7,8]. A patient perception of his or her own oral health is very important. Oral health is related to quality of life. The oral health related to the quality of life and featuring individual perception can be used as an indicator of strategies for prosthetic rehabilitation (OHIP-Edent) [9]. Furthermore, financial factors and the ability to adapt prostheses can alter the final results of the proposed treatment [10].
By comparing the level of satisfaction of patients treated with complete lower denture with the ones treated with lower overdenture, better results have been obtained for implant-supported rehabilitations [11]. Studies have also determined the level of satisfaction of patients treated only with implants, comparing the types of prostheses (overdenture or fixed denture) or analysing them separately [12-14]. However, there is no consensus yet, in literature, about which of these implant-supported treatments would provide a higher level of patient satisfaction and quality of life improvement [9,10].
Thus, considering the large demand for implant-supported rehabilitations and the possibility of several treatment options, questions have been raised regarding which treatment would provide comfortable oral health conditions and high-level satisfaction for the patient. Choosing between an overdenture and a fixed denture depends on the placement of implants at appropriate sites and in sufficient number, taking into account the local anatomy (bone) and the patient’s socioeconomic background. Hence, the objective of the present study was to verify which implant-supported rehabilitation-overdenture or fixed denture (protocol) most effectively restores comfort to patients with complete edentulous lower arch, using data obtained from satisfaction questionnaires and clinical evaluation.
Materials and Methods
A cross-sectional clinical study was carried out in patients with complete edentulous lower arches who were treated with either overdenture or fixed denture (Bränemark protocol), obtained from a random sampling in Southern Brazil. The study was conducted between March 2017-April 2019 at Clinic Dentistry-Faculty of Dentistry/UPF-RS/Brazil. The Research Ethics Committee of the University, resolution CNS 196/96 CAAE 0192.0.398.000-11, approved the study.
Sample selection: The sample consisted of 37 patients treated at the clinics of graduate programs in Implantology and Implant-Supported Prostheses in the University. The samples were the patients who participated in the Implantology Clinic in the March 2017-April-2019 and had lower overdenture or lower fixed dentures. Only patients who agreed and signed the informed consent form participated in the research.
A total of 18 patients treated with lower overdenture and 19 treated with lower implant fixed denture participated as volunteers, according to the Declaration WMA of Helsinki, 2001 respecting the risks, burdens and ethical benefits for medical research involving humans [15].
Inclusion criteria: The following were the inclusion criteria: patients treated with implant-supported prostheses for at least one year; prostheses supported on at least two implants for lower overdenture cases (because it’s the sufficient number of implants to support a overdenture), using O-ring retainers on implants (Neodent, Curitiba, PR, Brazil) and polymer gasket internally attached to the prostheses, the patients had completely removable upper dentures, removable partial upper prostheses or teeth on antagonist arch; prostheses supported on at least four and at most six implants for lower fixed dentures; implants with external hex connections (Neodent®Curitiba/Paraná- Brazil) in the interforaminal region; and age over 40 years and under 85 years.
Exclusion criteria: The following were the exclusion criteria: Poor general health status, e.g., decompensated diabetes, severe anaemia, long-term use of corticosteroid or anticoagulant therapy; submission to radiation therapy less than one year ago; chronic alcohol and drug users; and smokers.
Questionnaires
Three questionnaires were used to assess patients masticatory ability, satisfaction and quality of life. The first questionnaire contained five yes-or-no questions: 1) Can you eat well with your prosthesis? 2) Can you chew everything that you enjoy eating? 3) Have you changed your eating habits because of the prosthesis? 4) Can you eat raw carrots, peanuts or meat? 5) Do you eat only soft foods? When the patients gave three or more favourable answers to masticatory ability questions, this ability was classified as satisfactory (S); and as dissatisfactory (D) when two or fewer answers were favourable [16]. The questionnaire was free to use.
The second questionnaire assessed patient’s self-perception about masticatory ability using the VAS, where 0 indicated “totally dissatisfied” and 10 stood for “totally satisfied”. Those patients, who scored higher than 7 on the VAS, were considered satisfied [17].
The third questionnaire, the OHIP-EDENT, specific for edentulous patients, detected changes in oral health-related quality of life. The questionnaire consisted of 19 questions, with the following possible answers: 0=never, 1=sometimes, and 2=almost always, split into seven categories. The smaller the sum of the answers the higher the level of patient satisfaction [7].
Clinical Examination
After the application of the questionnaires, a specialist in Implantology and Implant-Supported Prostheses performed the clinical examination. The same researcher performed all clinical examinations and applied the questionnaires to patients. The intra-examiner reliability score was 0.86. Data were collected at the clinic of Implantology and implant-supported prostheses in patients who had the following clinical situations: lower overdenture and fixed prosthesis on lower implants as opposed to removable partial denture, upper denture and teeth. An average time of 20 minutes was stipulated for the volunteers to answer all the questionnaires. The questionnaires were applied only by a calibrated examiner who interviewed the volunteers.
Bleeding on probing index was assessed by the clinical reading of bleeding spots at the time of examination of the gingival crevice up to 20 seconds after measurement. This was recorded on the periodontal chart for the four implants sites (mesial, distal, buccal, and lingual) using a dichotomous index [18].
The bleeding index was calculated by the sum of the bleeding sites in each implant and its division by the total number of sites evaluated. The plaque indexes were evaluated at the cervical regions of the prostheses and at the four implants sites [19]. To obtain the index for each tooth, the scores of each face were added and divided by 4. The mean value of bleeding on probing and plaque indexes for each volunteer was obtained dividing the mean value recorded for each implant/tooth by the total number of implants/tooth evaluated [18]. A previous intra-examiner calibration to the survey for both the indices listed above, as for the questionnaire was carried out. Prior to the survey was conducted, a pilot project in six patients; three with lower fixed denture and three with lower overdenture. The same questionnaires were applied in the test study, but the patients in the pilot study were not included in the final study.
Statistical Analysis
Data on questionnaires, plaque index and bleeding on probing were analysed using the Mann-Whitney test (statistical power= 85.56%), with comparison of the medians. To determine the relationship between qualitative variables, the chi-square test (statistical power 82.23%) was used. The SPSS software, version 20.0 was used, and the significance level of all tests was 95% (0.05%). The results were reviewed by an independent statistician. The p-value <0.05 was considered statistically significant.
Results
The sample consisted of 18 volunteers treated with lower overdenture (seven women and eleven men) with mean age of 63.7 years (±10.3 years) and 19 volunteers treated with lower fixed denture (twelve women and seven men) with mean age of 62.0 years (±11.2 years), a total of 37 patients. The minimum and maximum ages were 43 and 83 years, respectively.
All volunteers gave three or more positive answers in questionnaire 1; thus, all treatments could be classified as satisfactory in terms of masticatory ability restoration. There was statistical difference between the groups (Mann-Whitney; U=102.000; α=0.05; p=0.0050), and volunteers treated with fixed denture had a higher median of positive answers [Table/Fig-1].
Median, Mean and Standard Deviation (SD), of positive answers in questionnaire 1 for overdenture and protocol groups.
| Overdenture | Protocol | p-value |
|---|
| Median | 4.5b | 5.0a | 0.0050* |
| Mean (SD) | 4.3 (0.8) | 5.0 (0.2) |
| Min | 3 | 4 |
| Max | 5 | 5 |
*Mann-Whitney test (α=0.05)
a,bThere was statistical difference between the types of prostheses
No association was observed between the frequency of positive answers and age (Chi-square test, χ2=0.8580; p=0.5600), sex (Chi-square test, χ2=0.8980; p=0.5830), and type of antagonist (Chi-square test; χ2=p=0.1870).
For questionnaire 2, all of the patients scored higher than 7 on the VAS in the four questions about masticatory ability. Therefore, all treatments were considered satisfactory. The medians of the groups were statistically different for all questions (p<0.05), and patients in the protocol group yielded higher median values [Table/Fig-2]. The frequency of answers with a score of 10, which corresponds to being completely satisfied, was 94.7%, 100%, 100% and 84.2% for questions 1, 2, 3 and 4, respectively for the protocol group. For the overdenture group, the frequency of total satisfaction was 16.7%, 38.9%, 38.9% and 44.4% for questions 1, 2, 3 and 4 respectively. Data analysis was performed to check Cronbach’s alpha [20] and its internal consistency for the questionnaires and the value obtained was α= 0.8030 [Table/Fig-2], α=0.6200 [Table/Fig-3].
Median, Mean, SD, minimum and maximum VAS values in questionnaire 2 for overdenture and protocol groups.
| Q1 – How do you rate your ability to chew foods? |
|---|
| Overdenture | Protocol | p-value |
|---|
| Median | 8.0b | 10.0a | 0.0001* |
| Mean (SD) | 8.4 (0.9) | 9.9 (0.5) | U=38.0 |
| Min | 7.0 | 8.0 | |
| Max | 10.0 | 10.0 | |
| Q2 – Are you satisfied with your lower dental prosthesis? |
| Overdenture | Protocol | p-value |
| Median | 9.0b | 10.0a | 0.0001* |
| Mean (SD) | 8.9 (1.1) | 10.0 (0.0) | U=66.5 |
| Min | 7.0 | 10.0 | |
| Max | 10.0 | 10.0 | |
| Q3 – Are you satisfied with the stability/retention of your prosthesis? |
| Overdenture | Protocol | p-value |
| Median | 8.5b | 10.0a | 0.0001* |
| Mean (SD) | 8.8 (1.0) | 10.0 (0.0) | U=66.5 |
| Min | 7.0 | 10.0 | |
| Max | 10.0 | 10.0 | |
| Q4 – Are you satisfied with the aesthetics of your prosthesis? |
| Overdenture | Protocol | p-value |
| Median | 9.0b | 10.0a | 0.0260* |
| Mean (SD) | 9.1 (1.0) | 9.6 (1.0) | U= 109.0 |
| Min | 7.0 | 7.0 | |
| Max | 10.0 | 10.0 | |
*Mann-Whitney test (α=0.05); U (alpha of Cronbach=0.8030)
a,bThere was statistical difference between the types of prostheses
Median, Mean, SD, minimum and maximum score values in questionnaire 3 for overdenture and protocol groups.
| Functional limitation | Overdenture | Protocol | p-value |
|---|
| Median | 3.0a | 1.0b | 0.0001* |
| Mean (SD) | 2.6 (0.9) | 1.4 (0.7) | U=53.0 |
| Min | 1.0 | 0.0 | |
| Max | 4.0 | 2.0 | |
| Physical pain | Overdentue | Protocol | p-value |
| Median | 1.0a | 0.0b | 0.0140* |
| Mean (SD) | 1.2 (1.1) | 0.4 (0.7) | U=97.0 |
| Min | 0.0 | 0.0 | |
| Max | 3.0 | 2.0 | |
| Psychological discomfort | Overdenture | Protocol | p-value |
| Median | 0.0a | 0.0b | 0.0010* |
| Mean (SD) | 0.8 (0.9) | 0.0 (0.0) | U=95.0 |
| Min | 0.0 | 0.0 | |
| Max | 2.0 | 0.0 | |
| Physical disability | Overdenture | Protocol | p-value |
| Median | 0.0a | 0.0b | 0.0820 |
| Mean (SD) | 0.4 (0.7) | 0.1 (0.3) | U=130.0 |
| Min | 0.0 | 0.0 | |
| Max | 2.0 | 1.0 | |
| Psychological disability | Overdenture | Protocol | p-value |
| Median | 0.0a | 0.0a | 0.1410 |
| Mean (SD) | 0.1 (0.3) | 0.0 (0.0) | U=152.0 |
| Min | 0.0 | 0.0 | |
| Max | 1.0 | 0.0 | |
| Social disability | Overdenture | Protocol | p-value |
| Median | 0.0a | 0.0a | 1.0000 |
| Mean (SD) | 0.0 (0.0) | 0.0 (0.0) | U=171.0 |
| Min | 0.0 | 0.0 | |
| Max | 0.0 | 0.0 | |
| Handicap | Overdenture | Protocol | p-value |
| Median | 0.0a | 0.0a | 1.0000 |
| Mean (SD) | 0.0 (0.0) | 0.0 (0.0) | U=171.0 |
| Min | 0.0 | 0.0 | |
| Max | 0.0 | 0.0 | |
| Total | Overdenture | Protocol | p-value |
| Median | 5.0a | 1.0b | 0.0001* |
| Mean (SD) | 5.2 (2.3) | 1.9 (1.4) | U=39.0 |
| Min | 2.0 | 0.0 | |
| Max | 9.0 | 4.0 | |
*Mann-Whitney test (α=0.05); U (alpha of Cronbach=0.6200)
a,bThere was statistical difference between the types of prostheses
The total sum of the OHIP-Edent questionnaire scores showed that there is statistical difference between the groups and that the protocol group had the lowest median, suggesting higher level of satisfaction of patients with this type of prosthetic treatment. The seven categories of the questionnaire were also analysed separately. In this case only the functional limitation, physical pain and psychological discomfort categories were statistically different [Table/Fig-3]. The protocol group had a higher median for bleeding and plaque indexes than did the overdenture group [Table/Fig-4].
Median, Mean, SD, minimum and maximum values of the bleeding index and plaque index for overdenture and protocol groups.
| Bleeding index |
|---|
| Overdenture | Protocol | p-value |
|---|
| Median | 0.00b | 0.31a | 0.0001* |
| Mean (SD) | 0.05 (0.07) | 0.33 (0.16) | U=29.0 |
| Min | 0.00 | 0.00 | |
| Max | 0.25 | 0.56 | |
| Plaque index |
| Overdenture | Protocol | p-value |
| Median | 0.25b | 0.75a | 0.0010* |
| Mean (SD) | 0.38 (0.40) | 0.93 (0.69) | U=63.0 |
| Min | 0.00 | 0.25 | |
| Max | 1.25 | 3.00 | |
*Mann-whitney test (α=0.05); U (alpha of Cronbach)
a,bThere was statistical difference between the types of prostheses
Discussion
Oral health self-perception has been one of the quality of life indicators widely used in Dentistry. In the present study, the self-perception of patients was quantified by means of three questionnaires in order to detect improvement in OHRQoL of patients rehabilitated with implant-supported prostheses [8,21-25]. These tools may clarify some questions dental surgeons might have about the type of rehabilitation that best suits the patient’s health status. Amongst the questionnaires found in literature, the Oral Health Impact Profile (OHIP), with its several versions was used [25]. In the present study, the OHIP-Edent was used, which assesses changes in the OHRQoL after rehabilitation with new prostheses as efficiently as does the original model (OHIP-49) [21].
Questionnaires 1 and 2 refer exclusively to masticatory ability. In both questionnaires, all volunteers obtained scores that were higher than the minimum limit to consider the treatment as satisfactory. However, the observed statistical differences show that the fixed denture group had a higher level of satisfaction than did the overdenture group. In questionnaire 2, which uses VAS, the frequency of answers with a score of 10, corresponding to total satisfaction, ranged from 86 to 100% for the protocol group, and from 14 to 44% for the overdenture group. These findings are in agreement with the studies [21,24,26,27] who also concluded that both protocol treatments (fixed denture) and overdenture [Table/Fig-5,6] are able to improve the quality of life and patient satisfaction, but with a slight preference for the protocol. However, we need more studies to support this statement.
Patient with lower implant fixed denture.
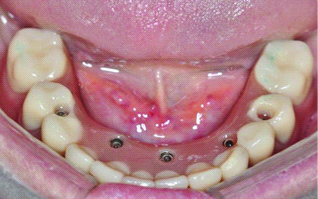
Patient with lower overdenture.
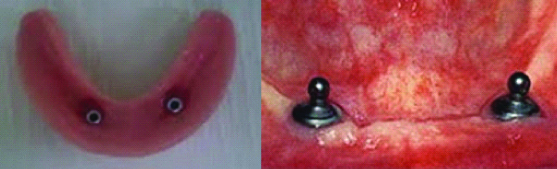
Consolidating the results obtained in the present study when using OHIP-49 and VAS to assess the impact on the oral health of individuals, another study proved the relationship between the implementation of implant-supported rehabilitation treatment (overdentures) in 44 individuals, with a survival of 100% of implants and prosthesis and consequently improves the quality of life of individuals. On the other hand, they observed an association between the variables age and gender and quality of life, which was not verified in the present study [28].
Satisfaction also depends on technical and patient related variables. The questions about physical pain dealt with pain and discomfort, revealing that the overdenture group was more dissatisfied. Regarding psychological discomfort, the questions dealt with preoccupation and embarrassment of patients over their prostheses. In this case, patients rehabilitated with overdentures also showed higher levels of dissatisfaction than those treated with fixed dentures. These results may differ from others depending on the sample and regional characteristics. As to physical disability, psychological disability, social disability and handicap condition, there was no statistically significant difference between the two groups. These categories include questions about the patient’s feelings towards treatment [12,21,29].
Results from the OHIP-EDENT questionnaire showed that patients rehabilitated with protocol were more satisfied with the treatment than those in the overdenture group [12,30]. On the other hand, in this study, when the score of each category was separately analysed, there was statistical difference between the groups only for the functional limitation, physical pain and psychological discomfort. Under these circumstances, the fixed denture treatment outperforms the overdenture one as it maintains the masticatory function stable. Food impaction is also unfavourable to removable dentures since the residues compress the oral mucosa, producing in some cases, lesions that eventually cause pain, discomfort and patient dissatisfaction [12,28].
A prospective mouth-split trial evaluated the benefits for quality of life with implant treatment with mandibular overdenture using OHIP-14 in a sample of 49 edentulous bimaxillary patients. They stated that, after three months of functional load, the OHIP-14 index was reduced considerably, suggesting an improvement in quality of life, which was maintained in the long term. The variables functional limitation, physical pain and psychological discomfort presented conflicting results for the mean values with the present study being 1.01, 1.09 and 1.23, (These results aren’t relative to our study, but the study mentioned above. So they aren’t present in [Table/Fig-3]) respectively [31].
Another study also used OHIP14 to assess the satisfaction of 45 patients who received full-arch removable overdenture anchored on two milled bars totaling 185 dental implants. At the end of the 2-year follow-up period, there was satisfaction with the aesthetic and functional results obtained. However, for functional limitation, physical disability the effect was moderate and for physical pain the size of the effect was exacerbated. According to the authors, these results can be explained by the fact that proportionally to greater retention and stability, there is a drastic reduction in the referred painful symptoms. In contrast, these results were not directly influenced by the gender or age of the individuals [10,32].
Another study, who evaluated the association between satisfaction of oral rehabilitation with mandibular conventional denture or implant overdenture and OHRQoL in 255 edentates, analysed that chewing ability and oral condition were significantly associated with quality of life. However type of treatment, gender, age and other socio-demographic variables were not significantly associated with improvement in OHRQoL [28].
A systematic review of studies comparing conventional complete denture and implant retained overdenture states that the socioeconomic level and education of individuals seemed to influence the satisfaction score with the prostheses, where patients with lower income but with fixed employment indicated greater satisfaction with the prosthetic rehabilitation treatment [29].
In a retrospective evaluation, unsplinted implant-retained maxillary overdenture therapy was associated with high implant and prosthetic survival, as well as high patient satisfaction and quality of life. Age, sex, maxillary mucosal health and mandibular dental status resulted in significant differences with respect to oral health related quality of life and patient satisfaction, indicating that this treatment option may be ideal for certain patients [32].
With similar methodology but with divergent results, a study was conducted on fifty-two patients rehabilitated using the Brånemark protocol (fixed denture) and twenty-three using overdenture prostheses. An adapted oral health-related quality of life questionnaire was used along with a clinical exam. The treatments presented satisfaction above of almost 90%, with no statistical difference. More of eighty percent of patients treated with overdentures and eighty percent of those treated with fixed denture had no pain [33].
Studies observed that patients rehabilitated with fixed dentures were more satisfied with their quality of life than those treated with either overdenture or conventional complete dentures, concurring with the findings of the present study [12,32,34,35]. On the other hand, studies didn’t find significant difference between the level of satisfaction reported by patients rehabilitated with overdentures and fixed dentures. However, when compared with conventional complete dentures, both treatment options yielded better results [14,33]. Loss of teeth has a negative influence on essential oral functions. Perceptions of edentulous patients’ about the impact of treatment options on oral health-related quality of life (OHRQoL) and satisfaction should be well understood. The results of this umbrella systematic review depicts the superiority of using overdentures compared with fixed dentures on the OHRQoL and patients’ satisfaction outcomes. However, this positive impact is enhanced when patients demand implant treatment or cannot adapt to denture treatment. Financial factors and adaptive capability affects patient compliance to both treatment modalities [10,29].
Clinical examination observed that patients treated with protocol showed higher plaque and bleeding on probing indexes. Patients with overdentures presented better oral health status. High rates of bacterial plaque, inflammation of marginal tissues and increase in probing depth was reported in a previous study with patients treated with protocol and clinical follow-up of 5 years [32].
However, the groups were homogenously distributed in terms of sex, age and type of dental service. Moreover, it was suggested that the results were not influenced by these variables, as no relationship was observed between the frequency of positive answers to the questions in questionnaire 1 and the aforementioned variables.
Overall, the protocol treatment improved the OHRQoL and patient satisfaction in comparison to the overdenture treatment. These findings could help dentists to choose the best treatment option for their patients.
Limitation(s)
Patients were obtained from a random sample in Southern Brazil at the clinics of graduate programs, which could be a study limitation.
Conclusion(s)
In this study, both rehabilitation methods (fixed denture and overdenture) used in complete edentulous patients substantially increase the satisfaction and improve the quality of life of patients. Fixed denture showed a higher satisfaction index for retention, stability of the prosthesis and also for chewing hard foods.
So, both rehabilitation treatments increased the satisfaction and improved the oral health and masticatory ability of edentulous patients. However, patients rehabilitated with fixed denture resented higher level of satisfaction, they also showed higher plaque and bleeding on probing indexes.
We suggest that further studies should investigate larger samples and perform longitudinal follow-ups of prostheses and implant treatments in order to improve the results reliability.
*Mann-Whitney test (α=0.05)
a,bThere was statistical difference between the types of prostheses
*Mann-Whitney test (α=0.05); U (alpha of Cronbach=0.8030)
a,bThere was statistical difference between the types of prostheses
*Mann-Whitney test (α=0.05); U (alpha of Cronbach=0.6200)
a,bThere was statistical difference between the types of prostheses
*Mann-whitney test (α=0.05); U (alpha of Cronbach)
a,bThere was statistical difference between the types of prostheses